Introduction
Advances in acute burn care during the past 25 years in terms of decreased mortality and decreased length of hospital stay have been truly remarkable. Current and historical perspectives on burn mortality can be found in preceding chapters. In almost every burn unit in the United States, the length of stay has decreased from nearly 3 days/% burn to less than 1 day/% burn. The success can be stated simply: patients with larger, more severe burns are surviving.
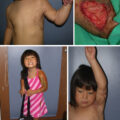
But if patients with larger and more severe burns are surviving, this has created new problems for patients’ quality of life. Although the problems are magnified in massively burned patients, they exist also in smaller burns. These problems are demonstrated in a pediatric burn patient with a 95% total body surface area (TBSA) burn ( Fig. 47.1 ). Cultured keratinocytes were utilized to achieve wound coverage. The child survived; however, when we examined the patient’s current and future reconstructive needs, they totaled 33 potential reconstructive procedures. Thus the reconstructive problems are monumental in a child with very few donor sites. With regard to survival, the results of this patient are impressive; however, we must ask the question: “Has the medical expertise in terms of survival progressed past the ability to reconstruct and rehabilitate patients?” Unfortunately, the answer is clearly “yes.” Are we returning our patients to a society that is not ready financially, psychologically, or socially to accept them? Again, unfortunately, the answer is clearly “yes.”
A pediatric burn patient with a 95% total body surface area burn.
Under Titles II and XVI of the Social Security Act, adult disability is defined as “the inability to engage in any substantial gainful activity, by reason of any medically determinable physical or mental impairment(s) which can be expected to result in death or which has or can be expected to last for a continuous period of not less than 12 months.” For children, the definition differs slightly: “a child under the age of 18 will be considered disabled if she or he has a medically determinable physical, mental, or combination of impairments that causes marked and severe functional limitations and that can be expected to cause death or last for a continuous period of not less than 12 months.” These guiding principles of functional assessment require a further definition. “Medically determinable… impairment” means that the impairment(s) can be demonstrated, witnessed, or otherwise known and described by some third-party means. These may include laboratory tests, physical examination demonstrating signs of the underlying disease process, and disease-specific historical information elicited during the interview. When impairment results from two or more systems, the ratings should be combined according to a combined values chart or its underlying formula. Using the American Medical Association (AMA) formula, the first diagnosis-based impairment is subtracted from a 100% whole person, and each subsequent impairment is subtracted as a percentage of the remaining, or fractional, unimpaired person. Disability ratings can only be performed after a patient has reached maximal medical improvement. This concept is unfortunately both subjective and undefined but retains its utility when applied with equal measures of common sense and medical judgment.
Postburn system-based disability assessment
Description of an alleged impairment should begin before physician introduction. Careful observation of general appearance—how an individual is groomed, enters the building, comports themself while waiting, interacts with clinical staff during check-in, and completes initial paperwork—all provide useful, global insight into how their life has been impacted by burn injury and how they have adapted to it. A whole person’s impairment depends on disruption of organ system function. For each system, impairment is categorized into five classes: 0 (no impairment), 1 (minimal), 2 (moderate), 3 (severe), and 4 (very severe). Generally, these correspond to function and symptoms, where 0 is no symptoms despite strenuous activity, 1 is symptoms only with strenuous activity, 2 is symptoms with normal activity, 3 is symptoms with minimal activity, and 4 is unabated symptoms. In cases where an objective measure is widely accepted to correlate with experiential symptoms, this objective measure becomes the key factor (e.g., see the section on respiratory function, which uses the results of pulmonary function tests as a key factor).
This classification allows assignment from no impairment to complete impairment of the system being evaluated, which can be expressed as a percentage of whole-person impairment. Within each diagnosis-based impairment class, impairment can be modified up or down based on additional clinical information or supplementary diagnostic tests. These vary somewhat for each condition (for full details, please refer to the individual chapters in the most recent edition of the AMA’s Guides to the Evaluation of Permanent Impairment ). The assessment of typical postburn sequelae is described in the following sections.
Constitutional
Body mass, composition, and growth curves in children provide important objective data regarding the overall magnitude of the postburn systemic insult. The weight trend, particularly compared with a preinjury weight, is helpful in estimating the loss of lean body mass, although confounding by body compositional changes does occur. In general, loss of 10% to 30% of body mass correlates with increasingly severe manifestations of malnutrition and catabolism, namely impaired wound healing, pressure sores, and pneumonia. Losses approaching 40% of preinjury body mass (in survivors seen for disability assessment) indicate a near-fatal systemic insult of malnutrition combined with postinjury hypermetabolism.
Although the gold standard of body compositional analysis is potassium-40 scintillation counting coupled with deuterium oxide dilution measurement of total body water, whole-body dual energy x-ray absorptiometry (DEXA) provides a useful and more readily available surrogate. Whole-body DEXA scans provide bone density measurements of the axial and appendicular skeleton, as well as assessment of peripheral and visceral fat mass, bone mass, and extremity/central lean mass. Bone metabolism is markedly disturbed after severe burn injury; accordingly growth arrest is seen in growing (prepubertal) children. This is attributable to stalled endochondral bone formation. Patients are also prone to fracture from trivial trauma such as ground-level falls, and fracture healing is slowed.
Skin/integument
As the skin is the organ most visibly affected by burn injury, photo documentation of affected areas can provide efficient insight into the magnitude of the injury and the status of the healing process. Scars from healed burn wounds or skin grafts and donor site morbidity are described by TBSA and location. It is also important to note associated venous congestion, tissue edema, chronic wounds, pain, itch, tissue disfigurement, and distortion of adjacent unburned mobile structures (nipple, umbilicus, and/or genitalia) by burn scar contraction. Large burns (>20% TBSA) can result in homeostatic impairment of the skin. Manifestations may include subjective heat intolerance, impaired thermoregulation, and loss of sweat function in the scars, or cold intolerance owing to loss of adipose tissue insulation. The latter is of particular concern after deep or infected burns with fascial excision or other significant adipose tissue debridement in the course of burn care. Although a goal of burn care is rapid, durable wound closure, chronic wounds still occur after burn injury. If present, these should be described including size, depth, location, exudate/odor, and status of the healing process/granulation tissue. Previously applied wound therapies should be described. If a wound has been present beyond 3 months, a more detailed assessment of the reasons for failure of healing is warranted (including malnutrition, pressure, infection/colonization, osteomyelitis, loss of sensation, tension, and lack of blood flow). This assessment may include a search for neoplasia (Marjolin ulcer) and related examination of the draining lymph nodes because nonbasal cell skin cancer (not in remission) is assigned 58% whole-person impairment. The claimant’s history is the key factor in classifying nonfacial skin/scar-related impairment, focusing on the impact of the skin-related conditions on an individual’s ability to perform activities of daily living (ADLs). Whole-person impairment resulting from nonface skin disorders can range from 0% to 58%.
Facial injuries, scars, and ear/nose/throat problems
Burn scars involving the face can be a significant cause of impairment. Beyond aesthetics, these may include cicatricial microstomia (causing weight loss and malnutrition), loss of facial expression, and nasal deformity/tissue loss with associated airway dysfunction and loss of humidification. Air passage deficits, including nasal injuries and vocal cord paralysis, are rated from 0% to 58% whole-person impairment based on the key factor of degree of dyspnea and interference with daily or work activities. Voice and speech impairment is rated at 0% to 35% of the whole person, based on the key factors of speech audibility, intelligibility, and functional efficiency of speech in everyday communication. Ear loss, in addition to the aesthetic deficit, can compromise sound localization/lateralization and make it difficult to wear glasses or similar headgear that rests on the ears. Auditory function may be compromised in several ways after burn injury. Significant blast injuries are associated with tympanic membrane (TM) rupture. Middle ear infection, often with TM perforation, may complicate convalescence from severe burns; multidrug-resistant organisms are usually observed, and clearance can require prolonged treatment. Resulting TM scarring may reduce auditory acuity. Several ototoxic medications (especially aminoglycosides and furosemide) are routinely used during critical care of the severely burned patient. The key factor for hearing evaluation is decibel threshold sum audiometry using sounds of 500, 1000, 2000, and 3000 Hz. Whole-person impairment from binaural hearing loss ranges from 0% to 35%, with the latter value reflecting complete hearing loss. Facial disfigurement is rated separately from overall skin assessment, and the key factor determining classification is the degree of facial anatomic distortion, loss of expression/facial features, and the degree of difficulty experienced by the patient in social settings because of facial disfigurement. Whole-person impairment resulting from facial scars/disfigurement can range from 0% to 45%.
Musculoskeletal
Burn-related amputations are not infrequent, especially in the setting of electrical injury. If an amputation is present, the requisite description is straightforward, including the level of the amputation, the condition of the stump (note if chronic wound present), any prosthetic used, how well it works for the patient, and specific (work and home) activities that are difficult or require adaptation because of the amputation.
The main cause of musculoskeletal impairment after burn injury is scar contracture across joints. In the acutely injured state, patients typically assume a “position of comfort.” Contraction of the burned joint may reduce the area of the wound to heal but at the cost of losing range of motion with scar formation. The use of splinting, exercise, and release with tissue interposition have all been shown to mitigate this problem, but rarely is function completely restored to the preburn state. In describing scar contractures, particularly involving joints, one may note that the resting position is often abnormal. Range of motion, strength, associated chronic wounds or ulcers, and pain/tightness at the scar also provide helpful medical evidence of impairment. The description of specific daily living or work activities that the patient finds difficult because of specific scars/contractures is needed to communicate the experiential severity of impairment.
Prolonged immobilization and excessive use of static splints may also lead to joint fibrosis and impaired range of motion. Heterotopic ossification, generally occurring in patients with burns greater than 30% TBSA, can cause near complete loss of joint mobility. When it occurs, the joint becomes immobilized in the position in which it was maintained. It causes significant pain, and the lost range of motion is generally refractory to surgical intervention and rehabilitation. For example, at the elbow, the ulnar nerve at the cubital tunnel can be affected.
Muscular conditions of systemic import may accompany burn convalescence. Sarcopenia is increasingly diagnosed after critical illness, sepsis, and prolonged immobilization. Rhabdomyolysis and compartment syndromes may lead to the rapid loss of mass of involved muscles. Especially common after electrical injury, these may exacerbate muscle wasting and skeletal muscle protein catabolism caused by the burn injury proper. Loss of lean muscle mass leads to decreased strength and endurance and can contribute to metabolic derangements including altered glucose homeostasis and decreased insulin sensitivity. Muscle bulk can be assessed by the examiner and extremity circumference measurements reported if they appear grossly abnormal. Ultrasound is increasingly used to quantitate the degree of sarcopenia (e.g., midfemur vastus lateralis thickness), but its role in routine disability assessment is not yet widely established. The key factor for musculoskeletal impairment classification is the diagnosis itself, supplemented with the “functional history,” and comprises the extent to which the diagnosis-defined problem interferes with vigorous activity, work, daily living, and basic functioning. It also considers the extent to which another person is required to accomplish these tasks. Because of the complexity in rating nonamputation impairments of the extremities, the reader is advised to obtain and refer to the most recent edition of the Guides to the Evaluation of Permanent Impairment.
Hand function
Hand function is both uniquely important to daily and work activities and frequently impaired by burn injury and scars. Loss or deformity of digits leads to a variety of deficits. Complete loss (amputation) results in the following impairment ratings:
-
■
Ring/small finger: 10% of hand, 9% of upper extremity, and 5% whole-person impairment
-
■
Index/middle finger: 20% of hand, 18% of upper extremity, and 11% whole-person impairment
-
■
Thumb: 40% of hand, 36% of upper extremity, and 22% whole-person impairment
-
■
Hand: 90% of upper extremity and 54% whole-person impairment
-
■
Entire upper extremity: 60% whole-person impairment
Flexion contracture or boutonniere deformity digit(s) leads to impairment in dexterous movements, and extension contracture compromises grip strength and carrying tasks. Scoring is more complex for partial losses and functional impairments but may not exceed the impairment rating for amputation. Because of the hand’s complex tissues and its response to splinting, immobilization, and vasoactive medications, it is not uncommon for muscle, tendon, and bone/joint involvement to be demonstrable in addition to the obvious skin/soft tissue cicatrization.
In the lower extremity, amputation results in the following impairment ratings:
-
■
Lesser toe: 3% of foot/ankle, 2% of lower extremity, and 1% whole-person impairment
-
■
Great toe: 17% of foot/ankle, 12% of lower extremity, and 5% whole-person impairment
-
■
Foot/ankle: 70% of lower extremity and 28% whole-person impairment
-
■
Entire lower extremity: 40% whole-person impairment
For nonamputation impairment at the upper and lower extremities, if none of the diagnosis-based grids reflects the patient’s impairment (as is often the case with significant musculoskeletal compromise after burn injury), then impairment can be rated according to range-of-motion testing. A comprehensive description of this process is beyond the scope of this chapter but can be found in Rondinelli et al.
An assessment of gait and balance (i.e., heel/toe, tandem gait, and Romberg tests) provides insight into the coordinated function of the nervous and musculoskeletal systems. Impairment of the ability to respond quickly to changing conditions (general weakness, loss of balance, or unsteadiness) can impair the ability to safely function in physically demanding occupations. Exertional tolerance, although subjectively reported, can be assessed by asking how far the patient can walk without resting or how many flights of stairs can be climbed without stopping. The reason for exertion limitation (e.g., shortness of breath, musculoskeletal cramps, general weakness, joint pain, chest pain, back discomfort, or other) often provides important insight into the dominant underlying disease state.
Neurologic
Both focal and global nervous system problems are possible after burn injuries. Traumatic brain or spinal injury may be seen in high-energy automobile crashes, blast injuries, and escape-related injuries. Burns sustained in closed-space fires are frequently accompanied by the inhalation of a cocktail of toxins and combustion byproducts. These cause inhalation injury (discussed later), but carbon monoxide, cyanide, and other metabolic poisons may also cause global hypoxic insults (classically the hippocampi are most vulnerable to hypoxia, with impairment in learning and memory). Cerebral edema often accompanies carbon monoxide poisoning or hypoxic insult, and herniation syndromes may lead to neurologic devastation. Cardiac arrest may also accompany severe burn injury (usually hypovolemic) with hallmark cerebral watershed infarcts between the distributions of the anterior, middle, and posterior cerebral arteries. Hypoxic and ischemic insults may lead to alterations in consciousness and awareness. Impairment is rated at from 0% to 100% of the whole person, with continuous impairments (e.g., nonepilepsy) rated higher, from 31% to 100% of the whole person. Alternatively, if consciousness and awareness remain intact, alterations in mental status, cognition, and highest integrative function may be present after traumatic injury or severe central nervous system insult. Resulting impairment is rated from 0% to 50% of the whole person, based on mental status exam and interference with ADLs, occasionally supplemented with neuropsychiatric testing. Individuals who have suffered an electrical injury may develop a condition characterized by progressive degeneration of fine and gross motor coordination. Resultant complications can range from inability to perform work-related tasks safely to an inability to perform the routine ADLs. It is a disease process that takes place over a significant period of time and may worsen after an individual has returned to work. It can be particularly vexing to differentiate this entity from the malingerer, and the objective neurologic exam findings must be cataloged in each case. A polyneuropathy of critical illness is also described and should be considered when prolonged intensive care unit treatment was needed for recovery. A prolonged systemic inflammatory response syndrome, hyperglycemia, corticosteroids (which are endogenously elevated for >12 months after burn injuries), and the use of neuromuscular blocking agents (paralytics) have variously been implicated in its pathogenesis.
Focal peripheral nerve lesions are also possible owing to postburn compartment syndromes. In the upper extremity the ulnar nerve is particularly vulnerable within Guyon’s canal and at the cubital tunnel, whereas the median nerve is vulnerable at the carpal tunnel. If a compartment syndrome is present for 4 to 6 hours without adequate release, irreversible nerve damage may occur anywhere within the affected compartment(s). Fortunately, the dire sequelae of contracture and complete defunctionalization of the upper extremity described by Volkman are infrequently encountered owing to rapid escharotomy and fasciotomy of impending compartment syndromes as a routine part of burn center care. The rating of impairment owing to peripheral nerve lesions is based grossly on sensory and motor findings, and the reader is advised to refer to the latest edition of the Guides to the Evaluation of Permanent Impairment for both the upper and lower extremities. ,
Characterization of gait, station, balance, sudomotor function, strength, deep tendon reflexes, and sensation (including as needed pain/temperature, light touch/two-point discrimination, and vibratory/joint position sense) deficits should be done; a detailed neurologic exam may be supplemented with electromyography or nerve conduction studies if needed.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree