Key points
• The facial skeleton provides the underlying frame for the face, and its configuration influences the facial rejuvenation surgery that should be done.
• Age-related changes in the periorbital area are significant and must be accounted for during rejuvenation procedures.
• The overall shape of the face can be categorized on a continuum—from wide or round to long and thin. Different facelift techniques are required for these different facial shapes.
• There are significant volume shifts in the aging face with ptosis of soft tissue, loss of soft tissue in some areas, and accumulation of soft tissue in other areas.
• Facial rejuvenation includes procedures to add volume, remove volume, and reposition tissue.
• The modern facelift should be customized to account for the uniqueness of everyone’s facial skeleton and its influence on the shape of the aging face.
Introduction
Facial rejuvenation surgery encompasses all those procedures with the goal to make a patient look younger. In most cases, patients seeking rejuvenation surgery wish to turn back the clock, rather than to undergo fundamental changes in their appearance. In view of these facts, facial rejuvenation surgery intersects with facial skeletal considerations in two ways. First, we must consider the existing facial shape, highly influenced by the underlying facial skeleton, because it dictates the type of soft tissue surgery that can or should be done. Second, age-related changes in the facial skeleton must be considered in the design of surgical procedures to rejuvenate the aging face. In the aging human face, soft tissue changes are only part of the story.
The aging face undergoes changes in three anatomic components: the skeleton (see Chapter 13 ), soft tissue (see Chapters 9 and 34 ), and the overlying skin. In this chapter, we will review the various surgical procedures available for facial rejuvenation and discuss how the state of the underlying skeleton influences the choice and performance of these procedures. Skin rejuvenation procedures will not be discussed.
Forehead rejuvenation
Aesthetics
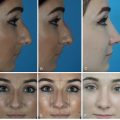
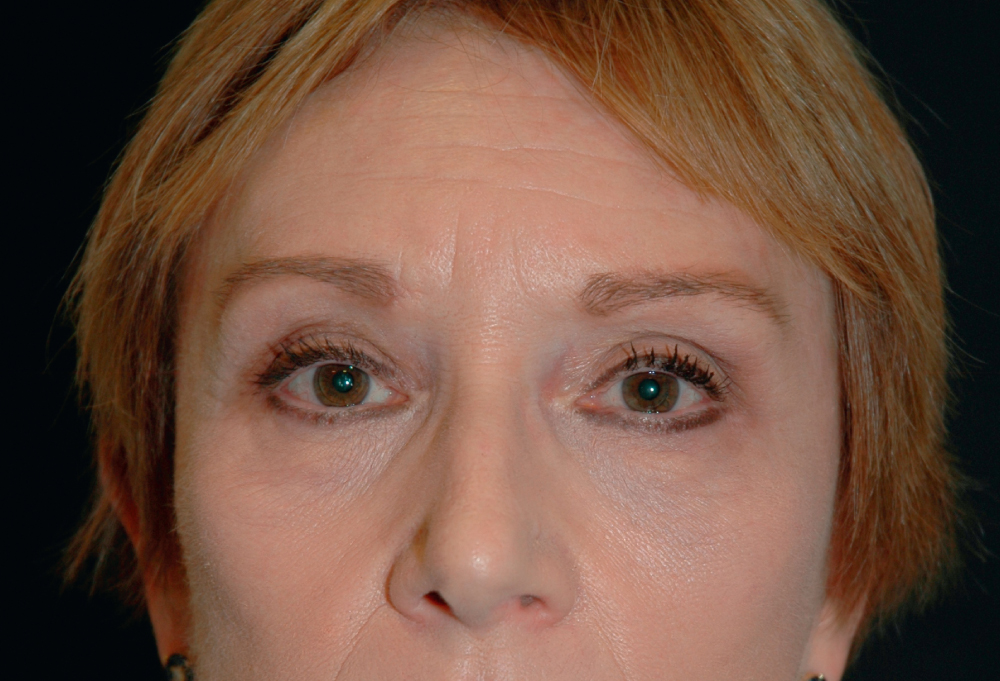
The most expressive part of the human face is the periorbital region. The eyes are framed by the eyebrows above and the lid–cheek junction below; alteration in either of these components will significantly influence facial appearance. Much has been written about the proper position and shape of the human eyebrow. Historically, patients have taken these variables into their own hands with eyebrow-shaping methods, such as eyebrow plucking, makeup, and tattoos. Studies have demonstrated that the level (height) of the eyebrows may or may not change over time, with many patients having a stable eyebrow position throughout their lives. Some patients demonstrate higher eyebrows with aging, likely due to chronic frontalis contraction, which, in turn, can be stimulated by incipient senile ptosis. The patient who lifts the eyebrow complex may also reveal a hollow upper lid sulcus, caused by fat atrophy and the underlying bony changes in the orbital skeleton. , However, about 50% of individuals develop eyebrow ptosis, which can be seen in the entire eyebrow, in just the medial brow, or most commonly, in just the lateral third of the brow. Some patients develop both brow ptosis and hollowing of the upper lid sulcus, a condition that must be managed carefully; elevating the brow without filling the sulcus will create an overly hollow upper lid sulcus ( Fig. 38.1 ).
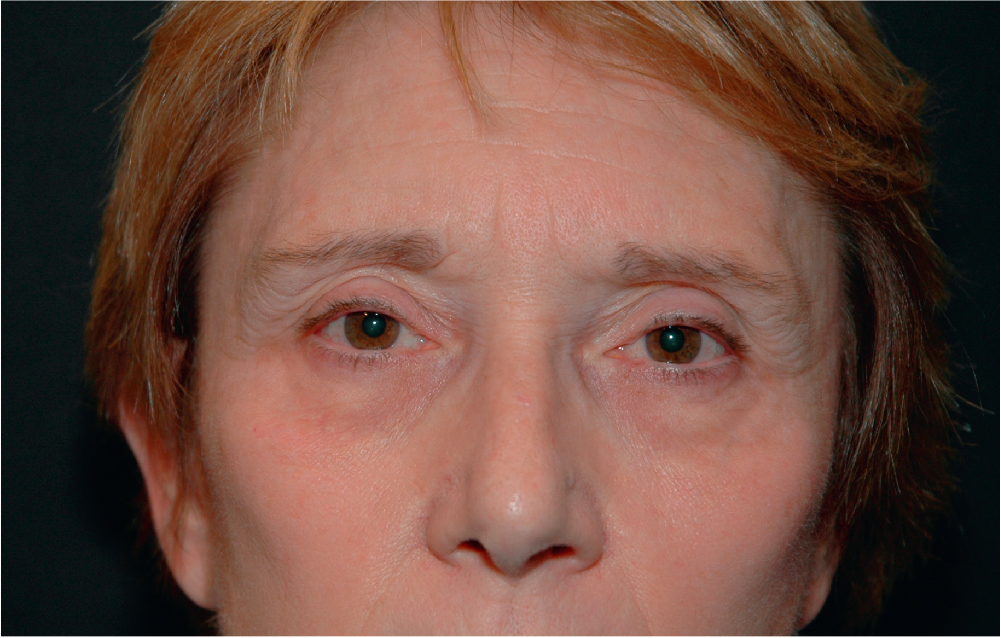
In the patient seeking forehead rejuvenation solely because of frown lines, treatment is generally limited to the injection of Botulinum toxin into the frown musculature. Small changes in brow shape can be accomplished with this method, as well as with injection of the lateral orbicularis. Some younger patients may have a congenital brow shape they wish corrected and for which surgery is the best option. The most common example is the downturned lateral brow, which gives people a sad or tired look. In the older individual who seeks facial rejuvenation, the forehead should always be reviewed in conjunction with an assessment of the upper eyelids and the upper lid sulcus. The upper eyelid–brow junction is an interrelated anatomic zone, where the function of any one part affects the other components in the zone. For the facial rejuvenation patient who is a candidate for brow surgery, surgical procedures are typically aimed at elevating all or part of the eyebrow complex.
Skeletal anatomy
Underlying the entire forehead is the frontal bone. It can be convex (a feminine trait) or flatter (a masculine trait), with a supraorbital ridge—more pronounced in the male. Laterally, the frontal bone is crossed by a curved ridge called the temporal crest (also called temporal ridge or superior temporal fusion line of the skull ). This palpable landmark separates the temporal fossa and the origin of the temporalis muscle from the forehead portion of the frontal bone ( Fig. 38.2 ). It also marks a change in nomenclature as the soft tissue planes transition from lateral to medial. The deep temporal fascia covering the temporalis muscle attaches along the temporal ridge and continues medially as the periosteum attached to the frontal bone. The superficial temporal fascia (also known as temporal parietal fascia ) continues medially as the galea aponeurotica, which encompasses the frontalis muscle.
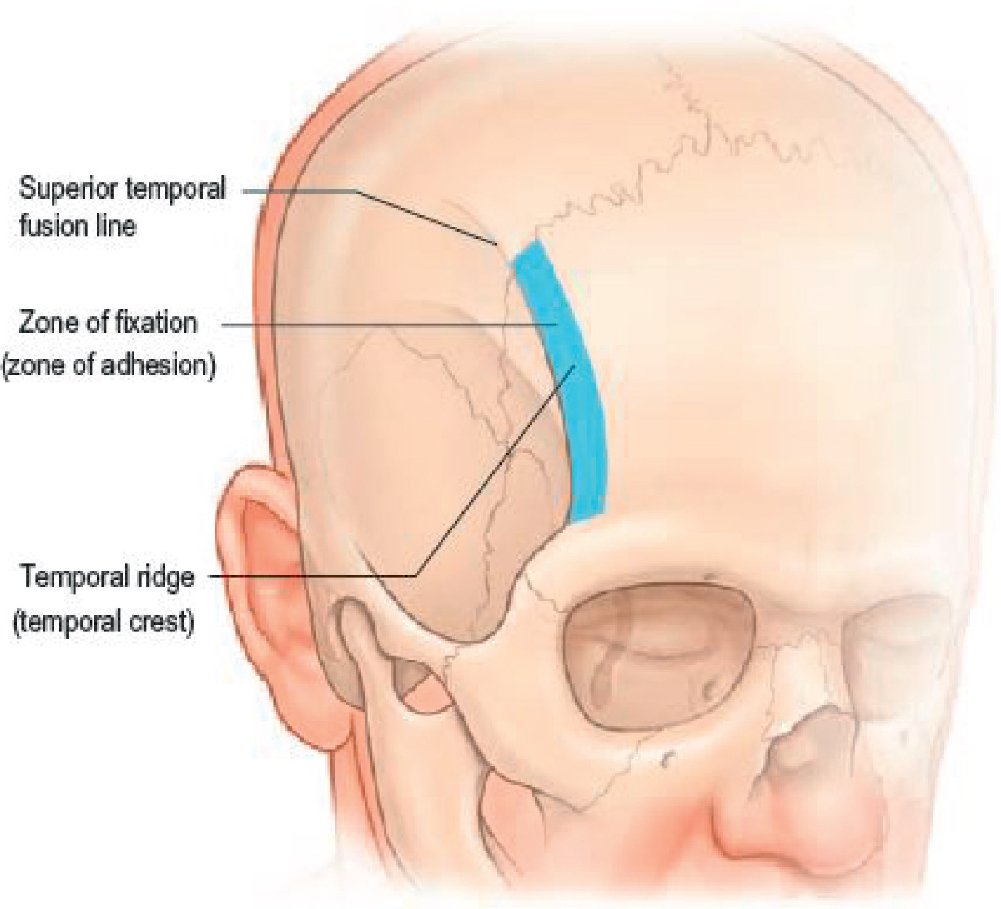
The surgical significance of the temporal crest line is that all fascial layers are tethered to bone in a band approximately 5 mm wide immediately medial to the palpable ridge. This has been called the zone of fixation or zone of adhesion. Where this zone approaches the orbital rim at its inferior end, the fascial attachment widens and becomes denser, forming the orbital ligament, also known as the temporal ligamentous adhesion. All fascial attachments in this region must be released from bone when a full-thickness forehead flap is being repositioned to elevate the lateral eyebrow. Inferior temporal septum and orbicularis–temporal ligament are terms that describe the criss-crossing white fibers which loosely attach the superficial to the deep temporal fascia in the midtemple. The inferior temporal septum is a useful landmark during dissection from above because it separates the safe upper zone containing no vital structures from the lower zone, where facial nerve branches travel in the cavity’s roof. The medial zygomatic temporal vein (sentinel vein) is also present in this lower zone, adjacent to the lateral orbital rim. The temporal branches pass immediately superior to this vein.
Surgical considerations
Surgical techniques available for forehead rejuvenation are numerous. Simple frown muscle modification can be done through the upper sulcus (blepharoplasty) approach or through the endoscopic approach from above. Brow lifting or reshaping can be done through the open coronal approach (incision within the scalp or at the anterior hairline), the endoscopic approach, the isolated temple lift, various subcutaneous lifts (incisions at the eyebrow, in a transverse brow crease or at the hairline), or transblepharoplasty browpexy.
The shapes of the frontal bone and the supraorbital ridge have a significant role to play in facial feminization surgery, where the prominence of the ridge can be reduced (see Chapter 43 ). Similarly, in the patient with a retrusive forehead in relation to the supraorbital rim, augmentation of the frontal bone may be indicated (see Chapter 42 ). In the setting of facial rejuvenation, patients who may present for forehead surgery can benefit from either of these techniques.
The underlying shape of the frontal bone can significantly influence the endoscopic brow lift procedure. When the underling forehead is flat, the view through the endoscope will be direct, and the surgical instruments will be easy to manipulate. When the forehead is convex, the endoscopic view can be impaired because the operator is using a straight scope to look around a curved surface. Also, straight endoscopic instruments will be more difficult to use in this setting. To deal with this issue, the entry incision for the endoscope can be made closer to the hairline than normal, at the anterior hairline or potentially within a transverse brow crease. Unlike the endoscope itself, endoscopic instruments can be curved or malleable, enabling the surgeon to work around a curved frontal bone.
In addition to affecting the ease of doing endoscopic surgery, the convex forehead also tends to limit the effectiveness of the brow lift itself—be it endoscopic or open coronal. This difficulty is compounded when the convex forehead exists in conjunction with a high hairline.
Upper lid blepharoplasty
Aesthetics
The junction of the upper eyelid and the eyebrow is a complex region with a number of anatomic variables that influence appearance. Many authors have tried to define the ideal appearance of this area, and some common themes have emerged. The most significant aesthetic factor is the amount of visible upper eyelid, known as tarsal show. The ideal amount of tarsal show has been defined by the ratio of visible eyelid as measured from the lashes to the palpebral fold, compared with the distance from the lashes to the eyebrow. Ideally, this ratio should be one third, at most one half, the distance to the eyebrow. The ratio is influenced by the position and shape of the eyebrow, the presence or absence of eyelid ptosis, the amount of excess upper eyelid skin, and the amount of protruding retroseptal fat, as well as the anatomic position and shape of the supraorbital rim.
With aging, the upper lid sulcus may age in two different ways. Some patients develop upper sulcus hollowing and increased tarsal show as orbital fat is lost and the supraorbital rim becomes more arched. This appearance often occurs in conjunction with a subtle degree eyelid ptosis. Conversely, the second, more classic form of eyelid aging is seen in patients who develop excess skin, redundant orbicularis, and protuberant orbital fat—all contributing to less visibility of the upper eyelid due to soft tissue hooding. This is the traditional indication for upper lid blepharoplasty, where upper eyelid skin, orbicularis muscle, and retroseptal fat are removed.
Skeletal anatomy
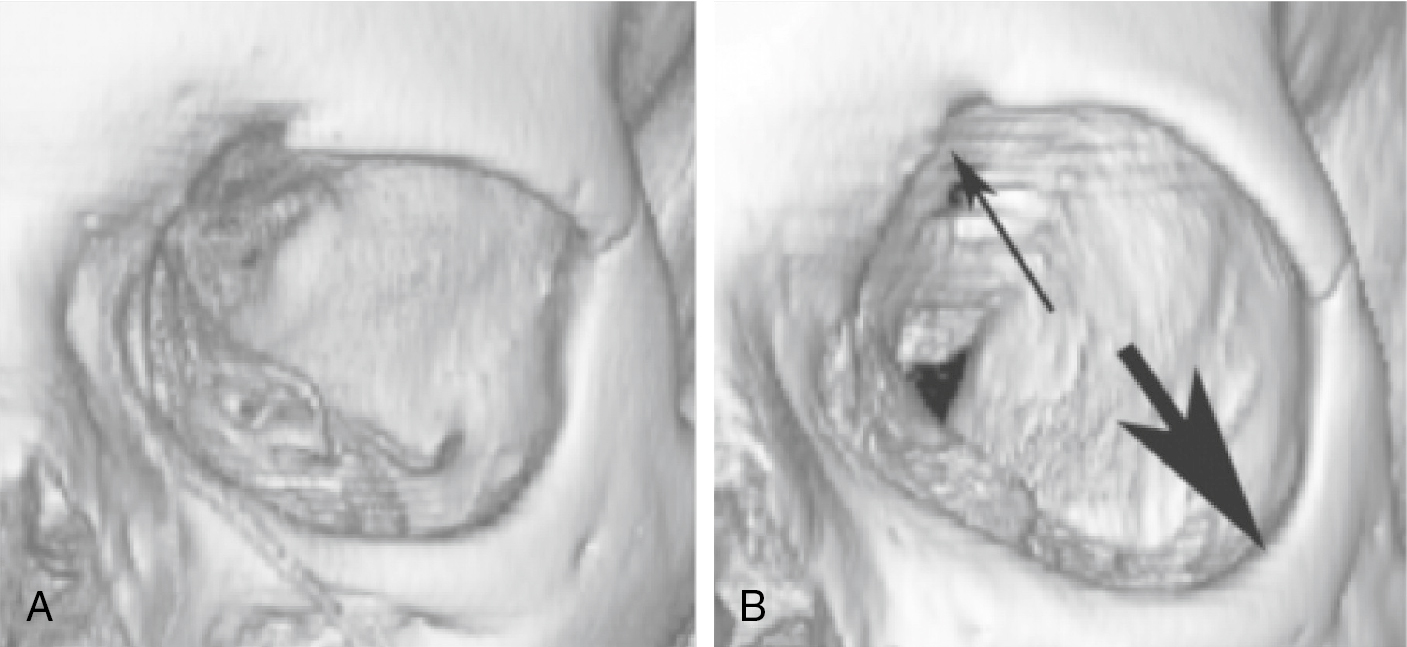
The supraorbital rim underlies the eyebrow and defines the upper limit of the orbit and upper lid sulcus. The septum orbitale attaches circumferentially around the orbit at the arcus marginalis and defines both the entry to the orbit and the retroseptal space. The supraorbital rim can be relatively low and flat (a masculine trait), or it may be arched, thus opening the upper lid sulcus. In a person with a low-lying transverse supraorbital rim, the upper lid sulcus will appear closed with minimal tarsal show, whereas the highly curved supraorbital rim creates a more open, hollow-looking upper lid sulcus with significantly more tarsal show. Rarely, in young people, a congenital arched supraorbital rim and upper sulcus hollowing may be a cause for concern. However, in the aging patient, there is a gradual enlargement of the orbit ( Fig. 38.3 A, B). This skeletal change, along with loss of upper sulcus fat, can lead to excessive openness and a hollow appearance in the upper sulcus, which will, in some patients, be a significant change from their youthful appearance. When combined with a congenital tendency for an arched supraorbital rim, this condition can be marked—an appearance sometimes referred to as “nursing home eyes.”
Surgical considerations
In the preoperative assessment of patients presenting for upper eyelid surgery, the shape of the orbital rim should also be assessed when the soft tissues are examined. The shape and position of the eyebrows should be considered as well. Patients with low-lying flat supraorbital rims and low-lying eyebrows are more likely to be candidates for a traditional excisional type upper lid blepharoplasty, without much fear of creating an overly resected, hollow upper sulcus. Conversely, the high-arching supraorbital rim with a concomitant hollow upper sulcus can be made excessively hollow with standard excisional surgery. Similarly, in the aging face where there has been orbital enlargement and the development of an arched supraorbital rim, the excisional approach to the upper eyelid should be limited or not done at all. Rather, the surgeon should consider rejuvenation methods to recreate the plump upper lid sulcus of youth. Reconstructive options will be aimed at lowering the visual appearance of the supraorbital rim to hide the hollow upper sulcus. Theoretically, bone grafts and custom implants could be used for this purpose, but with the refinement of fat-grafting techniques, this has become the preferred method in the aesthetic surgery setting. , Fat can be carefully infiltrated along the border of the supraorbital rim, placing it against the bone, anterior to the septum orbitale, creating the visual effect of a lower supraorbital rim with less visibility of the upper lid sulcus ( Fig. 38.4 ). Care must be taken to conservatively and carefully inject fat in this area to avoid visible lumps and to avoid intravascular injection of fat. Surgical strategies to improve the safety and efficacy of upper sulcus fat grafting are preinjection of the area with an epinephrine-containing local anesthetic to shrink blood vessels, use of a blunt injection cannula, use of low injection pressure, and avoidance of bolus injection by using a meticulous technique whereby the cannula is gently kept moving. In this way, upper sulcus reconstruction can be done in conjunction with other periocular procedures, such as blepharoplasty-style skin excision or brow lift.
Lower lid blepharoplasty
Aesthetics
The junction of the lower eyelid and the cheek is an area of important age-related changes that are often of concern to patients. In the lower eyelid itself, the orbital septum, which attaches to the orbital rim at the arcus marginalis, can attenuate, allowing orbital fat to bulge forward from the three lower eyelid fat compartments, creating the classic “bags under the eyes.” In the medial third of the infraorbital room, adjacent to the bulging fat above is the tear trough, also known as the nasojugal groove, which roughly follows the orbital rim. This is a surface contour depression that effectively sits between the bulging orbital fat above and the cheek soft tissue below; patients may perceive this depression as “dark circles” under their eyes. This groove gradually moves inferiorly with aging. If the tear trough extends laterally along the orbital rim, it is called the palpebromalar groove. Adjacent to the septal attachment, the orbicularis oculi muscle is attached directly to medial third of the infra orbital rim and is attached to the rest of the infra orbital rim via the orbicularis retaining ligament (also known as orbitomalar ligament ). As the anterior cheek ages, the soft tissue mass immediately inferior to the orbital rim becomes thinner and ptotic, thus accentuating the appearance of the tear trough. This change is due to atrophy of the deep fat compartments as well as ptosis of the superficial fat compartments. , Although the soft tissue changes predominate, there is also a significant contribution caused by age-related atrophy of the underlying bone.
Skeletal anatomy
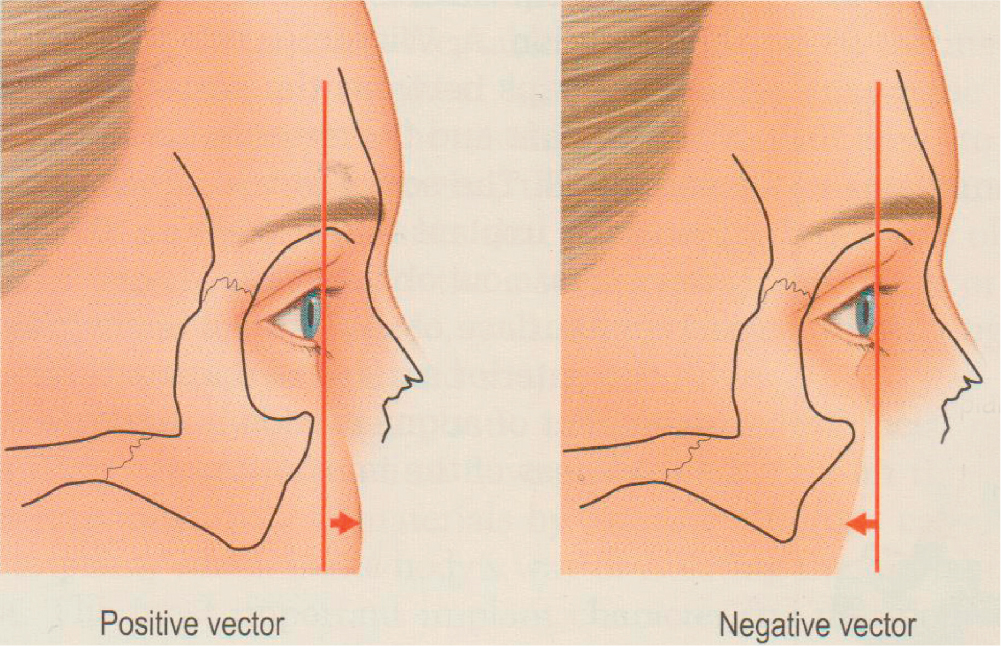
The infraorbital rim is the bony foundation of the lower eyelid–cheek junction and contributes to the support of the lower eyelid and the globe itself. Before aging becomes a factor, the relative prominence of the infraorbital rim to the globe has surgical implications. Projection of the soft tissue mass of the anterior cheek anterior to the globe was categorized by Jelks as a positive vector ( Fig. 38.5 ). This is normal. When the anterior cheek lies posterior to the globe, a negative vector is said to exist (see Fig. 38.5 ). If present in youth, the negative vector is caused by a congenitally deficient skeleton and typically leads to poor lower eyelid support with aging. A negative vector can also appear through the process of aging. Anatomic studies confirm the observation that with aging, posterior shift of the cheek soft tissue occurs, creating a negative vector in some patients. A major reason for this shift is the loss of underlying bone that occurs in certain areas of the aging facial skeleton (see Chapter 13 ). Areas prone to bony resorption include the anterior maxilla; the infraorbital rims, especially laterally; and the pyriform opening of the nose ( Fig. 38.6 ). An additional feature of the aging maxilla is the posterior inclination of the anterior maxillary face, which accentuates the process of cheek retrusion as soft tissue slides down the face of the maxilla in a retrograde manner. The resultant deficiencies in the skeleton contribute to loss of cheek volume and loss of support for the overlying soft tissue. In addition to retrusion of the anterior cheek, this leads to soft tissue descent and deepening of the tear trough.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree