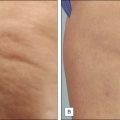
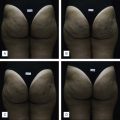
The etiology of cellulite has long been debated and several mechanisms have been proposed. While still controversial, understanding the pathophysiology behind cellulite is key when developing potential therapeutic treatments. This chapter will discuss mechanical techniques for the reduction of cellulite. To begin, it is important to underline the beneficial mechanism behind these types of treatment.
- •
Cellulite is a multifactorial condition which benefits from a combination approach to treatment
- •
Reduced blood flow and lymphatic drainage, which worsen the appearance of cellulite, can be improved by mechanical manipulation
- •
Mechanical manipulation, while beneficial as a safe, noninvasive technique, does not result in the permanent resolution of cellulite
Several mechanisms exist leading to the hypothesized benefit of treatment with mechanical techniques. Cellulite is thought to be, in part, a kind of local edema due to water retained in the skin by an increase in glycosaminoglycans (GAG) in skin overlying cellulite areas, possibly due to estrogen-activated fibroblasts increasing GAG synthesis. Increased GAG leads to an increased osmotic pressure and fluid retention. This is further aggravated by compressing small vessels, leading to reduced vascular flow and lymphatic drainage. Reduced blood flow along with compression of capillaries by adipocytes then leads to tissue hypoxia, local inflammation and increased collagen synthesis as well as inducing a local fibrotic response. This compression of capillaries by fat cells and arteriolar congestion was demonstrated in a photomicrograph of adipose tissue. It has also been noted that activation of hypoxia-inducible factor, HIF1A, correlates with the appearance of collagen septa and that individuals with a rare mutant allele of this gene are protected from the development of cellulite. Furthermore, cellulite has been associated with the presence of a specific polymorphism in the gene encoding angiotensin I converting enzyme, which then leads to increased angiotensin II formation resulting in reduced blood flow in the subcutaneous adipose tissue (SAT).
In addition to reduced vascular and lymphatic flow, cellulite worsens with age as a result of thinning of the dermis. This suggests that increasing the thickness of the skin may lead to improvements in the appearance of cellulite. Lastly, ultrasound shows herniation of fat into the dermis, identifying a possible benefit from treatments that result in SAT remodeling.
Endermologie ®
LPG ® Endermologie ® was developed by Louis Paul Guitay in 1970. Originally used for the treatment of scar tissue and trauma, it was quickly realized that this device may also have a beneficial effect on the appearance of cellulite. It has been cleared by the Food and Drug Administration (FDA) as a noninvasive massage system for the treatment of cellulite. This treatment works by creating positive pressure from rollers combined with negative pressure from aspiration influencing subcutaneous adipocytes. This mechanical strain is hypothesized to sublethally damage subcutaneous adipocytes, so they remodel with a better distribution of subcutaneous fat leading to an improved contour of the skin.
The Endermologie device consists of a treatment chamber with an aspiration system and two independent motorized rollers that roll and unroll skin folds. The treatment course consists of once- or twice-weekly treatment sessions lasting 10–45 minutes each. Wearing a special suit, which covers the patient’s entire body except the face, neck, hands and feet, the patient lies in prone and supine positions as well as on their side to facilitate massage of the entire body.
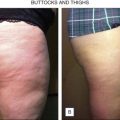
In a study, 118 women aged 19–63 years underwent twice-weekly treatments for 15 total treatment sessions, each lasting 35–40 minutes. Efficacy was graded using the Nürnberger–Müller scale ( Table 13.1 ). By analyzing photographs of the hips and thighs before and after treatment, blinded dermatologists found a statistically significant improvement in cellulite. Of the 19 subjects starting with grade 3 cellulite, 63% improved to grade 2. Furthermore, 54% of the 51 subjects with grade 2 cellulite improved to grade 1. No improvements were detectable in patients beginning with grade 1 cellulite; however, only four subjects were graded at this level, and thus the sample size was very small. Overall, 53% of patients achieved a reduction in cellulite. Furthermore, 99% of subjects had an overall reduction in average body circumference suggesting an additional benefit from this device. Lastly, data from a subjective, questionnaire-based response demonstrated that only 4% of subjects were not satisfied with their cosmetic outcome, while 69% expressed high patient satisfaction. Patients were monitored for adverse effects at each visit and no irregularities, bruising, telangiectasia formation, dimples or other serious side effects were noted.
| 0 | No or minimal alterations on skin |
| 1 | Orange peel appearance on the skin by pinch test or muscle contraction |
| 2 | Orange peel appearance at rest |
| 3 | Orange peel appearance at rest + raised areas and/or nodules |
Based on the study results, this treatment seems to be a well-tolerated technique for temporarily reducing cellulite and body circumference and is best for moderate to severe cellulite. This technique is safe for all skin types, but should be avoided in anyone pregnant, with serious heart defects, or any type of malignancy.
Acoustic wave therapy
The acoustic wave therapy (AWT) system utilizes compressed air to form acoustic waves on target tissue. Pulses are generated by accelerating a projectile with pressurized air that strikes against a stationary surface, the vibration transmitter, generating acoustic waves, which propagate directly to target tissue. These waves are intended to stimulate metabolism and enhance circulation along with stimulating neovascularization and cell proliferation. Furthermore, collagen remodeling is stimulated within the dermis as a result of the increase in cell proliferation and release of growth factors.
The AWT device uses two transmitters. A high impact acoustic wave handpiece (C-ACTOR ® ) is used to increase cell wall permeability to enhance the release of triglycerides. The vibrating massage handpiece (D-ACTOR ® ) generates slow impact acoustic waves, stimulating the target tissue as well as enhancing blood and lymphatic flow. Before initiating treatment, a gel is applied to the skin to reduce energy loss and reduce friction as the device is moved across the skin. The high impact handpiece can be set at an energy level from 0.45 to 1.24 mJ/mm 2 depending on the sensitivity of the patient. The vibrating handpiece is set at an energy level of 1.4–5 bar. The handpiece is moved with slight pressure in contact with the skin towards lymph nodes and backwards without pressure in a centripetal direction.
In one study, 11 patients were treated once a week for a total of eight treatments to the thighs and buttocks versus a placebo group of six patients. Assessments took place at baseline, before the last treatment and at 1 and 3 months following the last treatment. Measurement of efficacy was based on a patient questionnaire and both standard (two-dimensional) and three-dimensional photography. Out of the 11 treated patients, nine saw an improvement in the number and depth of dimples, eight visualized improvements in skin firmness and 10 noted improvements in skin texture. Standard photography was evaluated by blinded observers using the Modified Hexsel Scale which grades cellulite from 0 to 12. A statistically significant reduction in cellulite was assessed in the treatment group at 3 months following the last treatment, while no differences were identified in the placebo group. A study by Christ et al. further evaluated cellulite reduction as well as improvements in skin elasticity. Participants were divided into two groups, one group receiving six treatment sessions over the course of 3 weeks and the other receiving eight treatment sessions over 4 weeks. Improvements in skin elasticity were seen in both groups, with a larger increase in the second group. This indicates that doing more treatments may have an additive effect to end results. Skin elasticity in the first group showed 45% and 75% increases at the 3- and 6-month follow-ups, respectively, whereas the second group had 95% and 105% improvements, at 3 and 6 months’ post-treatment, respectively. Furthermore, based on ultrasound assessments, a change was detected in the collagen and elastin network within the dermis while the subcutaneous tissue became denser. These changes in elasticity are best seen in older individuals who already have poor elasticity. Adatto et al. treated female patients with six treatments over 4 weeks, each receiving 3000 pulses. Follow-up appointments were conducted at 1 and 12 weeks following the last treatment. Consistent with the previous study, treatments resulted in statistically significant improvements in skin elasticity, as well as decreased depth of cellulite dimples. By the 12-week follow-up, further improvements were seen, indicating both a short and relatively long term effect.
AWT is a localized, noninvasive, and safe therapy. No major adverse effects were noted, although mild pain and reddening of the skin during treatment is a possible side effect. Redness generally self-resolves within a few hours. Continual improvement is noted for up to 3 months, indicating at least temporary results. Longer term follow-up studies are required to determine the length of efficacy and proper maintenance intervals as AWT is not a permanent solution. As outcomes were not affected by differences in demographic data, this seems to be an effective treatment for a diverse group of patients.
Combination therapy
VelaSmooth™
VelaSmooth™ is a noninvasive system, cleared by the FDA for improving cellulite. It combines infrared (IR) light (700–2000 nm wavelength), bipolar radiofrequency (RF), suction and massage. The combination of RF with optical energy reduces the amount of optical energy required for effective tissue heating and allows for the use of the device on most skin types as RF does not target pigment. Cellulite has a multifocal pathology and combination approaches have the ability to effectively treat different areas of involvement simultaneously. Within this device, RF targets the collagen septa, while IR and RF together induce dissociation of oxyhemoglobin, allowing oxygen to be available for fat metabolism. Additionally, physical manipulation improves cellulite by increasing circulation and stretching connective tissue surrounding SAT. Altogether, this system may alter the architecture of fat protrusion and improve lipolysis.
Prior to treatment, the skin should be cleaned and a conductive lotion should be applied to moisturize the skin. Lotion does not need to be reapplied during treatment unless it becomes difficult to move the applicator across the skin. It is important to make sure that the applicator is sealed to the skin throughout the treatment session and air being sucked into the applicator should not be audible. Each area should be treated for 5 minutes with three to six passes per area. The target endpoint is significant erythema and warmth, 40 °C to 42 °C, maintained for 5–10 minutes. Total treatment time is about 20–30 minutes for each side of the body. Treatments are recommended once a week for 4–6 weeks. The highest levels of IR light and RF energy should be used as tolerated by the patient; however, all treatment levels should never be set to their maximum parameters simultaneously. The range of treatment parameters available is listed in Table 13.2 . The vacuum device should be set to a level of 1–2. In Fitzpatrick skin types IV–VI or in very tanned skin, IR light should be set to 1 or 2. If the patient does not experience lasting erythema or excessive heat, the level may be increased to 2 or 3.
| RF power | 10–100 W |
| Optical power | 10–100 W |
| Light spectrum | 680–1500 nm |
| Vacuum level | 150 mbar |
| RF | 1 MHz |
Several studies have been conducted on this device ( Table 13.3 ). Alster and Tanzi treated 20 patients with eight 30-minute sessions to the thighs and buttocks. Patients received treatments twice a week for 4 weeks with assessments at 1, 3 and 6 months following the last treatment. Improvements in the appearance of cellulite were seen in 90% of patients, with a mean improvement of 50% at 1 month following the last treatment. Patients were satisfied with the treatment and all but one were interested in subsequent treatment to the control leg. Improvements were best at 1 month follow-up and still visible 6 months after the last treatment, indicating a need for ongoing treatment intervals to maintain results.
| Study | Treatment sessions | Treatment parameters | Treatment assessment | Overall cellulite improvement | Average improvement score |
|---|---|---|---|---|---|
| Alster & Tanzi | Twice weekly for 4 weeks | 20 W RF 20 W IR | Quartile scale (similar to Sadick & Mulholland) | 90% | 1.82 at 1 month 1.4 at 3 mos 1.1 at 6 mos |
| Kulick | Twice weekly for 4 weeks | 20 W RF 12.5 W IR | Investigator-graded | 100% | 62% at 3 months 50% at 6 months |
| Sadick & Magro | Twice weekly for 6 weeks | Variable | Investigator-evaluated Quartile-based scale | 50% had >25% improvement | 6% had >50% improvement at 4 weeks 25% had >50% improvement at 8 weeks |
| Sadick & Mulholland | Group 1: twice weekly for 4 weeks Group 2: twice weekly for 8 weeks | Max. 20 W RF Max. 20 W IR | Investigator-evaluated Quartile-based scale | 100% | Group 1: 5% had >50% improvement at 4 weeks Group 2: 36% had >50% improvement at 4 weeks |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree