12 High-Risk Cutaneous Malignancies While the incidence of cutaneous malignancies has been rising in the general population, it has been particularly notable in certain groups, whom we term high-risk patients. Broadly, these patients can be divided into two categories: (1) those with genetic syndromes conferring a predisposition to skin cancer and (2) immunosuppressed patients. The types and numbers of malignancies acquired, the aggressiveness of tumors, the age of onset, their management, and their ultimate outcome differ in important ways in high-risk patients and in the general population. Here, we review contemporary understanding of the etiologies of and approaches to cutaneous malignancies in high-risk patients. Several genetic syndromes increase the risk of developing cutaneous malignancies. These include xeroderma pigmentosum (XP), Gorlin’s syndrome, Fanconi anemia, Bazex’s syndrome, and Bloom’s syndrome, among others.1 Below we focus on two of these rare conditions—XP and Gorlin’s syndrome—that confer a predilection for nonmelanoma skin cancers, and we also consider genetic predisposition to melanoma. XP comprises a group of disorders with autosomal recessive inheritance and a prevalence in the United States of 1:250,000 individuals. It is characterized by defects in genes involved in the nucleotide excision repair (NER) pathway of deoxyribonucleic acid (DNA) repair. This pathway is critical for resolving mutagenic adducts in DNA that result from ultraviolet (UV) exposure. Since the pathway is defective in XP patients, their keratinocytes accumulate numerous mutations, leading to accelerated tumorigenesis. Clinically, XP patients have normal skin at birth, but most show extreme photosensitivity with sunburn occurring even in infancy.2 Affected children develop innumerable freckles and other areas of hypopigmentation and hyperpigmentation. Such patients have a 10,000-fold increase in incidence of developing nonmelanoma skin cancer and a 2,000-fold increase in incidence of melanoma.2 Nonmelanoma skin cancers mainly occur on sun-exposed regions, with 80% occurring on the face, head, and neck.3 By contrast, approximately 45% of melanomas in these patients occur in the extremities. Not only do cutaneous malignancies occur more frequently in XP patients, but they also occur at an earlier age. The median age of onset for nonmelanoma skin cancer and melanoma are 9 and 22 years, respectively.2 Both are several decades earlier than in the general population. The most important step in management of XP patients is vigorous sun protection including avoiding peak sun exposure, use of UV-protective clothing and sunglasses, and window tinting. This should be complemented by vitamin D supplementation. If patients develop cutaneous malignancies, they are managed through disease- and stage-appropriate surgical and medical therapies. With these measures, some patients with XP live well into adulthood.4 Gorlin’s syndrome, or nevoid basal cell carcinoma (BCC) syndrome, is a rare autosomal dominant disorder in which patients develop BCCs, odontogenic keratocysts, and palmar or plantar pits. Affected patients can also show various bony developmental defects. Patients with Gorlin’s syndrome develop numerous BCCs in their lifetime—up to thousands in some cases.5 Gorlin’s syndrome patients with fairer skin are at particularly high risk.5,6,7 Alterations in the Hedgehog (Hh) pathway—a developmental cascade involved in cell growth and differentiation—underlie Gorlin’s syndrome in many patients. Specifically, germline mutations in the pathway inhibitor Patched (PTCH1) are the most commonly identified molecular lesions in patients with Gorlin’s syndrome.8 In the absence of PTCH1 activity, the protein smoothened (SMO) becomes constitutively active, leading to transcription of Hh pathway effectors. This is turn leads to dysregulation of cell growth and tumorigenesis. The recent clinical development of inhibitors of the Hh pathway, including several small molecule SMO inhibitors, provides hope for more efficacious treatment of patients with Gorlin’s syndrome. Indeed, these agents not only reduce BCC tumor burden, but also remedy the odontogenic keratocysts and palmoplantar pits characteristic of the disorder.8 Based on early clinical efficacy, vismodegib became the first SMO inhibitor to gain the approval of Food and Drug Administration (FDA) for patients with Gorlin’s syndrome in 2012. Better handling of treatment-related adverse events and methods to combat resistance will be required, however, before these novel agents achieve their full promise. Patients with familial atypical multiple mole melanoma (FAMMM) syndrome are at a greatly increased risk of developing melanoma and pancreatic cancer. The disease is defined by (1) melanoma in one or more first- or second-degree relatives, (2) high total body nevus count, including atypical nevi, and (3) specific histologic features of the nevi. FAMMM is inherited in autosomally dominant fashion with variable penetrance. In up to 40% of affected patients, mutations can be found in the CDKN2A gene which encodes the tumor suppressors p16INK4A and p14ARF.9 These genes are important for establishing cell cycle arrest or senescence in damaged cells. In the absence of CDKN2A gene product activity, incipient tumor cells may be allowed to progress in the evolution to melanoma. The large number of nevi that FAMMM patients develop increases the risk of malignant degeneration. Such patients should be screened at least every 6 months to document evolution of nevi. Total body photography and self-examination can be valuable adjuncts to identifying nevi requiring further investigation. Nevi whose appearance changes according to the asymmetry, border irregularity, color variegation, diameter, elevation or evolution (ABCDE) criteria should prompt early biopsy. Patients and their immediate family members should also be referred for genetic counseling. As the number of targeted therapies for melanoma increases, genetic sequencing may become part of the standard of care for such patients as well. As with spontaneously occurring melanomas, surgical excision is the mainstay of management when these lesions occur in FAMMM patients. Novel immunomodulatory agents for the treatment of aggressive melanomas will be discussed later. The number of patients who are chronically immunosup-pressed has increased markedly in recent decades. This reflects both natural and iatrogenic causes. The emergence and rapid spread of human immunodeficiency virus (HIV) since the 1980s has produced millions of people with severe immunosuppression worldwide. Autoimmune diseases have also increased in prevalence over the past few decades, particularly in the developed world.10 This fact, coupled with the use of immunosuppressive medications, has left many people relatively immunosuppressed during the chronic courses of these diseases. The development of effective immunosuppressive agents has also heralded a large increase in organ transplantation since the pioneering operations of the 1960s. While allogeneic transplants have saved or improved thousands of lives, the requirement for lifelong immunosuppression has deleterious consequences. Most notably, patients with long-term natural or therapeutical immunosuppression show an increased incidence of cutaneous malignancies and other cancers. Indeed, the spectrum of malignancies encountered in patients with HIV/acquired immune deficiency syndrome (AIDS) parallels that of patients on chronic immunosuppression. One recent meta-analysis found an increased incidence of 20 of 28 cancer types in transplant and HIV/AIDS patients when compared with the general populace.11 This suggests that immunosuppression itself can contribute to the development of cancer. Below, we first consider the mechanisms by which immunosuppression may promote cutaneous malignancy. Then we review specific cases of natural and iatrogenic immunosuppression and consider implications for the emergence and management of cutaneous malignancies. The concept that the immune system may control or eliminate malignancies was formally proposed by Thomas and Burnet more than five decades ago.12,13 Burnet argued that since cells of long-lived animals naturally accumulate mutations, some of which are tumorigenic, it is evolutionarily advantageous for the immune system to eliminate these cells.13 In its strictest form, this tumor surveillance concept remains controversial, in part because of the difficulty of proving a negative—incipient tumors eliminated by the immune system are not detected in the clinic. However, a number of lines of evidence at least indirectly support the notion that the immune system suppresses cancer development. If the immune system naturally suppresses cancer growth or spread, one would predict that patients with impaired immunity would be at higher risk of developing malignancy. This is indeed the case, both in patients with inherited and acquired immunodeficiency. Patients with common variable immunodeficiency (CVID) who have deficits in antibody-mediated immunity display an increased risk for lymphoma and various carcinomas.14,15 Patients with X-linked immunodeficiency with hyper-IgM (immunoglobulin M) and those with selective IgA (immunoglobulin A) deficiency are at higher risk for a variety of gastrointestinal malignancies.15,16 These examples demonstrate that severe, inherited immunodeficiency predisposes patients to cancer development, but the rarity of these genetic syndromes limits the generalizability of this finding. Just because some patients with inherited immunodeficiency develop cancer more frequently, it does not follow that the immune system in the much larger group of healthy individuals naturally prevents tumor development. More persuasive evidence in this regard comes from patients who are therapeutically immunosuppressed for autoimmune disease or for transplantation. It is estimated that over half a million patients have received organ transplants in the United States and the increased incidence of various malignancies in these patients has been amply documented. A recent study of 175,000 solid organ transplant recipients in the United States revealed an increased risk for 32 types of cancer in patients who had undergone lung, liver, heart, and kidney transplantation.17 Notably, the risk was increased both for tumors known to be caused by oncogenic viruses (implying that a decrease in antiviral immunity may contribute) and for those in which no viral cause is known (suggesting that impaired immune surveillance may play a role).17 Strikingly, in a prospective trial of kidney transplant patients on cyclosporine, the incidence of malignancies increased in a dose-dependent fashion and the majority of these were cutaneous malignancies.18 The increased risk of carcinogenesis in this group is not solely explained by decreased tumor surveillance, however. Several of the agents used in immunosuppressive regimens are themselves carcinogenic. In experimental studies, cyclosporine was shown to increase adenocarcinoma invasiveness and tumor growth even in mice that are already immunocompromised.19 Similarly, in squamous cell carcinoma (SCC) samples from patients treated with cyclosporine, there was a significant increase in the level of activating transcription factor 3 (ATF3), a transcription factor that can impair p53-dependent cellular senescence and thereby promote tumorigenesis.20 As with cyclosporine, use of the immunosuppressive drug azathioprine is associated with an increased risk of malignancy, in this case SCC.21 It is thought that azathioprine enhances photosensitivity, leading to a direct increase in mutagenic adducts in the deoxyribonucleic acid (DNA) of keratinocytes.22 In summary, the greater propensity for tumorigenesis in transplant recipients likely reflects an interplay between impaired immune surveillance, long-term exposure to carcinogenic drugs, and heightened sensitivity to environmental carcinogens such as UV light and oncogenic viruses. Further evidence for the tumor surveillance hypothesis can be gleaned from studies on patients infected with HIV. If untreated, these patients have decreased numbers of circulating CD4+ (cluster of differentiation 4 +) T cells and consequent deficits in adaptive immunity. Patients with HIV show an increased propensity to develop malignancies that are both related and unrelated to oncogenic viruses. Risks of Kaposi’s sarcoma (KS), lymphoma, and cervical, anal, and hepatocellular carcinoma are all elevated in patients with HIV.23,24,25 Lung cancer and multiple myeloma risks are also elevated.23,24,25 KS, non-Hodgkin’s lymphoma, and cervical cancer become much more prevalent as CD4+ counts drop and are therefore among the AIDS-defining illnesses.26 Interestingly, even lung cancer incidence is inversely correlated to CD4+ counts, despite the lack of a known viral etiology.25,27 This last fact in particular supports the notion that the immune system naturally suppresses cancer development. Perhaps, the most striking evidence of tumor surveillance is provided by the presence of immune cell infiltrates in many tumors and the ability of these cells to clear even advanced disease when sufficiently activated. Increasing numbers of infiltrating T cells have been shown to correlate with improved prognosis in a number of cancers, including those of lung, breast, and colon.26,28,29,30 Similarly, it had long been clinically observed that some melanomas spontaneously regress. Upon pathologic sampling of these tumors, dense infiltrates of T cells were found to be attacking melanoma cells.31 These observations coupled with the knowledge of cell surface proteins that downregulate T cell function led to the development of a novel class of cancer therapeutics aimed at activating the immune system. These immunostimulatory medications are monoclonal antibodies that target one of two cell surface proteins—cytotoxic T-lymphocyte associated protein 4 (CTLA4) or programmed death 1 protein (PD1). Ipilimumab, the first anti-CTLA4 monoclonal antibody to reach the market, was FDA approved on the strength of phase III clinical trials in patients with metastatic melanoma. In patients with stage III or IV melanoma who had failed previous therapies, treatment with ipilimumab improved overall survival, with a median overall survival of 10 months.32 A second phase III trial in previously untreated patients showed improved overall survival with ipilimumab plus dacarbazine versus dacarbazine alone.33 Recent long-term analysis of patients in this trial showed a 5-year survival of 18.2% in patients treated with ipilimumab plus dacarbazine versus only 8.8% for patients treated with dacarbazine alone.34 Two anti-PD1 monoclonal antibodies have been recently approved in patients with advanced melanoma. Pembrolizumab was approved in an accelerated fashion in 2014 for patients with unresectable or metastatic melanoma. Preliminary results from a phase III trial presented at the 2014 Society of Melanoma Research Congress revealed that patients treated with pembrolizumab had improved progression-free survival and an overall response rate of at least 21 to 24%. Nivolumab, another humanized monoclonal antibody to PD-1, was approved for patients with melanoma that has progressed during treatment with ipilimumab. It showed strong efficacy in the Checkmate 066 Phase III trial in which 1-year survival was 73% compared to 42% for patients treated with dacarbazine.35 Progression-free survival was also increased. UV radiation has long been known to contribute to cutaneous malignancy. This is particularly true of UVB radiation, which has been shown to promote BCC or melanoma following intense exposure and SCC following more chronic exposure.36,37 Irradiation by UVB has direct carcinogenic effects through the formation of mutagenic photoadducts in DNA as well as through generation of reactive oxygen species that attack DNA. Not surprisingly, a number of UV-associated mutations in oncogenes and tumor suppressors are found in the tumors of patients with cutaneous malignancies as well as in surrounding premalignant skin. A less appreciated role of UV radiation in promoting tumorigenesis is its contribution to immunosuppression. Seminal animal studies in the 1970s demonstrated that cutaneous malignancies in mice could be rejected when grafted onto immunocompetent recipients, but not by syngeneic animals first exposed to UV irradiation.38,39 Subsequent studies revealed that irradiation induced regulatory T cells (Tregs) that can impair the immune system’s ability to destroy tumor cells. The extension of these findings to the development of cutaneous malignancies in humans is plausible, but remains to be formally demonstrated. UV irradiation has been shown to decrease propensity for allergic responses such as delayed-type hypersensitivity or contact dermatitis, and indeed UV light exposure has been used as a therapy in atopic dermatitis. While this demonstrates that UV irradiation in humans can weaken allergic immune responses, these responses are not thought to be involved in controlling malignancies. Nonetheless, there is an indirect link between UV-mediated suppression of allergic responses and the development of cutaneous malignancies. Patients with a history of skin cancer were much more likely to have decreased contact hypersensitivity to a chemical irritant following UV irradiation compared to patients without skin cancer.40 Thus, impaired allergic responses correlate with a history of cutaneous malignancy, but any causal link remains to be demonstrated. Mechanisms proposed to contribute to UV-induced immunosuppression include induction of the anti-inflammatory cytokine interleukin-10 as well as the depletion of antigen presenting cells in the skin.41,42 Taken together, the above findings demonstrate that patients with impaired immunity are at higher risk of developing a variety of malignancies, likely through impaired tumor surveillance coupled with the direct oncogenic effect of some immunosuppressive medications, UV light, and oncogenic viruses. They also demonstrate the potential of the immune system to clear cutaneous malignancies when appropriately activated. A number of cancers are known to be caused, at least in part, by oncogenic viruses. In the setting of immunosuppression, latent viral infections can be reactivated and the ability to respond to ongoing infections is compromised. Therefore, some virally mediated cancers occur more frequently in immunosuppressed patients.43 Cancers associated with viral infection include KS (human herpes virus 8), lymphoma (Epstein Barr virus), cervical and anal carcinoma (human papilloma virus [HPV]), and hepatocellular carcinoma (hepatitis B and C viruses). HPV DNA has been detected in patients with nonmelanoma skin cancer, in particular up to 80% of SCC samples in some studies.44 Interestingly, HPV DNA is found more commonly in sun-exposed skin compared to protected skin, suggesting a potential synergy between UV irradiation and infection. However, the particularly high-risk serotypes of HPV are not always found in SCC lesions. These HPV serotypes express proteins that inactivate the tumor suppressors p53 and Rb, but SCCs often have direct mutations in p53 and Rb pathway components, obviating a need for the virally expressed proteins.45 The exact contributions of decreased tumor surveillance, unchecked viral oncogenesis, or both to the increased incidence of nonmelanoma skin cancer in immunocompromised patients remain to be determined. Further evidence of a viral contribution to skin cancer in immunosuppressed patients can be found from Merkel cell carcinoma (MCC). This rare, very aggressive neuroendocrine tumor of the skin is associated with Merkel cell polyomavirus (MCV). Immunocompromised patients are 15 times more likely to develop MCC than their immunocompetent counterparts and they are diagnosed with the malignancy an average of 10 years earlier.46 As with nonmelanoma skin cancer, MCC is more aggressive in immunocompromised patients with 56% of patients succumbing to their disease in one study with a mean time from diagnosis to death of only 13 months.47 HIV is the leading cause of acquired immunodeficiency in the world with an estimated 35 million people infected as of 2013 (World Health Organization). HIV attacks CD4+ T cells, the helper T cells that orchestrate immune responses to pathogens and also coordinate tumor surveillance. Untreated, HIV depletes the body of this vital cell population. When CD4+ T cell counts fall sufficiently, a host of attendant illnesses and opportunistic infections occur. These define the AIDS. The link between HIV infection and cutaneous malignancy is longstanding. The emergence of KS in immunosuppressed homosexual men in the early 1980s led to KS being among the original AIDS-defining illnesses. KS is associated with human herpes virus 8 (HHV8), with nearly all patients exhibiting viral DNA in tumor samples.48,49,50,51 The inverse relationship between KS and CD4+ cell counts provides powerful evidence that the immune system can suppress this malignancy. Consistent with this, the incidence of KS has declined dramatically since the advent of combination antiretroviral therapy (cART), which preserves functional CD4+ levels.52 Further, initiation of cART has been shown to decrease KS lesion size and number and represents a critical component of treatment.53,54 Nonmelanoma skin cancers are the most frequent non-AIDS-defining cancers in HIV+ patients.55 In a large, retrospective study of over 4,000 HIV-infected patients followed between 1988 and 2003, 32% of all malignancies were BCC and 16% were SCC. Patients who have progressed to AIDS have a threefold to fivefold higher risk of developing nonmelanoma skin cancers.56,57 The high incidence of nonmelanoma skin cancers in HIV+ patients may not be surprising since these are also the most common cancers in the general population. However, other characteristics of these tumors may differ in HIV+ patients. One study from the University of California, San Francisco, found earlier age of onset, higher risk of local recurrence and metastasis, and a higher lethality of SCCs in patients with HIV. Interestingly, BCC is found more frequently than SCC in the HIV+ patient population, mirroring the distribution of these tumors in the general populace. As discussed below, this is in contrast to transplant patients who show a relative propensity of SCC. Whether this reflects differences in virally versus chemically mediated immunosuppression or other factors remains to be seen. The aggressive nature of SCC in HIV+ patients necessitates vigilance and aggressive management. Wilkins and colleagues recommend early biopsy of suspicious cutaneous lesions along with frequent monitoring for possible recurrence or metastasis.58 These patients should be considered for sentinel node mapping for tumors presenting with an aggressive clinical presentation. These include recurrent lesions, tumors with depth of invasion more than 2 mm, tumors that exhibit perineural or lymphatic/vascular invasion, and poorly differentiated tumors. Tumors more than 2 cm in diameter on the trunk and 0.6 cm on the “mask” areas of the face, genitalia, hands, and feet are more likely to behave aggressively as well. Adjunctive therapies such as chemotherapy or radiation may also be considered.58 Patients with BCC should be treated in the standard fashion with wide local excision.58 Melanoma—already the most aggressive of common cutaneous malignancies—is even more lethal in patients with HIV. In a case control study of HIV+ and HIV– patients with melanomas of the same subtype and thickness, outcomes were significantly worse in patients with HIV.59 Both disease-free survival and overall survival were reduced among HIV+ patients. Further, the time to melanoma recurrence in treated patients was inversely related to CD4+ counts. This fact coupled with the recent success of immunostimulatory medications in treating advanced melanoma suggests that the immune system may play an important role in controlling this malignancy even in immunocompetent people. Management of melanoma in patients with HIV should follow standard treatment protocols with an emphasis on restoring or preserving immune function through cART. Use of new immunostimulatory medications for melanoma treatment in HIV+ patients is a promising area for the future. The development of effective immunosuppressive medications in the 1980s enabled an enormous increase in lifesaving organ transplantation. The need for replacement organs greatly outstrips supply with over 123,000 patients on waiting lists in the United States (Organ Procurement and Transplantation Network) and the gap continues to widen. Nearly 30,000 organ transplants were performed in the United States in 2013 (organdonor.gov). Further advances in immunosuppressive regimens, surgical technique, and posttransplant care have increased life expectancies for transplant recipients. Five-year survival approaches 85% for kidney transplant recipients, 48% for lung transplant, and 70% for liver and heart transplant.60 These advances have led to a large number of patients living long term with organ transplants. An estimated 140,000 transplant recipients live in the United States currently.60 The requirement for lifelong immunosuppression to prevent transplant rejection leaves these patients in a state of chronic immune deficiency. The deleterious consequences of transplant-associated immunosuppression include cardiovascular disease, heightened susceptibility to infections, and increased incidence of malignancies. Studies across transplant registry cohorts have revealed a twofold to fourfold increased risk of developing cancer in transplant patients relative to matched controls.17 A recent study examined more than 175,000 transplant recipients in the United States over an 11-year period, considering data from transplant and cancer registries.17 These patients had twice the risk of developing malignancies compared to the general population. The risk of developing cutaneous malignancies is particularly elevated among transplant patients with an estimated cumulative risk as high as 70%.61,62,63 This makes cutaneous malignancy the most frequently encountered cancer type in transplant recipients. These cancers include SCC, BCC, KS, MCC, and cutaneous lymphoma.64 Cutaneous malignancies are not only more frequent in organ transplant recipients, but also exhibit a more aggressive course ( The increased aggressiveness of cutaneous malignancies in transplant patients may be explained by alterations in tumor biology, impaired antitumor responses, or both. Evidence for the former comes from the observation that matrix metalloproteinase expression is elevated in SCCs from transplant recipients.67,68 These proteins degrade the extracellular matrix and may thereby provide a path for local invasion and ultimate metastasis. Interestingly, alterations in the matrix metalloproteinase (MMP) profile are also found in surrounding nonmalignant skin of transplant recipients. This finding may play a role in the “field cancerization” that contributes to the high ultimate lesional burden in these patients. It is also likely that impaired tumor surveillance and antitumor immune response allow incipient cutaneous malignancies to grow relatively unchecked. When combined with the direct carcinogenic role of some immunosuppressive medications, this decrease in antitumor response and increase in MMP activity create a vicious cycle that promotes carcinogenesis. Nonmelanoma skin cancers including SCC and BCC are the most frequent cutaneous malignancies in transplant patients, accounting for 95% of observed tumors.60,69 Unlike the general population, transplant recipients have a preponderance of SCC over BCC in a 4:1 ratio. Interestingly, this represents an inversion of the usual findings.70,71,72,73 The risk of developing SCC is elevated 65-fold and the risk of BCC is elevated 10-fold relative to the general population.74 As in the general population, these cancers tend to occur in sun-exposed regions such as the head and neck and upper extremities.74 Other markers of UV-associated skin damage such as actinic keratoses are associated with an increased risk of nonmelanoma skin cancer in transplant recipients.75 Interestingly, heart and lung transplant recipients have a higher overall risk of SCC development than do kidney transplant recipients, likely reflecting the more potent immunosuppressive regimens required for organ preservation in the former group.60 Melanoma risk is also elevated in organ transplant recipients. A threefold to fivefold increased risk of melanoma is present compared to the general population. These lesions occur with a mean duration of 5 years posttransplant.60 In a study of nearly 90,000 transplant recipients over a 10-year period, Hollenbeak and colleagues found an incidence of melanoma of 55.9 cases per 100,000 individuals on an age-adjusted basis, which corresponds to a 3.6-fold greater risk compared to the general population.76 Strikingly, among African-American kidney transplant recipients, the risk was 17.2-fold higher than in race-matched healthy counterparts. The remarkable success of immunostimulatory drugs in combating metastatic melanoma—a success all the more notable for the dismal natural history previously—points to an important interplay between the immune system and malignant melanocytes. Interestingly, oncogenic BRAF mutations appear less commonly in melanomas of transplant recipients.77 This suggests that immunosuppressive medications may activate alternative pathways to promote melanomagenesis or that impaired immune surveillance abrogates the need for this oncogenic pathway.77
12.1 Introduction
12.2 Genetic Syndromes
12.2.1 Xeroderma Pigmentosum
12.2.2 Gorlin’s Syndrome
12.2.3 Melanoma
12.3 Immunosuppression
12.4 Basic Science
12.4.1 Immune Surveillance
12.4.2 Oncogenic Viruses
12.5 Mechanisms of Immunosuppression and Association with Cutaneous Malignancies
12.5.1 Human Immunodeficiency Virus
12.6 Organ Transplantation
12.6.1 Biology
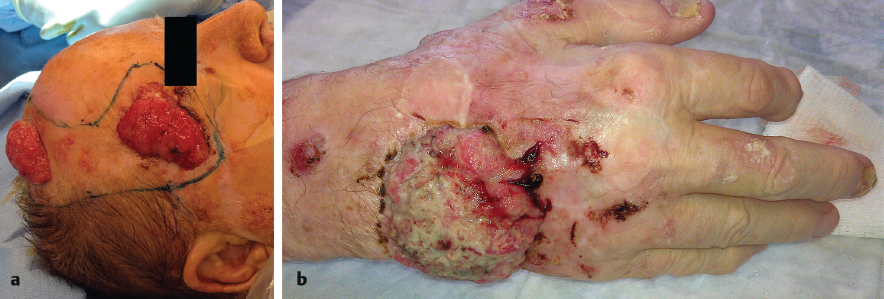
 Fig. 12.1). Data from the Cincinnati Transplant Registry demonstrate that 5% of transplant patients with cutaneous malignancies ultimately succumb to these tumors compared with 1 to 2% of patients who had not been transplanted.65 In kidney transplant patients, 13% of patients exhibit SCC recurrence in the 6 months following excision.61 Patients with metastatic cutaneous malignancies have overall and disease-free survivals at 3 years of only 48% and 56%, respectively.66
Fig. 12.1). Data from the Cincinnati Transplant Registry demonstrate that 5% of transplant patients with cutaneous malignancies ultimately succumb to these tumors compared with 1 to 2% of patients who had not been transplanted.65 In kidney transplant patients, 13% of patients exhibit SCC recurrence in the 6 months following excision.61 Patients with metastatic cutaneous malignancies have overall and disease-free survivals at 3 years of only 48% and 56%, respectively.66
12.6.2 Epidemiology
Plastic Surgery Key
Fastest Plastic Surgery & Dermatology Insight Engine