Diagnosis
Transgender is not a formal diagnosis. Transgender individuals possess persistent concerns, uncertainties, and questions about gender identity. These issues often become the most important aspect of their life and prevent the establishment of an unconflicted gender identity. These individuals have passed a clinical threshold.
When such an individual meets the specified criteria in one of the 2 official nomenclatures, The International Classification of Diseases-10 (ICD-10) or the Diagnostic Statistical Manual of Mental Disorders (5th Edition) ( DSM-5 ), they are diagnosed as having a gender identity disorder (GID) or gender dysphoria.
In 1994, the Diagnostic and Statistical Manual of Mental Disorders (Fourth Edition) (DSM-IV) committee replaced the diagnosis of “transsexualism” with “gender identity disorder.” According to DSM-IV , individuals must demonstrate a strong and persistent cross-gender identification and a persistent discomfort with their sex or a sense of inappropriateness in the gender role of that sex. In DSM-5 , published in 2013, the term “gender identity disorder” was replaced with the term “gender dysphoria.” The diagnosis of gender dysphoria requires a marked difference between the individual’s expressed/experienced gender, and the gender others would assign him or her. This difference must be present for 6 months and cause clinically significant distress or impairment in social, occupational, or other important areas of functioning.
The ICD-10 provides 5 diagnoses for GIDs. These diagnoses include Transsexualism (F64.0), Dual-Role Transvestism (F64.1), Gender Identity Disorder of Childhood (64.2), Other Gender Identity Disorders (F64.8), and Gender Identity Disorder, Unspecified.
Transsexualism has 3 criteria, as follows:
- 1.
The desire to live and be accepted as a member of the opposite sex, usually accompanied by the wish to make his or her body as congruent as possible with the preferred sex through surgery and hormone treatment.
- 2.
The transsexual identity has been present persistently for at least 2 years.
- 3.
The disorder is not a symptom of another mental disorder or a chromosomal abnormality.
It is important to realize that the DSM-V and ICD-10 are designed to guide research and treatment. The designation of GID or gender dysphoria as mental disorders is not a license for stigmatization or for the deprivation of gender patients’ civil rights. In order to gain and maintain access to medical treatments, individuals often need a diagnosis. The change from “disorder” to “dysphoria” is designed to facilitate access to care without stigmatization.
Hormonal therapy
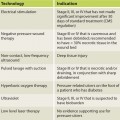
Many persons with gender dysphoria desire hormone therapy in order to transition, and endocrinologists or primary care providers typically guide treatment ( Table 3.1 ). Endocrine therapy can help relieve psychosocial discomfort by inhibiting the effects of endogenous hormones and inducing feminizing or masculinizing changes. As with surgery, hormone therapy requires a tailored approach. The administration of hormones is individualized based on the person’s goals. Some people seek maximum feminization or masculinization, whereas others experience relief with an androgynous presentation resulting from hormonal minimization of existing secondary sex characteristics.
| Hormone therapies for transwomen | ||
| Estrogens | Oral | |
| 17-β estradiol | 2–6 mg daily | |
| Ethinyl estradiol | 2–6 mg daily | |
| Conjugated estrogen | 2.5–7.5 mg daily | |
| Transdermal | ||
| Estradiol patch | 0.1–0.4 mg twice weekly | |
| Estradiol gel | 0.1–0.4 mg daily | |
| Parenteral | ||
| Estradiol valerate or cypionate | 5–20 mg IM every 2 wk or 2–10 mg IM weekly | |
| Antiandrogens | Spironolactone | 100–400 mg PO daily, divided doses |
| Cyproterone acetate a | 50–100 mg PO daily | |
| GnRH agonists | 3.75 mg subcutaneous monthly | |
| 5-α reductase inhibitors | Finasteride | 2.5 mg PO daily |
| Dutasteride | 0.5 mg PO every other day | |
| Hormone therapies for transmen | ||
| Testosterones | Oral | |
| Testosterone undecanoate a | 160–240 mg/d | |
| Transdermal | ||
| Testosterone patch | 2.5–7.5 mg/d | |
| Testosterone 1% gel | 2.5–10 mg/d | |
| Parenteral | ||
| Testosterone cypionate or enanthate | 50–200 mg IM weekly or 100–200 mg every 2 wk | |
| Testosterone undecanoate | 1000 mg IM every 10 wk | |
Not all gender surgeries (ie, chest surgery) require preoperative hormone therapy. However, third-party payers often require documentation of duration of hormone therapy, or an explanation as to why a patient does not take hormones, before providing insurance approval for surgery.
Although specific hormonal regimens may vary between centers, the surgeon should be familiar with the possible side effects of hormonal therapy and how they relate to the surgical care of the transgender patient. These possible side effects include issues related to liver function, risk of venous thromboembolism, electrolyte imbalance, drug-drug interactions, and possible malignancy (ie, breast cancer).
The goal of endocrine therapy is to change secondary sex characteristics in order to reduce gender dysphoria and/or facilitate a physical presentation consistent with the individual’s sense of self. Hormonal therapy should be individualized to the needs and desires of patients, based on their goals and associated medical conditions. Before initiating hormone therapy, a psychosocial assessment by a qualified mental health or medical practitioner should be performed. The Standards of Care (SOC) indicate the physician prescribing the hormones should
- 1.
Perform an initial evaluation that includes health history, physical examination, and relevant laboratory tests
- 2.
Explain what feminizing/masculinizing medications do and the possible side effects/health risks (including the effects on fertility)
- 3.
Confirm that the patient has the capacity to understand the risks and benefits of treatment and to make an informed decision about medical care
- 4.
Inform the patient of the SOC and eligibility/readiness requirements
- 5.
Provide ongoing medical monitoring, including regular physical and laboratory examination to monitor hormone effects and side effects.
Hormone Therapy for Transwomen
Feminization through hormonal therapy is achieved by 2 mechanisms: suppression of androgen effects and induction of female physical characteristics. Androgen suppression is achieved by using medications that either suppress gonadotropin-releasing hormone (GnRH) or are GnRH antagonists (progestational agents), suppress the production of luteinizing hormone (progestational agents, cyproterone acetate), interfere with testosterone production or metabolism of testosterone to dihydrotestosterone (spironolactone, finasteride, cyproterone acetate), or interfere with the binding of androgen to its receptors in target tissues (spironolactone, cyproterone acetate, flutamide). In addition, estrogen is used to induce female secondary sex characteristics, and its mechanism of action is through direct stimulation of receptors in target tissues.
Estrogens can be taken orally, intramuscularly, or cutaneously. Oral estrogens have the advantage of being inexpensive, widely available, and easy to administer. Oral estradiol is the preferred form of estrogen because it allows for straightforward measurement of serum estradiol concentration as a marker of efficacy. Other oral forms of estrogen include conjugated estrogens, such as Premarin, and synthetic estrogens, such as ethinyl estradiol. Importantly, use of oral estrogen, and specifically ethinyl estradiol, appears to increase the risk of venous thromboembolism. Intramuscular estrogens, such as estradiol valerate, can be taken every 1 to 2 weeks but can result in supraphysiologic levels of estradiol if serum levels are not properly monitored. Furthermore, many individuals find intramuscular injections inconvenient for long-term use. Cutaneous forms of estrogen, such as estradiol gel or estradiol patches, are also available and should be considered in patients with risk factors for venous thromboembolism. Cutaneous forms of estrogen have the disadvantage of more limited availability, increased cost, and potential adverse skin reactions.
Antiandrogens are often necessary as an adjunctive therapy to further reduce testosterone concentrations into the female range of less than 50 ng/mL. Spironolactone is the most commonly prescribed antiandrogen in the United States. Typical doses range from 100 to 400 mg daily in divided dosages. Cyproterone acetate, another commonly prescribed antiandrogen available in Europe and Canada, is not approved in the United States due to concerns with hepatotoxicity. This agent may have the additional advantage of having some progestin-like activity. Finally, 5-α reductase inhibitors (finasteride and dutasteride) block the conversion of testosterone to the more active agent, 5-α-dihydrotestosterone. These medications have beneficial effects on scalp hair loss, body hair growth, sebaceous glands, and skin consistency.
Progesterones can also be prescribed for transwomen. However, there is limited evidence that they offer any additional benefit in feminization of the body. In addition, because these agents may increase the risk of cerebrovascular disease, they are not routinely prescribed as part of the initial hormone regimen.
Within the first 6 months of therapy, there is typically a redistribution of body fat, decreased muscle mass, softening of skin, and decreased libido. Breast growth may be expected after 3 to 6 months of therapy and may continue for up to 2 years. Over a period of several years, body fat and facial hair become finer, although they are not completely eliminated by hormonal therapy alone. Progression of male pattern baldness may slow; however, hair does not typically regrow in bald areas. Many of the changes, perhaps with the exception of breast growth, are reversible with cessation of therapy.
Although there are many beneficial effects of hormone therapy, there are also potential risks. These potential risks include an increased risk of venous thromboembolism, weight gain, hypertriglyceridemia, gallstones, and elevated liver enzymes. Other possible risks include cardiovascular disease, hypertension, hyperprolactinemia, and diabetes. The risk of breast cancer is, as of yet, indeterminate.
While on hormone therapy, transwomen should undergo routine laboratory assessment to confirm that their dosing provides therapeutic and not supraphysiologic concentrations of estradiol. The risk of adverse events increases with higher doses, particularly doses resulting in supraphysiologic levels of estradiol. Optimal serum levels range from 100 to 300 pg/mL and should not exceed 400 pg/mL. In addition, electrolytes should be measured for those individuals on spironolactone, and testosterone should be measured to confirm that levels are in the female range.
Before gender confirmation surgery, patients should have their estradiol concentration measured in order to confirm that serum levels of estradiol are not supraphysiologic. Estrogen medication should be discontinued 2 weeks before surgery to reduce the risk of venous thromboembolism, and patients should be ambulatory before restarting estrogen therapy. Following orchiectomy, spironolactone can be discontinued, and estrogen doses may be lowered while still maintaining therapeutic concentrations of serum estradiol.
Hormone Therapy for Transmen
Masculinization through hormonal therapy for transmen follows general principles of hormone replacement for treatment of male hypogonadism. Both intramuscular and transdermal testosterone preparations are available and may be used to achieve testosterone values in the normal male range. Testosterone therapy results in increased muscle mass and decreased fat mass, increased facial hair and acne, male pattern baldness, and increased libido. In addition, testosterone results in clitoromegaly, temporary or permanent decreased fertility, deepened voice, vaginal atrophy, and cessation of menses. If uterine bleeding does not cease, GnRH analogues or depot medroxyprogesterone may be added to stop menses and to reduce estrogen levels to those found in biological males.
Transmen often prefer testosterone injections for their affordability, wide availability, and convenient schedule (every 1–2 weeks). However, some patients find the deep intramuscular injections painful. Testosterone undecanoate, a new intramuscular testosterone, can be taken less frequently (every 10 weeks) and was approved by the US Food and Drug Administration in 2014. However, warnings about pulmonary oil microembolism with this testosterone preparation have limited its use in the United States.
Testosterone patches or gels are good options for transmen but are also more expensive than intramuscular testosterone and require daily application. Skin irritation is often reported with patches, and gels carry the risk of transfer of testosterone to women or children in close contact. Subcutaneous testosterone pellets are another option for testosterone therapy, but they require a minor surgical procedure every 12 weeks.
Ideally, testosterone administered intramuscularly should be measured at the peak and trough to ensure that serum concentrations are in the therapeutic range (typically 400–1000 ng/mL). Timing for checking levels is less critical for patients on patches or gel, provided they are compliant with therapy. Complete blood count (CBC) and liver function level should be monitored because testosterone therapy can result in erythrocytosis and elevation in liver enzymes. Other risks of testosterone therapy include hypertension, excessive weight gain, salt retention, lipid changes, cystic acne, and adverse psychological changes.
Preoperatively, transmen should discontinue their testosterone 2 weeks before gender confirmation surgery. The risk of postoperative venous thromboembolism is lower than in a transwoman. However, testosterone can be converted to estradiol in adipose tissue by the aromatase enzyme, especially when present in high concentrations. Patients should not restart their testosterone therapy until they are ambulatory after surgery.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree