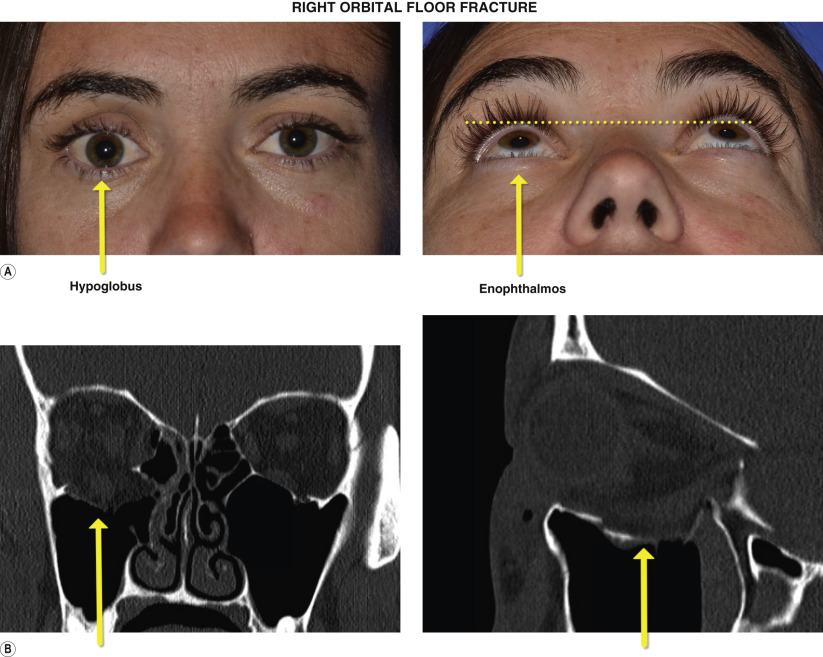
| Enophthalmos (>2 mm) |
| Extraocular muscle entrapment with diplopia |
| Hypoglobus |
| Oculocardiac reflex |
| Large floor fracture (>50%) |
| Exophthalmometry readings |
| Extraocular muscle movements and primary deviation |
| Measure globe dystopia |
| CT scan, axial and coronal views with thin cuts |
| Check infraorbital nerve sensation |
| Palpation for bony step off, trismus and signs of zygomaticomaxillary complex fracture (tripod) |
| Vital signs – heart rate, blood pressure; history of nausea/lightheadedness from oculocardiac reflex |
| Rule out globe injury; perform dilated fundoscopic exam |
Introduction
Bony and soft tissue injury can occur with any trauma to the orbit. The clinical presentation and treatment vary, based on the cause, findings, and symptoms. Fractures comprise the majority of bone injuries. Several types of fractures involve the orbit with blow-out fractures being the most common. Other fractures include zygomaticomaxillary complex (tripod) fractures, Le Fort fractures, and nasoethmoidal fractures. Orbital apex fractures involving the optic canal may result in optic neuropathy with vision loss.
Blow-out fractures occur when an object strikes the orbital entrance. Two theories are postulated: (1) the indirect hydraulic theory in which posterior pressure in the orbit causes a blow-out; and (2) the direct buckling theory in which direct pressure along the inferior orbital rim causes deformation along the floor. Symptoms may include diplopia from entrapment of the inferior rectus muscle, enophthalmos, infraorbital nerve hypesthesia, and hypoglobus. CT imaging with axial and coronal thin cuts is essential for diagnosis, treatment and decision making in fracture repair.
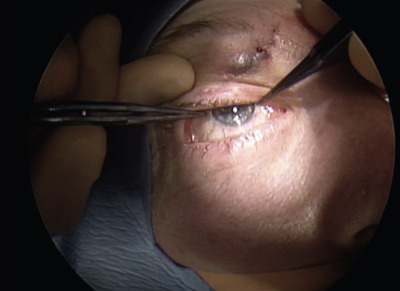
Urgent indications for fracture repair include the “white-eyed” blow out fracture in children where the fracture site incarcerates the rectus muscle causing possible ischemia, and the oculocardiac reflex resulting from muscle entrapment. Other indications vary but most surgeons will repair fractures within 2 weeks if one or more of the following criteria are met: diplopia within 30° of primary gaze associated with a positive forced duction test, clinically significant enophthalmos greater than 2 mm, and a fracture size greater than 50% of the orbital floor. Repair is typically via a transconjunctival approach with complete reduction of the orbital contents from the fracture site and placement of an alloplastic implant.
Tripod fractures can also be associated with orbital floor fractures but with a different mechanism. The zygoma is fractured along the fronto-zygomatic, zygomatic-maxillary, and zygomatic-temporal suture lines with possible soft tissue entrapment.
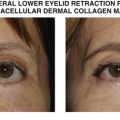
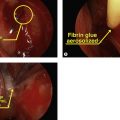
Our preference for implant choice depends on the location and amount of enophthalmos. For isolated orbital floor fractures, our preferred implants are thin porous polyethylene sheets or nylon foil. For fractures with significant enophthalmos, thicker barrier channel porous polyethylene is used. For combined medial and floor fractures, titanium-coated porous polyethylene is useful to precisely configure the implant to fit the desired shape. The use of bare titanium mesh or absorbable floor implants may increase risk of delayed orbital restriction.
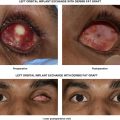
Complications include implant infection, extrusion, hemorrhage into the implant capsule, persistent hypesthesia of the infraorbital nerve, and eyelid malposition. Although excellent anatomic bony correction may be obtained, significant soft tissue injury may still be present. Residual enophthalmos, continued extraocular muscle imbalance, eyelid malposition, and traumatic ptosis all may necessitate additional surgery.
Surgical Technique

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree