• Skeletal contouring can add convexity to the profile and narrow the face from the frontal view.
• Procedures on the zygoma, mandible, and chin are usually combined to obtain optimal results.
• Skeletal contraction will result in increased soft tissue laxity, and secondary skin-related procedures may be necessary in older patients.
• Orthognathic surgery is a powerful aesthetic technique, which is indicated as the primary approach for achieving certain facial shapes.
• The surgery-first approach to orthognathic treatment saves the patient time and maintains improved aesthetics during the perioperative period.
Introduction
Although universal beauty may be difficult to agree on, there are key features of a beautiful face that many, regardless of the ethnic background, would include in their definition of beauty. Among these are symmetry, a youthful appearance, and well-balanced facial proportions. Many Caucasian women prefer high, sharply defined cheekbones, whereas Asian women prefer round or oval-shaped faces. In addition, many Asian women may have faces that appear overly flat and broad and lack contour. Two-dimensional (2D) photographs as well as movies may exaggerate the differences among ethnic groups or even within a single ethnic group; however, we live in a three-dimensional (3D) world, and the faces we observe directly are three dimensional. Assessing the face and “restructuring” the face must be three-dimensional and based on the surgeon’s perception and not on 2D images and 2D cephalometric analyses. Facial aesthetic surgery is a 3D procedure, and emphasis must be placed on altering the facial contours at multiple planes.
Facial bone contouring surgery for Asians has its roots in mandibular angle procedures and malar reduction procedures. Today, the approach has evolved to address the facial form as a whole. To achieve the ideal facial proportion and shape, the surgeon needs to change each component of the facial skeleton based on evaluation of facial contours in three dimensions: frontal, lateral, and oblique.
Patient evaluation
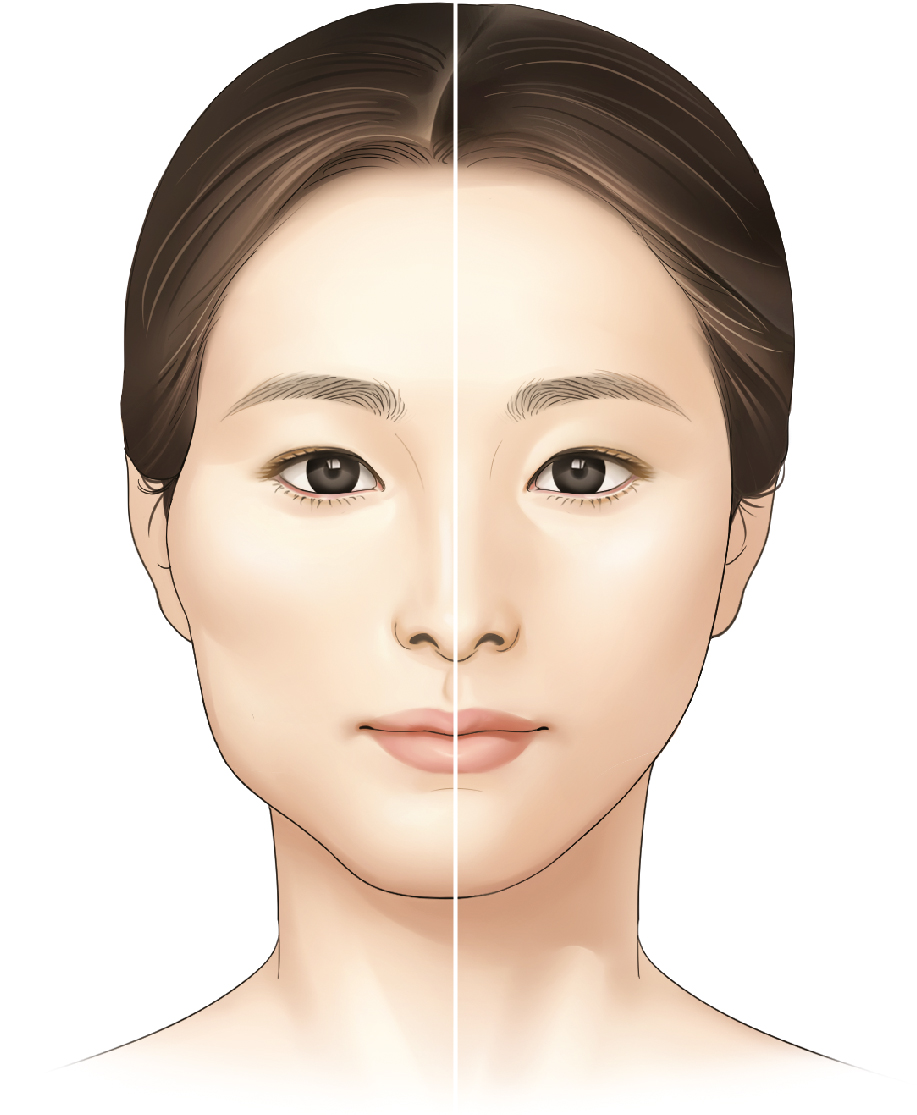
Asian faces are stereotyped most commonly as broad, with flattened contours of the eyes, nose, and face ( Fig. 23.1 ). Many Asians feel that attractive facial features include large eyes, a well-balanced nose with a well-defined profile, and a small lower third of the face. Such individuals who regard their facial features as falling below the mainstream ideals of beauty are willing to undergo facial aesthetic surgery that involves the skeletal framework. Younger individuals wish to undergo facial bone contouring to make their faces smaller. It is important to understand that these individuals seeking the ideal facial form are not asking surgeons to create for them the “average” or “normal” face but, instead, wish to appear above average—chic and stylish and not merely natural—according to their own set of ideals.
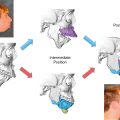
Historically, malarplasty was known as “malar reduction” or “zygoma reduction” because many of the malarplasty procedures in Asians had focused on reduction of the prominent malar bone. However, as we have gained a better understanding of the multidimensional aesthetics of the malar region reduction malarplasty, simple reduction of the zygomatic arch/body through ostectomy achieves a limited result and is currently considered only a single component of malarplasty. , Today, malarplasty is a multifaceted procedure that involves repositioning of the malar complex to an ideal location, with reshaping/contouring of the malar bone itself according to the patient’s desired features and preferences. The malar bone can be repositioned in a posterior direction and rotated, resulting in reduction of the malar arch.
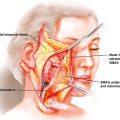
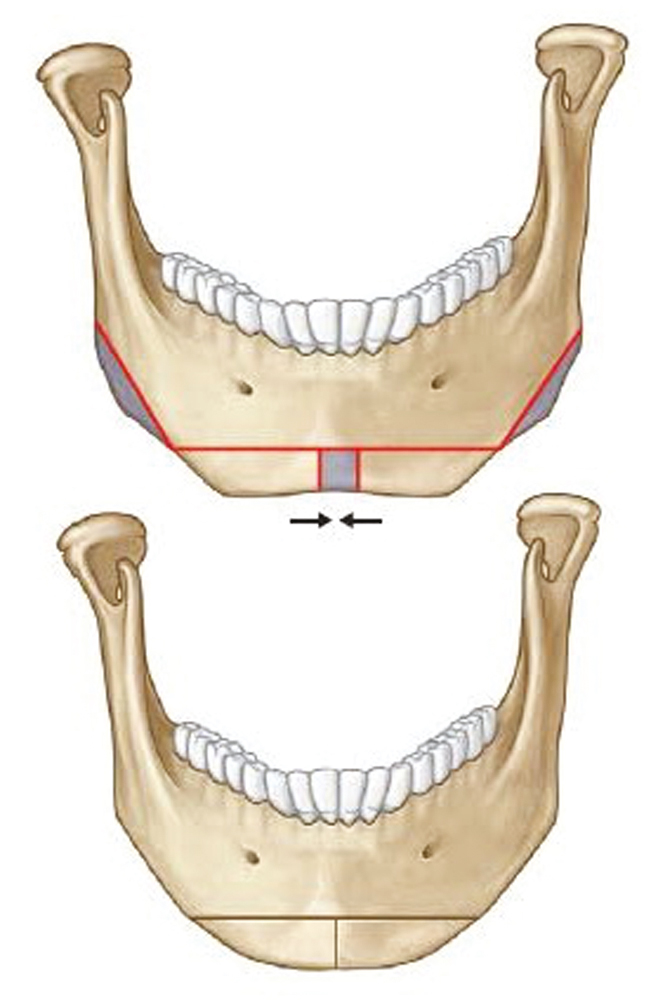
Similarly, the traditional mandibuloplasty, known as “mandible reduction” or “mandible angle reduction,” has evolved. In the 1990s and early 2000s, most Asian plastic surgeons focused on mandibular angle reduction to reshape the mandibular angle. As the concept of addressing the entire mandible evolved, treatment was no longer limited to the angle, and techniques involving the entire mandible were developed. Today, contemporary mandibuloplasty involves addressing all of the components of the mandible, not only the mandibular angle but also the body and the chin. Although simple mandibular angle reduction did improve the posterior width of the facial contour, patients noticed the residual and unintended consequences of a wider contour of the chin following mandibular angle reduction. As a consequence, contemporary mandibuloplasty must be individualized and address the aesthetic goals of the entire mandible in three dimensions and not just in the single dimension of the mandibular width. Today, we place a greater emphasis on position and the 3D shape of the chin. For the Asian ideal, we have found that the use of narrowing genioplasty or chin contouring is effective for shaping the patient’s facial contour ( Fig. 23.2 ). By combining contemporary malarplasty and mandibuloplasty as simultaneous procedures, the surgeon has the ability to reshape the upper and lower thirds of the face ( Fig. 23.3 ).
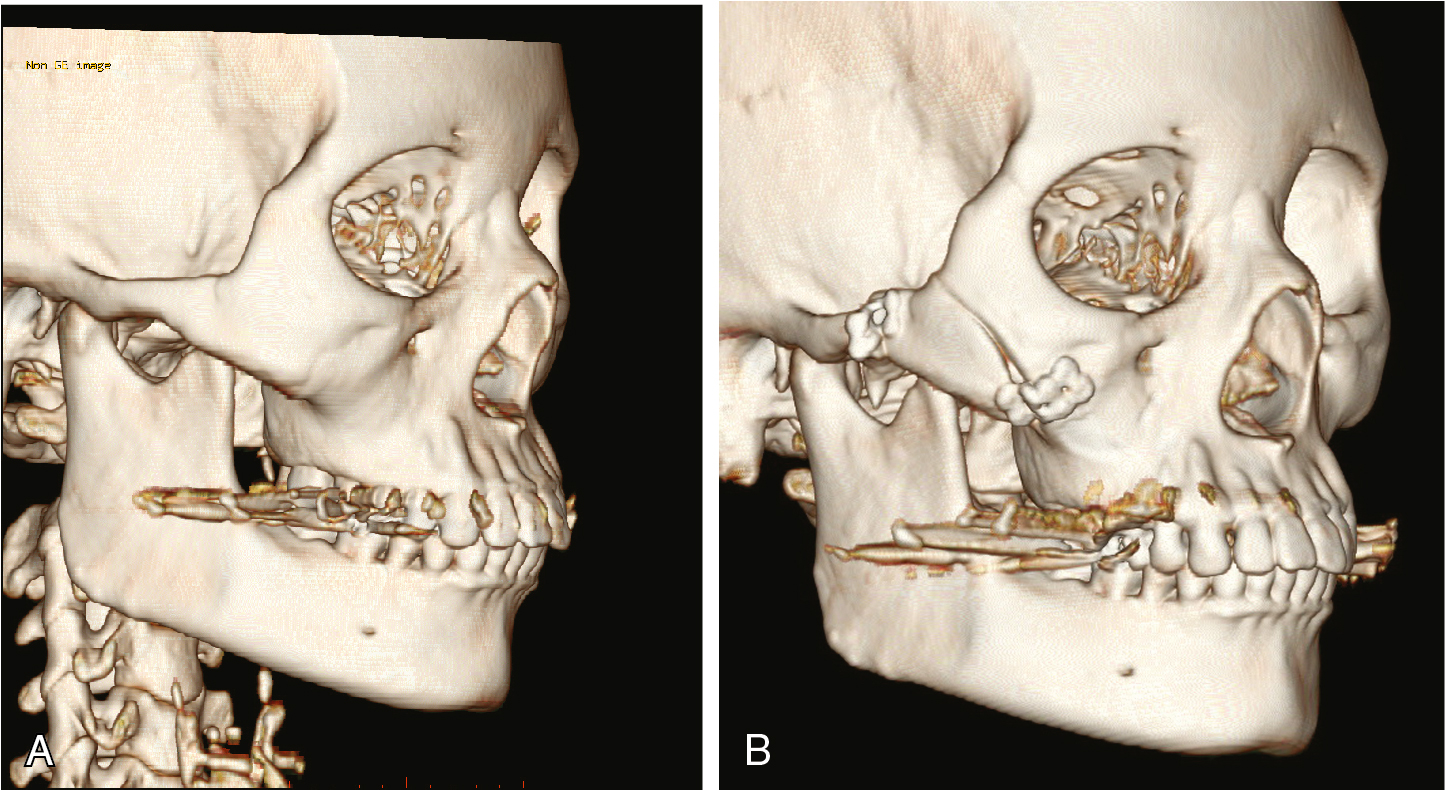
With the addition of orthognathic surgery to malarplasty and mandibuloplasty, the surgeon can address nearly any component of the Asian face to optimize both aesthetic and functional goals. This is a powerful combination. Orthognathic surgery differs from facial contouring surgery in that it seeks to restore the occlusion and facial aesthetics, whereas facial contouring surgeries, such as malarplasty and mandibuloplasty, seek to correct the facial contour itself while preserving the occlusion. Viewing orthognathic surgery purely from the aesthetic perspective, marked changes in the facial contour are possible by changing the occlusal plane, even in patients with near-normal occlusion. The entire upper and lower thirds of the face can be changed as a single unit by clockwise and counterclockwise rotations.
Genioplasty in Asian patients, either for reduction or advancement, is a procedure similar to that performed in Caucasian patients. The most common procedure in Asian women is narrowing genioplasty to make the lower face appear slender and the chin appear more feminine. This procedure is appropriate for the trapezoid, or broad chin, morphology.
History
Compared with the dolichocephalic craniofacial shape of the Western population, Asian faces tend to have a brachycephalic shape. Although the surgical procedures are technically similar, the aesthetic goals for the Asian face are not and require a different treatment plan. During consultation, the surgeon gains a clear understanding of the patient’s goals. A thorough physical examination is performed, as well as standard 2D photography and 3D imaging, if available. Craniofacial morphology in the Asian patient is assessed three dimensionally but can be broadly divided into the frontal and profile views.
Physical examination
Typically, Asian patients lack the desired convexity of the facial profile. Regions that are evaluated for their projection include the glabella, radix, nasal tip, subnasale, and pogonion. When these landmarks are underprojected, the face has a flat profile and lacks the convexity associated with an attractive face. Multiple approaches can be employed to address each of these areas: rhinoplasty, genioplasty, filler, or fat grafting. A rhinoplasty can increase the radix, dorsum, and tip projection, adding convexity to the profile. Dermal fillers can be used to augment the glabella and the lips; in some cases, fillers may be used to achieve augmentation of the chin and the nose as well. A chin implant or advancement genioplasty can advance the pogonion.
From the frontal view, the Asian face may appear broad, especially in the gonial, chin, and malar regions. The malar regions are evaluated in three dimensions to assess anterior projection, vertical height, and width. The mandible and the chin are also evaluated to determine where the excessive width occurs and what anatomic element is contributing to their width. It is important to discern if the degree of gonial prominence is primarily due to masseteric hypertrophy, mandibular hyperplasia, or both because the treatment is different for each etiology. The buccal fat pad may contribute to cheek fullness as well, and a determination can be made regarding the need for a buccal lipectomy at the time of surgery. When evaluating the patient, it is important to determine whether the face is too broad dimensionally or if it appears broad because of the square shape. If the face is dimensionally broad, narrowing procedures will be indicated. However, the face may be dimensionally normal but perceived as broad because of the square shape. In this case, narrowing procedures are not indicated because they will cause loss of soft tissue support. The dimensionally normal square face may be better treated with elongating genioplasty to achieve the desired result. It is acceptable to have a lower facial third that exceeds the height of the middle and upper thirds and maintain an aesthetically pleasing facial shape.
Preoperative imaging
At a minimum, preoperative imaging should include radiographs and 2D photographs of the patient’s face. Ideally, 3D computed tomography (CT) or cone beam computed tomography (CBCT) will be available to review and to rule out the presence of any bone pathology and to visualize relevant anatomy, such as the inferior alveolar canal. Virtual surgical planning (VSP) is useful, and as the soft tissue responses to bone movements are quantified, VSP may play a more critical role in predicting the final outcome of the planned osteotomies.
Indications and contraindications
The ability of these procedures to provide safe and predictable results has led to their popularity in Asian countries. Although the overall strategy has remained the same, the concept of facial bone contouring surgery or facial profiloplasty in Asians has evolved. Today, it is incorrect to assume that Asians seek to “Westernize” their faces. Although Westernization of the Asian face may have been a goal in the past, most patients currently seek to preserve their ethnic identity and simultaneously improve their appearance by changing their facial proportions. If a prominent malar bone is a problem, malarplasty should be performed, whereas if a prominent mandible is the major concern, mandibuloplasty should be considered. If the positions of the maxilla and the mandible are not ideal, an option is orthognathic surgery based on the facial profile. Surgeons who specialize in addressing the concerns of facial contours and profiles in Asians should be familiar and technically well versed in the nuances of the aesthetic goals and available surgical procedures ranging from reshaping (malarplasty and mandibuloplasty) to repositioning (orthognathic surgery).
Current issues about surgical techniques
In this section, we address the surgical nuances involved in malarplasty, mandibuloplasty, and orthognathic surgery.
Malarplasty
Preoperative planning
Malarplasty has evolved from a technique of simple in-fracture or burring of the zygoma to a 3D analysis and movement of the malar process. A wide zygoma will benefit from a simple in-fracture, but an anteriorly protruding zygoma will require posterior positioning in addition to the in-fracture. The patient’s malar eminence should be evaluated for anterior projection, lateral projection, and vertical height. 3D photographic morphing can be done to help the surgeon understand the patient’s concerns and goals. Once the patient and the surgeon agree on the desired objective, the surgeon develops a treatment plan to achieve the patient’s goals. Currently, our recommended technique is a linear osteotomy without bone removal ( Fig. 23.4 ).
Primary approach
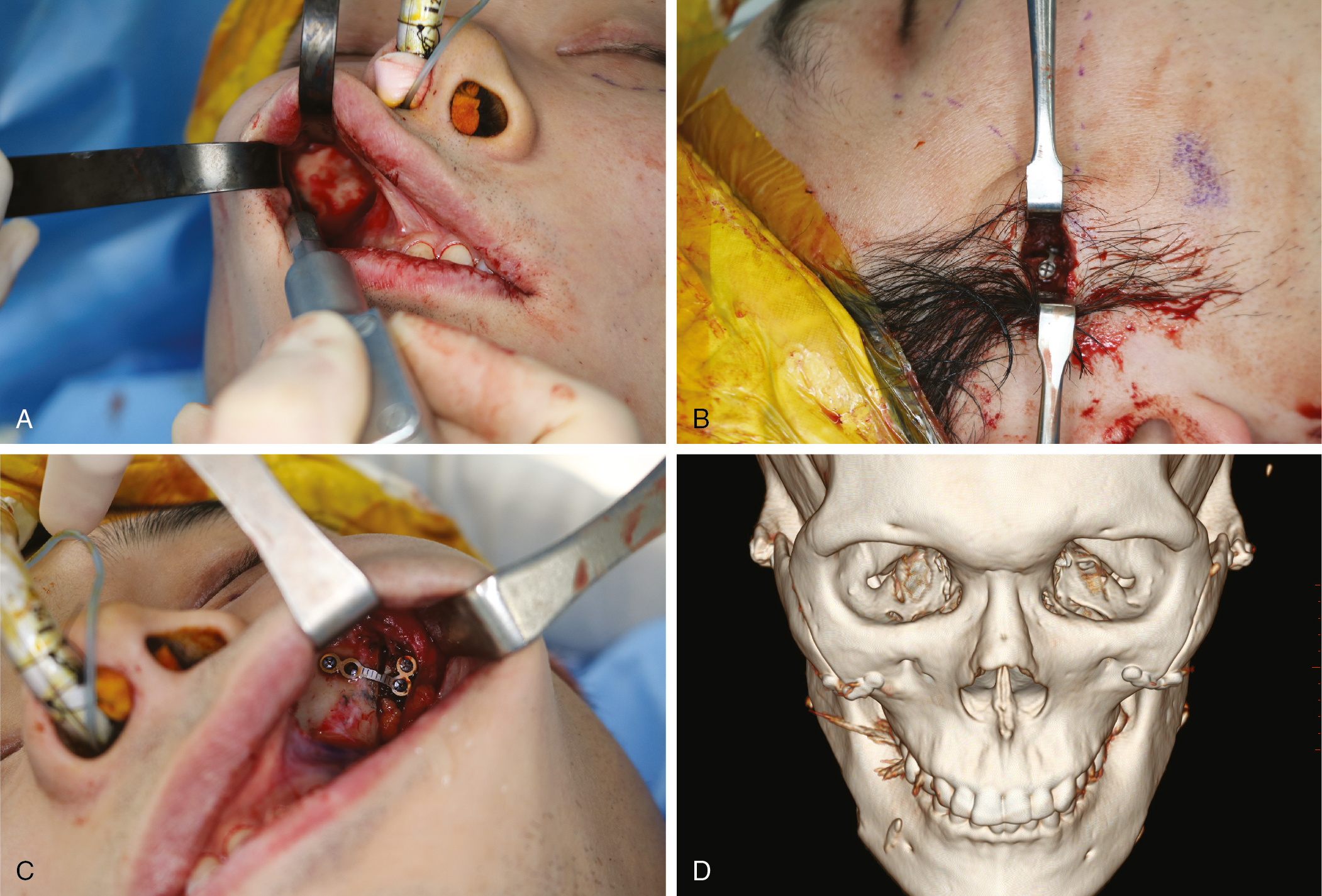
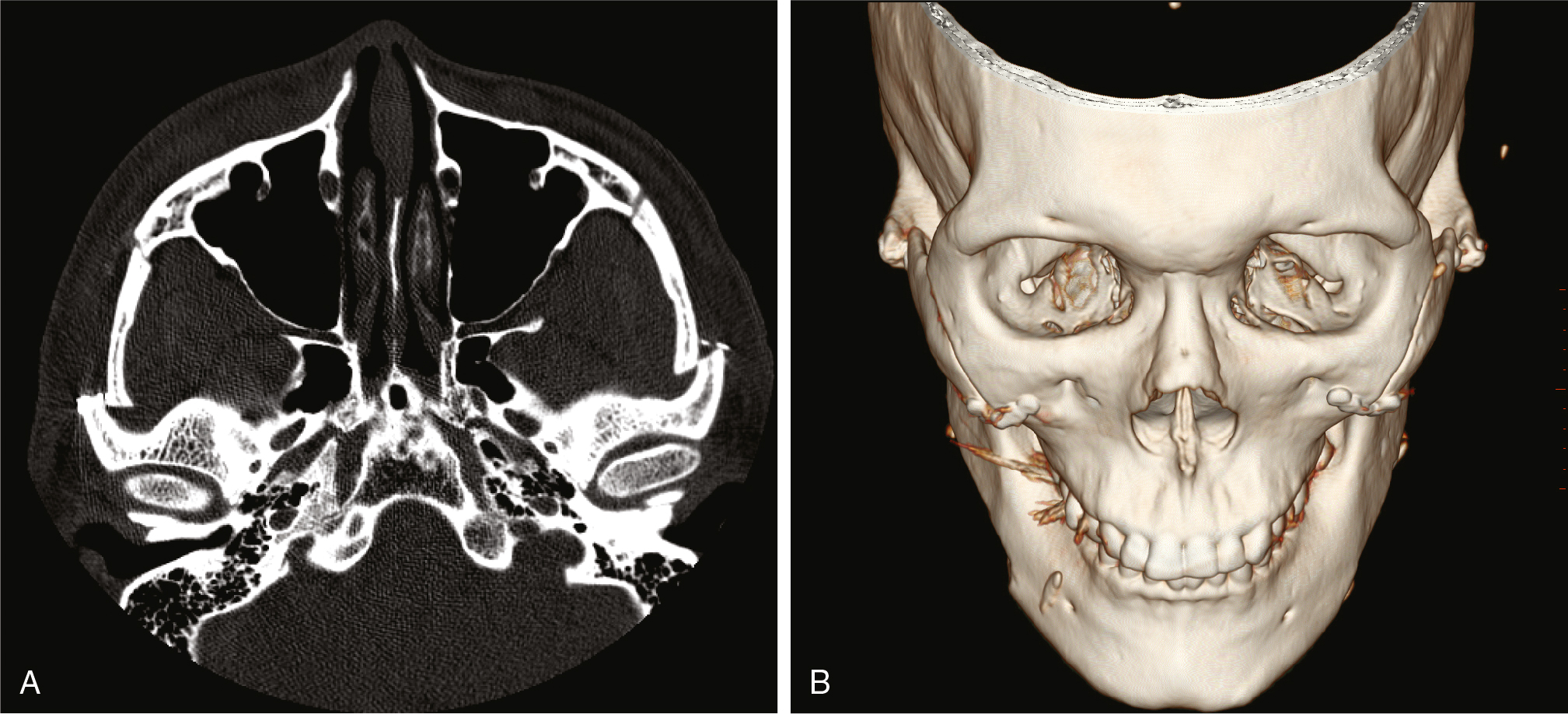
Lidocaine with epinephrine is injected before the patient is prepped and draped for surgery. Chlorhexidine oral rinse is allowed to sit for 5 minutes, and then an incision made 5 mm above the mucogingival junction from the lateral incisor to the first molar ( Fig. 23.5 ). Care is taken not to enter the buccal fat pad unless a buccal lipectomy is part of the treatment plan. It is important to keep subperiosteal dissection limited to the minimal degree necessary to perform the procedure to avoid postoperative soft tissue ptosis. A linear osteotomy is made with a reciprocating saw or side-cutting bur to make a vertical cut in the anterior zygomatic body. If anterior narrowing is to be achieved, a parallel vertical osteotomy can be made adjacent to the first cut, and the distance between the parallel osteotomies corresponds to the degree of anterior narrowing ( Fig. 23.6 ). The posterior zygomatic arch may limit the degrees of freedom in moving the anterior zygoma, and to free zygoma mobility, an osteotomy can be made with an osteotome or a reciprocating saw in the posterior arch. This can be done either intraorally or through a percutaneous incision near the posterior arch. After placing the zygoma in its intended position, it is important to rigidly fix the malar bones. Any mobility applied across the osteotomy from masseteric forces could lead to a nonunion if fixation is not secure. If any edges are apparent after fixation, a bur can be used to smooth the edges.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree