1 Our Introduction to Lower Extremity Reconstruction
Summary
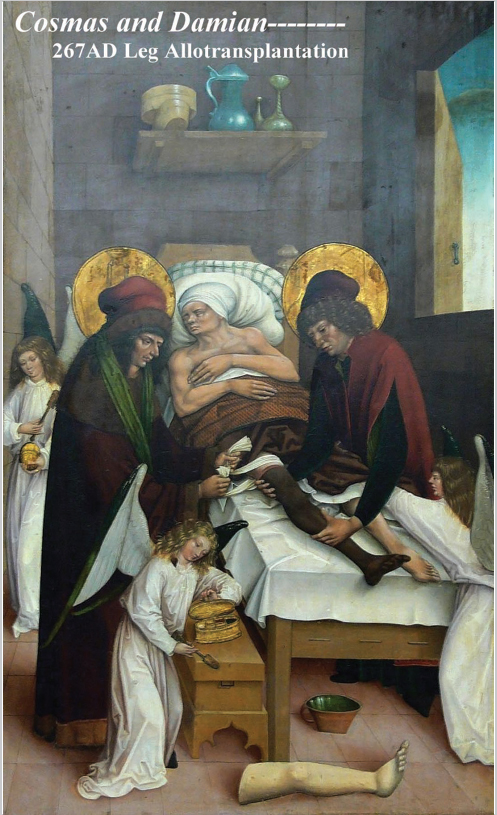
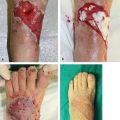
For a myriad of reasons, the lower extremity may be considered the most challenging of all body regions to reconstruct. Do not forget that the goal will always be to restore ambulatory function as much as possible, while ensuring long-term retention of vital structures or prosthesis, and obtaining an appearance that is satisfactory to the patient. Our capabilities to achieve this are in a constant state of evolution, as new techniques and/or innovations must be carefully scrutinized as to their efficacy. Although in the past amputation may have been the only treatment option, many surgical and nonsurgical means are now available to allow success in limb salvage. It behooves everyone interested in the management of these lower limb dilemmas to be aware of the long history of dealing with these challenges and to be familiar with the cornucopia of choices that must be made to best accomplish the outcome expected by the patients and their families (▶ Fig. 1.1).
Keywords: lower extremity reconstruction, lower limb salvage, amputation, microsurgery, perforator flaps
1.1 Introduction
Lower extremity reconstruction, whether needed for a sequela of severe trauma, cancer ablation, diabetes and/or vascular disease, or chronic infections, remains the most challenging of all reconstructions of the human body. The involvement of multiple discrete structures including bone, muscle, tendon, vessel, and nerve, all contained within the skin itself, makes it difficult to achieve the goal of restoring function, having long-term coverage of vital structures, and obtaining a satisfactory appearance of the lower limb. The objective of our effort then is to provide a pragmatic guide for our readers to understand the preoperative, intraoperative, and postoperative processes that will ultimately help them to develop a logical approach to lower extremity reconstruction that will more likely lead to a successful outcome.
Everyone must also understand that the management of lower extremity defects, whether complex or the most simple, is in a constant state of evolution as we are inundated daily by numerous new techniques and/or innovations that must be carefully scrutinized as to their worthiness. This has allowed the salvage of extremities today, whereas in the past amputation may have been the only alternative. For example, significant bone gaps can now be overcome by the current availability of vascularized bone grafts, Ilizarov lengthening, bone matrices, and growth factors. This coupled with new insights derived from our enhanced knowledge of anatomy like negative pressure wound therapy, tissue expansion or creep, and perforator flaps including propeller flaps has permitted superior soft-tissue coverage. Advances in microsurgery now reliably allow the use of small arteries (even < 1 mm in caliber for donor or recipient site anastomoses), or similarly permit lymphatic vessel interventions that will provide better surgical solutions for lymphedema.
Any attempt at lower extremity salvage must be recognized as a long and complex process for both the medical professional and the patients and their support systems. Therefore, as physicians it is important to ensure that all patients and family members are properly informed and included in any decision-making process,1 while maintaining on their part an accurate awareness of the expected prognosis. This approach should impact positively on any patient’s motivation and compliance while retaining the support of the family that will be critical not only during the necessary surgeries and hospitalization but also throughout the long phases of physical and psychological recovery.
1.2 History
Many say that the best use of the present is to rely on the past to make the future. What was the best solution may still be so, and at the least it has already had a definitive outcome that can appear predictable. So, history is important, and this has been acknowledged by us in the introduction of every chapter, where that pertinent saga has been included.
The early history of lower extremity reconstruction dates back to Hippocrates (460–370 BC), when amputation was the norm, and procedures trying to improve the success of amputation and survival of life itself were the main practice up to World War I.2 Although early amputation and rapid prosthetic fitting was believed to offer the potential of faster recovery at a lower cost, recent reports have differed from this traditional viewpoint. Undeniably, the choice of reconstruction will be a more challenging path to be taken; yet, the Lower Extremity Assessment Project (LEAP) study showed no significant difference in outcome when compared to amputation at 2 years.3 Interestingly, a cost analysis derived from this study concluded that amputation was more expensive than limb salvage, and amputation yielded fewer quality-adjusted life-years than salvage.4 Other reports have shown similar findings where projected lifetime health care costs for amputation may be as high as three times that spent on limb salvage.5,6 Even if the entire lower extremity cannot be salvaged, the primary goal now should be to maintain maximal limb length with durable soft-tissue coverage of any stump that can then be fitted properly with a prosthesis that will allow a functional gait. Preservation of the knee joint as in a below-knee amputation requires far less energy consumption, and has the potential for two- to threefold greater mobility when compared to an above-knee amputation.7,8
Not until the First and Second World Wars were pedicled flaps of some form used extensively to repair lower extremity injuries (▶ Fig. 1.2). Many of these had a discrete vascular supply, which today would be called “axial pattern flaps.”9 Stark10 and later Ger11 recognized that the leg muscles themselves were reliable flaps for leg coverage, having an abundant blood supply if outside the zone of injury (▶ Fig. 1.3).
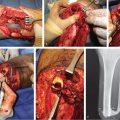
With the advent of microsurgical capabilities, extensive and complex defects even after severe trauma and truly radical debridements could be solved (▶ Fig. 1.4).
In 1986, a landmark publication for reconstructive lower extremity microsurgery by Godina established the principles of early extensive debridement, immediate free tissue transfer, and aggressive rehabilitation that routinely salvaged functional limbs.12 Radical debridement and coverage within 72 hours compared to more delayed treatment had superior outcomes, as only 0.75% of flaps failed, 1.5% of limbs became infected, and early bony union within 6.8 months was the norm.12
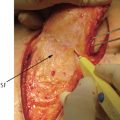
This dramatic deviation from established principles was followed by the development of functioning muscle transfers,13 innervated flaps to regain protective sensation of the sole,14,15,16 and tissue expansion to create a local flap option for large chronic defects17,18 or to minimize donor site morbidity.19 By the 1990s, Koshima (▶ Fig. 1.5) and Soeda20 provided convincing evidence of the value of perforator flaps (▶ Fig. 1.6), a cutaneous flap that best ensured preservation of muscle function. The anterolateral thigh flap—first introduced by Song et al,21 (▶ Fig. 1.7) just as Wei et al22 (▶ Fig. 1.8) proposed as the ideal soft-tissue flap for all purposes—is widely used worldwide today. However, currently perforator flaps in general allow better choice of a donor site that best matches the tissue qualities needed at the recipient site.23 Though originally utilized primarily as microvascular tissue transfers, increasingly they have become a local perforator flap option applicable to all zones of the lower extremity.24