Eye involvement in inherited epidermolysis bullosa (EB) can occur as a spectrum of symptoms and signs. This article describes these signs and symptoms. It also offers options for treatment.
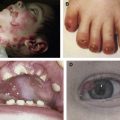
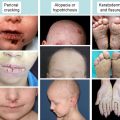
Eye involvement in inherited epidermolysis bullosa (EB) can occur as a spectrum of symptoms and signs, ranging from mild conjunctival irritation to severe cicatrisation of the eyelids, cornea, and the conjunctiva as reviewed in published case reports and case series. The ocular surface formed by the conjunctiva and the cornea and covered by the protective eyelids is derived embryonically from the surface ectoderm like the skin. There are various biochemical and ultrastructural similarities common to the skin and cornea, particularly the plasma membrane and the epidermal–dermal basement membrane zone of the two stratified epithelia. Careful ophthalmologic examination should become an integral part of the management of all patients with inherited EB. Ocular and adnexal abnormalities may be acute or chronic, symptomatic or asymptomatic, and they can be of variable clinical severity. Ocular involvement in EB can occur at any age (even as early as 1 month of age). Common ocular symptoms and signs in EB described are red watery eyes, photophobia, ocular pain, conjunctival injection, conjunctival edema, blepharoconjunctivitis, exposure keratopathy, corneal erosions, or abrasions. Ophthalmologists have a major role in the multidisciplinary approach in treating EB by preventing and controlling complications that occur in the eye.
Summary of reports and studies reporting on the frequency of ocular involvement
Common ocular involvement described in inherited EB includes corneal abrasions, corneal scars, corneal pannus, eyelid blisters or ectropion, conjunctival blisters, and symblephara. Other ocular associations reported in EB include cataracts, cornea plana, sclerocornea, refractive errors, amblyopia, lacrimal duct obstruction, strabismus, lens subluxation, posterior vitreous detachment.
The first publication report of ocular involvement in inherited EB was in 1904. Later, there were limited case reports and case series suggesting that various forms of involvement of the ocular surface and its adnexa can occur in some subtypes of inherited EB. Very few large series of EB patients have been studied. One of the largest involved 181 consecutive patients who were seen and given full ophthalmologic examination at London’s Great Ormond Street Children’s Hospital from 1980 to 1996. The overall frequency of ocular complications was 12%, 40%, 4%, and 51% in their children with EBs, junctional epidermolysis bullosa (JEB), dominant dystrophic EB (DDEB), and recessive dystrophic EB (RDEB), respectively. The only finding seen in a single patient with DDEB was conjunctival blistering. The only findings in EBs were present in those having the usually clinically severe Dowling-Meara subtype. Of these, 12% had peripheral corneal vascularization; eyelid blistering and corneal abrasions also were noted. In contrast, 14% of RDEB patients had a history of recurrent ocular erosions; 68% had some type of corneal complication (eg, abrasions, scarring, or pannus formation). Eight percent had exposure keratitis with ectropions of both upper and lower lids; 24% had conjunctival involvement, and 14% had eyelid blisters. The most common findings in their JEB patients were corneal scarring (20%) and exposure keratopathy (33%). Miscellaneous ocular findings in rare patients included amblyopia, squints, lacrimal punctal occlusion, punctal papilloma of the eyelid, subconjunctival hemorrhage, pseudopterygia, microophthalmos, and anterior polar cataract with astigmatism. Lin and colleagues reported findings in 204 patients with EB seen at Rockefeller University (New York) from 1986 to 1993. Findings were similar in type and frequency to those reported by Tong and associates. Gans reported the findings in 78 EB patients studied in nonlongitudinal fashion at Washington University (St Louis) from 1979 to 1986. The most common finding was the presence of corneal erosions in 55.5% of patients with junctional epidermolysis bullosa-Herlitz type (JEB-H) and 52.9% of patients with RDEB. About 25% of the RDEB patients had evidence of corneal scarring; blepharitis and eyelid blistering each occurred in about 20% of patients.
Before the reports of the National EB Registry (NEBR) database, the case series reported and published indicated the frequencies of ocular involvement in inherited EB as depicted in Table 1 .
| Form of EB | Study | Study | Study |
|---|---|---|---|
| Gans et al 1988 | Lin et al 1994 | Tong et al 1999 | |
| Simplex EB | Ocular involvement Weber Cockayne 8%, Dowling Meara 22%, Koebner 0% | Ocular involvement 3% | Ocular involvement 12% |
| Weber Cockayne (localized) 8% blepharitis Dowling-Meara 22% corneal scarring; 11% had eyelid blistering | No description of type 3% | Dowling subtype – 12% peripheral corneal vascularization | |
| Junctional EB | 55% | 39% | 40% |
| 55% corneal erosions, 22% corneal scarring, 11% blepharitis, 22% eyelid blistering | 39% | 20% corneal involvement; no eyelid or conjunctival involvement | |
| Recessive dystrophic EB | 52% | 51% | 51% |
| 52% corneal erosions 26% corneal scarring 20% eyelid blistering 20% blepharitis. | No description 51% | 68% cornea involved 35% corneal scarring 24% corneal pannus 8% exposure keratitis, eyelid scarring 24% conjunctival involvement 14% eyelid involvement | |
| Dominant dystrophic EB | 10% | 17.6% | 4% |
| 10% corneal erosions | No description 51% | 4% conjunctival blistering |
The 3280 consecutively enrolled patients in the NEBR comprise the largest cohort of EB patients ever assembled in the world and reflect up to 16 years of methodical clinical follow-up. Although the primary study was a cross-sectional one, most patients had some longitudinal data collection also. About one eighth of the entire study population also was selected randomly for formal prospective evaluation every 2 years. The only significant longitudinal data reported of ocular involvement in inherited EB have been the data that are extrapolated from the NEBR, an epidemiologic project established in 1986 by the National Institutes of Health (NIH). This registry contains both cross-sectional and longitudinal data of 3280 EB patients that are aimed at determining the risk of selected extracutaneous affection in inherited EB. The demographics of the study population included in the database closely resembled the general American population. The data reported by the NEBR database were significant, as the distribution of patients defined by major EB types and subtypes were observed to closely mimic data of reported cohorts of EB patients elsewhere in the world. Therefore, the NEBR data results are applicable to EB patients universally. Fine and colleagues were able to perform a rigorous analysis of the NEBR’s database, thereby enabling them to precisely measure the impact of ocular disease, by accurately estimating cumulative lifetime risk of corneal blistering, erosion, and scarring, for each of the major types and subtypes of inherited EB ( Table 2 ).
| Tissue Involved | Recessive DEB | Dominant DEB | JEB | EBs |
|---|---|---|---|---|
| Eyelid | Bullae, ulcers, crusted lesions, cicatrisation Blepharitis–8.9% Ectropion–1.4% Lacrimal duct obstruction–5.7% | Bullae, ulcers, crusted lesions, cicatrisation Blepharitis–0.4% Ectropion–0.4% Lacrimal duct obstruction–nil | Not frequent involvement Blepharitis–3.0% Ectropion–4.2% Lacrimal duct obstruction–3.6% | Occasional involvement Blepharitis–0.3% Ectropion–nil Lacrimal duct obstruction–1.3% |
| Conjunctiva | Conjunctivitis, keratoconjunctivitis, cicatrisation Symblepharon–3.6% | Conjunctivitis, keratoconjunctivitis, cicatrisation Symblepharon–nil | Not frequent involvement Symblepharon–1.2% | Occasional involvement Symblepharon–nil |
| Cornea | Keratitis, ulcers, opacities, perforation, pitting Corneal erosion–31.9% scarring–18.2% | Keratitis, ulcers, opacities, perforation, pitting Corneal erosion–0.4% scarring–0.4% | Keratitis, ulcers, opacities, perforation, pitting Corneal erosion–19.9% scarring–8.4% | Keratitis, ulcers, opacities, perforation, pitting Corneal erosion–0.9% scarring–0.2% |
| Lens | Involved | |||
| Retina | Occasionally retinal detachment, cysts, pigmentary changes. |
The distribution of patients by major EB type and subtype also was shown to closely mimic that seen within much smaller cohorts of EB patients elsewhere in the world, suggesting that these data are applicable to EB patients everywhere. Rigorous analysis of the NEBR registry’s database has allowed for more precise measurement of the impact of ocular disease, to include accurate estimation of the cumulative lifetime risk of corneal blistering, erosion, and scarring, for each of the major types and subtypes of inherited EB. The NEBR registry reported the ocular abnormalities secondary to EB as described in Table 3 .
| EB Simplex | Junctional EB | Dystrophic EB | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Weber-Cockayne | Dowling-Meara | Koebner | EBS-O | Herlitz | Non-Herlitz | DDEB | RDEB-HS | RDEB-nHS | RDEB Inversa | |
| Ocular abnormalities (case numbers) | 1092 | 113 | 96 | 379 | 40 | 190 | 424 | 139 | 265 | 17 |
| Corneal erosions or | 0.92 | 6.19 | 3.13 | 2.64 | 47.50 | 25.26 | 2.12 | 74.10 | 32.45 | 35.29 |
| blisters | ||||||||||
| Corneal scarring | 0.27 | 0.00 | 3.16 | 0.53 | 26.83 | 13.37 | 0.95 | 50.00 | 16.92 | 29.41 |
| Symblepharon | 0.00 | 0.00 | 0.00 | 0.00 | 4.76 | 2.11 | 0.00 | 10.07 | 1.89 | 11.76 |
| Blepharitis | 0.37 | 0.88 | 2.08 | 0.26 | 7.14 | 6.32 | 0.71 | 17.52 | 6.46 | 17.65 |
| Ectropion | 0.00 | 0.00 | 0.00 | 0.00 | 14.29 | 2.11 | 0.00 | 7.19 | 1.90 | 0.00 |
| Lacrimal duct obstruction | 1.19 | 2.65 | 1.04 | 1.85 | 2.38 | 4.23 | 1.65 | 5.80 | 5.30 | 11.76 |
| Impaired vision | 13.17 | 13.27 | 15.63 | 16.14 | 16.67 | 13.68 | 17.18 | 38.13 | 21.89 | 41.18 |
| Blindness | 0.82 | 1.77 | 0.00 | 0.53 | 0.00 | 1.58 | 0.94 | 6.47 | 1.14 | 0.00 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree