Flexor Tendon Laceration
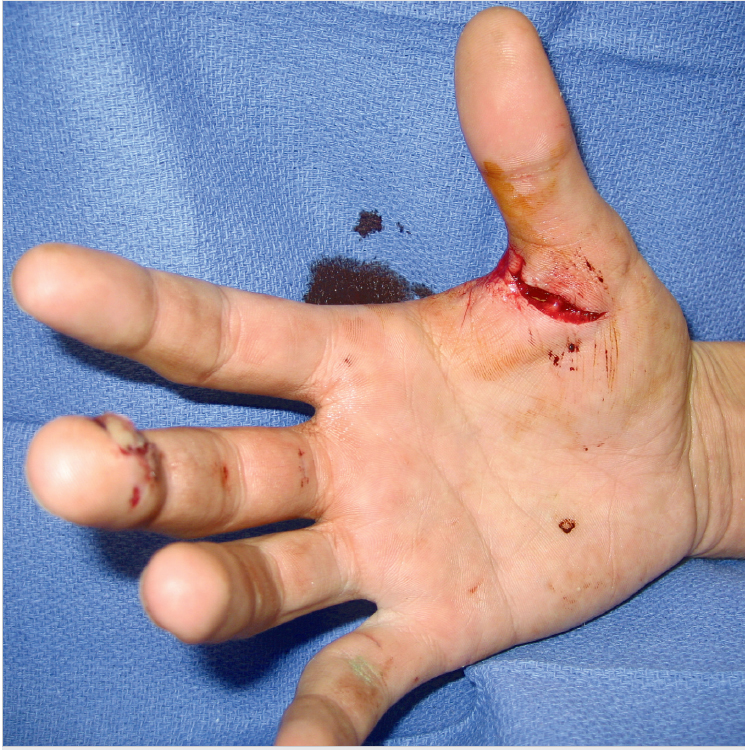
Description
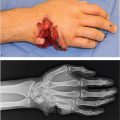
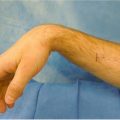
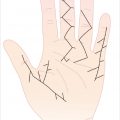
Laceration over the volar first web space, extending onto the thenar eminence and resulting in injury to the flexor tendon in zones T2 and T3.
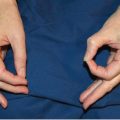
Physical examination reveals inability to actively flex the thumb at the interphalangeal (IP) joint. No other range of motion (ROM), sensory, or strength deficits noted.
Work-up
History
Mechanism of injury (e.g., sharp, blunt, avulsion).
Position of hand and affected digit at time of injury (flexed vs extended).
Time elapsed since injury.
Hand dominance.
Occupation.
Previous hand injuries.
Any associated injuries and medical comorbidities.
Physical examination
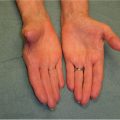
Cascade of the hand
In the resting position, the fingers are flexed, with the degree of flexion increasing from the radial to the ulnar side.
Disruption of the cascade due to abnormal extension of a digit signifies flexor tendon injury.
Tenodesis effect
Passive extension of the wrist causes flexion at the metacarpophalangeal (MCP) and IP joints.
Abnormal extension of a digit signifies flexor tendon injury.
Assess flexor digitorum superficialis (FDS) and flexor digitorum profundus (FDP) function separately along with flexor pollicis longus (FPL).
FDS: Flexion of finger at proximal interphalangeal (PIP) joint while holding all other digits in extension.
FDP: Flexion of finger at distal interphalangeal (DIP) joint while holding PIP joint in extension.
FPL: Flexion of the thumb at IP joint while holding proximal phalanx and MCP joint in extension.
Sensory and vascular examination.
Partial tendon laceration results in weakness, limited movement, triggering of pain with flexion.
Pertinent imaging or diagnostic studies
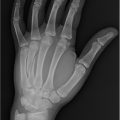
X-ray of hand with three views (anteroposterior, lateral, oblique): Evaluate for bony injury and foreign bodies.
Treatment
Advanced trauma life support (ATLS) protocol.
Antibiotics and tetanus prophylaxis.
If unable to perform flexor tendon repair immediately, any visible tendons may be tagged with suture and the skin may be closed.
The patient should be splinted with the wrist and MCP joints in flexion to minimize retraction.
Flexor tendon repair
Timing
Ideally, flexor tendons should be repaired as soon as possible. Immediate exploration is warranted if nerve or arterial damage is suspected.
In order to avoid staged tendon grafting for zone 2 injuries, flexor tendons should be repaired within 72 hours. Longer delays in repair have been reported for injuries outside of zone 2 with variable outcomes.
Delays > 6 weeks require tendon substitution procedures (tendon grafts, tendon transfers) or salvage procedures (tenodesis, capsulodesis, arthrodesis).
Flexor tendon repairs should be performed in the operating room with a tourniquet.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree