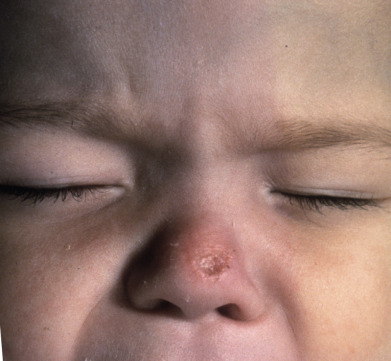
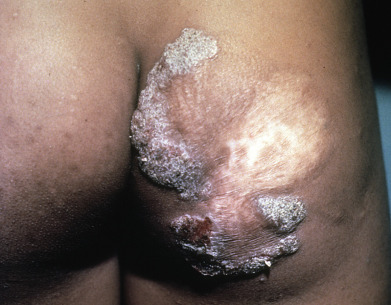
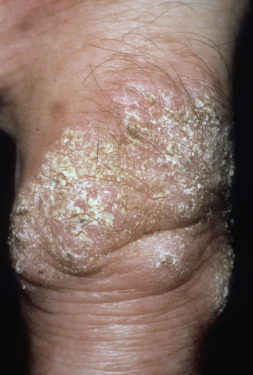
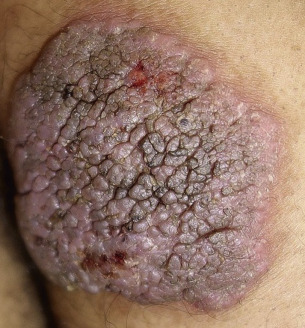
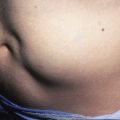
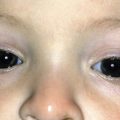
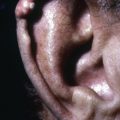
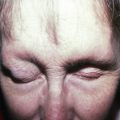
Tuberculosis and atypical mycobacterial infections can be difficult to diagnose clinically and require a high index of suspicion and familiarity with their manifestations in the skin.
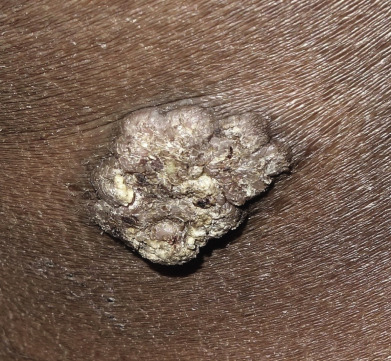
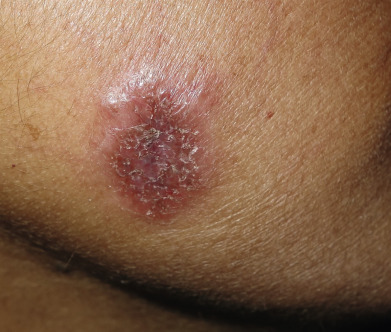
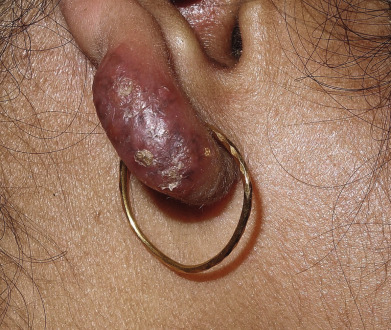
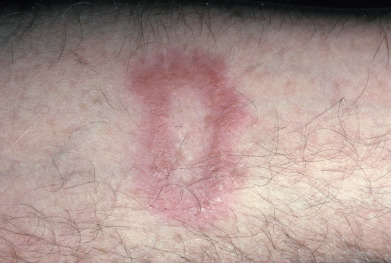
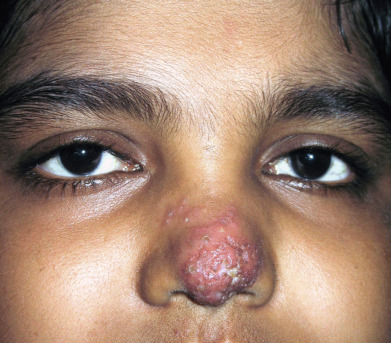
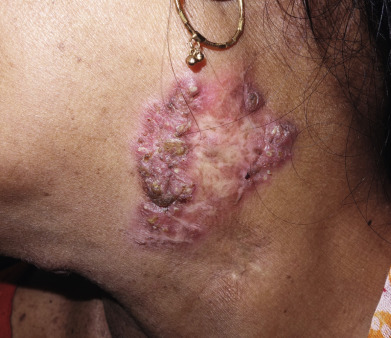
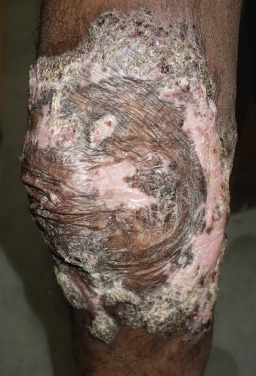
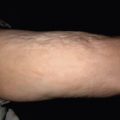
Tuberculosis (TB) is more prevalent in the developing countries, especially those with particularly high rates of human immunodeficiency virus (HIV)–positive populations. The classification system of cutaneous TB depends on how the infection was acquired, and these four forms include many different cutaneous lesions. Examples of these four categories include 1) verrucous papules or plaques of primary inoculation TB (TB verrucosa cutis); 2) masses and nodules with possible suppuration and ulceration overlying infected lymph nodes representing endogenous, contiguous spread; 3) widespread macules, papules, pustules, nodules, or purpura seen in miliary TB from hematogenous spread; and 4) persistent nodules of the posterior lower calf representing a lobular panniculitis known as erythema induratum , a form of a tuberculid. These cutaneous manifestations of TB, along with the many other specific and nonspecific findings, should prompt testing including skin biopsy, tissue culture, screening with blood testing if available such as QuantiFERON-Gold, tuberculin skin testing, and in some, a chest x-ray.
Atypical mycobacterial infections can occur in immunocompetent hosts after trauma, surgery, or exposures to organisms in specific locations such as fish tanks ( Mycobacterium marinum ) or pedicure spas ( Mycobacterium fortuitum ). Immunocompromised individuals are at risk of developing infections with atypical mycobacteria such as the Mycobacterium avium-intracellulare as seen in patients infected with HIV. Despite the great variety of atypical mycobacterial organisms, the clinical findings tend to be similar and nonspecific, including papules, pustules, nodules, and ulcers. They can be localized or widespread depending on the cause, exposure, and underlying immune status of the patient. Tissue culture with antibiotic sensitivity testing is helpful, but can take several weeks to be completed.
This chapter of the atlas catalogs the many cutaneous findings seen in patients with both TB and nontuberculous mycobacterial infections.