• Orthognathic surgery should achieve a functional occlusion while optimizing facial form.
• Aesthetic facial analysis takes priority over cephalometric norms when developing the treatment plan.
• Treatment plans should be designed that will optimally support the soft tissue as the patient matures.
• Expansion of the facial skeleton optimizes soft tissue support.
• Skeletal contraction will prematurely age a person’s face.
• Skeletal disproportion can be aesthetically pleasing.
• Avoid net skeletal contraction in the treatment plan.
• Orthognathic surgery should be viewed as an aesthetic operation.
Introduction
The goals of facial skeletal aesthetic surgery are to achieve an aesthetic result with skeletal stability and optimal soft tissue support. Stability issues relate to establishing skeletal form that resists relapse, whereas aesthetic considerations focus on optimizing facial balance, facial proportion, and soft tissue support. The soft tissue will dictate the final aesthetic result; however, the underlying skeleton is the foundation on which the soft tissue drapes and therefore determines soft tissue support and contour. The success of many soft tissue rejuvenative procedures is limited by suboptimal skeletal support, and an appreciation of the importance of the underlying facial skeleton is critical to optimizing aesthetic results in all facial surgery.
Traditionally, aesthetic goals had to be weighed against skeletal stability. Rigid fixation has allowed surgeons to overcome stability problems and expand the aesthetic surgical options available to patients. Counterclockwise occlusal plane rotation, once considered heresy in orthognathic surgery, is now a common option to enhance facial aesthetics while achieving a class I occlusion in orthognathic surgery. Rigid fixation allows the surgeon to develop an optimal aesthetic treatment plan with less concern about relapse.
Patient evaluation
Historically, treatment planning goals have been largely based on normative data derived from both skeletal and soft tissue cephalometric analyses. The error in this approach is that normalcy is simply not synonymous with beauty. When we look at celebrities or models who are considered beautiful, many of them exhibit a facial proportion that deviates from the Greek ideal of facial proportion. In contrast, we are all aware of people who have well-proportioned facial form but would not be considered beautiful. One can begin to understand why this traditional treatment planning philosophy, which involves achieving a balance between aesthetics and stability and basing aesthetic decisions on normative cephalometric data, was significantly flawed. Treatment objectives should not be based on normal values, but on aesthetically ideal dimensions. Several studies have examined the dimensional relationships in aesthetically pleasing faces among both men and women and compared them with those of normative populations. The anthropomorphic values of beauty differ from those of the average population.
The patient shown in Fig. 16.1 is a good example to explain this philosophy. The patient was an 18 year old who presented for surgical correction of a class III malocclusion. To correct her malocclusion, a 4-mm maxillary advancement would be the only procedure necessary. However, if we evaluated the facial form with careful consideration of the soft tissues, we would see that her face had a rather flat profile. Although only advancing the maxilla would correct her malocclusion and achieve modest improvement of her appearance, the extent of the improvement would be suboptimal. If we made a treatment plan with the intent of correcting the occlusion and the facial form, we could consider double-jaw surgery, eliminating the constraints that the malocclusion places on the aesthetic result. This patient’s treatment plan included a 10-mm advancement of the maxilla, a 6-mm advancement of the mandible to achieve a class I occlusion, and a 5-mm lengthening genioplasty. This approach provided for an aesthetic result in both the frontal and profile views, which could not have been achieved with single-jaw surgery. In addition to the patient having an optimized facial form immediately postoperatively, she now has improved soft tissue skeletal support that will continue to benefit her appearance as she continues to age. Thus the occlusal result is the same whether single- or double-jaw surgery is undertaken. For the purposes of this discussion, the occlusal result is considered to have served as a means to an aesthetic end rather than as an end in and of itself. In summary, orthognathic surgery should be considered an operation that corrects malocclusion while achieving the optimal aesthetic result as well. As virtual surgical planning simplifies treatment planning, and further research enhances our understanding of the three-dimensional soft tissue response to surgery, the aesthetic results of orthognathic surgery will continue to improve.
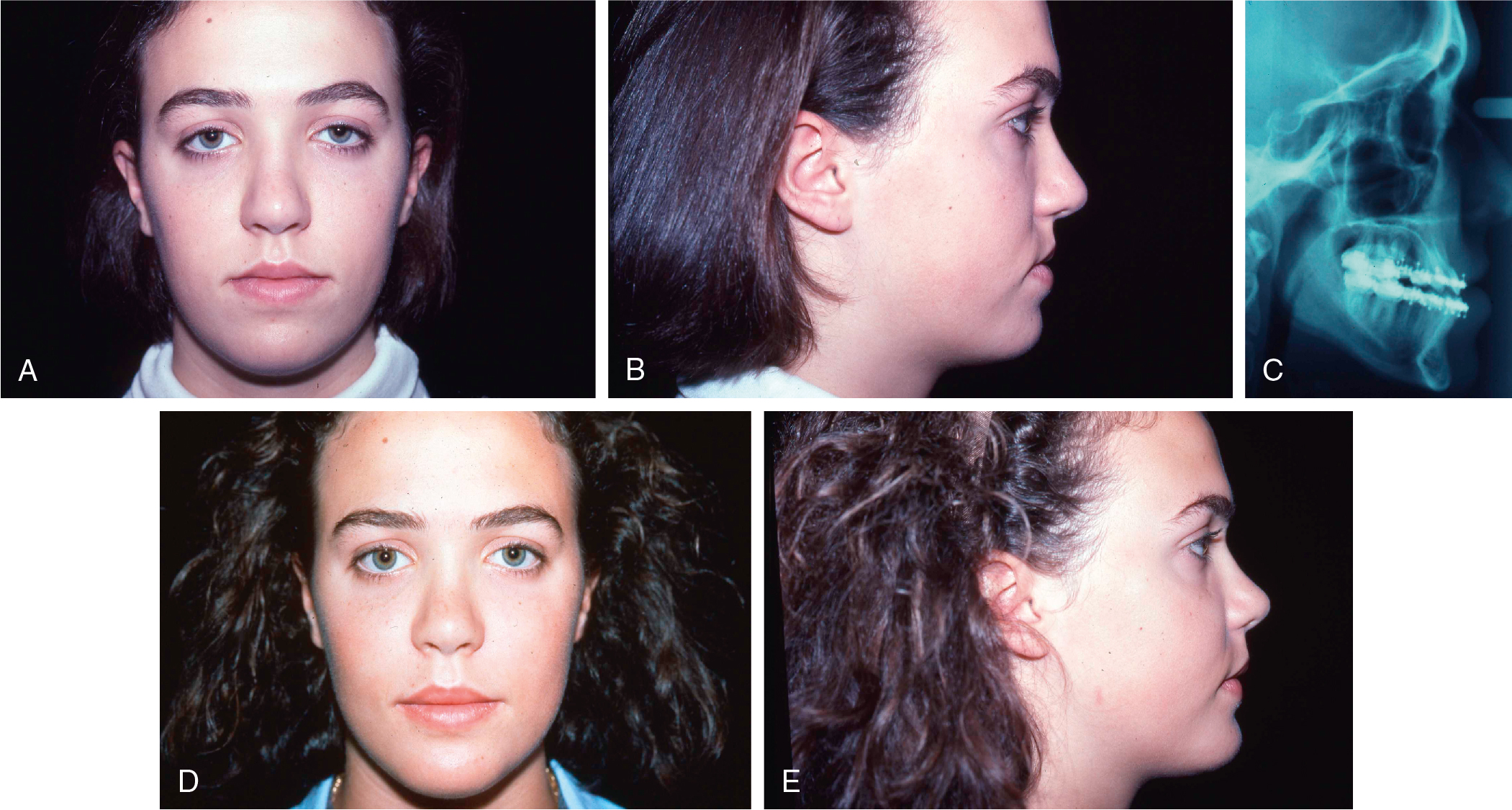
If this is the treatment planning philosophy that one is willing to pursue, it then makes little sense to rely on skeletal diagnoses to make treatment plans for patients. It must be remembered that skeletal diagnoses are derived from skeletal cephalometric data that are compared with normative data derived from “normal” individuals, not necessarily individuals who are considered beautiful or attractive. It bears repeating that normalcy is not necessarily synonymous with beauty. In addition, skeletal cephalometric data are limited to the midsagittal plane and give us no information regarding soft tissues.
An example of the deficiencies of treatment planning based on skeletal cephalometric data is seen in Fig. 16.2 . This patient was referred with a clinical diagnosis of mandibular prognathism supported by an excessive sella–nasion–B point (SNB) and normal sella–nasion–A point (SNA) angle. Despite these data, this patient would receive a suboptimal result if his treatment plan was limited to posterior positioning of the mandible. Although an isolated mandibular setback would correct the occlusion, it would have an adverse aesthetic effect on the soft tissue of his neck and do nothing to correct his poor cheek projection. Instead, the maxilla was advanced and vertically elongated to achieve greater exposure of the anterior maxillary teeth. The perceived large mandible was camouflaged by a setback genioplasty. The occlusal result would have been the same regardless of the treatment planning approach, but by basing the treatment plan on the patient’s observed three-dimensional facial form, a superior aesthetic result was obtained over that which would have been achieved by using solely cephalometric data. Although soft tissue cephalometric data are more clinically relevant than skeletal data, the use of soft tissue cephalometric landmarks is limited by the fact that it is a two-dimensional representation of three-dimensional facial form.
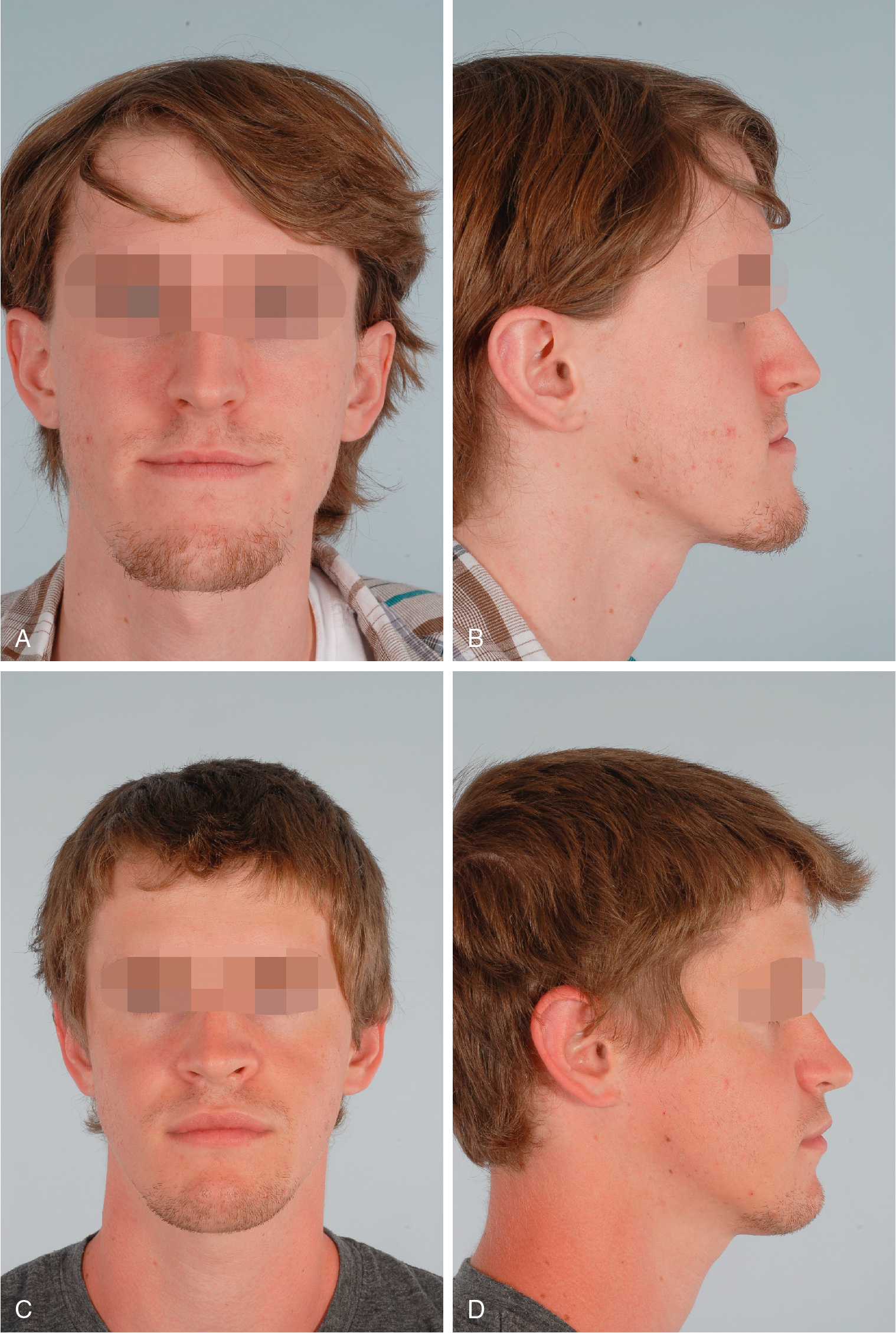
Alternatively, the best possible approach to aesthetic treatment planning relies on a thorough description of the facial morphology of the patient through the most basic of all clinical modalities, the physical examination. This is meant to be a “qualitative” assessment of how one can best alter the facial morphology to the maximum aesthetic benefit of the patient. Most important, this qualitative assessment must take into account the very dynamic interrelationship between the underlying skeletal foundation and the overlying soft tissues. It is important to realize how one can affect the appearance of the other and incorporate this principle into the treatment plan. A thorough physical examination is the first step in this process.
Facial analysis
Facial analysis begins with the frontal facial evaluation. The vertical facial thirds should have approximate symmetry and are divided into the following thirds: trichion to glabella, glabella to subnasale, and subnasale to pogonion. In many attractive faces, the lower facial third is slightly longer than the upper and middle thirds.
When the lower third of the face appears abnormal, the surgeon must determine whether the problem occurs in the maxilla, the mandible, the chin, or all three. Proper vertical position of the maxilla is determined by evaluating the amount of anterior upper incisal visibility with the lips in repose. Historically, this value was 3 to 5 mm; however, by prioritizing aesthetic over “normal” appearance, surgeons now accept 4- to 7-mm incisal show to create a face that projects youth and vitality. This determination is much more important than the extent of gingival show with full smiling because the latter also involves the dynamics of the individual smile in addition to structural considerations. The occlusal plane angle may also contribute to the height of the lower facial third. A steep occlusal plane angle is associated with a longer lower face, and in contrast, a shallow occlusal angle plane is associated with a short lower face. Rigid fixation allows surgeons to modify the occlusal plane angle with predictability and stability, giving the surgeon more control over facial aesthetics. Finally, the chin contributes to the lower facial height. An obtuse labiomental angle is commonly associated with a vertically long chin, and an acute labiomental angle is associated with a vertically shorter chin.
Facial asymmetry is universal when the surgeon carefully evaluates facial form. Symmetry is evaluated in the forehead, the orbits, the cheeks, the nose, the mandible, and the chin. Any abnormalities that are notably unaesthetic or cause concern in the patient are noted. Additionally, it is important to evaluate the presence of an occlusal cant. Commonly noted issues of asymmetry are chin point deviation, mandibular border asymmetry, and occlusal cant.
The soft tissues of the face are evaluated in the frontal view as well. Soft tissue regions that have an impact on facial aesthetics are the nasolabial creases, malar cheek pads, marionette lines, jowls, and submental neck tissue. These are common areas for which patients seek dermal fillers to reverse the signs of aging. Skeletal procedures, such as alloplastic implants, orthognathic surgery, or a genioplasty, will have a profound impact on these soft tissue regions and, thus, offer the surgeon an opportunity to enhance the patient’s facial aesthetic form immediately and into the future as the patient matures.
