| Diagnosis of unknown orbital mass |
| Removal of orbital mass causing optic neuropathy |
| Visual acuity, pupillary reaction, automated visual fields, color testing |
| Slit lamp examination |
| Exophthalmometry |
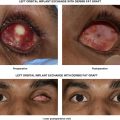
| Clinical photographs |
| Orbital imaging (contrast-enhanced CT or MR) |
| Anticoagulant status |
| Communication with pathologist – suspected lesions requiring immunohistochemistry or special stains/preparations |
Introduction
Successful orbital surgery requires: a detailed knowledge of orbital anatomy and orbital disease pathology; careful preoperative planning with orbitofacial imaging, optimal management of anticoagulants, aesthetically minded incision design; and careful and meticulous surgical technique to maximize exposure, lighting and hemostasis with appropriate instrumentation.
Multiple orbital imaging modalities can be employed to provide information about suspected lesions. CT imaging is readily available at almost all centers and is useful for evaluation of trauma, infection, foreign bodies, paranasal sinuses, orbital lesions and fine details of the bony orbit. A contrast agent may be used for evaluation of vascular malformations, infections and suspected orbital masses, but in the acute trauma setting or as a primary screen tool it is often unnecessary. MR imaging is superior for delineation of orbital soft tissues, but it provides poor resolution of bone. Dynamic vascular MR angiographic imaging is particularly useful for vascular lesions of the orbit. MR imaging is contraindicated for suspected metallic foreign bodies, while CT imaging is contraindicated in pregnancy and should be avoided when possible in children.
Orbitotomy is performed for diagnostic and therapeutic indications. For diagnosis of unknown orbital lesions, the decision should be made to perform an excisional versus an incisional orbitotomy. A careful history, clinical examination and orbital imaging allow formulation of a differential diagnosis to guide surgical decision making.
Excisional biopsy is performed to completely remove an orbital lesion and is appropriate for well-circumscribed lesions on orbital imaging. Examples of such lesions include a cavernous hemangioma, hemangiopericytoma, fibrous histiocytoma or schwannoma. Encapsulated lesions of the lacrimal gland such as pleomorphic adenoma should also be removed in completion to minimize the potential for malignant degeneration.
Incisional biopsy partially removes an orbital mass for histopathologic study. Communication between the orbital surgeon and pathologist is critical to assure proper handling of precious orbital tissues. Suspected lesions such as lymphoma may be sent fresh for immunohistologic markers instead of default placement in formalin solution. Meticulous handling of orbital specimens is also carried out as crush artifact or excessive cauterization may disrupt tissue architecture.
Orbital surgery requires specialized instrumentation that should be made available before the start of surgery. Desmarres and Senn retractors are used for skin and eyelid distraction. Malleable retractors of multiple widths as well as neurosurgical cottonoids are critical to retract orbital fat. Freer periosteal elevators and peanut sponges are useful for blunt dissection. A drill and bone saw should be available for creating osteotomies when needed. A cryoprobe is useful for stabilization and traction of orbital masses. A skilled surgical assistant is invaluable to provide exposure and retraction for the primary orbital surgeon. A fiberoptic or LED headlight with magnifying loupes is essential to provide illumination within the deep orbit. The operating microscope can be used but often impedes full access to the surgical field. We reserve the use of the microscope for finer operations such as optic nerve sheath fenestration ( Chapter 71 ).
General anesthesia is preferred, particularly for dissection within the retrobulbar space. A sequential compression device is placed on both legs to prevent deep venous thrombosis and the surgery is performed in a hypotensive environment when possible and with the head in reverse Trendelenburg position. Throughout the operation, frequent breaks are taken when performing orbital retraction in order for the pupillary reactions to be examined.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree