Introduction
Reconstruction of the face after burn injuries presents some of the most complex and formidable challenges in plastic surgery. Facial burn wounds and deformities and their treatment often have lifelong repercussions for the patient. Unlike any other body part, the face is a unique and fundamental component of an individual’s identity and personality. Alimentation, breathing, communication, and emotional expression depend on functional facial anatomy. Disfigurement and impaired function can significantly impact a patient’s self-image, emotional well-being, social engagement, and productivity. To successfully treat postburn facial deformities, the surgeon must possess technical mastery, sound clinical judgment, and a deep understanding of wound healing and scar progression. They must also be proficient in nonsurgical treatments such as topical agents, pressure therapy, laser therapy, and laser-assisted drug delivery (LADD). Specialized burn care infrastructure and an experienced multidisciplinary team, including skilled nurses, occupational and physical therapists, psychologists, and social workers, are critical to effectively treat and support patients and their families during what is often a long recovery and rehabilitation process. , The surgeon plays a leading role in restoring facial function and appearance by collaborating with these team members and working closely with patients to align goals and expectations.
In the last 100 years, the approach to assessing and treating burn scars and contractures has evolved because of new insights into burn pathophysiology and technologic innovations. These advances have considerable implications for the face, where normal appearance and function are paramount. Facial scars and deformities, even when small, can be consequential and debilitating. The constricted and deformed tissues resulting from burns alter the face’s features, proportions, and expression. Other sequelae include changes in skin texture and pigmentation. Ultimately, the primary goal of reconstruction is to create a tension-free appearance and reestablish the features, proportions, and expression of the face. It should not be to remove scars surgically. In treating soldiers injured during World War I, Sir Harold Gillies, the father of modern plastic surgery, began pursuing scarless burn reconstruction by replacing facial burn scars with tubed pedicle flaps ( Fig. 58.1 ). This brilliant surgical innovation was premised on the idea that scar replacement with flaps of normal skin produces better outcomes than rehabilitated scarred skin or skin grafts. , Aided by advances in anatomic knowledge and surgical techniques like microsurgery, many surgeons adopted Gillies’s concept and pursued increasingly larger scar excisions and flap closures. Scar removal, in effect, became a goal of burn reconstruction. Skin grafting after scar excision also evolved and became more frequent as improved grafting techniques and devices were popularized. Unfortunately, history has shown that in many facial burn cases, excision and closure can lead to new deformities that make patients appear even worse off rather than restored more closely to their preinjury condition ( Fig. 58.2 ). , Replacement of facial scars with uninjured tissue creates iatrogenic donor sites on other areas of the body. Such surgery is typically complex and can potentially result in severe complications. Furthermore, replacing a scar with another scar can lead to new tension and distortion of facial landmarks.
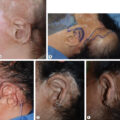
(A) World War I British Army soldier with facial burn scars in 1918. (B and C) Sir Harold Gillies excised the scars and replaced them with a tubed pedicle flap of abdominal skin. The flap resulted in a beardless left face with different colored and textured skin. There is a slight lateral and upward contracture of the left oral commissure. The linear hypertrophic scars seen in (A) would have been ideal tissue for Z-plasties and laser therapy.
(From Gillies HD. Plastic Surgery of the Face Based on Selected Cases of War Injuries of the Face Including Burns with Original Illustrations . H. Frowde; 1920:369–371.)
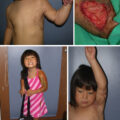
(A) Young male with extensive hypertrophic burn scars to the right face. (B–J) Facial deformity resulting from scar excision and advancement flap. Note the right oral commissure displacement, right lower-eyelid scleral show, blunting of the cervicomental angle, and mandibular growth discrepancy, likely all related to increased tension on the right face.
Successful restoration of form and function in patients with facial burns depends on accurate and early diagnosis, conservative management, and the application of classic and modern surgical techniques and minimally invasive or noninvasive scar therapies. Leveraging Z-plasty and a laser’s ability to regenerate and remodel skin makes more aggressive surgical approaches unnecessary and counterproductive in many cases. By adhering to a thoughtful and methodical treatment plan that aims to reestablish appropriate facial animation and a tension-free visage, one can achieve impressive outcomes and avoid iatrogenic catastrophes, even in patients with the most devastating burn deformities.
Epidemiology
A limited number of studies focus on the epidemiology of facial burns. According to various reports, the most common site of burn injury is the head and neck, with a prevalence that varies from 6% to 66%. This range is likely attributable to differences in healthcare settings, population, and facial burn definition, among other factors. Flame and scald are the two most common causes of facial burns, with flame burns more common in adults and scald burns more common in children younger than 5 years. Age (young children and working-age adults), male sex, and more prominent total body surface area (TBSA) burn are risk factors. , Hoogewerf et al. found that patients were more likely to undergo facial reconstruction if their injury was to the ventral aspect of the neck, was caused by fire/flame, or if they underwent facial surgery during acute treatment. Because of advances in burn care in recent decades, there has been a decline in burn incidence, burn severity, length of stay, and mortality rate worldwide. These trends have been most notable in highly developed countries, but the data are less consistent in highly and medium-developed countries. ,
Goals of reconstruction
The prolonged time course of wound healing and scar evolution and the frequent need for multiple surgeries for severe facial burns warrant a surgical strategy for facial deformities that takes a long view. The plan for reconstruction established during the acute period will inevitably be influenced by the severity of a patient’s injuries and the anticipated trajectory of wound healing and scar formation. However, as a patient recovers and rehabilitates, the fundamental goals of reconstruction remain unchanged. According to Donelan, the primary objective is to create a tension-free appearance and reestablish the features, proportions, and expression of the face. It is not to surgically remove scars, as in many cases, scars can be successfully transformed using noninvasive treatments or less complex surgeries such as Z-plasties with or without laser therapy. Rose stated that enhancing aesthetic appearance is equally important as mitigating functional impairment. He provided five goals for aesthetic facial restoration: (1) an undistracted “normal” look at conversational distance, (2) facial balance and symmetry, (3) distinct aesthetic units fused by inconspicuous scars, (4) “doughy” skin texture appropriate for corrective makeup, and (5) dynamic facial expression. Discussing and clarifying treatment goals with patients and family members is essential to maintain realistic expectations. Including patients and family members in the planning process helps educate them and provides perspective about the arduous journey that can be expected. A patient who is appropriately invested in the surgical plan and understands the short- and long-term goals is more likely to be pleased with the eventual outcome of the reconstruction. The surgeon and the rest of the care team are responsible for instilling hope and optimism in patients and their families.
Acute management
Accurate assessment of burn wounds and their healing potential during the acute phase ensures a surgical plan is developed that can achieve an optimal functional and aesthetic outcome. Meticulous and informed decision-making during the early postinjury period can minimize scar formation and potential complications. Initial assessment of the facial burn patient should follow the principles of advanced trauma life support, given the high potential for airway injury. After acute stabilization, restoration of function is the next priority. For example, issues such as eyelid ectropion and microstomia should be addressed before cosmetic concerns ( Fig. 58.3 ).
(A) 7-year-old child with third- and fourth-degree facial burns. Open wounds of forehead and scalp were present months after the initial injury was treated in his home country. Open wounds led to full-thickness loss of the lower lip and devastating contractures and contraction of multiple areas, most dramatically the upper and lower eyelids, lips, and cheeks. Note the bilateral upper-eyelid ectropion. (B) Upper eyelids were released and grafted with split-thickness skin grafts. Cosmetic issues were addressed later in the recovery period.
Initial evaluation
The mechanism of injury, the extent of tissue trauma, and the viability and regenerative potential of wounded skin all influence the surgical strategy. Although early excision and grafting of deep partial-thickness and full-thickness burns is standard of care, this approach is less straightforward for the face because of the challenges of evaluating facial burn depth and correctly predicting a patient’s long-term functional and aesthetic status. Burn wounds are often heterogenous, making it challenging even for experienced surgeons to precisely diagnose their depth by observation alone, especially for wounds of indeterminate depth. Laser Doppler imaging (LDI) has been validated for objective and accurate burn depth assessment and can help prevent excessive excision. Although it is FDA approved, LDI’s adoption has been slow because of cost, ongoing skepticism, and organizational constraints. ,
Inflammation and infection
The resultant acute inflammatory state caused by burn injuries puts these patients at high risk for infection and sepsis. Injury to the skin, the primary barrier against the external environment and microorganisms, puts these patients in a continuous immunocompromised state. Possible infections include but are not limited to pneumonia, bloodstream infections, catheter-related infections, urosepsis, central venous catheter infections, burn wound infections, and necrotizing soft-tissue infections. Standard markers of sepsis, such as fevers, leukocytosis, tachycardia, and tachypnea, are altered in the burn patient and thus poor indicators of sepsis. As a result, a consensus conference by the American Burn Association determined that the Marshall Multiple Organ Dysfunction Scoring System was the best system to be used and should not be calculated until the acute phase of resuscitation (after day 3) is complete.
Persistent infection can stagnate the wound healing cascade, resulting in defective new extracellular matrix, decreased angiogenesis, and impeded reepithelialization. Colonization and infection of facial burn wounds can limit the use of acellular dermal matrix (ADM) in reconstruction. Topical antibiotics can help mitigate inflammation of infected burn wounds. However, the evidence for systemic steroids and nonsteroidal antiinflammatory drugs controlling local inflammation is less clear.
Antibiotics
Multidrug-resistant bacteria are common in the burn population secondary to heavy antimicrobial therapy, prolonged length of stay, colonization, and invasive medical monitoring (e.g., central venous catheters, Foley catheters). There is a low threshold for initiating empiric broad-spectrum antibiotics in burn patients with suspected infection. Antibiotic regimens are variable and dependent on patient history, colonization, and the institution’s antibiogram and susceptibilities. For example, significant Staphylococcus aureus resistance has been built against previously effective antibiotics such as ciprofloxacin and penicillins.
Topical antibiotics are the cornerstone of the treatment of facial burn wounds. However, a recent systematic review concluded that there is primarily low or very low certainty evidence of the effects of topical agents on wound healing in patients with facial burns. Silver-based compounds are the most recommended first-line topical agents for partial- and full-thickness burn wounds. Various antimicrobial wound dressings incorporate silver, and all have advantages and disadvantages. The newer generation of products contains nanocrystalline silver that elutes the metal over several days.
Silver sulfadiazine (Silvadene) has been widely adopted as an initial treatment, given its ability to reduce sepsis and mortality associated with burn wounds. It is a broad-spectrum sulfonamide-containing bactericidal agent effective against gram-positive and gram-negative bacteria, including Pseudomonas aeruginosa and some yeasts. It has an excellent safety profile, good eschar penetration, and limited systemic absorption and effects. Despite its strengths and rare toxicity, silver sulfadiazine’s application on facial wounds can be tricky, as it can irritate the eyes and mucosal surface of the lips and mouth. Additionally, a pseudoeschar can form with repeated use, masking the wound and preventing proper assessment. ,
Mafenide acetate (Sulfamylon) is a broad-spectrum bacteriostatic topical agent against gram-negative bacteria, including P. aeruginosa, but it has limited activity against gram-positive bacteria such as S. aureus . It is available as both a solution and a cream. It is commonly used acutely on full-thickness burns and burns with eschar and after excision over skin grafts. Mafenide acetate has excellent eschar penetration and efficacy in preventing and controlling wound sepsis but retards wound healing by slowing reepithelialization. It can be painful and can form neo-eschar when applied in higher concentrations. It can also lead to metabolic acidosis when used in large areas. The 5% mafenide acetate solution reduces these side effects and is the most commonly used formulation.
Mupirocin (Bactroban) ointment is bactericidal against penicillinase-producing and methicillin-resistant strains of S. aureus but is ineffective against most aerobic gram-negative bacteria and anaerobes. The ointment has minimal tissue penetration and results in no inflammatory response. It is the optimal first topical antibiotic to use on facial burns. The cream formulation is less commonly used as it can cause local inflammation.
Bacitracin is a topical antibiotic that provides an alternative to silver sulfadiazine in patients with a sulfa allergy. Bacitracin can be applied as part of a triple therapy ointment with neomycin and polymyxin B, but this treatment is typically less effective than mupirocin.
Primary excision and coverage
Early excision and grafting are the standard of care for burns, culminating in the seminal work of Jackson, Janzekovic, Monafo, Burke, Tompkins, and Herndon. , However, even for experienced surgeons, accurate removal of necrotic tissue while preserving healthy tissue is challenging, especially for mixed-depth wounds. Excessive debridement of facial burns has considerable implications for the face’s eventual appearance and function. As such, one must approach the excision of facial burns differently from wounds on the rest of the body. Multiple studies have demonstrated the safety and efficacy of bromelain-based enzymatic debridement (BBED) for deep partial- and full-thickness burns. , This technique has become more widely adopted in the last decade as it selectively removes eschar while maximally preserving viable tissue. Most studies have focused on BBED in areas other than the face. In 2017, Schulz et al. reported multiple benefits from BBED in patients with facial burns treated with BBED compared with those who underwent excisional debridement.
Most facial burns heal within 3 weeks without surgical debridement, requiring only daily wound dressing changes and topical antibiotics. Full-thickness burns require early excision and grafting within 7 to 10 days to expedite wound closure and diminish contractile forces ( Fig. 58.4 ). The optimal treatment strategy is less clear for wounds that have not healed by 3 to 4 weeks. Proponents of a more aggressive approach argue that excision and grafting can facilitate healing while mitigating scars and contractures. Outcomes achieved with excision and grafting have been noteworthy. Those who favor a conservative strategy assert that excision and grafting may prevent a patient with a grafted face from having the opportunity to epithelialize and heal their partial-thickness wounds. The conservative approach has demonstrated excellent outcomes and is generally preferred. It has been enhanced by numerous therapies now available that facilitate scar remodeling, including silicone, pressure, massage, 3D-printed face masks, topical and intralesional steroids, vitamin E, 5-fluorouracil, pulsed dye lasers, ablative fractional CO 2 lasers, LADD, and electrophotobiomodulation. Most facial burns can be managed conservatively, limiting excision and grafting to full-thickness burns. Grafting should be reserved only for patients with this treatment, which is the best option.
(A–C) Panfacial full-thickness burns requiring primary excision and coverage with split-thickness skin grafts. (D) About 6 weeks after skin grafting. (E) Nine and a half years after burn injury and multiple reconstructive flaps and grafts.
Pathogenesis
Burn depth largely determines the degree of scarring, contraction, and pigmentary changes. Superficial second-degree burns typically do not result in scarring with dyspigmentation. Second-degree burns that are somewhat deeper usually epithelialize in 10 to 14 days. In rare cases, they can lead to scarring and dyspigmentation ( Fig. 58.5 ). The evolution of deep second-degree burns that require 21 days or more to epithelialize is less specific, although these burns are predisposed to develop hypertrophic scars. The greater the severity of a burn, the more contraction is evident during the healing phase. In patients who begin to exhibit early scarring, suppressive therapies should be initiated as soon as possible. When indicated, options include laser, silicon, pressure, intralesional corticosteroids, and tension-releasing local tissue rearrangement, such as Z-plasty. Full-thickness facial burns are typically treated with excision and grafting.
(A) Secondary healing and dyspigmentation years after second- and third-degree facial burns. (B) Late treatment for dyspigmentation is recommended to allow time for possible repigmentation. If this does not occur, then can treat with dermabrasion and thin epithelial grafting, as was done in this patient.
Evaluation of facial burn deformities
Developing an appropriate plan for reconstructing facial burn deformities requires a thorough evaluation and a clear understanding of the critical issues. First, one must identify the area of the problem and distinguish scars from contractures. In many cases, scars should not be excised and replaced with tissue from elsewhere on the body. Instead, laser therapy and local tissue rearrangement can significantly improve scar elasticity, morphology, and camouflaging with adjacent tissues. Scar excision should be avoided, especially in the early phases of scar maturation. This thinking influences how one evaluates scars and what surgical and nonsurgical strategies can be pursued.
The assessment of facial burn deformities is unique compared with other areas of the body, given the intricacies and complexities in facial anatomy and the delicate balance of treating both form and function. These deformities should be evaluated individually and together, as local reconstructive options can be compromised because of damaged surrounding tissue. Intrinsic and extrinsic contractures must be identified. Every deformity, scar, or contracture must be assessed for location, degree of alignment with relaxing skin tension lines, shape, length, contour, maturity, pigmentation, vascularity, and reconstructive options. Patient age and ethnicity also influence a scar’s characteristics and prognosis. If a deformity has already undergone a prior failed treatment, it is critical to understand what contributed to the suboptimal outcome so mistakes are not repeated.
Typical stigmata of panfacial burns that can develop secondary to contracture include lower eyelid ectropion, shortened nose with ala flaring, retruded upper lip with philtral column loss, lower lip eversion and inferior displacement, flattened facial features, and loss of jawline definition ( Fig. 58.6 ). In the most severe panfacial burn cases, many, if not all, of these stigmata are present. The majority of burns, however, are not panfacial but involve focal or diffuse scarring with or without contractures. These patients have largely normal-appearing faces. Any intervention must not distort the normal aspects of the face by establishing iatrogenic tension on tissues. Again, focal deformities can often be successfully treated with scar revision using Z-plasty, local flaps, and laser therapy. Focal contractures require tension-relieving modalities such as surgical release, skin grafting, Z-plasty, and tissue expansion.
(A and B) Severe burn deformities in 13-year-old female with 45% total burn surface area resulting from house fire. Note facial burn stigmata: left eye ectropion, shortened nose with ala flaring, retruded upper lip with philtral column loss, flattened facial features, and loss of jawline definition. (C and D) Appearance after 10 years of serial reconstruction, including extensive split-thickness skin grafts and full-thickness skin grafts, tissue-expanded chest flap to neck, and scalp flap to nasal tip.
After identifying the various deformities in patients with panfacial burns, the chosen surgical strategy should aim to restore normal facial proportions and the position and contour of standard facial elements. Contractures are often addressed in a calculated, stepwise manner, with the eyelids treated first, followed by the lower lip and chin, upper lip, cheeks, nose, and other deformities. Once these have been surgically corrected, scar revision and resurfacing can help obscure borders with normal skin and camouflage textural and pigmentary abnormalities. Generally, grafting to the neck should be carried out before grafting to the lips and face.
Principles of reconstruction and techniques
Aesthetic units
Facial aesthetic units are subunits characterized by similarities in skin tone, thickness, texture, mobility, hair distribution, and degree of subcutaneous tissue. Major aesthetic units of the face include the forehead, eye, eyebrow, nose, lips, cheek, and chin, which are further divided into additional subunits. This widely adopted concept was first described by Gonzales-Ulloa in 1956, who advocated restoring these units when considering reconstructive options ( Fig. 58.7 ). , Proponents of this concept favor staying within the lines of the subunits and not reconstructing them to minimize facial scars.
Facial aesthetic units (modified version of Gonzales-Ulloa’s units). (A, B) Frontal and profile views of the aesthetic units and subunits of the face. 1, Forehead unit (1A, central subunit; 1B, lateral subunit; 1C, eyebrow subunit); 2, nasal unit; 3, eyelid units (3A, lower lid unit; 3B, upper lid unit; 3C, lateral canthal subunit; 3D, medical canthal subunit); 4, cheek unit (4A, medial subunit; 4B, zygomatic subunit; 4C, lateral subunit; 4D, buccal subunit); 5, upper lip unit (5A, philtrum subunit; 5B, lateral subunit; 5C, mucosal subunit); 6, lower lip unit (6A, central subunit; 6B, mucosal subunit); 7, mental unit; 8, auricular unit; 9, neck unit.
(From Fattahi TT. An overview of facial aesthetic units. J Oral Maxillofac Surg . 2003;61(10):1207–1211.)
Firm adherence to this principle can lead to resection of entire subunits to maximize outcomes even if the defect did not involve the whole subunit. However, destroying normal or near-normal tissue in a subunit can potentially eliminate reconstructive approaches that use normal tissue or rehabilitated scars. Facial aesthetic units can be handy when planning for a significant contracture release. For example, an entire lower lip contraction is often released without removing any scar or normal tissue.
Contractures
Facial burn contractures and burn scars are distinct problems. Burn contractures form when a second- or third-degree burn wound epithelializes and contracts, thickening and tightening over time. They are often found on the face in areas of chronic tension and relaxation, such as perioral commissures, or chronic inflammation, such as chronic folliculitis resulting from ingrown beard hair. Contractures can present as linear or diffuse and be intrinsic or extrinsic to the involved anatomic part. Linear contractures exhibit a taut, narrow band, surrounded by softer or normal skin on one or both sides. Diffuse contractures are broad based and do not have a dominant band ( Fig. 58.8 ). Intrinsic contractures distort from within the affected area, whereas extrinsic contractures distort the affected area by putting tension on it from a distance. Frequently, contractures are not evident until one observes extremes of motion such as neck extension, head rotation left or right, or extreme mouth opening causing ectropion.
Diffuse extrinsic contractures resulting in (A) right eye scleral show and (B) bilateral lower eyelid ectropion.
Facial deformities resulting from contractures often lead to significant functional concerns, such as ectropion from eyelid contractures (intrinsic or extrinsic) or microstomia from oral commissure contractures. Ectropion responds well to tension release (e.g., neck contracture treated with release, skin grafting). Microstomia can often be improved with perioral local tissue rearrangements, such as Z-plasty or Y-V plasty without hypertrophic scar excision.
Linear contractures are often best addressed using Z-plasties and other scar-lengthening techniques. Multiple small Z-plasties in series are usually more effective than one large Z-plasty over the same length. Broad contractures can be addressed using a transverse releasing incision, placing a dart or a fishtail configuration at both ends. This technique results in a release defect most commonly filled with a full-thickness skin graft (FTSG). However, a thick split-thickness skin graft (STSG) can be used. STSGs are typically used in the acute phase, whereas FTSGs are usually employed in the chronic healing phase. In some cases, instead of skin grafts, one can employ a local transposition flap using uninjured skin adjacent to the contracture.
Z-plasty and local tissue rearrangement
The importance of Z-plasty in facial burn reconstruction cannot be overstated. It is the workhorse of burn scar revision, with roots in the 19th century. In 1837, W.E. Horner reported the first Z-plasty correcting ectropion caused by a 4-year-old burn scar ( Fig. 58.9 ).
Horner’s figures of his surgery to correct ectropion are considered the first reported case of a Z-plasty, although the term was not used until the early 20th century. In figure B, flap “a” was taken from the cheek and transposed to the lower eyelid. Pins were placed at “b” and “c” to keep the flaps in place.
(From Horner WE. Clinical report on the surgical department of the Philadelphia Hospital, Blockley for the months of May, June and July 1837. Am J Med Sci . 1837;21:105–106.)
In a local tissue rearrangement, tissue to treat the contracture is borrowed in one direction to lengthen in another, optimally placing more elastic skin across the tension line. The Z-plasty lengthens a scar, decreases its transverse dimensions by using two opposing triangular flaps of adjacent normal or near normal tissue, and transposes them along the scar axis. The classic Z-plasty has limbs of the same length with 60-degree angles for the triangular flaps, theoretically increasing scar length by 75% and narrowing it by 30% ( Figs. 58.10 and 58.11 ). , This technique changes a scar’s geometry and physiology by relieving tension placed on scar tissue and inducing collagen to break down and remodel. Ultimately, this surgical magic improves a scar’s elasticity and morphology and makes its borders irregular, helping it blend with the surrounding tissue. The various iterations of Z-plasty and other local tissue rearrangement techniques can flatten hypertrophic scars and raise atrophic scars. Intrascar Z-plasty also helps decrease chronic tension and dramatically resolve scar hypertrophy ( Fig. 58.12 ).
(A) Classic Z-plasty. (B) Serial Z-plasties resulting in elongation of the limbs and transposition of quadrangular flaps. (C) Two options shown for a Z-plasty: option “a” produces a better orientation of the flaps than option “b”.
(From Shockley WW. Scar revision techniques: Z-plasty, W-plasty, and geometric broken line closure. Facial Plast Surg Clin North Am . 2011;19(3):455–463.)
Theoretical increase in length of central limb in Z-plasty based on central limb-lateral limb angles.
(From McGregor IA. The theoretical basis of the Z-plasty. Br J Plast Surg . 1957;9(4):256–259.)
(A) Ten-year-old male with 40% total body surface area electrical and flame burn. (B) Left face hypertrophic scarring 2 years after injury. (C–E) Multiple intrascar Z-plasties to decrease tension on the scar. (F) Pressure therapy. (G and H) Four years after Z-plasties and two scar treatments with pulsed dye laser to decrease erythema.
Grafts
Skin grafting originated in ancient India when thick skin from the buttock was reportedly used to reconstruct a nasal defect. In the 1800s, grafting became integral to burn care with the research and innovations of Bunger, Warren, Reverdin, Pollock, Ollier, Wolfe, and Thiersch, among others. , When using a graft for reconstruction, various factors influence the outcome: use of split-thickness versus full-thickness skin, donor site location, timing of graft placement, and postoperative care of the graft. STSGs contract more than FTSGs and take on a wrinkly, shiny appearance. They are more susceptible to secondary contracture, which occurs while the graft is healing. FTSGs, which can grow hair, are more elastic and durable than STSGs and maintain a more normal, matte appearance. FTSGs are more susceptible to graft loss if placed on a compromised or infected wound bed or during acute care. Donor sites for FTSGs are limited compared with STSGs. Meshed grafts should be avoided in facial reconstruction as the mesh pattern causes a reptilian appearance and worsens secondary contraction.
STSGs are best used on the periphery of the face, and they are excellent for upper eyelid resurfacing. FTSGs are incredibly reliable and are most suitable for repairing central facial structures, including the upper and lower lips, lower eyelids, nasal dorsum, and cheeks ( Fig. 58.13 ). Donor site selection is essential for facial recipient sites, given the need to closely match the color, texture, and thickness. For example, donor sites for the face often include the supraclavicular region, nasolabial fold, auricular concha, pre- and postauricular skin, and neck. In severely injured burn patients, there are often limited donor sites, thus FTSGs are frequently reserved for final resurfacing or release.
Acid burn to right face, neck, and chest requiring treatment of external auditory meatus closure, ectropion, and nasal stenosis. (A) Scarring to nasal dorsum resulting from third-degree burn. (B) Full-thickness skin grafted onto the nasal dorsum with nasal stents in place. (C) Appearance about 1 year after graft placement. Patient eventually underwent forehead flap to nose to resurface external skin.
Regardless of the graft type, it must be immobile to ensure it adheres to the underlying tissue and heals properly. Snug bolsters that minimize graft motion are crucial to success.
Various biologic and synthetic skin substitutes have increasingly become integral to managing acute burns and burn reconstruction. These substitutes are especially valuable in treating patients suffering from extensive burns where skin graft donor sites are limited or unavailable. Most of these substitutes involve a two-step process of vascularization of the ADM followed by autografting.
Flaps
Flaps are an important reconstructive tool for facial burn deformities, but their limitations must be understood. Given the reduced secondary contracture, local flaps offer advantages over skin grafts in certain situations. However, flaps can still contract, compressing and obscuring underlying tissue morphology. Local flaps of normal skin facilitate an improved range of motion and elasticity across hypermobile areas such as perioral tissues and the neck. Additionally, local flaps provide closer color and texture matching than distant flaps. Local flaps should be the first choice for reconstruction if tissue adjacent to the deformity is normal or near normal.
Unfortunately, facial burn injuries, especially severe ones, often extend to the neck and chest and therefore eliminate many local flap options in these patients. Rotational and transposition flaps are preferred over advancement flaps, given the tendency for the latter to retract. Distant flap options include radial forearm, upper arm (Tagliacozzi), anterolateral thigh, latissimus, groin, and rectus flaps but often require significant debulking to more closely match the characteristics of facial skin ( Fig. 58.14 ). Advancement flaps, most notably from the neck to the face, can add tension, causing secondary deformities such as ectropion, oral commissure displacement, and even mandibular growth disturbances in children (see Fig. 58.2 ). Given these risks, one must approach flaps cautiously and avoid being overzealous in the surgical plan. Excising a scar while introducing new skin tension and contracture does not advance reconstructive goals.
(A) Panfacial scarring secondary to second- and third-degree burns. (B) Woodcut of Tagliacozzi flap from 1597. (C–E) Creation of tubed pedicle on upper left arm. (F) Inset of tubed pedicle flap. (G) Stabilization of left arm with tubed pedicle flap in place. (H) Division of flap. (I and J) Postop result.
(B, from Tagliacozzi, G. Apud Gasparem Bindonum juniorem . 1597.)
Tissue expansion
At a meeting of the American Society of Plastic and Reconstructive Surgeons in 1956, tissue expansion was first described by C. Neumann for an ear deformity that was reconstructed using skin expanded with a latex balloon. In the United States, the pioneering work of C. Radovan and E. Austad generated significant interest after presenting cases at a national meeting in 1979. Since then, tissue expanders have been a safe and effective technique for reconstructing soft tissue deformities and contractures.
Tissue expanders are premolded balloons of various shapes (e.g., circular, rectangular, crescentic) inserted under the tissue for reconstruction once sufficient expansion has occurred. The silicone balloons undergo expansion via intermittent, sequential saline injections through a remote or integrated port. This technique is a robust option for burn reconstruction by providing and preserving local vascularized tissue with similar color, texture, thickness, and hair-bearing characteristics. It eliminates the need for distant flaps or microsurgery and mitigates donor site morbidity. The technique can expand a local flap, a distant flap, or skin that can be harvested for an FTSG. Disadvantages include serial expansion visits, multiple reoperations, poor temporary aesthetic appearance, and the potential complications of expander exposure, leakage, rupture, infection, and port malfunction.
There are various areas of the body in which tissue expanders can be used for facial burn reconstruction, including the scalp, forehead, cheek, neck, and chest. The scalp provides an incredibly effective and well-tolerated reconstructive option ( Fig. 58.15 ). Scalp expanders in burn patients typically have lower complication rates than are seen with expanders used in the extremities, which have been reported to be as high as 50% in some studies. The scalp provides superb vascularity and a firm base on which to expand.
Panfacial burn from a house fire at age 2. (A) Scalp tissue expander before nasal reconstruction. (B and C) Forehead flap design and multiple surgical delay procedures to ensure scar flap survival. Indocyanine green (ICG) evaluation used intraoperatively to safeguard flap survival. (D) Postop showing forehead flap in place. (E) Four and a half years after forehead flap index surgery. Patient later had cadaveric cartilage placement to nose to improve airway and aesthetics. Cartilage has not resorbed.
One must exercise caution using expanded cervicopectoral flaps transposed to the face, as they can cause iatrogenic contour deformities because of tension placed on the face. In contrast, expanded neck tissue advanced across the neck and not onto the face can interpose elastic tissue to the neck and decrease facial tension.
Laser therapy
Laser therapy, built on selective photothermolysis and fractional thermolysis, has contributed to a paradigm shift in how we think about scars and how they are evaluated and treated. , , Lasers offer a minimally morbid alternative to surgically removing hypertrophic and contracted scars by inducing a patient’s tissue to remodel, regenerate, and return to a more normal condition. In many cases, scars are the optimal reconstructive anatomy: they are autologous tissue already in the ideal location. When laser therapy is used alone or in combination with simple, classic plastic surgery techniques such as Z-plasty and local tissue flaps that mitigate tension and realign scars, the scars can sufficiently blend in such that excision is rarely needed. Laser therapy is beneficial in early recovery and while awaiting scar maturation. The rehabilitation of injured skin in its native location can often produce outcomes superior to flaps from remote sites of the body that do not match adjacent skin. Fifty years ago, virtually every burn scar was excised. Today, local tissue rearrangement and laser therapy make that approach unnecessary for many scars and contractures.
Timing of reconstructive surgery
Considering three phases of reconstructive surgery for facial burn deformities is useful: acute, intermediate, and late. The optimal time for a surgeon to become involved in caring for a patient with facial burns is the acute phase, which can last up to a year after injury. Ideally, in coordination with a multidisciplinary burn care team, the surgeon develops short- and long-term reconstructive goals, setting the stage for planned surgeries. The timing of those surgeries and the location and conservation of donor sites are critical decisions in the overall care plan. During the acute phase, perioral scarring can cause microstomia, compromising airway access and alimentation. This problem can be resolved by acutely releasing the oral commissures and using local tissue rearrangement or grafting, with care taken to avoid excessive incisions that can result in macrostomia. When macrostomia is present, it is usually caused by contractile forces originating from wounds and grafts in the cheek and perioral areas. These tension vectors evert both lips and move the oral commissure laterally, resulting in debilitating loss of oral competence. Prompt release and grafting of the lower and upper lips can address this problem, with definitive reconstruction postponed for a later time.
A surgeon can also intervene during the intermediate phase when scars are months to years old and typically maturing. In this scenario, a patient may have received all preceding care elsewhere. During the intermediate phase, focus is placed on rehabilitating scars with local tissue rearrangement and laser therapy to alter scar orientation, reduce tension, and induce remodeling. Contractures are treated with surgical release, skin grafting, and local tissue rearrangement. During the late phase of reconstruction, the surgeon is tasked with revising deformities and scars that are typically (but not always) soft, mature, and stable many years after the acute injury. Again, Z-plasties and laser therapy are often sufficient to achieve excellent results.
Reconstruction of the burned lip and mouth
General principles of lip reconstruction
The lips and mouth are critical aesthetic components of the face, and even subtle irregularities are easily noticeable to the layperson. The upper lip is bound centrally by the nasal base, and the nasolabial folds laterally, whereas the lower lip is bound inferiorly by the mental sulcus. Lip reconstruction presents specific challenges, given the unique relationship of the lip with its surrounding cutaneous borders and the relationship between the upper and lower lip. Both functional and aesthetic goals are integral to reconstruction. Functional goals include the preservation of phonation, mobility, sensation, oral access, and oral competence. Aesthetic goals include tissue matching and preservation of anatomic landmarks, facial subunits, and lip symmetry. Reconstruction should employ local tissues whenever possible and replace skin with skin and vermilion with vermilion.
Perioral burns are rarely found in isolation and are often associated with extensive facial burns involving the neck, cheeks, and nasal regions, limiting available adjacent tissues for reconstruction. Significant soft tissue loss of the lips is uncommon. Discerning healthy from necrotic lip tissue during the acute period is typically particularly challenging. A cautious approach that avoids early debridement and allows eschar to separate is best. In some cases, when eating or breathing is impaired, early debridement and reconstruction may be necessary. Lip wounds have a protracted healing period because of their constant motion and contact with food and oral bacteria, and hypertrophic scarring often develops.
Scar contractures resulting from perioral burn wounds or skin grafts can have a purse-string effect on the mouth, leading to microstomia. Macrostomia can develop when perioral contraction of burn wounds or skin grafts affects the upper and lower lips and laterally displaces the oral commissure. Both deformities can cause impaired speech, alimentation, oral hygiene, and facial expression; injury to dentition; upper/lower lip ectropion; and airway compromise. The absence of underlying skeletal support facilitates an enhanced effect of scar contractures on the oral commissure and the development of microstomia. In addition to extensive facial burns, microstomia can result from electrical injury to the oral commissure, most commonly seen in young children. Persistent oral scar contractures in pediatric patients hinder the development of the underlying maxillofacial skeleton and can lead to malocclusion, retrogenia, and speech pathology. Neck contractures often cause lower lip eversion and must be corrected before lower lip reconstruction ( Fig. 58.16 ).
Acid burn to right face, neck, and chest. (A and B) Neck contracture causing severe mouth distortion and oral incompetence. (C) Tissue-expanded left neck with local flap to right neck followed by split-thickness skin graft placed after neck contracture release. Full-thickness skin graft also placed to right lower lip. (D and E) About 3 years postop showing restored position of both lips.
The panfacial burn usually results in macrostomia. During the acute period, contracture release and perioral skin grafts are often employed to maintain the airway. The grafts typically contract over time, requiring revision. Microstomia can develop when the upper and lower lips are grafted, requiring commissuroplasty with local tissue rearrangement for definitive treatment.
Evaluation
As with all burn injuries, evaluating the underlying pathology and developing an optimal solution is essential. Soft tissue deficits, distorted landmarks, and functional impairment must be carefully assessed. The vast majority of burned lip injuries are cutaneous, some with resultant scar contracture. It is critical to note the involvement of the vermilion and other vital structures. When contractures are present, STSGs and FTSGs often provide an appropriate remedy when the underlying orbicularis oris muscle is intact and other facial muscles and nerves are not compromised. Minor contractures can usually be treated with Z-plasties combined with laser therapy. Skin grafting for larger contractures can achieve excellent outcomes and prevent the need for complex flaps. The functioning gracilis muscle-free flap may be suitable for severe deep burns requiring muscle reconstruction.
Lower lip
The lower lip is made of a single facial aesthetic subunit. Reconstructive options include FTSGs, local flaps, regional pedicled flaps, and microvascular free flaps ( Fig. 58.17 ). Classic flaps used in oncologic reconstruction may not be applicable to burn reconstruction in which only the skin is impacted and the orbicularis oris muscle and mucosa are intact. Injured orbicular oris preserves oral continence while any skin contracture is being treated.