Introduction
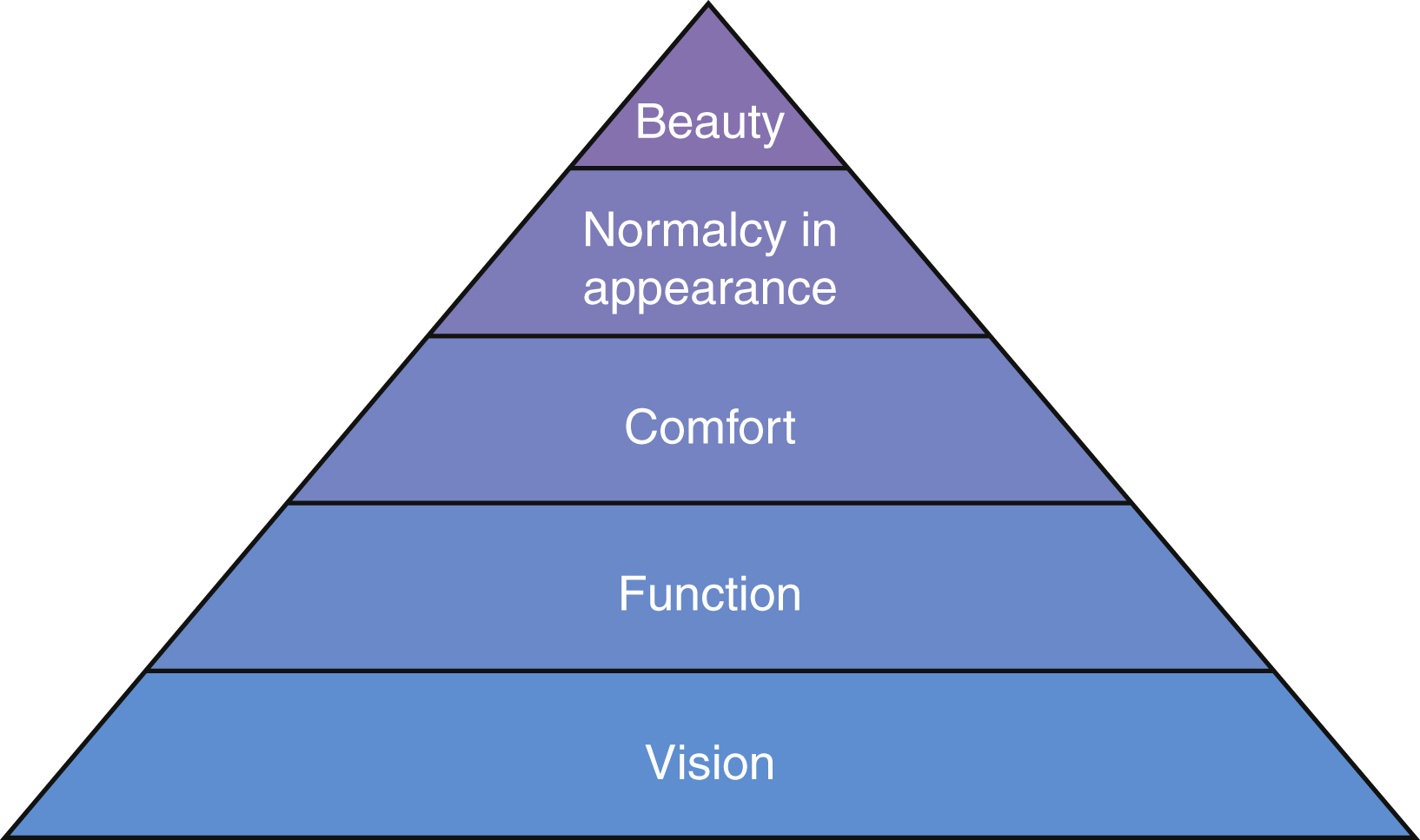
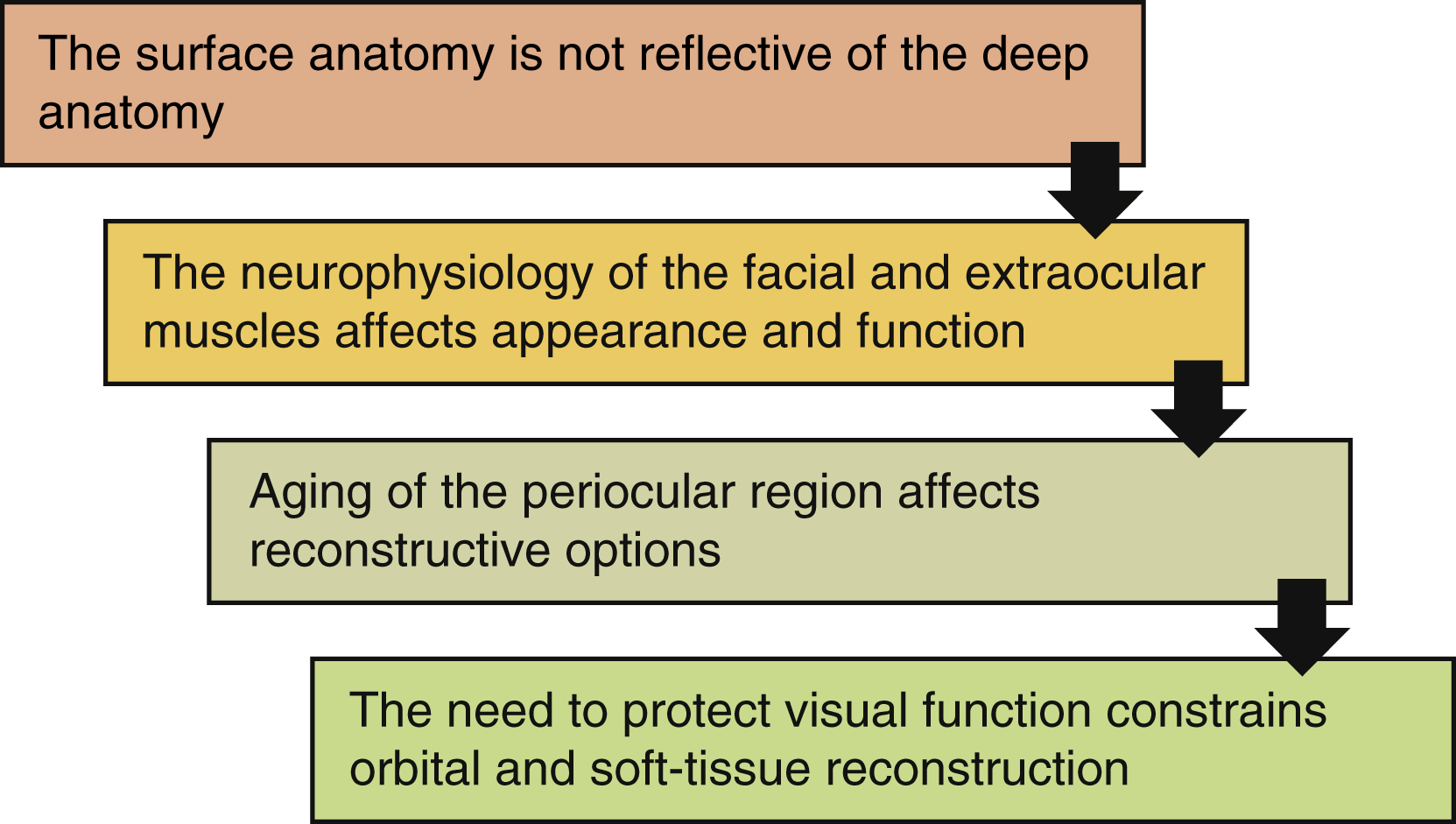
Reconstructive surgery of the face and eyelids has undergone significant changes in the past half century. The increased specialization and advanced understanding of anatomy and physiology of the periocular region has coincided with an increased number of reconstructive options available to the surgeon. With this widened armamentarium and a changing expectation of patients, aesthetic awareness is now a significant part of reconstructive surgery even if the primary goal is protecting the eye and restoring or preserving function ( Fig. 31.1 ).
One of the most significant advances in the past several decades is the awareness of the role of volume in functional and esthetic restoration. Patients with protuberant eyes (negative vector orbit) resulting from exophthalmos or hypoplastic orbit and midface encounter significantly more challenges in reconstruction than those with relative enophthalmos. Similarly, procedures outside the immediate periocular region (e.g., microvascular free flap reconstruction of the midface) can cause significant distortions to the eyelid and secondary functional deficits. The patient’s age is an important factor in the decision to pursue a particular reconstructive option. Older patients with more tissue laxity have generally better options with local tissue rearrangements than younger patients in whom free flaps may be superior.
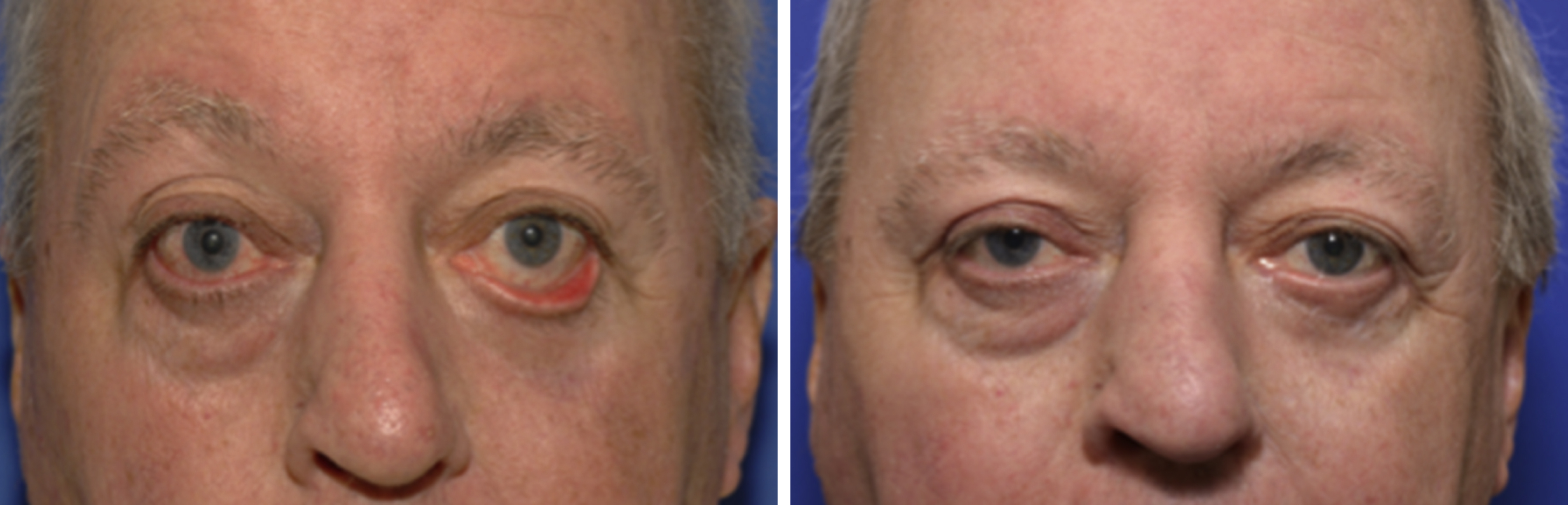
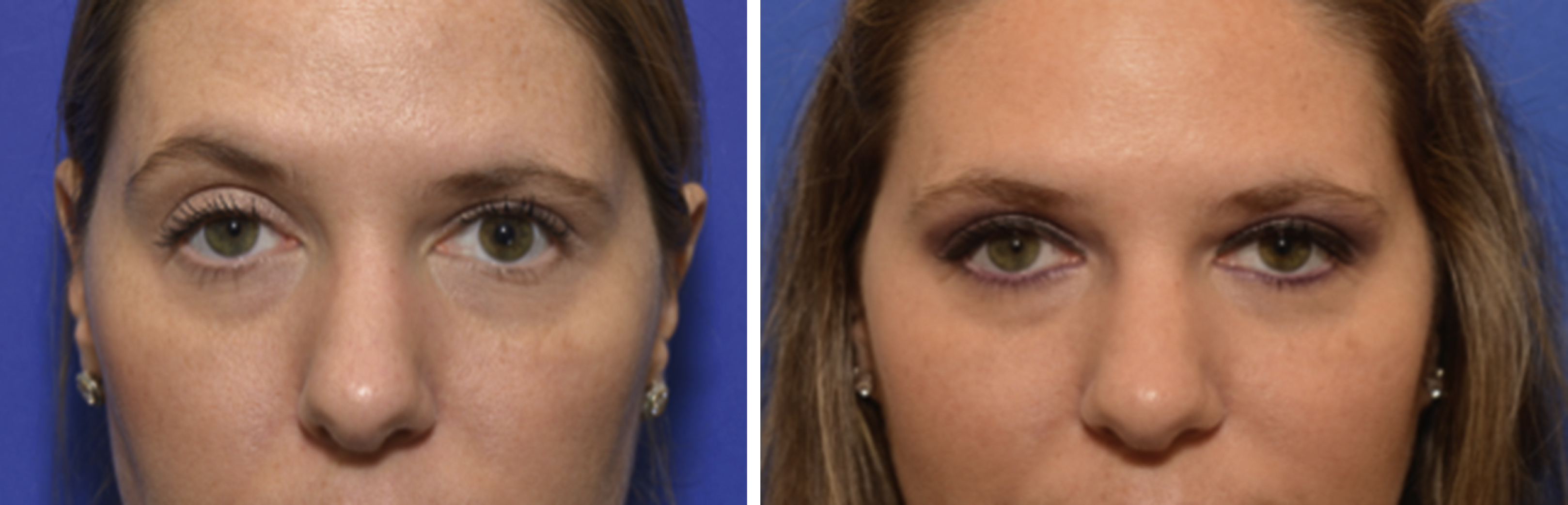
Finally, an important, but often overlooked element in periocular reconstruction is the dynamic physiology of the periocular region. A number of neurological reflex pathways govern the position and function of the eyelids. Hering’s law of equal innervation refers to the shared efferent pathway of the third cranial nerve to both levator palpebrae superioris (LPS) muscles. A patient with unilateral ptosis will often have retraction of the contralateral eyelid and vice versa. Furthermore, in a majority of patients elevation of the eyebrow occurs on the ipsilateral side (Sherrington’s reflex). These combined reflexes often result in retraction of the orbital fat and deepening of the superior sulcus on the ipsilateral side. Matsuo et al have also shown that ipsilateral ptosis can result in increased scleral show by causing a reflex contraction of the inferior rectus muscle in response to the contraction of the levator palpebrae superioris and superior rectus muscles. Rootman et al have demonstrated a 15% change in brow height in patients undergoing ptosis repair ( Fig. 31.2 ). Ignoring such dynamic shifts in reconstructive surgery can lead to functional deficits and aesthetic dissatisfaction with the final outcome ( Fig. 31.3 ) .
Periocular Physiology
The eyelids are a dynamic structure and their function is to protect the ocular surface, simultaneously maintaining corneal wetting and normal tear outflow. Normal horizontal eyelid tension created by the medial and lateral suspensory ligaments maintains the eyelids snug against the eye. The vertical balance of eyelid protractor and retractor muscles ensures complete closure of the eyelids with passive blinking and adequate opening of the eyelids to clear the pupil and visual axis. Contraction of the orbicularis oculi muscle during blinking pumps tears into the lacrimal outflow tract. A complex neural pathway involving cranial nerves V and VII regulates the balance between tear production and outflow. Excessive tearing, or epiphora, from overproduction is most commonly a result of reflex tearing from corneal irritation, such as aberrant lashes or corneal exposure. Exposure keratopathy caused by eyelid malposition can lead to corneal dryness, chronic pain, scarring, infection, loss of vision, and even loss of eye. Epiphora from insufficient drainage can occur when any part of the lacrimal outflow system is interrupted, so special attention is paid to this during medial eyelid surgery.
Periocular Anatomy: Fundamentals of Eyelid Anatomy
The eyelid subunits include the upper and lower lids as well as the lateral and medial canthi. The eyelids can generally be considered a bilaminar structure enveloping the orbital septum and fat (aka the middle lamella).
The anatomical features of the eyelid vary with the distance from the eyelid margin. The vertical height of the central upper eyelid tarsus is 10–12 mm and in the central lower eyelid it is 4–5 mm with some variation between sexes and ethnicities. In most instances the levator aponeurosis is bifurcated in its aponeurotic layer. The eyelid crease is defined by the anterior extensions of the aponeurosis onto the pretarsal skin. Superior to this eyelid crease, the layers include skin, orbicularis oculi muscle, septum, preaponeurotic fat, levator aponeurosis, Müller’s muscle, and conjunctiva. The lower eyelid has a similar multilayer, with the capsulopalpebral fascia analogous to the levator muscle and the inferior tarsal muscle analogous to Müller’s muscle. The eyelid margin from posterior to anterior includes: the mucocutaneous junction, the meibomian gland orifices, the gray line (formed by the marginal portion of the palpebral orbicularis muscle), and the eyelash line.
The levator palpebrae superioris (LPS) and Müller’s muscles in the upper eyelid are the main retractors. The levator muscle originates from the lesser wing of the sphenoid bone and inserts on the anterior surface of the tarsus as a broad aponeurosis and is innervated by the superior division of cranial nerve III (oculomotor nerve). The Müller’s muscle, which is sympathetically innervated, originates from the posterior surface of the levator and inserts onto the superior border of tarsus. The orbicularis oculi muscle is the main protractor of the eyelids and receives its innervation from cranial nerve VII (facial nerve). The superficial musculoaponeurotic system (SMAS) of the cheek interdigitates with the orbicularis oculi muscle in the lower eyelid. Posterior to the orbicularis oculi muscle is the orbital septum. It is an avascular fascial extension of the arcus marginalis of the orbital rim and separates the superficial eyelid adnexa from the orbit, making it an important surgical landmark. Incision of the orbital septum allows access to the various extraconal orbital fat compartments.
The lateral canthal tendon inserts posteriorly and superolaterally onto Whitnall’s tubercle on the inner aspect of the lateral orbital rim. The medial canthal tendon is anatomically more complex because it includes the lacrimal system. The anterior and posterior limbs surround the lacrimal sac. The posterior limb acts as the horizontal supporting band of the lower eyelid, directing the medial eyelid posteriorly to follow the curvature of the globe. Reconstruction at either canthus is aimed at recreating the deep attachments of the canthal tendons inside the orbit to avoid problematic eyelid malpositions.
The conjunctiva is a mucous membrane that forms a single continuous lining over the anterior surface of the eye and posterior eyelids. In reconstructive eyelid surgery, conjunctiva can be rotated or advanced as a flap, grafted from the ipsilateral or contralateral eye, or replaced with analogous nonkeratinizing mucosal epithelium.
A rich vascular supply to the eyelids comes from branches of both the internal and external carotid arteries. These branches form a highly vascularized anastomotic network of vessels that contribute to the high survival rate of grafts and flaps in periocular reconstruction. In general this obviates the need to design flaps based upon specific vessels. As in any surgery, attention to careful hemostasis is important, especially in the periocular region where a retrobulbar hemorrhage resulting in an orbital compartment syndrome can lead to vision loss.
General Principles of Reconstruction
The goal of periocular reconstruction is the restoration of eyelid function, appearance, and maintenance of visual function. Because myriad choices are available to the surgeon (e.g., graft vs. flap), it is valuable to review some general principles that can underlie these choices.
- •
Protection : Since the eyelid’s function is primarily to protect the sight organ, reconstruction should be directed to protect vision. The role of the upper lid is critical in humans. The eyelid must be able to cover the majority of the cornea with a blink and during sleep. Small degrees of opening (lagophthalmos) can be tolerated by many patients during sleep as a result of Bell’s phenomenon whereby the eye is in an upgaze position during most sleep hours. The cornea cannot tolerate significant exposure for long periods of time and must be protected by other means if a staged operation is planned. A number of methods have been employed such as placement of temporary gold weight on the upper lid, tarsorrhaphy, or injection of botulinum toxin to the levator muscle.
- •
Mobility : The eyelid position under normal circumstances is defined by the static anatomy of the periocular structures and the neurophysiology of the protractor and retractor muscles. In reconstructing the eyelid, special attention must be paid to avoid cicatricial changes resulting in inadvertently connecting these separate layers. Patients with scarring between the LPS and orbicularis oculi muscle or orbital septum may have the inability to open and close the eyelids resulting from significantly diminished levator function.
- •
Esthetics : It is critical for the reconstructive surgeon to be familiar with the esthetic principles underlying oculoplastic surgery. For optimal functional and cosmetic outcomes, the surgeon must consider the anatomical relationship of the eyelids to neighboring regions of the face. The face is divided into several esthetic units. Most relevant to periocular reconstruction are its neighboring esthetic regions: the forehead, the cheek, and the nose. Taking into account the unique topography of these borders will aid in incision design, scar camouflage, construction of flaps and grafts, and volumetric balance. It is also helpful to think of normative features that are universal regardless of ethnic origin. Useful examples include the following:
- •
The outer canthus should be approximately 5–10 degrees (or 2 mm) above the medical canthus.
- •
The upper lid generally covers the upper border of the iris on primary gaze.
- •
The lower lid is generally at or within 1 mm of the lower iris border. Any further scleral show is generally considered displeasing.
- •
The upper eyelid peaks nasally to the pupil. Lateralization of this peak can alter a person’s esthetic identity.
- •
A number of technical principles should also be considered in guiding the reconstructive surgeon.
- •
Maintain vascularity. Although recently challenged by some researchers, it is generally accepted that continuous vascularity is necessary in at least one layer of the eyelid if the other layer is to be grafted. A bilaminar grafting of the eyelid can result in necrosis and subsequent tissue loss. Several classically described procedures such as the Hughes or Cutler–Beard procedure (described below) take advantage of these principles.
- •
Diminish excess tension, especially as it applies to the lower lid. Due to the weak support of the eyelid at the canthus, any excess tension especially on the midface will result in an ectropion of the eyelid. For this reason, no downward pull must be felt by the eyelid during reconstruction. In cases where canthal laxity is present, a canthal tightening procedure (canthopexy, canthoplasty or tarsal strip procedure) can be performed. However, the inferior vector pull of the midface must be addressed separately by supporting the midface. Under certain circumstances, a staged approach may provide the ideal esthetic and functional outcome while minimizing scar size ( Fig. 31.4 ).
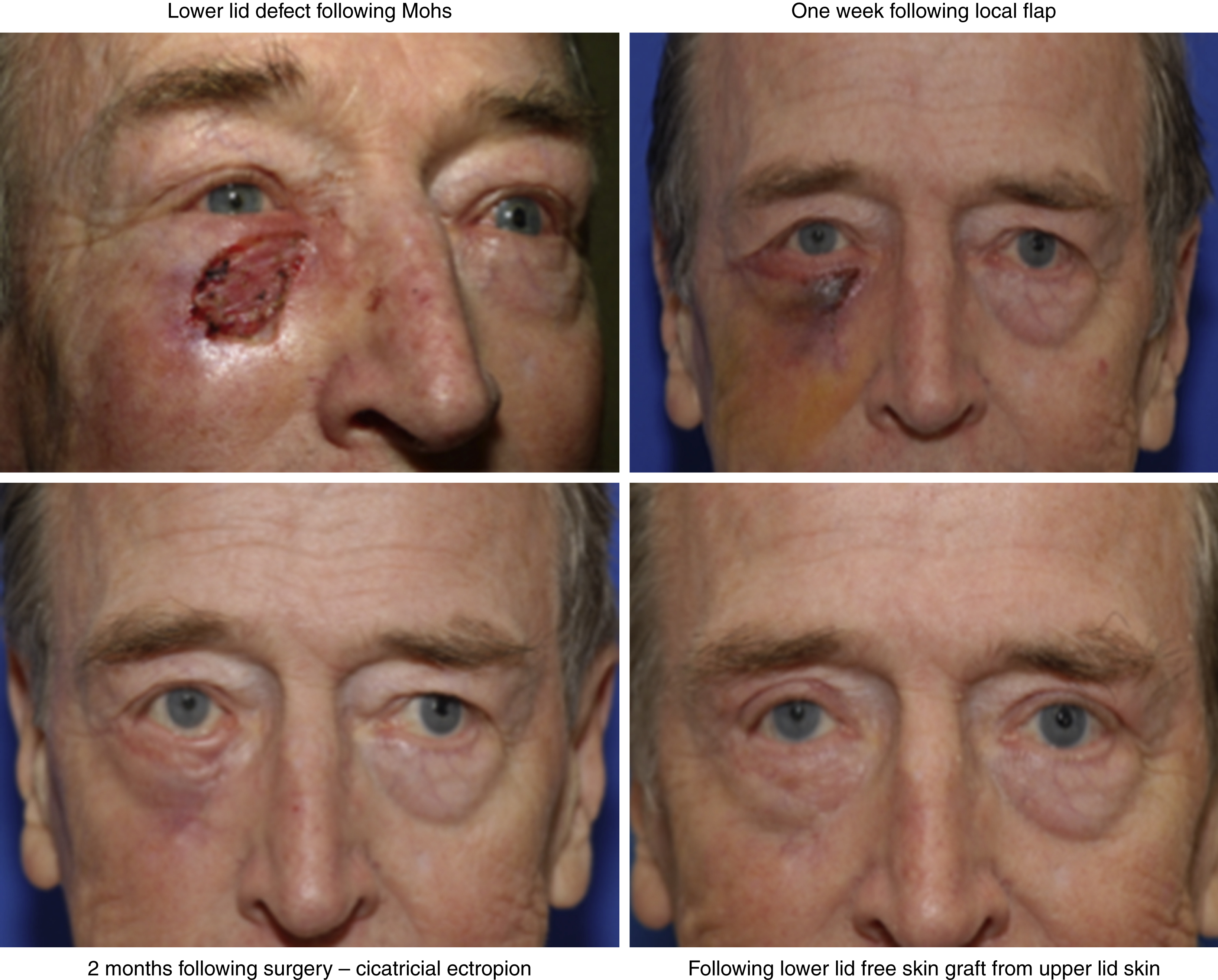
Fig. 31.4
Staged approach to lower eyelid reconstruction. First, the lower eyelid defect is closed with a local advancement flap. Two months later, cicatricial ectropion is noted, which is sometimes unavoidable in older individuals with lower eyelid laxity. This is repaired with a free skin graft from the upper eyelid, paired with a contralateral blepharoplasty for optimal cosmesis.
- •
Choose ideal skin match. Generally, the best match for a defect is the local surrounding tissue that retains the esthetic characteristics of the missing tissue. Thus, whenever possible, a local flap would be preferable. This principle must be weighed against the overall size of the incision necessary to mobilize tissue to cover the defect. If distal tissue is used, the ideal donor size is in descending order: eyelid skin, retroauricular skin or other sources of thin, non-hair-bearing regions such as the supraclavicular skin.
- •
Minimize incision size. It is sometimes said that with a sufficiently long scar most facial defects can be primarily closed. The goal of every reconstructive surgery is therefore not only to repair the existing defect, but minimize the length of incisions and potentially resultant scarring. In addition to gaining familiarity with specific techniques, it is helpful to consider these principles in the perioperative decision planning:
- •
Whenever possible, incisions should follow Langer’s relaxed skin tension lines (RSTLs) of the face that result in more inconspicuous scarring.
- •
Delaying the repair often results in a smaller defect, allowing for a smaller incision.
- •
With cautious and judicious exercise in clinical judgment, both the anterior and posterior lamella of the ipsilateral or contralateral eyelid can be very useful sources of tissue. In patients with upper lid dermatochalasis, the use of upper lid skin can not only provide an ideal coverage of a defect but result in an overall improved facial appearance. Due to the surgeon and patient bias alike, cosmetic enhancement is often not thought of as a goal of reconstructive surgery, often to the detriment of the patient ( Fig. 31.5 ).
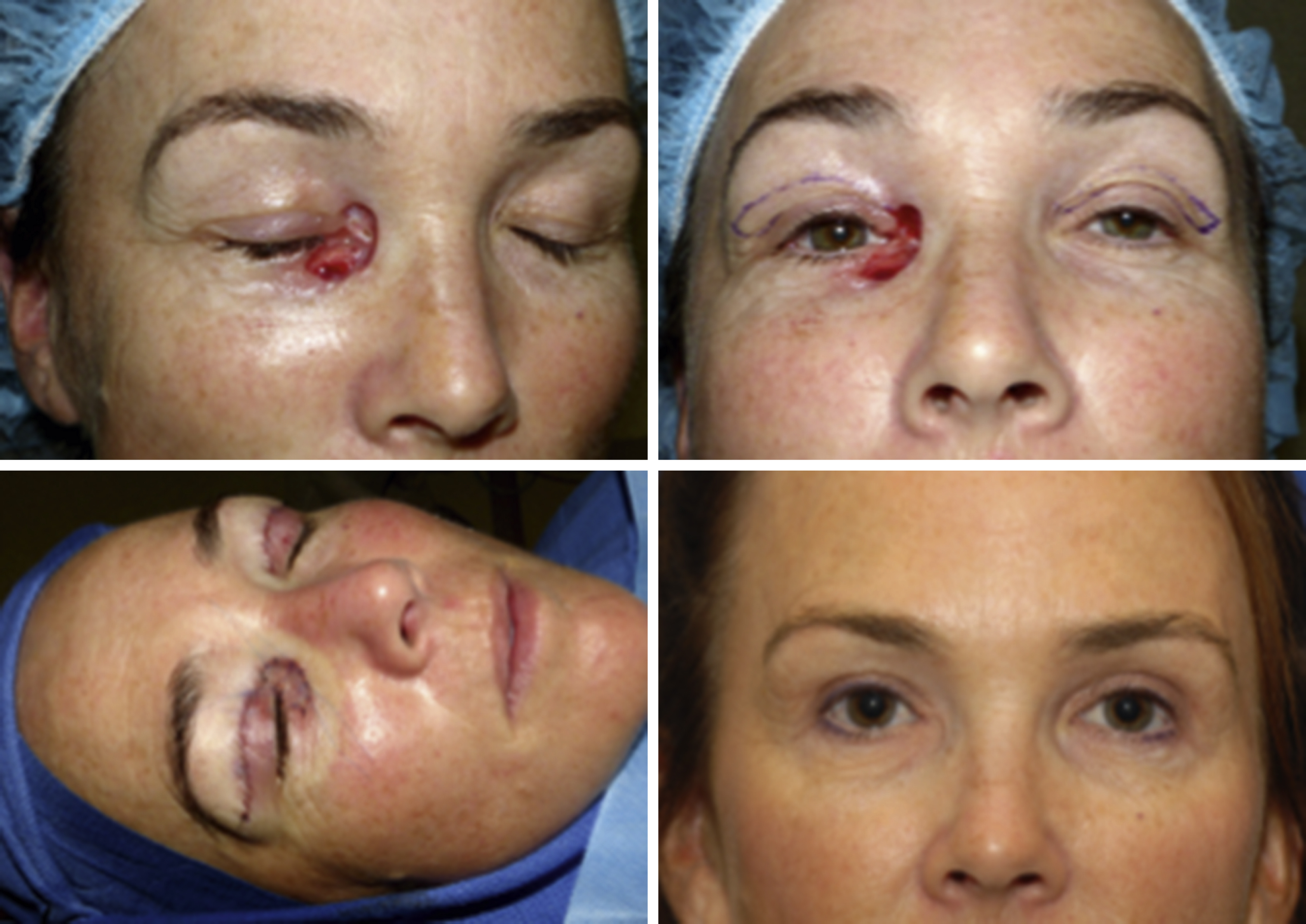
Fig. 31.5
Free skin graft from the ipsilateral upper eyelid was used to reconstruct a medial canthal defect. This was paired with a contralateral blepharoplasty for optimal esthetic result.
- •
Similarly with a conservative approach, another very useful source of posterior lamellar reconstruction is the upper tarsus. As long as 4 mm of vertical upper tarsus is preserved, the remainder can be used to reconstruct a posterior lamellar defect, often obviating the need for more invasive procedures that would require stages.
- •
Anesthesia and Perioperative Tips
Many extensive procedures require the use of general anesthesia, the risk of which must be weighed against the use of local anesthetic in an outpatient setting. This is especially true for patients who are anticoagulated and the elderly. Thus, the appropriate use of local anesthesia can be immensely helpful in reducing perioperative risk. In our practices, we generally use a 50:50 mix of lidocaine 1% with 1:100,000 epinephrine and bupivacaine 0.75% combined with 8.4% sodium bicarbonate in a 1:9 dilution. Occasional hyaluronidase is added to help local anesthetic diffusion. Whenever possible, we inject our local anesthetic with a cannula to minimize ecchymosis. In addition, the use of oral medications containing benzodiazepines, inhaled nitrogen oxide, or combined preparations such as sublingual MKO (midazolam 3 mg, ketamine HCl 25 mg, ondansetron 2 mg – Imprimis, New Jersey, USA) can provide safe and effective means of controlling patient anxiety in an outpatient setting.
Topical proparacaine 0.5% or tetracaine 1% is used before preparation to anesthetize the ocular surface. Corneal shields lubricated with ophthalmic ointment are used to protect the eye during eyelid surgery. When a corneal shield is not used or otherwise temporarily removed intraoperatively, frequent rewetting with ophthalmic petrolatum ointment is done to prevent corneal dryness and abrasions. Surgical marking is done before infiltration with local anesthetic because fine eyelid creases and RSTLs are easily lost when volume is added. Local anesthetic is delivered slowly, making sure to direct the needle in such a way that patient movement does not result in globe penetration. It is useful to slightly bend the needle at 30 degrees and direct it away from the globe while pulling the eyelid away from the globe during injection. In this manner any penetration of the eyelid is immediately observed, and the needle redirected. Depending on the case, a 27G, 30G, or 33G needle can be useful. Transconjunctival injection is less painful than skin injection and is especially useful to anesthetize a lower eyelid full-thickness defect. The needle should penetrate conjunctiva in the fornix (below the inferior edge of tarsus, not into tarsus). In the lateral canthus, additional anesthesia is administered over the orbital rim. In the medial canthus, direct injection into the puncta or canaliculus is avoided.
Techniques
No two defects will be the same. Defects can be described as primarily anterior lamellar, posterior lamellar, or full thickness. A full-thickness eyelid defect involving one-third of the eyelid may be repaired with simple direct closure in an elderly patient with significant eyelid laxity, but in a young patient would require lateral canthal release to achieve closure. In many cases there is more than one design that works and selection is based on surgeon experience and preference. The following provides a list of reliable and predictable reconstructive techniques that, when guided by the principles previously described, will help achieve successful eyelid reconstruction.
Anterior Lamellar Defects
Primary Closure
Healing by granulation or secondary intention may be appropriate for small wounds away from the mobile eyelids, such as in the medial canthal region. Conjunctival incisions in the inferior cul-de-sac can heal nicely without closure. However, in most other periocular areas, scar contracture can cause eyelid malposition.
The simple ellipse may be used to remove most superficial periocular skin lesions and it can be closed primarily. The ellipse should be oriented vertical to eyelid RSTLs to avoid vertical cicatricial tension. Since the ellipse sacrifices normal tissue in addition to the surface area of the original defect, modifications of the ellipse such as the double-S ellipse and O-to-Z-plasty can be used to conserve more normal tissue. Closure is typically performed using interrupted sutures with slight eversion of the wound edges, skin-to-skin, using 6-0 dissolvable material (such gut, polyglactin or poliglecaprone 25) or nondissolvable material (such as nylon or polypropylene, to be removed in 5–7 days).
Local Flaps
For larger anterior lamellar defects, where there is adequate skin elasticity, tissue can be mobilized in the form of advancement or rotational flaps.
Advantages of flaps over free skin grafts are better skin color and texture match, they undergo less contraction, they can support free grafts for posterior lamellar reconstruction, following healing there is near normal innervation of the skin, and they require shorter surgical time (locally available tissue means less injecting, prepping, and draping of a different body site). They also carry a native blood supply, so they are a good choice in smokers and patients with irradiated tissues where vascular supply is already compromised.
Advancement Flaps
The standard unipedicle or bipedicle advancement flaps can be used to repair lower eyelid, upper eyelid, and eyebrow defects. Parallel incisions are designed beginning at one edge of the defect, which becomes the leading edge of the rectangular-shaped flap. The resulting scars fall parallel or into the eyelid creases and any resulting dog-ears are excised.
Transposition Flaps
Hemi-Tripier Flap.
A bipedicled flap designed to reconstruct a lower eyelid defect using upper eyelid tissue in patients who have adequate upper dermatochalasis. It can be transferred as a cutaneous or musculocutaneous flap. The vascular pedicle and pivot point is usually at the lateral canthus and can extend to cover a lower eyelid defect from the lateral to the medial canthus.
Technique
- 1.
The upper eyelid skin crease is marked like for a blepharoplasty. At least 20 mm of eyelid skin should be preserved.
- 2.
A template of the lower eyelid defect is made.
- 3.
The template is transferred to the upper eyelid, with the inferior margin of the lower lid defect aligned with the upper eyelid crease incision.
- 4.
More skin is taken from the upper lid than is required to cover the defect, to allow room for graft contracture.
- 5.
The upper eyelid flap is dissected in the suborbicularis plane.
- 6.
The flap is sutured into the defect using interrupted 6-0 nonabsorbable monofilament suture.
Postoperative Management
Topical ophthalmic ointment and ice packs are applied three times daily. Sutures are removed in 5–7 days.
Fricke Flap
The Fricke flap is a similar, though less frequently utilized, transposition cutaneous flap from the supraorbital area for both upper and lower eyelid anterior lamellar defects. In the first stage, the length of the flap is marked out just above the brow, with the lateral aspect of the flap kept wide. In the second stage the flap is transposed to either an upper or a lower eyelid defect, followed by wound closure.
Rhomboid Flap
These are versatile flaps, especially useful in the periocular region for reconstruction in the medial canthus. Glabellar and median forehead flaps are also used in this anatomical space, but are not discussed in this chapter.
The median forehead flap, not discussed in detail here, is commonly used to repair larger anterior lamellar defects involving the medial eyelid, medial canthus, and/or bridge of the nose especially when down to bare bone. It can be combined with other procedures such as the Mustardé cheek rotation for large combination defects. The flap is constructed along the axis of the contralateral supraorbital and supratrochlear neurovascular bundle and, by necessity, leaves a vertical scar in the forehead. It is debulked during a second stage procedure approximately 6 weeks later.
Full-Thickness Skin Grafts ( Fig. 31.6 )
There are several donor sites ideal for replacing eyelid anterior lamella, which have thin, hairless skin with a close match in color and texture. The graft should be placed on a well-vascularized bed of tissue. Full-thickness skin grafts do not take well on bare bone.
- •
Upper eyelid : Ideal for patients with dermatochalasis, this site has the best color and texture match. A contralateral blepharoplasty can be done at time of reconstruction to achieve aesthetic balance.
- •
Pre- and post-auricular region : Results in inconspicuous donor site scars. The skin color, especially post-auricular, is somewhat lighter and thicker. Availability is also limited by variation in patient’s hairline.
- •
Supraclavicular : Larger surface area available for harvesting. In some patients this area has a similar sun-exposed color match.
- •
Inner upper arm : Large surface area available of thicker and generally lighter skin.