Abstract
Irritant contact dermatitis (ICD) represents one of the most common dermatoses and it is caused by an incredibly diverse source of provocative agents. Determination of the inciting irritant or irritants is critical to the successful diagnosis and subsequent treatment of this frustrating, and at times disabling, disorder. The protean range of clinical presentations varies from sensory disturbances without visible skin findings to severe chemical burns and ulcers. The correct diagnosis rests on an analysis of critical objective signs of disease coupled with an insightful targeted history. Sources of irritants are ubiquitous, i.e. they are not limited to the workplace but are a part of routine everyday activities. Preventative measures include work process change, personal protective equipment, and maximizing the barrier defenses of the epidermis. Common causes of ICD and their sources are discussed herein.
Keywords
contact dermatitis, irritant contact dermatitis, irritation, hand dermatitis, toxic contact dermatitis, chemical burn, irritant reaction, irritancy, corrosives
- ▪
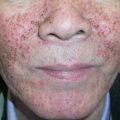
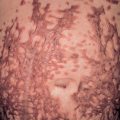
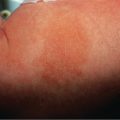
Irritant contact dermatitis (ICD) is a localized, non-immunologically initiated, cutaneous inflammatory reaction. Its clinical characteristics are polymorphous, and they include erythema, scaling, edema, vesiculation, and erosions in acute cases, with erythema, lichenification, hyperkeratosis, and fissures in chronic cases
- ▪
ICD results from a direct cytotoxic effect due to single or repeated application of a chemical substance or physical insult to a cutaneous site
- ▪
ICD is a common disorder and represents an important spectrum of clinical presentations in both general and occupational dermatology, occurring when the normal epidermal barrier is disrupted and secondary inflammation develops
- ▪
Despite different pathogeneses, allergic contact dermatitis and ICD have similar clinical appearances, especially their chronic variants
- ▪
ICD is a multifactorial syndrome determined by the properties of the irritating substance as well as host and environmental factors; a dose–response relationship is related to exposure parameters such as concentration, pH, temperature, occlusion, repetition, and duration of contact
- ▪
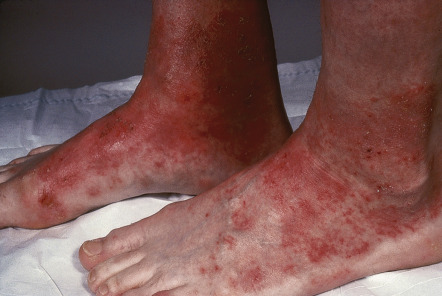
Strong or absolute irritants such as strong acids and alkalis, as well as oxidants, produce erythema, edema, vesicles that may coalesce into bullae, oozing, and, in severe cases, necrosis and ulceration. The latter is vernacularly termed a “chemical burn”
- ▪
The clinical features of chronic ICD from repeated exposure to low-grade or marginal irritants (e.g. soaps, solvents, cleansers, weak acids and bases) include erythema, lichenification, excoriations, scaling, and fissures
Introduction
There are two major forms of contact dermatitis: irritant and allergic. Irritant contact dermatitis (ICD) is a cutaneous inflammatory disorder resulting from activation of the innate immune system by direct cytotoxic effect of a chemical or physical agent, whereas allergic contact dermatitis is a delayed-type hypersensitivity immune reaction mediated by hapten-specific T cells .
Occupational contact dermatitis is a matter of public health importance , contributing to combined direct and indirect annual costs in the US of up to $1 billion when accounting for medical costs, workers’ compensation, and lost time from work . A recent National Health Interview Survey suggested that in 2010, 15 million Americans were affected by occupational dermatitis , a figure 100-fold higher than in prior reports by the US Bureau of Labor Statistics. Overall, the impact of occupational skin diseases on both society and the individual is formidable in light of both prevalence and economic factors.
History
One of the earliest documented irritant skin reactions is in the writings of Celsus around 100 AD, when he described skin ulceration resulting from corrosive metals . For the next several centuries, little attention was paid to the skin problems incurred by tradesmen. The first accounts of occupational skin diseases focused on ill health among miners, and in 1556, Georg Agricola detailed the deep ulcers observed among metal workers. Eleven years later, Paracelsus discussed the etiology, pathogenesis and therapy of skin changes caused by salt compounds. In 1700, Bernardino Ramazzini published a detailed treatise on the diseases of tradespeople in which he described skin disorders incurred by bath attendants, bakers, gilders, midwives, millers, and miners . Physicians began to more widely recognize occupational irritant dermatitis during the Industrial Revolution with the development of new materials and chemicals, both natural and synthetic, for both industrial and household use . Germany and France were the first to enact laws compensating workers for industrial skin diseases. Early prospective studies of ICD in 1919 involved experimentation with the irritant mustard gas dichloroethylsulfide .
Epidemiology
ICD is the most common form of occupational skin disease, estimated to constitute between 70% and 80% of all occupational skin disorders ( Table 15.1 ). Data from the North American Contact Dermatitis Group indicate that in groups of patients with contact dermatitis, ICD (as a primary diagnosis) accounts for 9–10% of those screened for allergic contact dermatitis via patch testing, and when hands are affected, ICD predominates over all other causes of contact dermatitis .
| EXPOSURES TO IRRITANTS BY OCCUPATION | |
|---|---|
| Occupation | Irritants |
| Agriculture workers | Artificial fertilizers, disinfectants, pesticides, cleaners, gasoline, diesel oil, plants/grains |
| Artists | Solvents, clay, plaster |
| Automobile and aircraft industry workers | Solvents, cutting oils, paints, hand cleansers |
| Bakers and confectioners | Flour, detergents |
| Bartenders | Wet work, detergents |
| Bookbinders | Solvents, glues |
| Butchers | Detergents, meat |
| Cabinet makers and carpenters | Glues, detergents, thinners, solvents, wood preservatives |
| Cleaners | Detergents, solvents, wet work |
| Coal miners | Dust (coal, stone), wet conditions |
| Construction workers | Cement |
| Cooks and caterers | Detergents, vegetable juices, wet work |
| Dentists and dental technicians | Detergents, hand cleansers, wet work |
| Dry cleaners | Solvents |
| Electricians | Soldering fluxes |
| Electroplaters | Acids, alkalis |
| Floor layers | Solvents |
| Florists and gardeners | Manure, artificial fertilizers, pesticides, wet work |
| Hairdressers | Permanent wave solutions, shampoos, bleaching agents, wet work |
| Homemakers | Detergents, cleansers, foods, wet work |
| Hospital workers | Detergents, disinfectants, foods, wet work |
| Jewelers | Detergents, solvents |
| Mechanics | Oils, greases, gasoline, diesel fuel, cleaners, solvents |
| Metal workers | Cutting oils, solvents, hand cleansers |
| Nurses | Disinfectants, detergents, wet work |
| Office workers | Paper products, solvents in cleaners, adhesives, and photocopiers/toner |
| Painters | Solvents, thinners, wallpaper adhesives, hand cleansers |
| Photography industry workers | Solvents, wet work |
| Plastics workers | Solvents, acids, styrene, oxidizing agents |
| Printers | Solvents |
| Rubber workers | Solvents, talc, zinc stearate |
| Shoemakers | Solvents |
| Tannery workers | Acids, alkalis, reducing and oxidizing agents, wet work |
| Textile workers | Fibers, bleaching agents, solvents |
| Veterinarians and slaughterhouse workers | Disinfectants, wet work, animal entrails and secretions |
The US Bureau of Labor Statistics data show that occupational skin diseases accounted for a consistent 30–45% of all patients with occupational illnesses from the 1970s through the mid-1980s. However, occupational skin disease rates have since fallen dramatically, e.g. from an average rate of 16.2 events/10 000 full-time workers in 1972 to 2.8 events in 2013 . Although skin disease accounted for only 17% of all recorded non-fatal occupational illnesses in 2007 , it still ranks second and is only surpassed by musculoskeletal disorders. The incidence of occupational contact dermatitis in several other countries is similar to that in the US, with a range of 50 to 70 cases/100 000 workers/year . In 1996, the United Kingdom created a voluntary reporting system that combined information from the EPIDERM study with the occupational physicians’ reporting activity (OPRA). The annual incidence of occupational contact dermatitis reported by dermatologists was 0.9 per 10 000 workers, and for occupational physicians, it was 3.1 per 10 000 workers .
In 2010, the National Institutes of Occupational Safety and Health sponsored the National Health Interview Survey which utilized a sample cohort of 27 157 individuals (to represent 229 million US civilian adults), the majority of whom were employed or recently employed . The overall prevalence of dermatitis was 10.2%, ranging from 7.3% in those who never worked to 9.8% in currently employed workers to 11.8% in those recently, but not currently, employed.
In addition to manufacturing, industries with the highest non-adjusted and adjusted rates of dermatitis include healthcare and social assistance; arts, entertainment and recreation; and accommodations and food services. Rubber chemicals, soaps and cleansers, wet work, resins, acrylics, and nickel are some of the more common sources for irritant and allergic contact dermatitis. Additional high-risk occupations are discussed in Chapter 16 .
Clinical manifestations of ICD are determined by the properties of the irritating substance as well as host and environmental factors. These include concentration, pH, mechanical pressure, temperature, humidity, and duration of contact. Low ambient humidity and cold are important factors in decreasing the water content of the stratum corneum and, consequently, increasing the permeability to irritants such as soaps, detergents, acids, bases, and solvents. Cold alone may also reduce the plasticity of the horny layer, with consequent cracking of the stratum corneum. However, in one study, the application of cold had a protective effect on the development of ICD if applied during the provocative exposure, in this case to sodium lauryl sulfate . Occlusion, excessive humidity, and maceration increase the water content of the stratum corneum, with consequent enhanced percutaneous absorption of water-soluble substances ( Fig. 15.1 ). In addition, irritated skin may become more susceptible to superimposed allergic sensitization.
Important predisposing characteristics of the individual include age, sex, pre-existing skin disease, anatomic region exposed, and sebaceous activity. There are age-associated changes in the skin that can alter the skin’s response to irritants. Both infants and the elderly are more often affected by ICD because of their less robust epidermal barrier, and they also develop more severe symptoms. While skin irritation may be seen more often on the upper extremities of women than men, this higher prevalence of ICD may be due to increased frequency of exposure rather than inherent gender differences. Genetic factors also play a role in the development of ICD, as shown in studies with monozygotic twins . Patients with a history of atopic dermatitis have a 13.5 times greater risk of developing occupational dermatitis , and a reduction in epidermal filaggrin can reduce the inflammatory threshold for irritants . Lastly, the most commonly affected sites are exposed areas such as the hands and the face, with hand involvement seen in ~80% of patients and facial involvement in 10% . Excessive exposure to water, soaps and detergents, common causes of ICD, play a critical role given that wet work (immersion in water for >2 hours, occlusive protective gear, and/or hand washing >20 times/day) represents one of the most important risk factors for developing irritant dermatitis .
Pathogenesis
Although the cellular mechanisms of ICD remain elusive, increasing evidence suggests that activated keratinocytes act as signal transducers in the control of host homeostatic responses to exogenous stimuli and they serve as key immunoregulators. An irritant chemical’s ability to induce cutaneous damage may serve to trigger pattern recognition receptors (PRR), including Toll-like receptors, providing the necessary impetus to activate the innate immune system . While other mediators such as prostaglandins, leukotrienes, and neuropeptides may possibly play a role, cytokines carry the most interest in ICD as they are the central mediators in T-cell recruitment and inflammation.
Several pathomechanisms have commonly been associated with ICD, including denaturation of epidermal keratins, disruption of the permeability barrier (see Ch. 124 ), damage to cell membranes, and direct cytotoxic effects, with different mechanisms at work with different irritants ( Table 15.2 ). The mechanisms involved in the acute and chronic phases of ICD are fundamentally different. Acute reactions involve direct cytotoxic damage to keratinocytes, while repeated exposures to solvents and surfactants cause slower damage to cell membranes by removing surface lipids and water-retaining substances.
| IRRITANTS AND MECHANISMS OF TOXICITY | |
|---|---|
| Irritant | Mechanisms of toxicity |
| Detergents | Barrier disruption, protein denaturation, membrane toxicity |
| Acids | Protein denaturation, cytotoxicity |
| Alcohols | Protein denaturation |
| Alkalis | Barrier lipid denaturation, cytotoxicity through cellular swelling |
| Oils | Disorganization of barrier lipids |
| Organic solvents | Solubilization of membrane lipids, membrane toxicity |
| Oxidants | Cytotoxicity |
| Reducing agents | Keratolysis |
| Water | If barrier is disrupted, cytotoxicity through swelling of viable epidermal cells |
The pathogenic pathway in the acute phase of ICD, common to many chemically unrelated irritants, begins with penetration of the irritant through the permeability barrier (stratum corneum), mild damage or stress to keratinocytes, and the release of mediators of inflammation with resultant T-cell activation. In this manner, once activation is initiated via epidermal cells, continuous T-cell activation independent of the exogenous agent may be maintained and barrier dysfunction perpetuated . Tumor necrosis factor-α (TNF-α) and interleukin (IL)-1α are the major mediators, and they are capable of inducing production of other cytokines, chemokines, and adhesion molecules, leading to leukocyte recruitment to the site. Specifically, TNF-α, IL-6, and IL-1β upregulate expression of intercellular adhesion molecule-1 (ICAM-1) . This is a predominant feature of ICD. In addition, IL-1 receptor antagonist (IL-1RA) and IL-8 increase substantially after exposure to the common irritant sodium lauryl sulfate.
In the chronic phase of ICD, the role of the stratum corneum as a barrier is disrupted. Damage to the stratum corneum lipids (which mediate barrier function) is associated with loss of cohesion of corneocytes, desquamation, and an increase in transepidermal water loss. Transepidermal water loss is one of the triggering stimuli that promote lipid synthesis, keratinocyte proliferation, and transient hyperkeratosis during the restoration of the cutaneous barrier. However, damage with a solvent can disrupt this protective mechanism by occlusion and blockage of water evaporation, thus halting lipid synthesis and barrier recovery. After chronic exposure, the result is increased epidermal turnover manifested clinically by the chronic eczematoid irritant reaction .
Clinical Features
Several different types of ICD have been described (see below). Consequences of the myriad forms of ICD range from postinflammatory pigmentary changes to poorly healing ulcers ( Table 15.3 ).
| CLINICAL FEATURES SUGGESTING AN IRRITANT OR TOXIC ETIOLOGY | ||
|---|---|---|
| Clinical feature | Possible irritant or toxin | |
| Ulcerations | Inorganic acids (chromic, hydrofluoric, nitric, hydrochloric, phosphoric, sulfuric) Strong alkalis (calcium oxide, sodium hydroxide, potassium hydroxide, ammonium hydroxide, calcium hydroxide, sodium metasilicate, sodium silicate, potassium cyanide, trisodium phosphate, sodium carbonate, potassium carbonate) Salts (arsenic trioxide, dichromates) Solvents (acrylonitrile, carbon bisulfide) Gases (ethylene oxide, acrylonitrile) | |
| Folliculitis | Oils and greases Tar and asphalt Chlorinated naphthalenes and polyhalogenated biphenyls Arsenic trioxide Glass fibers | |
| Miliaria | Occlusive clothing and overheating Adhesive tape Ultraviolet and infrared radiation Aluminum chloride | |
| Pigmentary changes | ||
| Any irritant or allergen, especially phototoxic agents such as psoralens, tar, asphalt, psoralen-containing plants Metals, such as inorganic arsenic (systemically), silver, gold, bismuth, mercury Radiation: ultraviolet, infrared, microwave, ionizing | |
| p -Tert-amylphenol | p -Cresol |
| p -Tert-butylphenol | 3-Hydroxyanisole | |
| Hydroquinone (HQ) | Butylated hydroxyanisole | |
| Monobenzyl ether of HQ | 1-Tert-butyl-3, 4-catechol | |
| Monomethyl ether of HQ | 1-Isopropyl-3, 4-catechol | |
| p -Tert-catechol | 4-Hydroxypropriophenone | |
| Alopecia | Borax Chloroprene dimers | |
| Urticaria | Animals (arthropods, caterpillars, corals, jellyfish, moths, sea anemones) Balsam of Peru Cosmetics (e.g. sorbic acid) Drugs (alcohol [ethanol], benzocaine, camphor, capsaicin, chloroform, iodine, methyl salicylate, resorcinol, tar extracts) Foods (cayenne pepper, fish, mustard, thyme) Fragrances and flavoring agents (cinnamon oil, cinnamic acid and aldehyde, benzaldehyde) Metals (cobalt) Plants (seaweed, stinging nettles), woods Preservatives (benzoic acid) Textiles (e.g. blue dyes) | |
Acute Irritant Contact Dermatitis
Acute ICD, commonly seen with occupational accidents, develops when the skin is exposed to a potent irritant. The latter is capable of profound reactions on the skin surface: oxidation, reduction, desiccant, vesicant, or ion disruption . The acute reaction reaches its peak quickly, usually within minutes to hours after exposure, and then starts to heal. This is termed the decrescendo phenomenon. Symptoms of acute ICD include burning, stinging, and soreness of the directly affected sites. Physical signs include erythema, edema, bullae, and possibly necrosis. These lesions are restricted to the area where the irritant or toxicant damaged the tissue, with sharply demarcated borders and asymmetry pointing to an exogenous cause. If there is no dermal injury, healing should be complete . The potent irritants that most frequently lead to ICD are acids and alkalis, resulting in chemical burns.
Acute Delayed Irritant Contact Dermatitis
Acute delayed ICD is a retarded inflammatory response characteristic of certain irritants, such as anthralin (dithranol), benzalkonium chloride (preservative/disinfectant), and ethylene oxide. Adverse reactions to these chemicals are considered idiosyncratic, except when they are applied to previously injured skin, e.g. sites of xerosis or atopic dermatitis . Clinically visible inflammation is not seen until 8 to 24 hours (or more) after exposure, and thus may mimic allergic contact dermatitis; however, the associated symptom is more frequently burning rather than pruritus. Sensitivity to touch and water is elicited. This form of ICD is commonly seen during diagnostic patch testing.
Irritant Reaction Irritant Contact Dermatitis
Irritant reaction ICD is a type of subclinical irritant dermatitis in individuals exposed to wet chemical environments, such as hairdressers, caterers, metal workers or those with frequent exposures to soap and water. It is characterized by one or more of the following signs: scaling, redness, vesicles, pustules and erosions, often beginning under occlusive jewelry (e.g. rings) and then spreading onto the fingers and then the hands and the forearms. It may simulate dyshidrotic dermatitis and ultimately result in cumulative ICD if exposure is prolonged; however, ICD tends to resolve if exposure is discontinued.
Cumulative Irritant Contact Dermatitis
Cumulative ICD is a consequence of multiple sub-threshold skin insults, without sufficient time between them for complete restoration of skin barrier function (see Fig. 16.4 ). It may be due to a variety of stimuli or frequent repetition of one factor, e.g. exposure to water both at the work place and at home. Clinical symptoms develop only after the cumulative damage exceeds an individually determined manifestation or elicitation threshold, which may decrease with progression of the disease. Weak irritants do not lead to clinical ICD if they are encountered far enough apart to allow for restoration of skin barrier function. However, if the same irritant exposures follow each other closely in time, or when the manifestation threshold is reduced (e.g. in a patient with active atopic dermatitis), cumulative ICD can develop. The properties of the irritating substance, e.g. pH, solubility, detergent action, physical state, are also important. In contrast to acute ICD, the lesions of chronic ICD are less sharply demarcated. Pruritus and pain due to fissures of hyperkeratotic skin are symptoms of chronic ICD. Signs may include xerosis, erythema and vesicles, but lichenification and hyperkeratosis predominate.
Asteatotic Dermatitis
Asteatotic dermatitis , also referred to as asteatotic eczema, eczema craquelé, or exsiccation eczematid ICD, is a special variant seen primarily during dry winter months. Elderly individuals who frequently bathe without remoisturizing are at particular risk of developing asteatotic dermatitis. Intense pruritus is common, with the skin appearing dry with ichthyosiform scale and characteristic patches of superficially cracked skin (see Ch. 13 ).
Traumatic Irritant Contact Dermatitis
Traumatic ICD may develop after acute skin trauma, such as from burns, lacerations, or acute ICD. Patients should be asked whether they have cleansed the skin with strong soaps or detergents. It is characterized by eczematous lesions, most commonly on the hands, that last for weeks to months with persistent redness, infiltration, scale, and fissuring in the affected areas.
Pustular and Acneiform Irritant Contact Dermatitis
Pustular and acneiform ICD results from exposure to certain irritants, such as metals, croton oil, mineral oils, tars, greases, cutting and metal working fluids, and naphthalenes (see Table 15.3 and Ch. 16 ). This syndrome should be considered in conditions in which folliculitis or acneiform lesions develop in settings outside of typical acne, particularly in patients with atopic dermatitis, seborrheic dermatitis, or prior acne vulgaris. The pustules are “sterile” and transient. Miliarial reactions, which may become pustular, can develop in response to occlusive clothing, adhesive tape, or ultraviolet and infrared radiation.
Non-erythematous Irritant Contact Dermatitis
Non-erythematous ICD may be defined as a subclinical form of ICD with early stages of skin irritation seen as changes in the stratum corneum barrier function without a clinical correlate.
Subjective or Sensory Irritant Contact Dermatitis
Subjective or sensory ICD is characterized by reports of a stinging or burning in the absence of visible cutaneous signs of irritation. Irritants capable of eliciting this reaction include propylene glycol, hydroxy acids, ethanol, and topical medications such as lactic acid, azelaic acid, benzoic acid, benzoyl peroxide, mequinol, and tretinoin. Sorbic acid, a preservative in concentrations of up to 0.2% in foods, cosmetics and drugs, may also produce sensory irritation in predisposed individuals. This reaction to irritants such as lactic or sorbic acid may be reliably reproduced with dose responsiveness in double-blinded exposure tests.
Airborne Irritant Contact Dermatitis
Airborne ICD develops in irritant-exposed sensitive skin of the face and periorbital regions. While this often simulates photoallergic reactions, involvement of the upper eyelids, philtrum, and submental regions in patients with airborne ICD may aid in distinguishing between these two entities. Airborne ICD results from exposure to floating dusts, fibers (particularly fiberglass), and volatile solvents and sprays .
Frictional Irritant Contact Dermatitis
Frictional ICD is a distinct ICD subtype resulting from repeated low-grade frictional trauma. It is often acknowledged to also play an adjuvant role in allergic contact dermatitis and ICD. The frictional response includes hyperkeratosis, acanthosis, and lichenification, often progressing to hardening, thickening, and increased toughness.
Contact Urticaria
Contact urticaria is divided into non-immunologic and immunologic subtypes (see Ch. 16 ), with the former occurring more frequently and in the absence of previous exposure. Irritants that can produce immunologic contact urticaria include parabens (preservatives), henna, ammonium persulfate (oxidizing agent), and latex. Non-immunologic contact urticaria can be caused by a number of exposures, from caterpillars and jellyfish to stinging nettles and foods (see Table 15.3 ) . Risk factors include atopy, hand dermatitis, previous mucosal exposure to latex (e.g. urinary catheterization), and allergies to fruits (e.g. kiwi, avocado; see Table 16.6 ).
Pathology
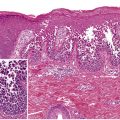
The histopathologic features of ICD vary according to the nature of the irritant, but often include mild spongiosis, necrosis of keratinocytes, and an inflammatory infiltrate rich in neutrophils. The combination of a neutrophil-rich superficial perivascular infiltrate plus widely scattered necrotic keratinocytes is most typical; sometimes there is even full-thickness epidermal necrosis and subepidermal clefting. Mild ICD can resemble allergic contact dermatitis. Over time, additional histologic findings include acanthosis with mild hypergranulosis and hyperkeratosis. In aggregate, these elements are not specific, and they cannot be confidently differentiated from either chronic allergic contact dermatitis or other types of chronic eczemas.
Classification of Irritant Chemicals
Acids
A variety of both inorganic and organic acids can be corrosive to the skin. Acids cause epidermal damage via protein denaturation and cytotoxicity. Principally, all strong acids give the same clinical features, including erythema, vesication, and necrosis.
Inorganic acids are commonly used in industry, especially hydrofluoric, sulfuric, hydrochloric, chromic, nitric, and phosphoric acids ( Table 15.4 ). Hydrofluoric acid and sulfuric acid cause the most severe burns, even at low concentrations, and there can be significant absorption leading to systemic toxicity .
| IRRITANT CHEMICALS: USES, PROPERTIES AND SIDE EFFECTS | ||
|---|---|---|
| Compound | Uses/exposures | Properties and side effects |
| Inorganic acids | ||
| Chromic acid |
|
|
| Hydrochloric acid |
|
|
| Hydrofluoric acid |
|
|
| Nitric acid |
|
|
| Phosphoric acid |
|
|
| Sulfuric acid |
|
|
| Organic acids | ||
| Acrylic acid |
|
|
| Formic acid |
|
|
| Alkalis | ||
| Cement (mixed with water) |
|
|
| Metal salts | ||
| Arsenic compounds (including arsenic trioxide) |
|
|
| Beryllium |
|
|
| Calcium oxide (quicklime) |
|
|
| Cobalt salts |
|
|
| Copper salts (e.g. sulfates, oxides, cyanides) |
|
|
| Mercury, inorganic |
|
|
| Mercury, organic |
|
|
| Selenium compounds (including sulfide) |
|
|
| Thimerosal |
|
|
| Solvents | ||
| Benzene |
|
|
| Chlorinated hydrocarbons (e.g. carbon tetrachloride, trichloroethylene, tetrachloroethane, methylene chloride, ethylene chloride) |
|
|
| Coal tar derivatives (e.g. toluene, xylene, ethyl benzene, cumene) |
|
|
| Petrochemicals (e.g. gasoline, hexane, kerosene, Stoddard solvent) |
|
|
| Disinfectants | ||
| Aldehydes (e.g. formaldehyde, glutaraldehyde, hexa-methylenetetramine) |
|
|
| Ethylene oxide |
|
|
| Halogens – Chlorines |
|
|
| Halogens – Iodines |
|
|
| Phenolic compounds (e.g. Lysol ® [cresol and soap solution], pentachlorophenol, chloroxylenol) |
|
|
| Quaternary ammonium salts (e.g. benzalkonium chloride) |
|
|
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree