| Maximal orbital decompression |
| Need for access to the intraconal space |
| In combination with a medial and lateral orbitotomy approach for lesions near the orbital apex |
| Complete ophthalmic examination with attention to optic nerve status |
| Orbital imaging studies – CT, MRI, angiography when indicated |
| Exophthalmometry readings |
| Extraocular muscle movements and primary deviation |
| MRD1 and MRD2 |
| Photographic documentation of eye movements and worm’s eye view |
Introduction
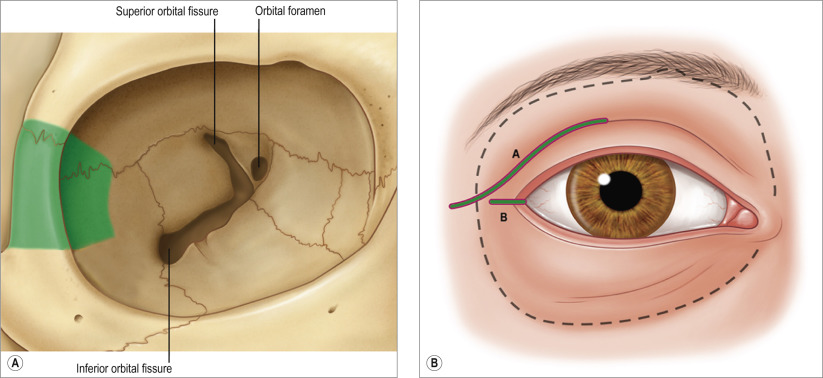
Marginotomy of the lateral orbital rim is performed to improve access to the retrobulbar space and in cases of maximal orbital decompression for severe thyroid-related orbitopathy (TRO). Improved visualization and approach to intraconal lesions is facilitated with removal of the lateral orbital rim. For medial masses, the lateral rim can be removed to allow the globe to rotate laterally, which allows for more space medially.
Our preferred skin incision is the lateral upper eyelid crease incision. Through this incision, osteotomy is performed in two locations; one at the frontozygomatic suture and the other inferior bone cut is made just above the zygomatic arch. Pre-drilled holes allow for ease of replacement with sutures.
In most instances the orbital rim is temporarily removed for access and then replaced. In the case of orbital decompression, the rim is typically removed and not replaced (see Table 64.3 , Chapter 64). The thin lateral orbital wall and deeper marrow space of the greater wing of the sphenoid is removed to allow for maximal decompressive effect. The zygomaticotemporal nerve should be preserved to avoid a small area of hypesthesia just lateral to the brow in the temple region. We have found that removing the lateral orbital rim and leaving it off in cases of maximal decompression causes minimal cosmetic deformity and improves the decompressive effect significantly.
Surgical Technique