Epidermolysis bullosa (EB) nevi are large, eruptive, asymmetrical, often irregularly pigmented melanocytic lesions. Such nevi may give rise to small satellite nevi surrounding the primary nevus, and thus frequently manifest clinical features suggestive of melanoma. They usually arise in sites of previous bullae or erosions. At least twice a year all persisting wounds and EB nevi should be evaluated with a low threshold for histopathologic examination if warranted. Our practice is to punch biopsy EB nevi showing dermoscopic features of concern as well as dermoscopically featureless lesions. Given the skin fragility and potentially impaired wound healing in EB patients, we avoid prophylactic total excision of large EB nevi, but rather use the dermoscope to select appropriate sites for punch biopsies within giant EB nevi.
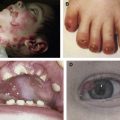
Epidermolysis bullosa nevi (EB nevi) are large, eruptive, asymmetrical, often irregularly pigmented melanocytic lesions ( Boxes 1 and 2 ). Such nevi may give rise to small satellite nevi surrounding the primary nevus, and thus frequently manifest clinical features suggestive of melanoma ( Fig. 1 ). They usually arise in sites of previous bullae or erosions ( Fig. 2 ). The nevi were initially reported in generalized atrophic benign EB (now classified as non-Herlitz junctional EB). Today it is well accepted that the occurrence of EB nevi is a frequent phenomenon in patients suffering from all variants of EB, which, however, are apparently only recessively inherited.
Asymmetric architecture of the lesion
Nests of melanocytes of different sizes and shapes along the dermoepidermal junction
Melanocytes in lower epidermal layers or scattered single melanocytes (“spreading”) in upper epidermal layers
Moderate (to severe) nuclear atypia
Dermal fibroplasia
Fibrosis and scarring with thickened collagen bundles
Dermal lymphocytic infiltrate with melanophages
From Bauer JW, Schaeppi H, Kaserer C, et al. Large melanocytic nevi in hereditary epidermolysis bullosa. J Am Acad Dermatol 2001;44(4):577–84.
Pattern analysis criteria
Multifocal hypo- or hyperpigmentation (17 of 23)
Multicomponent pattern (20 of 23) ( Fig. 4 )
Atypical pigment network with irregular meshes and thick lines (17 of 23) (see Fig. 4 )
Irregular dots and globules of different size (16 of 23) (see Fig. 4 )
Homogeneous areas (23 of 23) (see Fig. 4 )
Vascular pattern
Milky red areas (5 of 23)
Comma vessels (2 of 23)
“Glomerular clumps” (5 of 23)
Atypical vascular pattern (ie, linear, dotted, globular red) (2 of 23)
ABCD rule of dermoscopy criteria (asymmetry, border irregularity, color variegation, and diameter larger than 6 mm)
Structural asymmetry in two axes (23 of 23)
Abrupt border cut-off (3 of 23)
The colors white (23 of 23), light brown (23 of 23), dark brown (13 of 23), blue-gray (12 of 23), and red (11 of 23) dominated, while black and blue were almost absent.
From Lanschuetzer CM, Emberger M, Laimer M, et al. Epidermolysis bullosa naevi reveal a distinctive dermoscopic pattern. Br J Dermatol 2005;153(1):97–102.
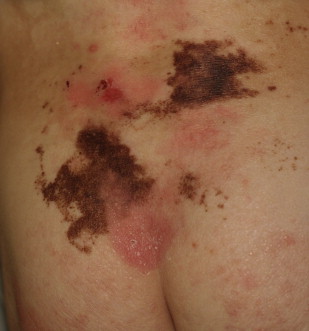
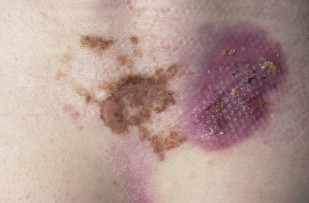
Two pathogenic theories about the development of EB nevi have been proposed. According to one theory, the repetitive disruption of the basement membrane primes local nevus cell nests or single melanocytes to break senescence and undergo proliferation. According to the second theory, viable melanocytes/nevus cells, probably deriving from incipient nevi or subclinical nests of nevus cells, free-float in the fluid-filled cavity of an EB blister and, after settling down at random (often at the edge of the blister), proliferate excessively in the microenvironment of epidermal regeneration. We detected such “flocking-bird” melanocytes histologically in the blister cavity (produced by the biopsy trauma) in a histologic section of an EB nevus of a patient with junctional EB. Furthermore, we found melanocytic cells in a cytospin specimen prepared from a blister located on top of a large EB nevus. We detected in addition cytokines and growth factors, such as hepatocyte growth factor, interleukin 8, granulocyte-macrophage colony-stimulating factor, prostaglandin E2, and leukotriene B4 in such fluid, which might potentiate melanocytic proliferation. Interestingly, eruptive nevi have been reported to develop following various other bullous diseases as well.
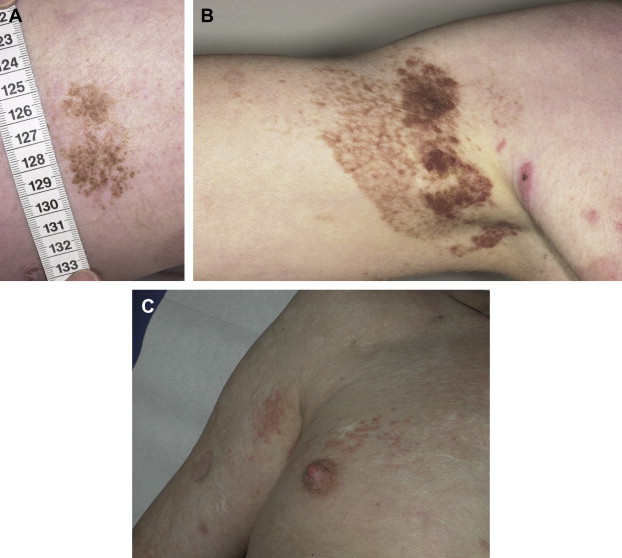
EB nevi mature as most common acquired melanocytic nevi: They begin as flat, pigmented lesions, and later, while acquiring dermal components, lose their pigment. More precisely, EB nevi gradually appear in infancy or adolescence as stippled maculae, and over years develop papular areas resulting in dermal shagreen-nevi (see Fig. 2 , Fig. 3 ).

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree