Key points
• Osseous genioplasty is a more versatile procedure compared with chin implant surgery.
• The chin can be advanced, set back, narrowed, widened, lengthened, shortened, centered, and leveled with genioplasty.
• Osseous genioplasty gives the surgeon control of the labiomental crease.
• Perioral facial rejuvenation is much more powerful with osseous genioplasty than with a chin implant.
• The facial shape can be profoundly altered with osseous genioplasty, given the dimensional control provided to the surgeon.
• Osseous genioplasty is a powerful tool in facial rejuvenation.
Introduction
The chin is an important structure in the creation of an aesthetic facial shape and harmony. It is vital not only in contributing to facial proportion in frontal and lateral views but also in supporting the overlying soft tissues. The chin can be moved three dimensionally with an osteotomy (osseous genioplasty) or can be augmented with an alloplastic implant (alloplastic genioplasty) for more limited changes in chin position. The versatility of an osteotomy provides more precision to move the chin to its ideal position, but it is a more invasive procedure compared with the use of an implant. Chin augmentation with an alloplastic implant is considered a simpler procedure by most surgeons and has a faster patient recovery time, but in the majority of indications, it cannot provide the same results as those of an osseous genioplasty. Compared with other maxillofacial procedures, either type of genioplasty is a relatively straightforward procedure offering predictable results and fast patient recovery.
Osseous genioplasty is a very powerful procedure to alter facial aesthetics. At a minimum, it advances the chin point in a sagittal direction. However, the ability to move the chin three dimensionally allows for making changes in facial symmetry, proportion, soft tissue support, and shape.
Anatomy
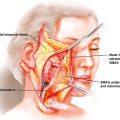
The chin comprises skin, subcutaneous tissue and fat, muscles, and bone. The depressor angularis oris, depressor labii inferioris, and mentalis muscles attach to the anterior plane of the chin. The geniohyoid, genioglossus, mylohyoid, and anterior belly of the digastric muscles attach to the lingual aspect of the chin at the genial tubercle. The blood supply to the mental area is from the inferior alveolar artery and vessels from the geniohyoid, genioglossus, and anterior belly of the digastric muscles. The mental nerve supplies sensation to the anterior mandibular gingival mucosa and the lower lip. This nerve is a continuation of the inferior alveolar nerve and becomes the mental nerve after it exits the mental foramen between the first and second premolars. The mental foramen has been shown to be located 14.61 mm superior to the inferior border of the mandible. Because the inferior alveolar canal runs lower than the mental foramen, the osteotomy must be planned at least 5 mm caudal to the foramen.
Patient evaluation
Frontal view
Because the chin contributes to facial proportion, it is important to have an understanding of its normal and aesthetic values before planning treatment with an osseous genioplasty. When examining the face, it is important that teeth are in occlusion and that the lips are in repose. The vertical height of the face can be divided into thirds. The upper third is from the trichion to the glabella, the middle third is from the glabella to the subnasale, and the lower third is from the subnasale to the menton. The lower facial third can be further subdivided so that the chin is divided in half by a line passing through the stomion, and the distance between the stomion and the menton should be twice as long as the distance from the subnasale to the stomion.
The width of the chin is evaluated as the focal point of the mandible. In the male, the jaw will diverge from the chin with a broad and defined gonial angle, giving a strong masculine appearance. In the female, a soft, narrow, heart-shaped mandible diverges from the chin. The width of the chin will have a dramatic effect on the perception of the jaw shape. It is important to assess the width of the chin because it can be changed with an osseous genioplasty, thus altering the appearance of the jawline and the lower facial shape.
When assessing for the transverse symmetry of the chin, it is useful to mark several points (glabella, nose, dental midlines, vermilion, and chin) to see if all are congruent. Occasionally, these points are not aligned, and the surgeon needs to point this out to the patient preoperatively to explain the limitations of surgery. Ideally, the center of the chin is congruent with the mandibular skeletal and dental midlines. If the chin is not centered, a centering genioplasty is indicated. If the chin and the mandibular midline are not centered, a mandibular osteotomy is necessary to correct the asymmetry. When the chin is moved, a 1:1 ratio of bone to soft tissue movement is anticipated when planning the final position.
The perioral soft tissues are also assessed. Marionette lines and jowls may be improved after osseous genioplasty. If the bone is advanced sagittally or vertically, the perioral soft tissues will improve as the underlying skeletal support is increased. Even in young patients, it is important to be aware of these beneficial effects so that the surgeon can develop a treatment plan that will benefit a young patient as he or she matures.
Lateral view
From the lateral view, the four aspects of the chin that most affect aesthetics are the sagittal and vertical projections of the chin, the labiomental angle, and the submental soft tissue support. The sagittal projection of the chin may be determined by several methods. Byrd has described a method wherein a line is dropped from the middorsum of the nose inferiorly and tangential to the upper lip. Assuming that the nose is of normal length, the chin should be about 3 mm posterior to this line. Another method is to drop a line inferior and perpendicular to Frankfurt horizontal (FH) plane that is tangential to the lower lip. The chin should be just posterior to this line in females and at or slightly anterior to it in males. A final analysis is the Riedel line. This line connects the most prominent points of the upper and lower lips, and the most prominent point of the chin should be the third point on this line.
The labiomental angle is another important dimension that contributes to the aesthetic appearance of the chin in profile. Vertical reduction or anterior movements will increase the acuity of the labiomental angle, and vertical elongation or posterior positioning will make the angle more obtuse. Farkas described the normal labiomental angle in adult females as 121 degrees and that in adult males as 114 degrees, and Reyneke has stated it to be 130 degrees. , However, it is important to remember that in the majority of cases, the patient does not necessarily want to be “normal” but beautiful. Iglesias-Linares et al. reviewed the labiomental angles in the 40 most beautiful white and black females, as voted by a popular beauty magazine, and the average labiomental angle in this group is 108.75 degrees for the 40 white women and 104.75 degrees for the 40 black women. There is no statistically significant difference between the two groups. The ultimate judgment of the result is the patient, but it is important to note that norms do not always equate with the aesthetic ideals.
Influence of facial features on the perception of the chin
Other factors that affect the perception of chin position, but are not intrinsic to the chin itself, are nasal projection, vertical maxillary position, and mandibular projection. An overprojected nose may give the illusion of a small chin, and vice versa. Vertical maxillary excess will cause the mandible to be rotated in a clockwise position, which will decrease anterior chin projection. A vertically short maxilla will lead to counterclockwise mandibular rotation, which will increase chin projection. Problems related to an abnormal vertical maxillary position are best treated with a maxillary osteotomy.
The labiomental fold and the chin–lip relationship will aid in determining whether deficient chin projection is due to the chin, the mandible, or both. A deficient chin with a normal labiomental angle and lower lip relationship is likely due to mandibular retrognathia. If the labiomental crease is obtuse and the chin is well posterior to the lower lip, the deficiency is likely due to the chin. The degree to which the mandible contributes to chin projection may be evaluated by examining the occlusion. If an overbite is noted on physical examination, the degree to which the mandible would need to be advanced to achieve class I occlusion is typically the degree of mandibular deficiency. This value assumes normal maxillary projection and normal dental alignment. After advancing the mandible, if the chin remains deficient, the chin can be advanced to achieve an ideal projection based on the criteria discussed previously.
Preoperative planning
The ideal results of genioplasty include achieving a chin in ideal proportion, well-supported soft tissues, an ideal labiomental crease, and an aesthetic cervicomental angle. One must assess each of these variables in developing a treatment plan. As in rhinoplasty, changing one variable may have unintended effects on another. Several important relationships warrant review:
- •
The acuity of the labiomental crease becomes more obtuse when the chin is elongated or moved posteriorly.
- •
Soft tissue support is compromised by a movement that contracts the skeletal chin-shortening or posterior positioning.
- •
Soft tissue support is enhanced by a movement that increases skeletal chin advancement or vertical elongation.
- •
Advancing the chin tightens the muscles inserted on the genial tubercle, enhancing submental soft tissue contour.
When developing a treatment plan, it is important to incorporate these principles to optimize the aesthetic result for each patient. A patient who presents with deficient chin projection and an obtuse labiomental crease will do well with simple advancement genioplasty or a chin implant. However, a patient with deficient chin projection who has a normal or acute labiomental crease preoperatively will have an unaesthetic, severely acute labiomental crease if the chin is only advanced in the sagittal plane. In a case like this, it is important to assess if the chin can be lengthened without creating an excessively long lower facial third. The increase in acuity created by chin advancement will be offset by the opening of the labiomental angle created by lengthening the chin, resulting in an increase in chin projection with an aesthetic postoperative labiomental angle. Because it is difficult to vertically elongate the chin with an implant, the patient with sagittal chin deficiency and a normal labiomental crease is not ideally treated with a chin implant. In this case, the increase in chin projection due to the implant creates an excessively acute labiomental angle because the implant is not capable of neutralizing this effect with compensatory vertical elongation.
In patients who cannot tolerate an increase in the height of the lower facial third, the compensatory effect on the labiomental crease may not be tolerated. The tradeoff between chin projection and labiomental crease aesthetics must be discussed preoperatively to educate the patient about the limitations of the procedure. Maintaining an ideal labiomental crease may sacrifice ideal chin position, and vice versa. A similar dilemma occurs in a patient who has a strong chin and desires posterior repositioning to reduce the chin prominence. As the chin is posteriorly positioned, soft tissue laxity develops submentally. Vertical elongation of the chin is an effective method of negating the submental redundancy, but if the patient’s lower facial third dimension does not tolerate lengthening, the degree of posterior chin positioning may need to be limited unless the patient is willing to undergo a neck lift to address submental laxity. Preoperative three-dimensional imaging is a useful tool in aiding the patient to determine his or her aesthetic goals.
Orthognathic camouflage
A patient may exhibit mandibular retrusion but will present with a class I occlusion. This is typically a patient who originally would have been ideally treated with orthognathic surgery but opted for nonsurgical orthodontic treatment. These patients will demonstrate a dental class I occlusion but at the expense of facial disharmony through orthodontic dental compensation. Frequently, orthodontists will extract the upper premolars to allow room for the upper teeth to be pulled back to meet into a class I occlusion with the lower teeth. As the upper teeth are moved posteriorly, lip support is lost, giving the perception of an overly projected nose. This commonly encountered group of patients will have the appearance of a large nose and a small jaw/chin yet have a class I occlusion. In addition to advancement genioplasty, these patients also may be candidates for rhinoplasty (this topic is covered in detail in Chapter 25 , Orthognathic Camouflage).
Facial rejuvenation
In adult patients with suboptimal chin projection, genioplasty is a powerful procedure, alone or in combination with a neck or facelift to rejuvenate the perioral soft issue. The geniohyoid, genioglossus, mylohyoid, and anterior belly of the digastric muscles attach to the lingual aspect of the chin, and as the chin is advanced, these muscles tighten, creating a taut submandibular contour. Additionally, the increase in length from the cervicomental crease to the pogonion will create the appearance of a more well-defined neck.
In patients who present with deficient chin projection, perioral tissue laxity, submental laxity, and an obtuse cervicomental angle, advancement genioplasty will have rejuvenative effects on the overlying soft tissue. Rosen has demonstrated that skeletal projection has beneficial effects on the overlying soft tissue envelope. , The majority of adult patients presenting for genioplasty desire pure anterior advancement. In middle-aged patients, it is important to determine whether they can tolerate vertical elongation of the chin as well. As long as the elongation does not create an excessively long lower facial third, it is a powerful adjunct to the anterior movement to support the perioral soft tissue to the fullest extent. This combination approach rejuvenates jowls, marionette lines, and the submandibular tissues. For these reasons, osseous genioplasty is an excellent option for patients who exhibit retrogenia and desire soft tissue rejuvenation of the lower facial third. Osseous genioplasty is also a powerful adjunct procedure when combined with a neck lift or facelift.
Digital imaging
Digital imaging is important for both treatment planning and documentation. Recommended views include frontal, right and left lateral, right and left oblique, worm’s eye, and bird’s eye views of the patient’s face. From these images, a dimensional analysis of the patient’s chin can be made, incorporating the previously mentioned normative values. Predictive digital imaging can also be performed, giving the patient an idea of the final result. However, it is important to inform the patient that the predicted image is not a guarantee of the result but a prediction to ensure the surgeon and the patient have the same goals in mind. To improve accuracy in treatment planning, it is recommended that a ruler be placed next to the patient’s face and the image enlarged to a 1:1 reproduction. This allows for accurately quantifying movements in millimeters and producing the most accurate assessment of the patient’s goals. The amount of movement that is desired by the patient as seen in the image will dictate the amount of surgical skeletal movements of the chin. Studies have shown that soft tissue follows skeletal movements in a 0.9-1.0:1 ratio for chin advancement procedures and a 0.6-1.0:1 ratio for chin reduction procedures, so the millimeter difference between the preoperative predicted image can be directly translated to the skeletal movements of the chin. When using an implant, the soft tissue-to-implant ratio is 0.8:1. Radiographic imaging should be obtained as well to document the absence of any osseous pathology before performing osseous surgery of the chin.
Radiographic imaging
A radiograph should be obtained before the chin surgery is performed to rule out the possibility of any osseous pathology, such as a cyst, tumor, vascular malformation, or foreign body. Any imaging that allows for visualization of the anterior mandible is sufficient. Cone beam computed tomography (CBCT) or pantographic radiography images obtained from a local dental office work well, are inexpensive, and require a low dose of radiation. Any previous images of this region that the patient has obtained within the past several years are acceptable as well.
Primary operative approach and surgical technique
The following technique applies to the standard single-piece advancement genioplasty. Most of these steps apply to all genioplasties, and where modifications are necessary, they will be described in each specific section.
- •
Infiltrate lower lip mucosa and mentalis with 10 cc 1% lidocaine 1:100,000 epinephrine. Because the injection is done before prepping and draping the patient, it will have redistributed by the time of the procedure so that accuracy is not compromised by the volume of infiltration.
- •
The patient is prepped after the injection allowing the epinephrine to take effect.
- •
The throat pack is placed, and chlorhexidine mouth rinse is poured into the oral cavity and allowed to sit for 5 minutes before being suctioned.
- •
Use the nondominant hand to evert the lip, using the index finger to palpate below the intraoral incision.
- •
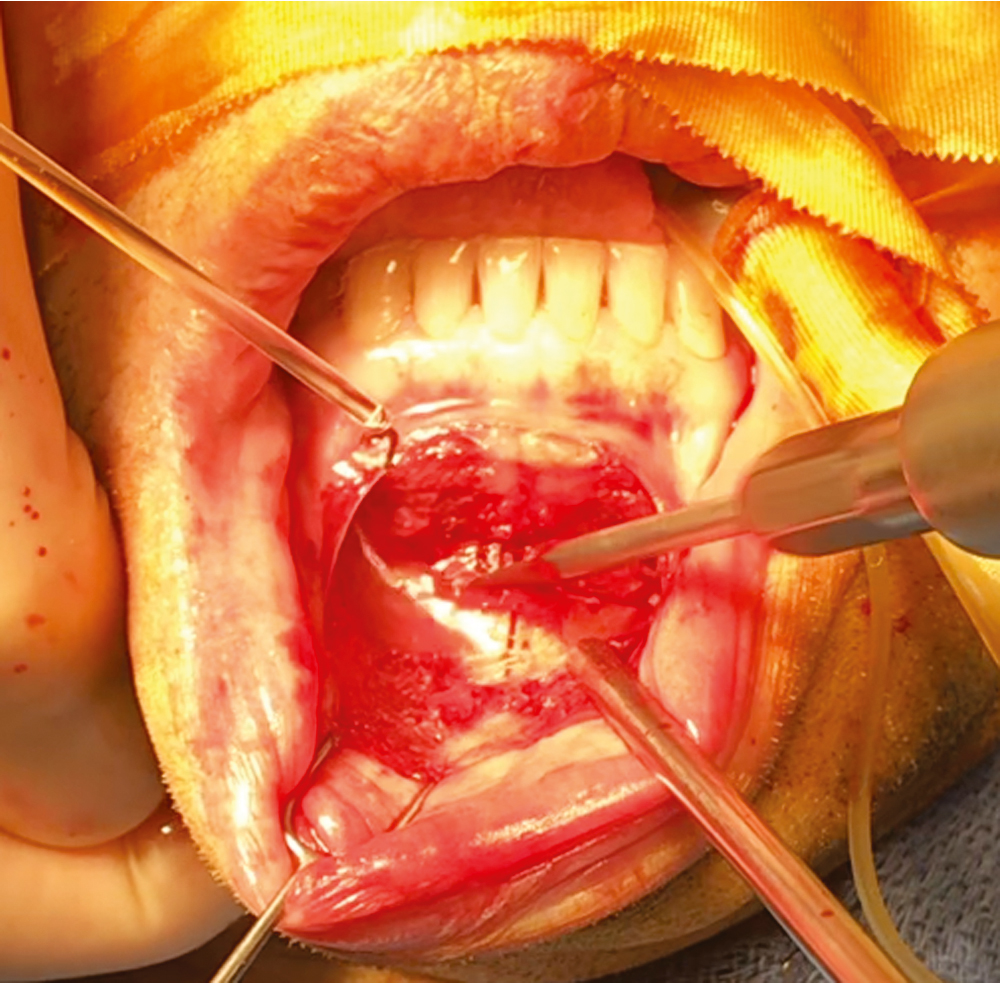
Using a guarded blunt tip Bovie, make the initial mucosal incision from canine to canine then redirect the Bovie toward the bone to divide the mentalis muscle. The left index finger is used to make sure that the Bovie tip does not inadvertently cut through the cutaneous surface ( Fig. 27.1 ).
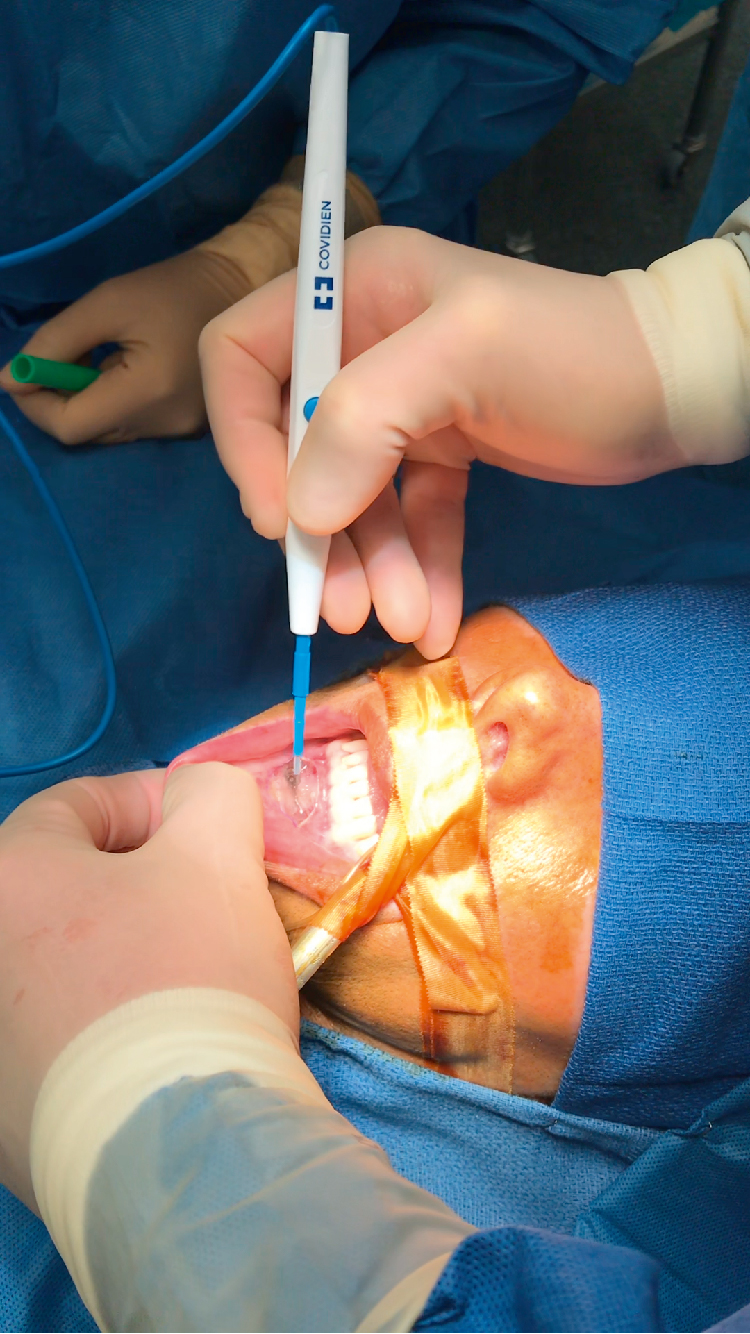
Fig. 27.1
The lip is everted, and the nondominant index finger is placed under the everted lip to palpate the electrocautery tip and to ensure that the surgeon does not inadvertently buttonhole the incision.
- •
A periosteal elevator is then used to dissect from the incision to the inferior border of the mandible in an inferior direction. Once the inferior border has been identified, the periosteal elevator can be used to dissect laterally in the subperiosteal plane along and parallel to the inferior aspect of the mandible. Because the mental foramen is 14 mm superior to the inferior mandibular border and the widest Obwegeser periosteal elevator is 10 mm wide, this dissection can be done rapidly and blindly without worry of hitting the mental nerve as long as the surgeon keeps the elevator flush with the inferior border of the mandible. We refer to this region as a dissection “hot lane,” meaning the dissection can be done very quickly without risk of injury to the mental nerve. Once this dissection has been done bilaterally, careful superior elevation easily identifies the mental nerve ( Fig. 27.2 ).
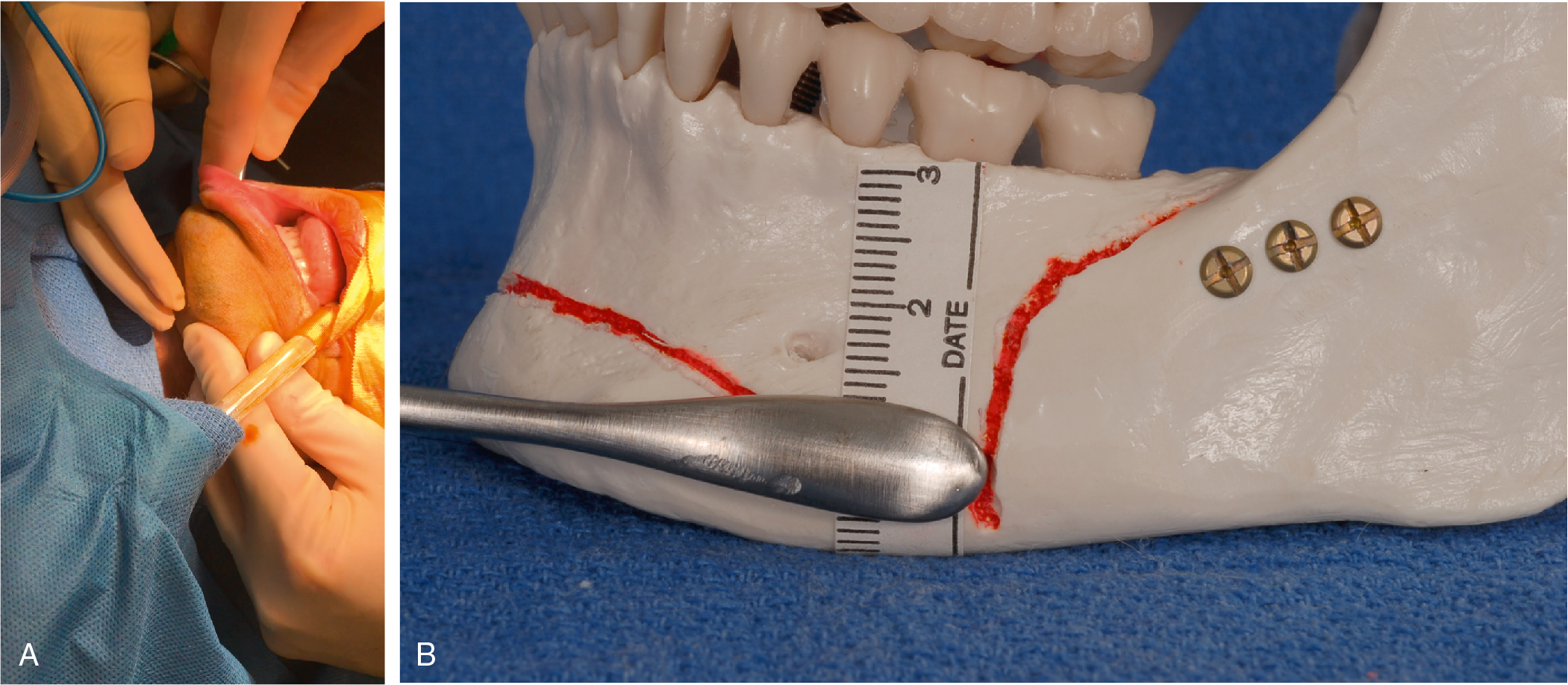
Fig. 27.2
(A) The Obwegeser periosteal elevator is placed such that the edge is adjacent to the inferior border of the mandible. The location is confirmed by palpation, and the surgeon can advance the elevator laterally in a subperiosteal plane to dissect the pocket rapidly. As long as the elevator’s inferior edge is congruent with the inferior border of the mandible, there is little risk of injuring the nerve, and the dissection can be done blindly. (B) The widest of the Obwegeser periosteal elevators is 10 mm. The distance from the inferior border of the mandible to the mental foramina has been shown to be 14.61 mm. Given that there is a 5-mm safety margin, a rapid blind subperiosteal dissection can be performed as long as the edge of the elevator hugs the inferior edge of the mandible.
- •
A reciprocating saw with a long blade is used to make a vertical line or score between the midline of the lower central incisors and additional lines 10 mm lateral to the midline on both sides. The midline cut is typically made between the lower central incisors; however, if it is slightly off midline, it is of no relevance because it is drawn merely as a reference to make sure that the chin remains midline when the plate is secured or as a reference if a transverse movement is planned ( Fig. 27.3 ).
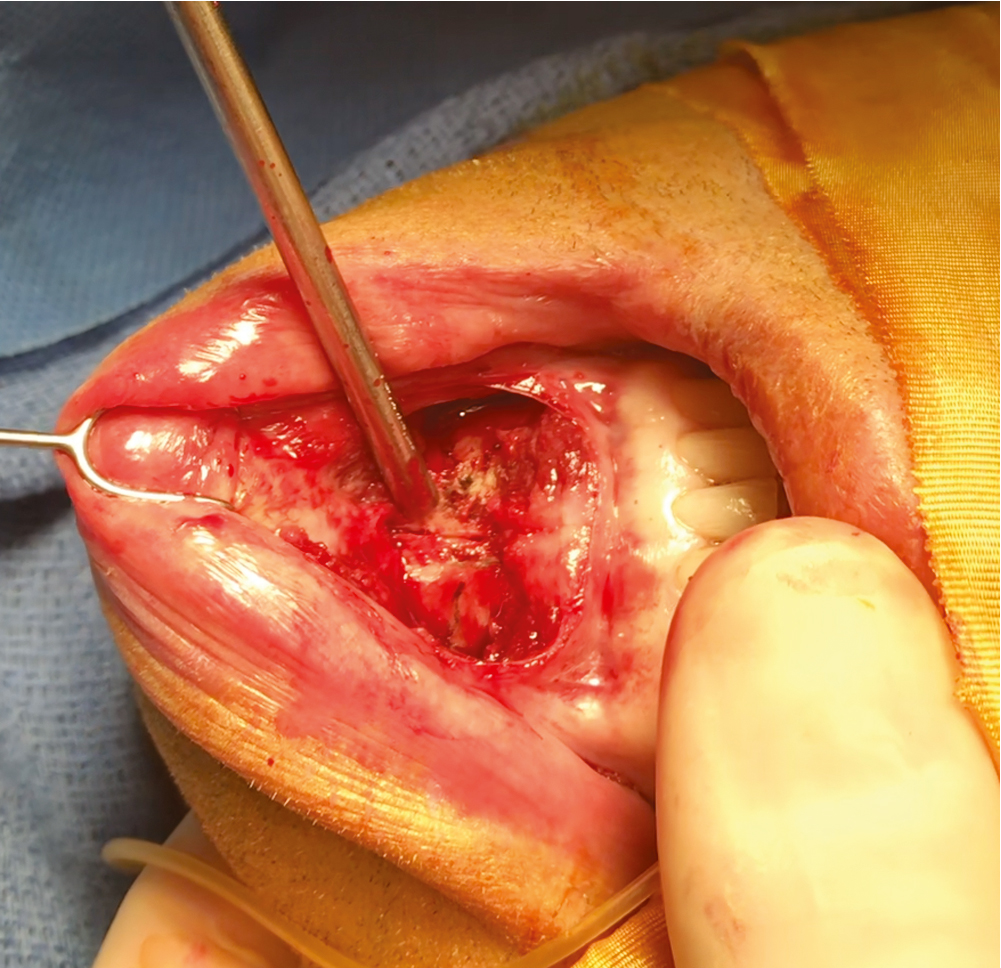
Fig. 27.3
A vertical cut is made just deep enough to score the midline of the anterior mandible. As long as the cut is unicortical, there is little danger of damaging the tooth roots. The vertical cut does not need to be midline because it serves only as a reference point to ensure that the inferior segment is moved accurately in relation to the mandible.
- •
Genioplasty retractors are placed to retract the mucosal tissue and to identify the mental foramen and protect the mental nerve. The osteotomy cut should be at least 5 mm inferior to the mental foramen because the nerve runs through the mandible inferior to the mental foramen before exiting and rises superiorly as it exits the mental foramen ( Fig. 27.4 ).