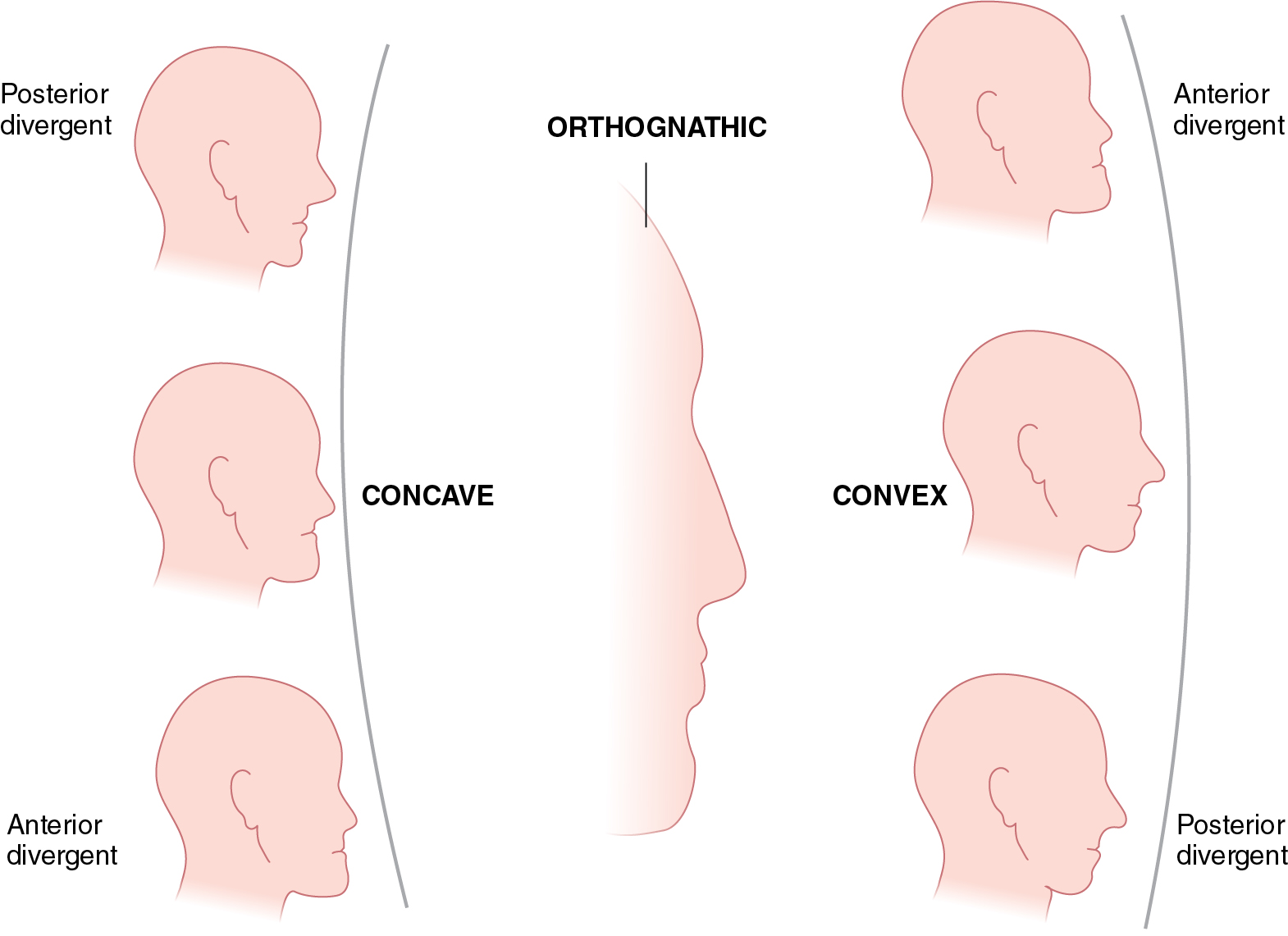
In the lateral view, an assessment is made of the projection of the zygoma, maxilla, mandible, and chin. The soft tissues are evaluated as well: labiomental crease angle, nasolabial crease depth, malar cheek pad projection, and presence of marionette liens, or jowls. The face is also evaluated to assess for facial divergence and facial convexity or concavity ( Fig. 16.3 ). Facial divergence is determined by the sagittal position of the soft tissue pogonion relative to a vertical line dropped from the glabella. If the pogonion appears to be posterior to this line, the face diverges posteriorly. If it appears to be anterior to this line, the face diverges anteriorly. Overall, facial convexity or concavity is a description of the profile by a line connecting the glabella to the subnasale to the pogonion. These points may subtend a line that is straight or one that is convex or concave. , An additional, and perhaps more important, consideration is the description of the parasagittal profile—that is, what are the sagittal relationships of the soft tissues from the infraorbital area to the paranasal area to the parasymphyseal area, and does this provide one with a general impression of a convex or concave appearance? A profile that is straight with neutral divergence is described as an orthognathic profile. The most aesthetic profiles are convex both in the midsagittal and parasagittal planes.