div class=”ChapterContextInformation”>
65. Treatment of Male Stress Urinary Incontinence: Artificial Urinary Sphincter
Keywords
Urinary incontinenceMaleArtificial urinary sphincterUrethral slingRevisionOutcome65.1 Introduction
Stress urinary incontinence (SUI) is defined by the International Continence Society as the complaint of involuntary leakage on effort or exertion, or on sneezing or coughing [1]. Any surgical or radiotherapeutic manipulation of the external urinary sphincter may result in SUI, with radical prostatectomy (RP), transurethral resection of the prostate (TURP), and radiation therapy accounting for the majority of iatrogenic etiologies [2].
Primary surgical management of men with persistent, bothersome stress urinary incontinence (SUI) either with urethral sling placement or artificial urinary sphincter (AUS) placement, is typically highly successful [3, 4]. However, as with most surgical procedures, appropriate patient selection and counseling are a crucial component to obtaining excellent outcomes. Here, we review the preoperative considerations, operative technique, postoperative outcomes, and complications for artificial urinary sphincter placement.
65.1.1 Background and Design
Originally introduced in 1974, the AUS is the most efficacious option in the surgical management of severe male stress urinary incontinence [5]. In the United States, AUS implantations represent approximately 12% of anti-incontinence procedures performed for men with urinary incontinence [6]. This may be secondary to risks of the procedure and/or patient preferences regarding implanting a mechanical device [7].
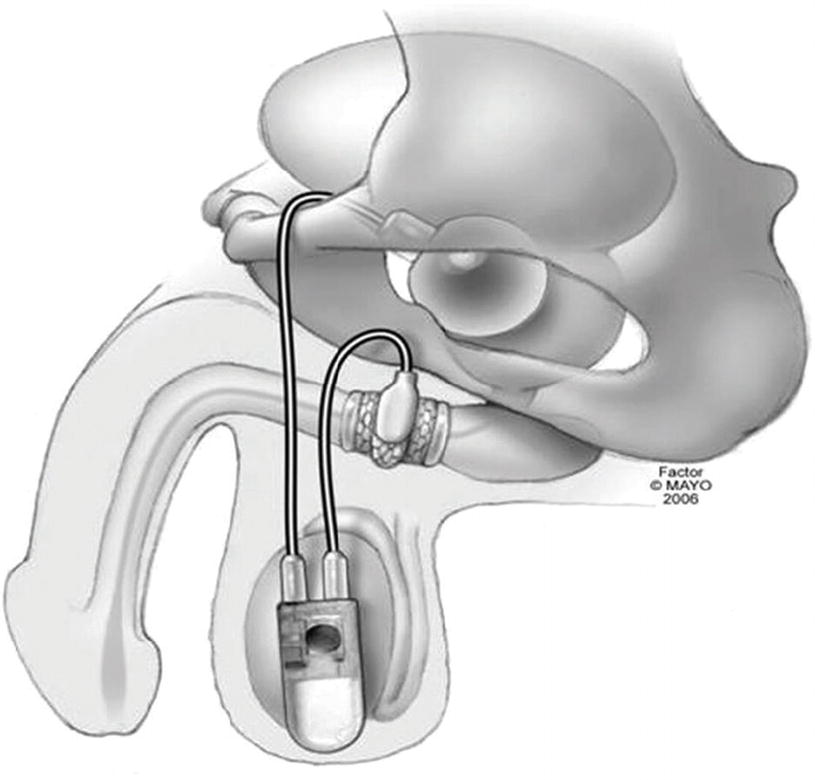
Representative illustration of an artificial urinary sphincter including: urethral cuff, abdominal reservoir, and scrotal pump
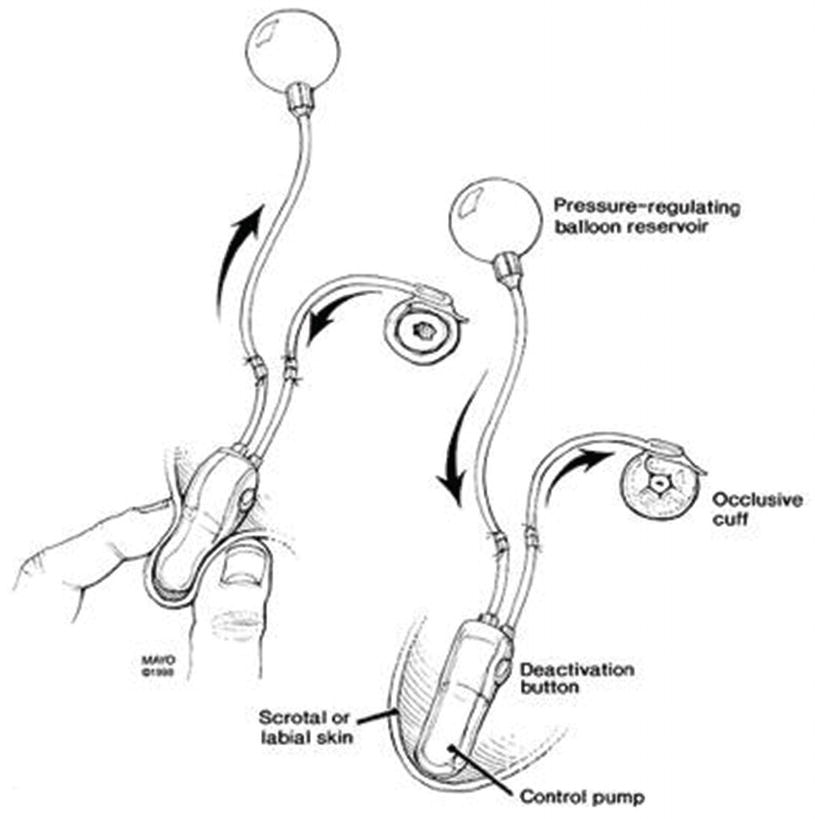
Representative demonstration of artificial urinary sphincter pump cycling
65.2 Clinical Evaluation
Males presenting with bothersome stress urinary incontinence should undergo a history and physical examination with attention paid to the duration of time from any surgical or radiotherapeutic manipulation of the external urinary sphincter, noting any change or improvement in continence over time. Also worth noting are stress versus urge incontinence symptoms, a history of underlying urologic pathology (e.g. urethral stricture, urothelial malignancies, prior urolithiasis, etc.), a history of hematuria or urinary tract infections, and any prior genitourinary treatments (including pelvic radiation). Notably, a consensus panel on AUS implantation advocated for a waiting time of 6 months following surgery in cases of severe (i.e. gravitational) incontinence that are not improving with conservative management [9]. They noted that if the patient’s incontinence is progressively improving, even at 12 months, surgical therapy can be delayed at the surgeon’s discretion [9]. Additional further evaluations of the patient’s degree of incontinence (e.g. pad weight, validated questionnaires, etc.) may be employed per the discretion of the treating physician.
With regard to potential artificial urinary sphincter placement, specific attention during the physical exam should be focused on the patient’s capacity to potentially manipulate the device. In elderly patients, acceptable AUS success rates have been reported provided that they have the mental and physical capacity to justify device placement [10, 11].
65.2.1 Additional Testing
The extent of additional testing may depend on which treatment for incontinence the patient wishes to pursue. In all patients, we perform a urinalysis and noninvasive uroflow test with post void residual to assess for active urinary tract infection and incomplete bladder emptying. Likewise, we typically perform cystoscopy to evaluate for urethral stricture, vesico-urethral anastomotic stenosis, or other urothelial pathology. Further testing including imaging (e.g., history of nephrolithiasis, urothelial carcinoma, hematuria), urine cytology (e.g., irritative lower urinary tract symptoms, history of urothelial carcinoma), and PSA may be obtained as clinically indicated. While we do not routinely perform complete multichannel urodynamic studies in those interested in AUS placement, these are used in cases with suspicion of altered bladder compliance (e.g. prior radiation, neurologic disease, etc.) or urge-predominate mixed urinary incontinence . By comparison, urodynamic evaluation, including an evaluation of detrusor contractility, may be more useful in those interested in compressive urethral sling placement.
Patients with prior histories of urothelial carcinoma, urethral stricture disease, and anastomotic stenosis among others, should demonstrate a sufficient period of disease stability prior to consideration of AUS placement to reduce the risk of erosions resulting from subsequent repeated cystoscopic interventions.
65.2.2 Urethral Sling Versus AUS
Depending on the results of the preoperative evaluation, patients can consider treatment with a urethral sling or AUS . The decision regarding which procedure to perform in males presenting with stress urinary incontinence is based on several factors, including patient preferences [7]. Notably, for optimal outcomes with male urethral sling placement, patient selection is crucial. In that regard, several factors have been associated with increased rates of persistent stress urinary incontinence following sling placement including pad weight greater than 450 grams per day, previous pelvic radiation therapy, and a low detrusor leak point pressure [12]. For these patients, or those who have failed a prior urethral sling, AUS placement may achieve greater continence when patient capability and preferences permit.
65.3 Operative Technique
65.3.1 Approach and Preparation
In terms of the surgical technique for AUS placement in males, we prefer to use a perineal approach, with patients in the dorsolithotomy position and placement of the urethral cuff around the proximal bulbar urethra. Penoscrotal techniques for AUS implantation have been described, but in our experience these tend to lead to more distal cuff placement and subsequent revisions. In fact, a multicenter study found that there is a higher completely dry rate, with fewer subsequent revision surgeries, with a perineal approach than with a penoscrotal approach [13].
For the surgery, the skin is prepped with Chlorhexidine , as this has been associated with lower device infection rates than a povidone-iodine preparation [14]. Intravenous antibiotics are administered within 60 minutes prior to incision; we prefer the use of vancomycin and an aminoglycoside. Draping is performed based on a “no-touch” technique using Ioban, as described in the penile prosthesis literature [15]. We then place a 12 Fr urethral Foley catheter to drain the bladder and proceed with the perineal dissection.
65.3.2 Cuff Placement
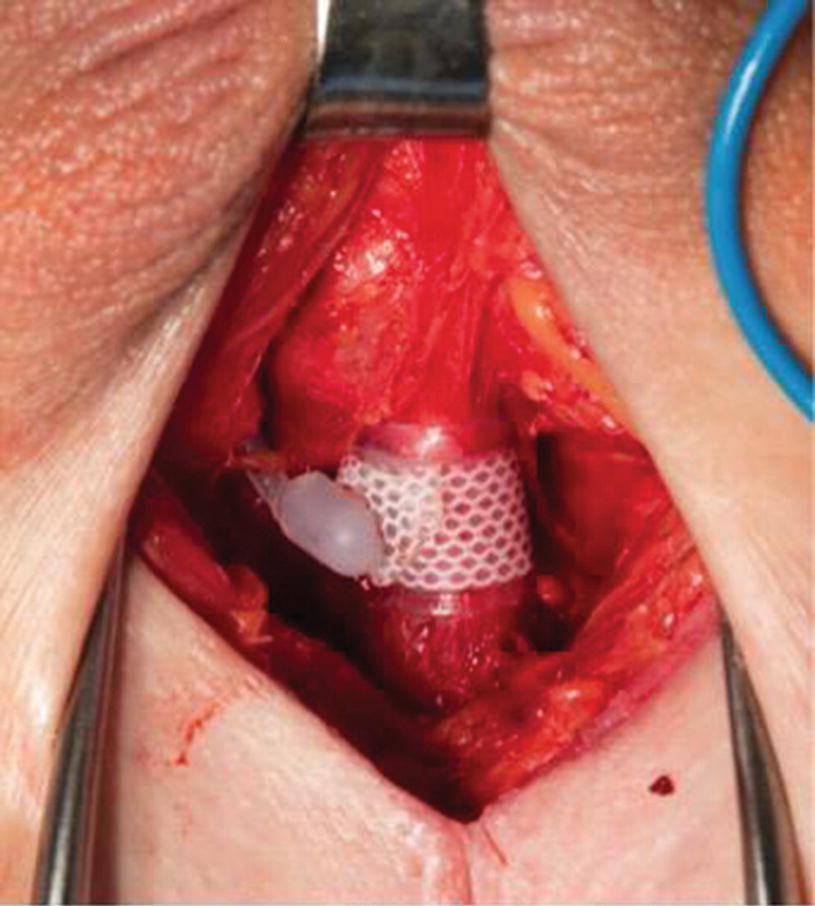
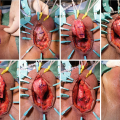
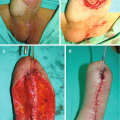
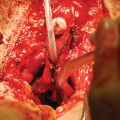
Intraoperative photo demonstrating the perineal dissection and placement of the urethral cuff at the proximal bulbar urethra
65.3.3 Reservoir and Pump Placement
Following completion of the urethral dissection, attention is turned to placing the abdominal reservoir and scrotal pump. We use a separate abdominal incision for ectopic submuscular/preperitoneal placement of a 61–70 cm abdominal reservoir. The reservoir can be filled with either normal saline or iso-osmotic contrast. In our practice, 22 cc of iso-osmotic contrast, a water/contrast mix of 48 ml iohexol (Omnipaque 350) and 60 ml sterile water, is instilled in the reservoir at the time of placement to assist with identification of mechanical failure during future evaluations if they are needed for recurrent stress incontinence [20]. The scrotal pump is placed in the anterior scrotum on the side of the patient’s dominant hand (and the same side as the tubing of the other components), in an effort to avoid difficulty with pump manipulation. A clamp is passed from the abdominal wound to the perineal wound to retrieve the urethral cuff tubing. Excess tubing is trimmed and the Quick Connector System is used to complete the connections between the tubing from the three components [9].
65.3.4 Post-op
At the end of the procedure, the device is left in the deactivated position and the 12 Fr Foley catheter is left indwelling. In our practice, patients stay overnight in the hospital for observation and their catheter is removed the morning following surgery. After a voiding trial, the patient is instructed on pulling the scrotal pump to a dependent position twice daily until their 6-week follow-up visit. At the 6-week visit the device is activated and patients are instructed on routine use.
65.4 Outcomes
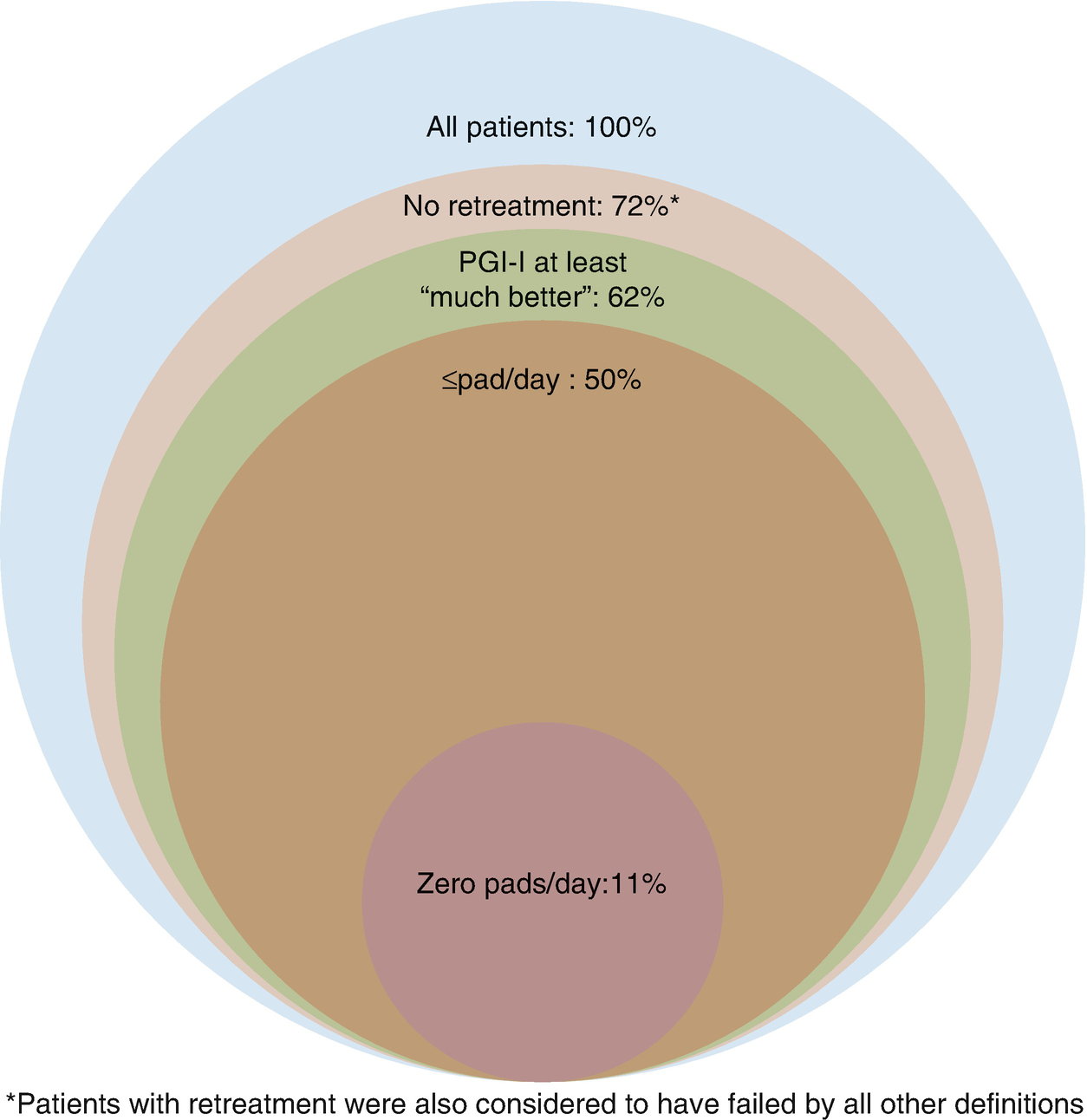
Venn diagram illustrating success rates of AUS placement using four definitions of success. Percentages are calculated from total population n = 309
In addition, the majority of studies have poorly-defined or undefined inclusion/exclusion criteria, with significant heterogeneity of the patient populations, including inconsistent inclusion of patients with varied etiologies for stress incontinence and variable lengths of follow-up. These factors, among others, limit the ability to draw comparisons between studies and surgical techniques.
Notably, despite variation between studies, the current literature consistently demonstrates high long-term success rates for primary AUS implantation [3, 19, 22–26]. That is, a recent pooled-analysis showed an overall re-intervention rate of 26% (range 14.8–44.8%) [3] and a 5 year AUS device survival ranging from 59% to 79% [3, 19, 22–26]. Furthermore, in the few available studies, the reported 10-year device survival rates range from 28% to 64% [4, 22, 25, 27]. For instance, in a review of 124 patients, with a median follow-up of 6.8 years, Kim et al. found an overall revision rate of 37% [27]. Additionally, with regard to functional outcomes, a recent systematic review evaluating patients with non-neurogenic etiologies for incontinence leading to AUS placement in studies with a minimum of 2 years of follow-up noted a “dry or improved” rate of 79% (range 61–100%) [3]. Likewise, high levels of patient satisfaction (over 90%) following AUS placement are commonly reported, though the rate of continence decreases over time [3, 4, 28].
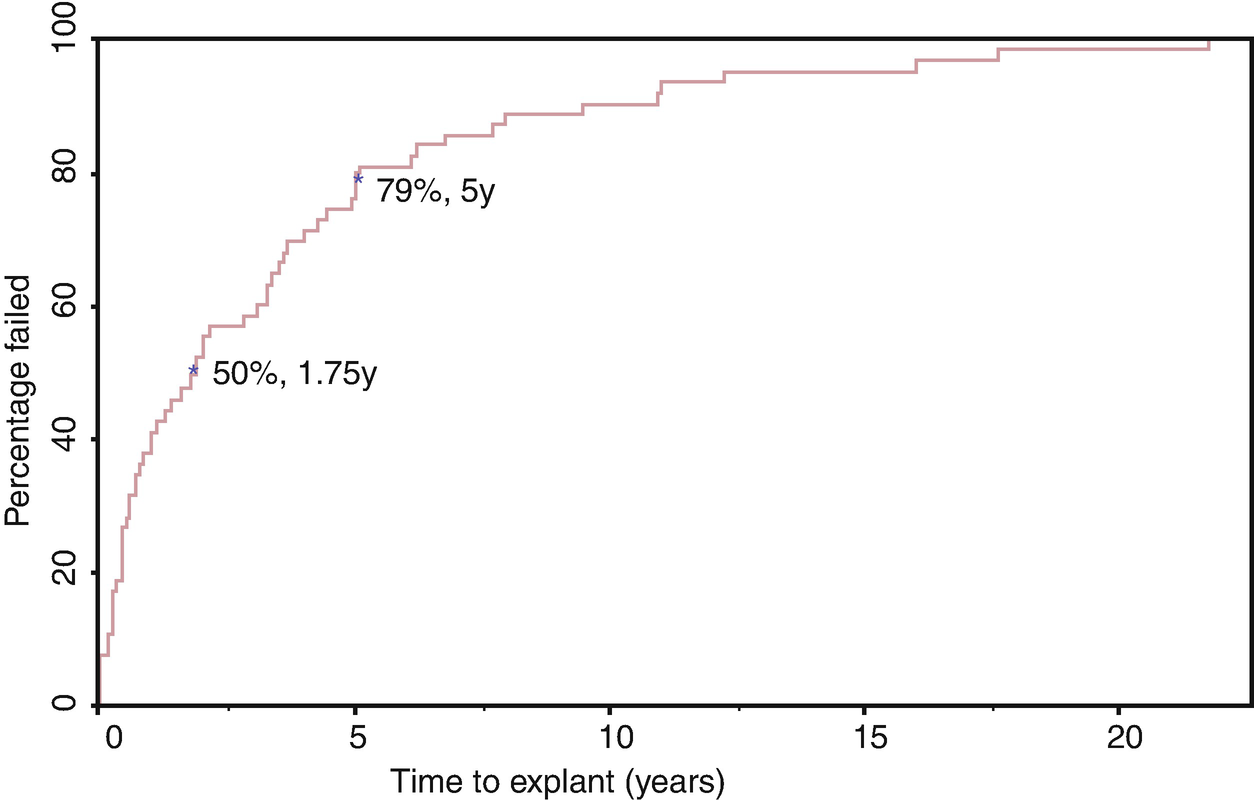
Data regarding outcomes beyond 10 years in the literature is sparse [4, 22]. In the two available series, the 15-year device survival rate was 15% and 41% [4, 22]. In the series by Leon et al., which included 57 men that underwent AUS placement over an 8 year period and had a median follow-up of 15 years, the AUS survival rates without revision were 59%, 28%, 15% and 5% at 5, 10, 15 and 20 years, respectively [22]. This study was unique in that the authors noted that no patients were lost to follow-up. In our own retrospective series of 1082 primary AUS implantations performed at our institution, we found 5, 10 and 15 years device survival rates of 74%, 57% and 41%, respectively [4]. As mentioned above, differences in device survival between series may be due to disparate patient populations, length of follow-up available, patient loss to follow-up, and surgical technique.
65.4.1 Pelvic Radiation and AUS Outcomes
With regard to device outcomes, numerous studies have attempted to identify potential risk factors for adverse AUS device survival [26, 29–38]. A comorbidity that is frequently discussed is receipt of pelvic radiation prior to AUS implantation [29–33]. This is a common clinical scenario as we have found that 37% of patients that underwent AUS in our practice had received prior pelvic radiotherapy [30]. The studies available in the current literature evaluating the association of radiotherapy and device survival have met with conflicting results [29–33]. However, in a recent meta-analysis of 15 series, including 1886 patients, men with a history of radiation therapy in addition to prostatectomy had a higher rate of AUS revision than those treated with prostatectomy alone [33]. The majority of the surgical revision risk was secondary to device infection and urethral erosion events. Likewise, patients with prior radiation therapy were more likely to have persistent urinary incontinence after AUS placement [33]. Given the available AUS literature, many of these studies were small retrospective series, and the authors noted a high level of heterogeneity. Notably, when subanalyzing without the four largest studies, in an effort to decrease heterogeneity, the relative risk of surgical revision was no longer significantly different between those with or without prior radiation therapy [33]. A recent analysis of 925 patients in our practice who underwent primary AUS placement from 1983 to 2011 found no association between pelvic radiation therapy with prostatectomy and increased risk of device infection or erosion when compared to prostatectomy alone. The size of this study is significantly larger than the four studies that were excluded in the subanalysis of the study discussed above [39].
Further studies, including those focused on functional outcomes and quality of life are needed to better define the impact of prior radiotherapy on AUS outcomes and to provide useful information for better patient counseling. It should be noted that patients treated with pelvic radiation therapy should not be excluded from receiving an AUS solely based on this comorbidity.
65.4.2 AUS Following Failed Urethral Sling
Many men prefer urethral sling placement even if they are not ideal candidates. This preference may stem from a desire to avoid a mechanical device, the risks of device malfunction or erosion, and the need for AUS manipulation and replacement over time [7]. For patients with persistent or recurrent stress urinary incontinence after male urethral sling placement, revision surgery either via repeat urethral sling or, more commonly, AUS placement have been reported [40–44]. In this setting, placement of an AUS is typically utilized as the presence of fibrosis hinders urethral compression and/or mobility which are important for sling efficacy [12, 45, 46].
Several reports have demonstrated, albeit in small series, excellent outcomes for AUS placement after a previous urethral sling [41–44]. For instance, similar high success rates with limited complications were seen in a series of 28 patients undergoing AUS after a failed urethral sling when compared to a control group without prior urethral sling surgery [42]. Likewise, in a comparative analysis of patients with stress urinary incontinence after a failed urethral sling, patients undergoing repeat urethral sling placement (transobturator) were six times more likely to have persistent incontinence than those who had an AUS [41].
In cases of failed urethral sling placement, our preference is to place an AUS. Notably, in our experience, in the majority of these cases, the sling can be left in situ without need for excision. If the sling is encountered, we prefer to incise the sling rather than perform urethrolysis as this risks urethral injury and may potentially compromise urethral blood supply.
65.5 Complications Following AUS Placement
65.5.1 Urinary Retention and Hematomas
Perioperative or early postoperative complications following AUS placement most commonly consist of urinary retention, scrotal hematoma and device infection/urethral erosion. In our prospective series of postoperative AUS complications, urinary retention was most common [47]. Postoperative urinary retention following AUS placement is thought to be secondary to urethral edema from the periurethral dissection, error in cuff sizing, or unrecognized surgical injury. Interestingly, in our series, transient postoperative urinary retention was associated with adverse overall device survival and a significantly increased rate of AUS infection/urethral erosion [47]. In cases of post-operative retention following catheter removal the morning after surgery, we teach patients to perform intermittent self-catheterization with a 12 Fr catheter. Other options include leaving an indwelling catheter for a short period of time (24–48 hours) or suprapubic tube placement if retention is longer lasting [9]. Notably, while prolonged catheterization (greater than 48 hours) is reported to increase the risk of erosion, data regarding the potential impact of self-catheterization on AUS outcomes in a non-neurogenic adult population is sparse [48, 49].
Scrotal hematomas may range in size and severity, though most can be managed conservatively. In patients having difficulty with pain control, large/expanding hematoma size, concern for infection, or issues with pump position, hematoma evacuation may be warranted.
65.5.2 Infection and Erosion

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree