div class=”ChapterContextInformation”>
30. Use of Bowel for Urethral Reconstruction
Keywords
Bulbar necrosisEnterourethroplastyUrethroplasty30.1 Introduction
There has been precedence in using bowel segment to substitute affected urinary system structures. Ileum has previously been used to replace the ureter in long ureteric strictures that are not salvageable using conventional treatment [1].
Urethral reconstruction in patients with several previously failed attempts becomes particularly demanding. This subgroup of patients include failed urethral repairs resulting in bulbar urethral necrosis, such as after multiple failed pelvic fracture urethral injuries.
30.2 Discussion
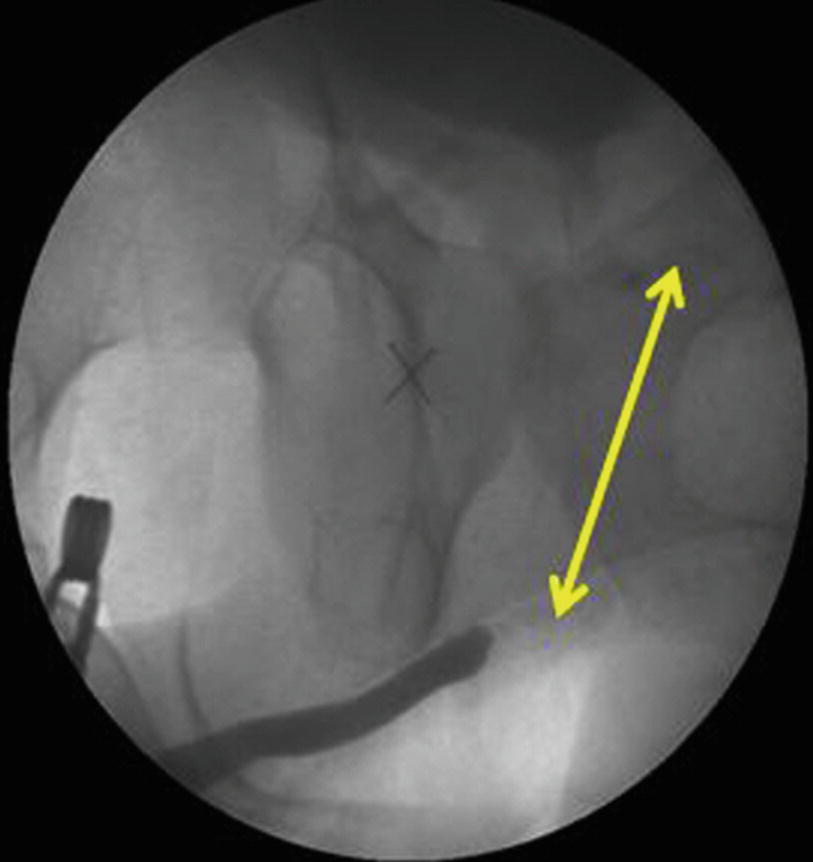
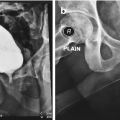
RGU and MCUG depicting bulbar urethral ischemic necrosis (BUIN)
Several publications in the literature evaluate the use of bowel segments both in experimental and clinical studies . These studies describe the use of free colonic mucosa and pedicled bowel segments including – stomach, ileum, right colon, transverse colon and sigmoid colon. The choice of bowel segment depends upon several factors – length and site of urethral substitution, previous bowel surgery, bowel disease and blood supply to the bowel [2–6].
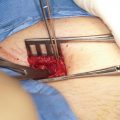
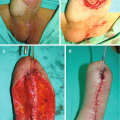
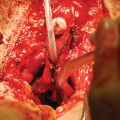
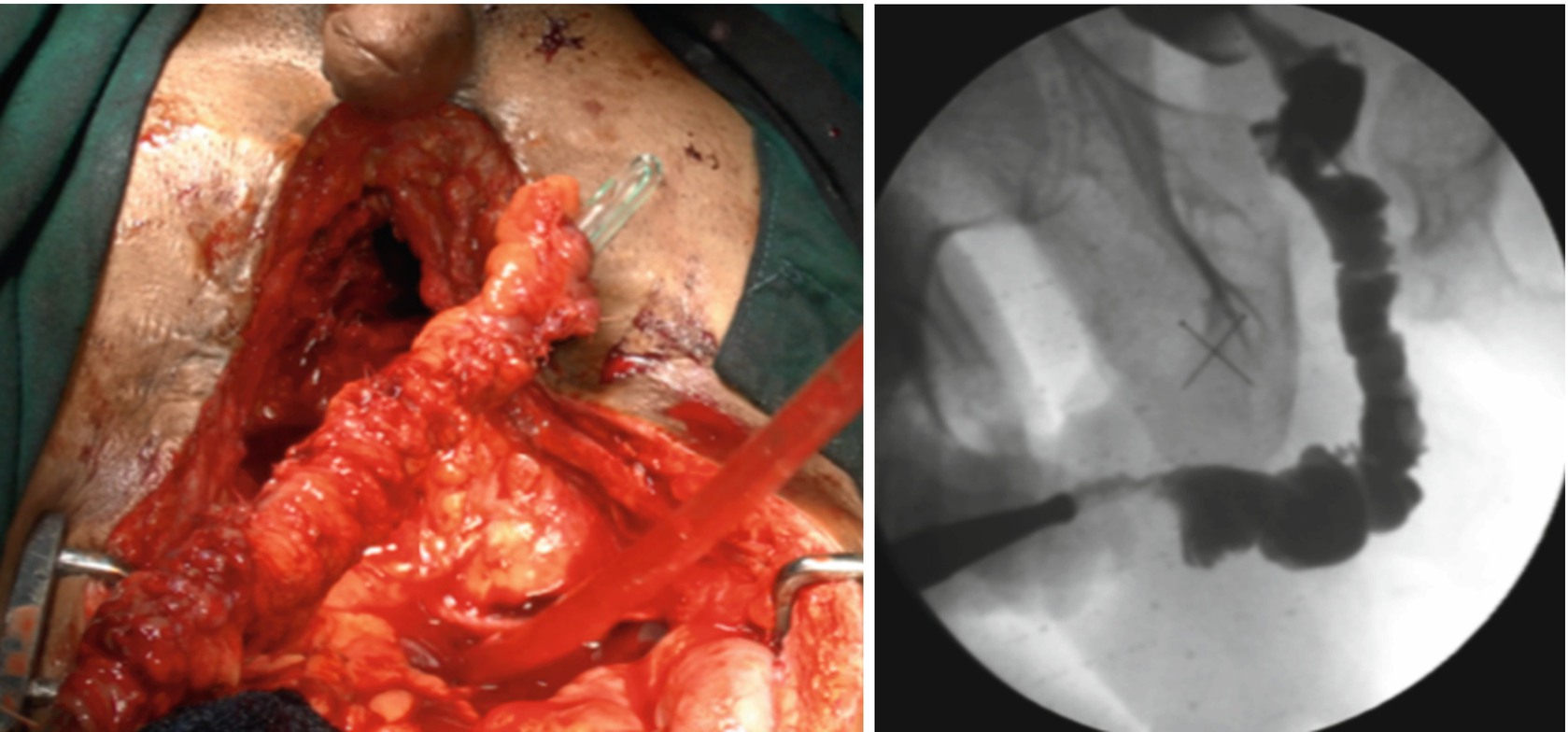
Patient selection for these procedures is of paramount importance. The key is to evaluate which patient would benefit from urethral substitution using a bowel segment. The next challenge is to find the best suited bowel segment for the reconstruction. Usually the bowel segment with pedicle closest to the prostate is suitable. The preferred choice is the use of sigmoid colon. Patients need to admitted a day prior to urethroplasty. Bowel preparation is given and may include enema. Preoperative intravenous prophylactic antibiotics are started. Urethroplasty usually starts with a perineal incision and dissection. The healthy end of anterior urethra is identified. Crural seperation and inferior pubectomy is performed as and when necessary. In our experience, these patients often have a high bladder neck requiring a transpubic approach. This is usually performed with a infraumbilical midline incision. The initial disssection is retroperitoneal. Posterior pubectomy is performed and scar tissue excised. The posterior urethra is incised on a bougie passed from the SPC tract. This avoids opening the bladder. Once the posterior urethra is adequately freed from scar tissue, assesement of length of gap is made. The sigmoid colon is mobilised on its mesentery. The lower protion of sigmlid colon needs to be sacrificied and the upper part is swinged down on its pedicle. The sigmoid is refashioned to 26-30 Fr on a Nelatons catheter. The tailored sigmoid segment is then transposed to the perineum through abdomino perineal window. We usually keep the arch of pubic bone intact and perform inferior pubectomy (from below) and posterior pubectomy (from above). The challange is in performing the anastomosis between proximal sigmoid end and bulbo membranous junction. One trick is to keep a guide wire across the anastomosis which helps in insertion of Foleys catheter. Anastomosis is performed with 4-0 Polydiaxone suture. The distal anastomosis is done from perineum. We have additionally always mobilised omentum and wrapped around the proximal anastomosis.Clear oral fluids are started on post op day 1 as per the latest protocol. We do not keep patients fasting. Abdominal drain is kept for 5 days and once bowel movements start, drain is removed.Full oral diet is started on day 5–6. Patients are discharged on day 6–8. Catheter is removed after 6 weeks. We perform pericatheter urethrogram before removal of catheter.
The earliest report of use of bowel segment in urethral reconstruction comes from Hennebert and Jain in 1969 [4]. They described an experimental study in dogs and four short case reports of ileourethroplasty . The other case is from Lee et al. who described the use of a reconfigured flap of sigmoid colon in a patient with complicated pelvic fracture urethral injury along with a simultaneous sigmoid colocystoplasty who did well at 15 months follow up [5].
The largest series of 11 patients is described by Mundy and Andrich where they use various segments of bowel to replace complex long segment strictures of the urethra [6]. The follow up ranged from 2–12 years and 6 patients had an uneventful recovery. Three patients developed proximal anastomotic strictures; one was treated with regular interval dilatation, one requiring revision of the anastomosis and the third requiring a completely new flap. Two patients developed stones – one requiring the stone removal and the other requiring a Mitrofanoff procedure as the stone removal resulted in irreversible damage to the ileal mucosa.
We have performed urethroplasty in 115 patients of bulbar urethral necrosis. Amongst these, we performed enetrourethroplasty using sigmoid colon in 3 patients with 100% success [7].

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree