Chapter 6 Limited scar brachioplasty
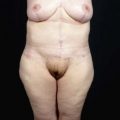
• Good for many, but not all, cases of brachial dermatolipodystrophy in non-massive weight loss patients. The vertical height from the mid-humerus to the most dependent portion of the mid-upper arm (with the arm at 90° to the body) should be no greater than 10 cm. For excessive upper dermatolipodystrophy, the traditional method should be used.
• The tailor tack method should always be used intraoperatively to confirm the accuracy of the preoperative markings. This should be done after any liposuction, if necessary, is performed. Corrections or modifications can be made at this time. The tailor tack closure should always be checked with the patient in the upright position and the arm at a 90° angle to the lateral chest.
• A superficial plane should be used for the resection of the involved area, taking only a thin layer of fat with the resected specimen.
• The elbows should not be raised above the level of the shoulders until 3 weeks postoperatively.
• During the preoperative marking, the transverse axis width of the incision (in the axillary fold) should stop at 1.5–2 cm medial to the visible portion of the axillary crease on the anterior and posterior shoulder. This helps in preventing the final scar from extending into visible areas.
• Undesirable anterior axillary and post-axillary fullness can also be corrected during this procedure.
• 12% of patients need some form of revisional surgery performed at 1 year or later. The most common reason is for scar correction.
Introduction
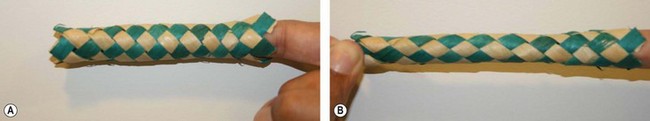
There is an ever increasing demand, mainly in women, for correction of brachial dermatolipodystrophy. Most patients, however, are not willing to accept the traditional brachioplasty scar that extends, in various configurations, from the axilla, running along the inner arm to the elbow. Following the seminal paper by Pollock,1 which described his technique for the treatment of hidradenitis suppurativa by excision of the involved axillary area followed by direct closure, I began to adapt this approach for esthetic brachioplasty. I now have 25 years of experience with this approach. There have been numerous refinements over the years.1–8 The minimal incision brachioplasty (MIB) technique is the preferred approach for most patients that I see, save for those with excessively dependent dermatolipodystrophy of the upper arms (as commonly seen in massive weight loss patients). In all other cases, it provides predictably good results that are equal to those achieved in comparable patients with the traditional approach. I am most frequently asked how simply tightening the skin of the axilla, in the minimal incision approach, can replicate the result achieved when the customary extended incision method is employed. This is best demonstrated by referring to the mechanics of the classic bamboo finger trap (Fig. 6.1), which when pulled on just one end circumferentially tightens the entire length of the tube.
Surgical Technique
Markings
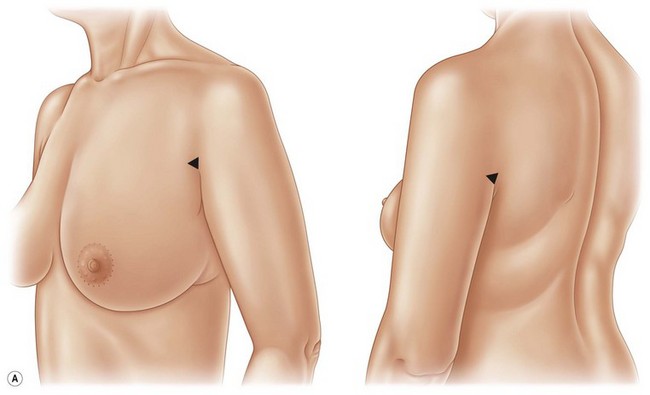
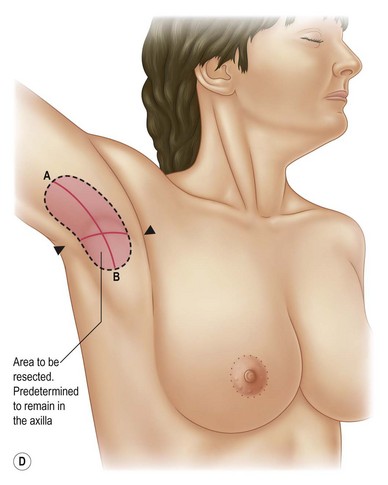
1. Marking is performed in the preoperative holding area with the patient in the upright position. With arms against sides, mark the anterior and posterior shoulders at the junction of the axilla with the shoulder. The final scar should not be visible beyond these markings (Fig. 6.2A).
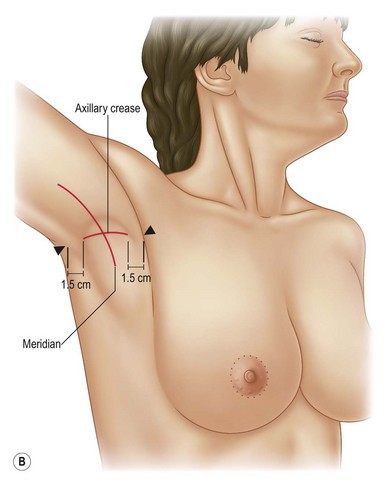
2. Mark longitudinal axis from central inner arm, through center of axilla, to the midlateral chest area (Fig. 6.2B).
3. Mark the transverse axis from anterior shoulder to posterior shoulder in the axillary crease or fold. This line should stop 1.5–2 cm medial to the anterior and posterior axillary crease–shoulder junction. This helps avoid a scar that will extend into a visible area of the shoulder (Fig. 6.2B).
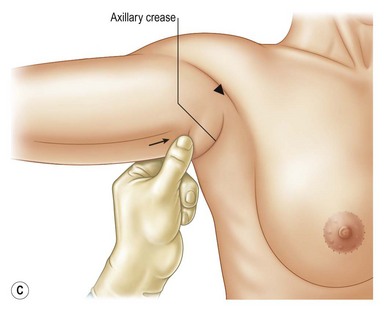
4. Determine the longitudinal length of excision using the pinch technique. First, move the skin of the triceps towards the transverse axis line until the arm has a pleasing contour. Then move the lateral chest skin towards the transverse axillary line. It is important to advance the lateral chest skin towards the transverse axillary crease to fix and stabilize the upper arm correction (Fig. 6.2C, D).
5. Mark areas that require liposuction. These should include, if indicated, the area of lipodystrophy of the upper outer breast/anterior axillary area as well as the posterior shoulder/axillary area. Both of these areas of lipodystrophy – which patients frequently point out as being of concern – can be easily corrected during the MIB procedure by liposuction and the subsequent axillary skin tightening.
< div class='tao-gold-member'>
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree