Mandibular Area and Neck
OVERVIEW
Many of the conditions seen on the chin and neck represent an extension of disorders found on the face, scalp, or trunk. Acne, folliculitis, and pityriasis rosea are common examples. Benign neoplasms such as skin tags, small seborrheic keratoses, and acanthosis nigricans also frequently appear on the neck.
On the chin and neck, folliculitis barbae (“shaving bumps”) and acne lesions present problems for men who shave. Pseudofolliculitis barbae (PFB) is especially a challenge for black men. The chin, beard area, and neck are also subject to bacterial (staphylococcal folliculitis) and, less frequently, fungal (sycosis barbae) and viral folliculitis (herpetic) infections. The beard is also a common site for alopecia areata to appear in men.
The area under the chin and other shaded areas, such as those covered by long hair, are shielded from chronic sun exposure and are generally spared from sun-related disorders and malignant neoplasms. Basal cell carcinomas and squamous cell carcinomas, when they do arise on the neck, usually occur in men in areas that are chronically sun-exposed—the nape, “V,” and lateral neck.
Acne keloidalis nuchae, a disorder that appears most often in black men, is noted on the posterior neck and occipital area. The posterior neck is also often a focus for chronic pruritus and lichen simplex chronicus.
Furuncle (“Boil”)/Carbuncle
A furuncle, commonly referred to as a “boil,” is a deep infection of the hair follicle that usually develops from a preceding folliculitis. It is most frequently seen in children and adults. Coagulase-positive Staphylococcus aureus is the responsible pathogenic bacterium in most cases. Furuncles arise more commonly in patients who are diabetic, obese, or immunocompromised.
The furuncle typically presents as a tender red nodule found in hairy areas of the body. If untreated, it can drain spontaneously or enlarge and become increasingly tender. When multiple furuncles coalesce, the lesion is called a carbuncle. Furunculosis may become recurrent in cases where patients are carriers of S. aureus or when there is ongoing transmission among close contacts.
Distinguishing Features
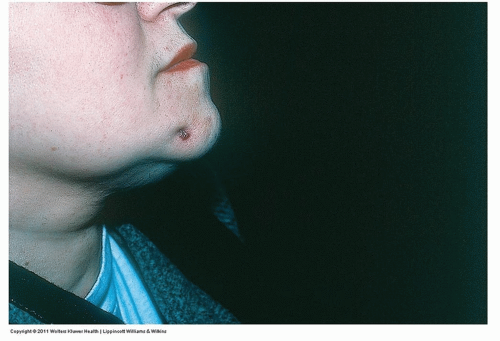
Gradually a subcutaneous nodule becomes fluctuant and develops central suppuration (Fig. 10-1)
Often quite tender
Carbuncles are furuncles with multiple “heads” (Fig. 10-2)
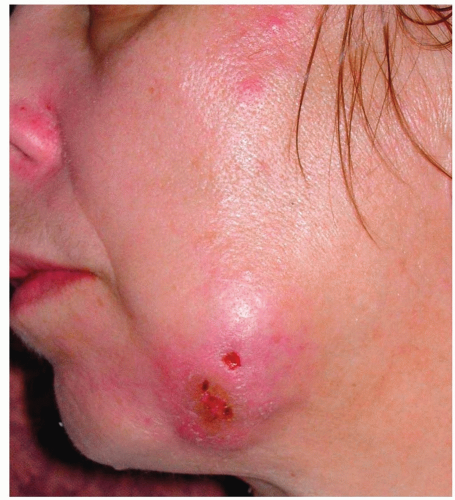 Figure 10-1 Furuncle (“boil”), carbuncle. Multiple furuncles formed this carbuncle on this patient’s jawline. (Figure courtesy of Miguel R. Sanchez, MD.) |
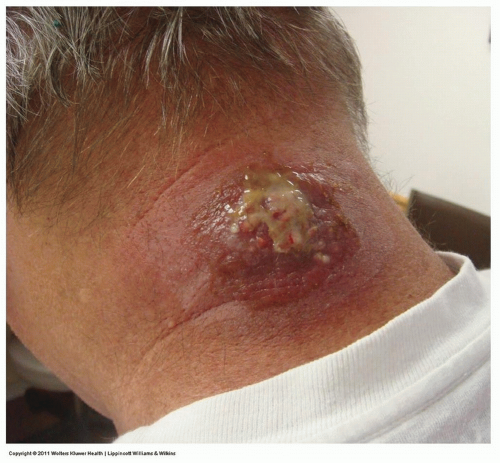 Figure 10-2 Furuncle (“boil”), carbuncle. Note the contiguous cluster of purulent furuncles on the posterior neck in this patient. |
Management
Incision and drainage is the primary treatment for single, simple boils
Warm compresses or soaks can help to encourage spontaneous drainage
Bacterial culture should be sent, especially if the patient will be treated with antibiotic therapy
Systemic antibiotics are recommended for extensive disease or for multiple sites of infection
In children, first-line antibiotics include dicloxacillin (12.5 to 25 mg/kg/day divided q6 hours) or cephalexin (25 to 50 mg/kg/day divided q 6-12 hours)
For recurrent furunculosis, treatment includes one of the following decolonization strategies: Mupirocin (Bactroban) ointment intranasally twice daily for 5 days, monthly for 3 months; a skin antiseptic solution (e.g., chlorhexidine) for 5 to 14 days or dilute bleach baths. An oral antibiotic in combination with rifampin (if the strain is susceptible) may be considered for decolonization if infections recur despite above measures
Odontogenic Sinus
An odontogenic sinus (dental sinus) is an abnormal channel that drains from a longstanding intraoral abscess associated with a necrotic or dead tooth. The sinus may drain to the inside of the mouth (an intraoral sinus) or to the skin surface of the face or neck (an extraoral sinus). Because an active toothache is usually absent when the skin lesion is noted, the patient frequently goes to a doctor rather than a dentist.
Distinguishing Features
May present as a persistent, painless draining furuncle-like papule with or without an overlying crust (Fig. 10-3)
Management
Referral to an endodontist
This condition is often resolved by endodontic treatment and does not have an indication for antibiotic use
These lesions are frequently misdiagnosed and treatment is often delayed.
Poikiloderma of Civatte
Poikiloderma of Civatte is a common condition that occurs primarily in middle-aged, fair-skinned women who have experienced long-term sun exposure. This finding symmetrically involves sun-exposed areas such as the sides of the neck and lateral aspect of the cheeks.
Poikiloderma of Civatte characteristically spares the area under the chin and other shaded areas, such as those covered by long hair. Other contributing factors include photosensitizing components of cosmetics and toiletries, especially perfumes, and hormonal changes related to menopause.
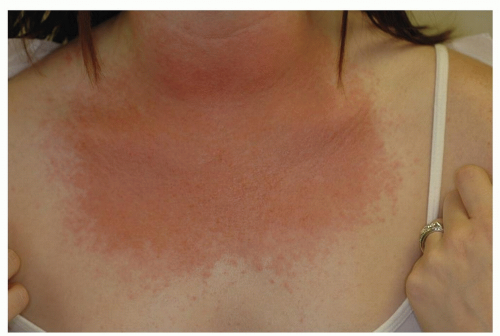
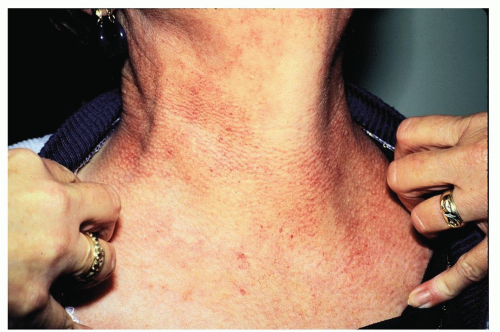 Figure 10-4 Poikiloderma of Civatte. The persistent erythema in this patient is characteristic. Note sparing of the shaded areas under the chin. (Image courtesy of Robert I. Rudolph, MD.) |
Distinguishing Features
Most commonly occurs in middle-aged or elderly females
Erythema associated with a mottled hyperpigmentation located on the sides, and “V” of the neck (sun-exposed areas) (Fig. 10-4)
The term poikiloderma refers to a change in the skin where there is thinning, increased pigmentation, and dilation of the fine blood vessels (telangiectasia)
The shaded submental and submandibular areas are spared
Diagnosis
Clinical
Management
It is mainly a cosmetic concern to patients
The patient should be advised about avoiding sun exposure and the proper use of sunscreens to prevent further skin involvement
Avoidance of all perfumes on or near the affected area
Hydroquinone-containing preparations may help fade areas of hyperpigmentation
Although there is no totally effective medical treatment, the pulsed-dye laser has been noted to decrease the redness of this condition, and intense pulsed light treatments help to reduce the telangiectasia and pigmentation
Polymorphous Light Eruption
Besides sunburn, polymorphous light eruption (PMLE) is the most frequently seen acute skin reaction caused by ultraviolet (UV) exposure. It generally occurs in adult women aged 20 to 40 and is more common in those who are fair skinned.
PMLE is thought to be caused by an immune reaction to a compound in the skin that is altered by exposure to UV radiation. It is usually provoked not only by short-wavelength UVB but also longer wavelength UVA.
The term polymorphous stems from the wide spectrum of clinical lesions that occur in various patients (“different patterns in different patients”); however, the lesions in any one patient tend to be relatively uniform. PMLE is usually most prominent following the first sun exposure in the spring, early summer, or during a winter trip to a sunny climate. The rash appears hours to days after exposure, lasts for several days, and resolves spontaneously. There is often some degree of “hardening” after continuous exposure after which more sun can be tolerated without a rash.
Distinguishing Features
Usually seen in women
On different patients, lesions may be papules (most common), papulovesicles, erythematous plaques, erythema multiforme-like, or purpuric
Usually only one morphology dominates in a given individual
The rash appears within hours to days of exposure, and it subsides over the next 1 to 7 days
The areas of greatest involvement are the “V” areas of the neck and chest (Fig. 10-5) and particularly the extensor surfaces of the arms. Curiously, the face is usually spared
Most patients experience pruritus, while others describe stinging and pain
Typically, the lesions of PMLE first erupt with the first seasonal exposure to the sun and disappear gradually over time