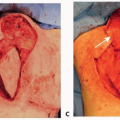
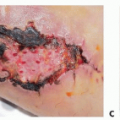
Pericranial Flap Harvest for Frontal Sinus Obliteration
Mahmoud Hassouba
John A. van Aalst
DEFINITION
The pericranial flap is a well-vascularized, versatile cranial periosteal flap that can be based anteriorly on the supratrochlear and supraorbital arteries or laterally on the superficial temporal artery.1
The pericranial flap is most commonly used for reconstruction of anterior skull base defects, including obliteration of the drainage system of the front sinus following frontal sinus fracture.
ANATOMY
The scalp consists of five layers: skin, subcutaneous connective tissue, galea aponeurotica, loose areolar tissue, and the pericranium.
The pericranium is the periosteum of the skull bones and is continuous with the endosteum along the cranial suture lines.
The pericranial flap consists of the skull periosteum with the overlying subgaleal areolar tissue.
The blood supply of the anteriorly based pericranial flap is derived from the deep branches of the supraorbital and supratrochlear arteries, and both are branches of the ophthalmic artery.
The deep branches arise from the supratrochlear and supraorbital artery exiting at the level of the supraorbital rim.2
There is wide variation in the size of these arterial branches depending on the size of the frontal branch of the superficial temporal artery.2
The axial length of these branches ranges between 15 and 60 mm and most commonly is approximately 40 mm in length.2
In the horizontal plane, the anastomosis between the deep branches is not well developed, and except for the glabellar region, no anastomoses cross the midline.
PATHOGENESIS
The most common indication for sinus obliteration requiring pericranial flap is a fracture of the posterior wall of the frontal sinus.
As with most craniofacial injuries, frontal sinus fractures result from high-velocity blunt trauma such as motor vehicle accidents.
PATIENT HISTORY AND PHYSICAL FINDINGS
Frontal sinus fractures are often associated with other facial injuries that require a detailed history, including the mechanism of trauma, as well as a thorough general and craniofacial-centric physical examination.
History taking may be complicated due to patient head injury with loss of consciousness.
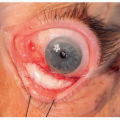
The main presenting symptoms are forehead swelling with or without skin lacerations, forehead paresthesia, and forehead and nasal pain.
Signs of frontal sinus fractures include forehead tenderness, contour deformity, crepitus, and cerebrospinal fluid (CSF) rhinorrhea.
Displaced fractures without skin lacerations may be masked by the overlying soft tissue swelling.
All lacerations should be examined under aseptic conditions to evaluate the integrity of both the anterior and posterior tables as well as the dura.
The nasal cavity should be examined for the presence of CSF drainage.
IMAGING
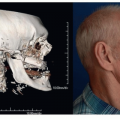
CT scan of the facial bones with coronal and axial cuts is the standard for diagnosis of fractures involving the frontal sinus.
3D reconstructions may be helpful in diagnosing associated craniofacial injuries.
SURGICAL MANAGEMENT
Indications for frontal sinus obliteration include fractures of the floor or posterior wall of the sinus, oncologic or inflammatory lesions of the frontal sinus such as osteomas or osteomyelitis, vascular lesions such as arteriovenous malformations, and failure of endoscopic sinus drainage surgery.3
PREOPERATIVE PLANNING
Routine preoperative lab results should be reviewed, and any abnormal finding should be corrected to prepare the patient for surgery.
All available imaging should be available and displayed in the operating room.
A sterilized radiographic template of the frontal sinus can be prepared from a Caldwell radiograph.
Doppler ultrasound should be available in the operating room for intraoperative localization of the flap pedicle if distorted anatomy is anticipated.
Positioning
The patient is placed in supine position on the operating room bed.
Oral intubation is preferred with the tube placed centrally and inferiorly.
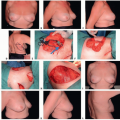
Approach
If a forehead laceration already exists, it can be extended into a natural crease.
A midforehead incision or a butterfly transglabellar incision may be used.4
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree