Introduction
The atypical skin lesions are a diverse group of tumors that are uncommon but clinically important. They include a spectrum from benign lesions through to those that demonstrate local invasion and/or distant metastatic potential. Since these lesions are only seen infrequently during clinical practice, it is important to know the patterns associated with the more malignant of these tumors, how they may be discerned from common, benign lesions, and to understand the principles of their management so that clinically impactful mistakes are not made. For this reason, we cover some common surgically relevant lesions of the skin, including common types of cysts. We have divided the atypical lesions into benign or malignant and then by their cell/tissue of origin. Such a framework is not perfect due to our evolving understanding of the molecular and cellular bases of these tumors, but it provides a solid foundation for their study.
Benign Lesions
Benign lesions are clinically important for several reasons. They can be confused with malignant lesions, be symptomatic due to their size, appearance, location, irritation, and bleeding, or may undergo malignant transformation. Knowledge of the uncommon benign lesions can also provide a means to understand their malignant counterparts. Such knowledge is invaluable to the surgeon when examining the correlation between the clinical presentation and the histopathological diagnosis. Any discrepancy between these two should prompt the surgeon to seek clarification and/or a second opinion regarding the histopathological diagnosis. Good communication between the surgeon and the histopathologist is essential for good care.
Cysts
True cysts are defined as epithelial-lined “fluid-filled” spaces and are relatively common in clinical practice. There can be many names for various cysts, including a “wen,” and often terms are incorrectly applied in general usage.
Epidermoid Cysts (Keratin Cysts)
These common cysts enlarge subcutaneously but maintain a connection to the overlying skin at their punctum. Lined by squamous epithelium, they produce soft keratin that fills the cyst with a waxy/cheesy material. Although often called sebaceous cysts, this is a misnomer as they do not contain sebum. True sebaceous cysts are uncommon, arising from the sebaceous glands. There are two types of epidermoid cyst. Epidermal inclusion cysts result from the inoculation of squamous epithelium into the dermis during trauma (e.g., body piercing). Infundibular cysts specifically arise at the infundibular portion of the hair follicle, but are otherwise clinically the same.
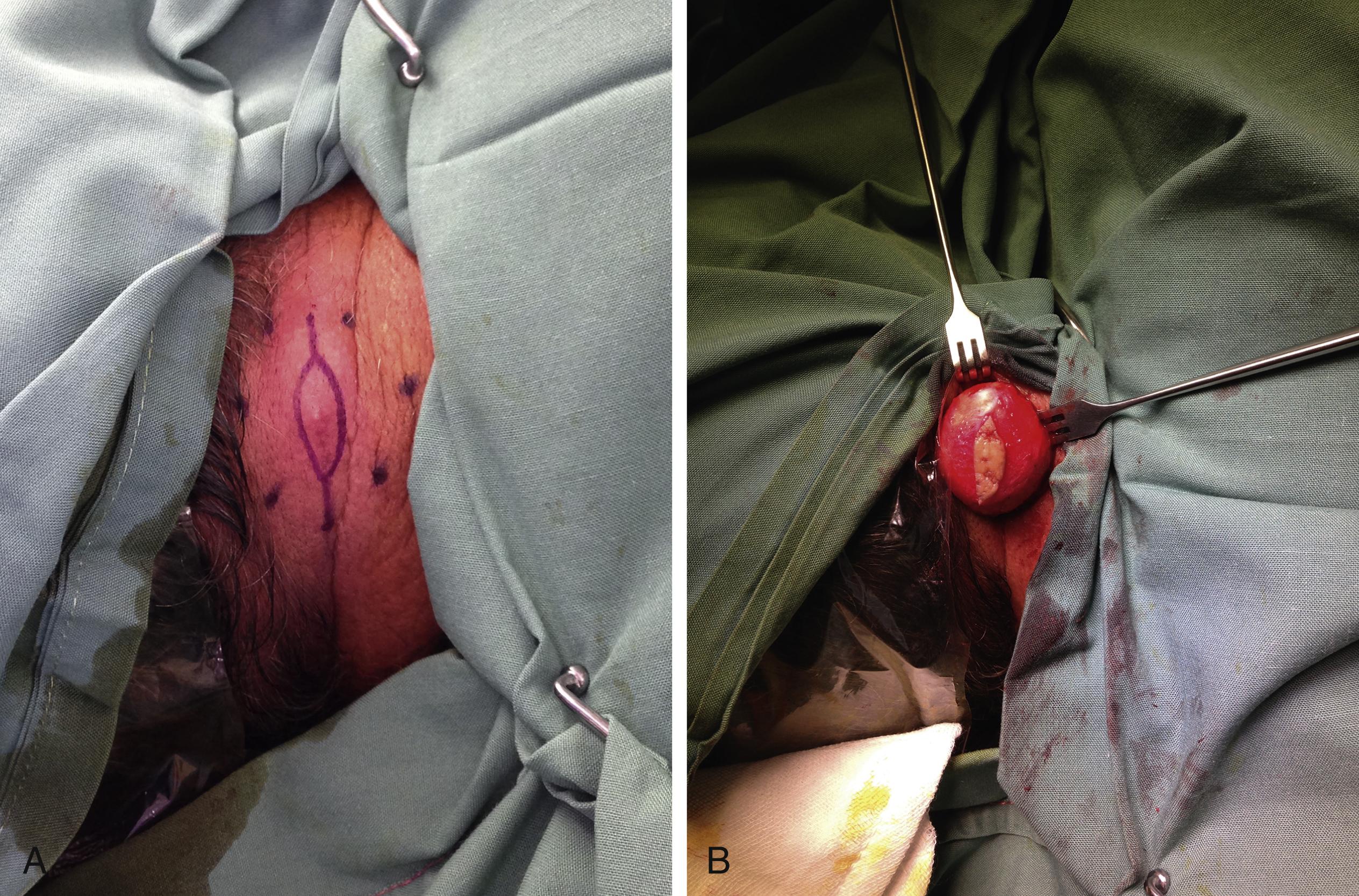
Management depends upon the state of the cyst at presentation. Patients typically present with cysts either as non-tender lumps attached to the undersurface of the skin or when they become infected. Surgical excision in quiescence is ideal, but must include excision of the attachment to the overlying skin (the punctum) ( Fig. 10.1 ). Significant compression can cause a release of keratin through the punctum, but this also increases the risk of infection. In infection, decompression of the cyst abscess, removal of the cyst material, and curettage of the cyst lining allows resolution of the infection and often reduces the size of the lesion down to a small scar. Curettage is associated with a significant risk of recurrence because of its inability to ensure complete removal of the lining of the cyst. Once the scar has settled appropriately, the scar, remaining cyst, and its punctum can be removed to stop recurrence. Uncommonly, they spontaneously resolve by becoming marsupialized and discharging.
Tricholemmal (Pilar) Cysts
Tricholemmal cysts are similar to epidermoid cysts except that they specifically arise from the outer root sheath of hair follicles. For this reason, they are sometimes referred to as isthmus-catagen cysts and are mobile and filled with keratin. They typically arise in the scalp as this has the highest density of hair follicles. They are usually multiple and the tendency to form tricholemmal cysts runs in families. Surgical excision is the treatment of choice and when excised with the overlying hair follicle, recurrence is unlikely. On histology, they can demonstrate areas of nuclear atypia, mitotic figures, and dyskeratosis and therefore be confused with squamous cell carcinoma, but it is rare for them to undergo malignant transformation.
Dermoid Cysts
Dermoid cysts are hamartomas, often containing multiple epithelial derivatives (skin, hair etc.) and occasionally other tissues including fat, cartilage or bone/teeth. They are found in numerous organs and regions of the body. In the skin they are often near the midline or in the head and neck along tissue fusion planes. They can have intracranial, intraspinal, and other deep connections, including down to bone. As they are developmental in their origin and are present at birth, those with a superficial position and/or in the head and neck usually present at an early age, whereas dermoid cysts in other areas are more likely to be incidental findings or found following slow enlargement at any time in life. The key factors in their management are recognition of their potential to involve deeper structures (e.g., nasal dermoid with intracranial extension) and their potential to be associated with other conditions. Excision of the cyst with any communications to underlying structures is effective to prevent recurrence.
Benign Lesions Associated with Epidermis
Acrochorda
Acrochorda ( acrochordon = singular) or skin tags are fibroepithelial polyps that appear as raised, smooth or irregular-surfaced pieces of skin on a small stalk called the peduncle. Nearly half of the adult population has at least one near skin creases in the neck, axilla, groin, breasts and eyelids. Shear forces of skin on skin are thought to be their underlying cause and therefore they are common in obesity. Female gender, human papilloma virus 6 and 11 and familial tendency are all thought to predispose to them. They may be symptomatic due to irritation from clothing or jewelry or when they bleed because of tractional injury. Acrochorda are usually small (2–5 mm) but occasionally larger. They are composed of a fibrovascular core and adipose tissue covered by normal skin. Numerous treatment modalities are available from ligation to cryotherapy and simple surgical removal, but the patient must be aware of the risk of further lesions.
Warts
Warts are focal (verrucous) keratinized lesions caused by human papilloma virus (HPV). The virus replicates in the stratum granulosum, inducing underlying basal keratinocytes to proliferate, causing a hyperkeratotic response. They may appear raised, flat, filiform, cauliflower or ingrown (e.g., plantar warts) and can also occur under or around the nails. Over 150 different types of HPVs have been characterized but, typically, only 1–2 strains cause each normal variant (verruca vulgaris HPV 2 and 4, cauliflower/Butcher’s warts HPV 7, palmoplantar warts/myrmecia HPV 1, flat warts HPV 3 and 10). These are distinct from the HPV strains associated with genital warts (HPV 6 and 8) and those producing an increased risk of intraepithelial neoplasia or invasive tumors affecting the vulva, penis, cervix or oral cavity (HPV 16 and 18). Warts may be singular or multiple, with a predilection for the hands due to contact transfer. Wart infections are self-limiting and resolve once the host mounts an immune response to the virus. Surgical excision produces some release of HP virions, but topical therapies are a less invasive approach to induce an immune response.
Therapy is largely divided into management of the hyperkeratosis and induction of a suitable immune response. Hyperkeratosis management can be undertaken by multiple means, including use of salicylic acid (3%–60%, daily or twice/day), occlusive dressings, cryotherapy, and shaving by scalpel or sharp curette.
Topical therapies to promote an immune response include podophyllin (resin or toxin), formalin (3% solution), imiquimod (Aldara), retinoids such as tretinoin and 5-fluorouracil (5-FU). Podophyllin is available over the counter in most countries and can be applied without specific training. Other approaches that have been used include laser therapy, intralesional agents (bleomycin and interferon-alpha) and topical allergens or caustic agents. While usually successful, they have significant potential side effects not found with the mainstream therapies above. Patient education usually helps to avoid surgical intervention and scarring. Histologically warts demonstrate koilocytes (vacuolated cells with viral infection) and hypergranulosis with columns of parakeratosis and compact orthokeratosis. Typically, the marked hyperkeratosis and papillomatosis are associated with elongated rete ridges sloping inwards to the center of the lesion.
Malignant transformation is sometimes seen in long-standing immune suppression, but it is unclear to what degree HPV infection contributes because the patients already have increased risk of skin cancers. Epidermodysplasia verruciformis (Lewandowsky-Lutz dysplasia) is a rare autosomal recessive skin disorder that increases the susceptibility to HPV infections. These patients have a very high risk of skin cancer due to the increased risk of malignant transformation of their lesions.
Benign Lesions Associated with Hair Follicles
Pilomatrixoma
This benign appendageal tumor typically occurs in the head and neck region and demonstrates differentiation towards hair (follicular) cells. While considered tumors of children, they can occur in adults. They are associated with a mutation in the CTNNB1 gene and while familial cases have been observed, the mode of inheritance has not yet been established. In addition to sporadic cases, they may be associated with Gardner syndrome (familial colorectal polyposis), myotonic dystrophy (especially if multiple lesions), and sarcoidosis. Pilomatrixomas present as firm nodules that are usually solitary and asymptomatic, but are occasionally associated with local pain if infected or inflamed. Usually slow-growing, they can be confused with other skin lesions, including nodular basal cell carcinoma, despite their deep position in the lower dermis or underlying adipose tissue. Lesions often contain calcium deposits that are visible on medical imaging. Pilomatrix carcinoma is well documented but very rare.
Histology demonstrates irregular islands of epithelial cells surrounded by a connective tissue capsule that produces a diffuse lesion in most cases. The epithelial cells are divided into basophilic (germinal) cells around the periphery and shadow cells (anucleated) centrally in keeping with a hair-like process. Chronic lesions have fewer basophilic cells and calcium deposits can be visualized through the use of special stains (von Kossa). The diffuse nature of most lesions leads to a greater risk of local recurrence unless a wide local excision is performed (1 cm or greater). Mohs micrographic surgery (MMS) has been trialed to minimize resection of uninvolved tissue, but its effectiveness remains unclear relative to standard surgical excision.
Trichoepithelioma
Trichoepithelioma is a tumor of the hair follicle and adnexae that is often confused with basal cell carcinoma (BCC). They typically arise as single or multiple small (<1 cm), firm round lesions on the face before or after puberty that may display pearling. The lesions form a basic hair follicle but no hair shafts and may have a different surface color depending on their site of origin. Solitary lesions are typically sporadic, but a familial (multiple) form of trichoepithelioma has been associated with mutations on chromosome16q21 (Brooke–Speigler syndrome). Trichoepitheliomas are composed of nests of basophilic cells often arranged like a hair follicle but they do not display the surrounding myxoid stroma or perinest-clefting found in BCC. A desmoplastic variant commonly forms an annular shape that can be confused with BCC and has a marked desmoplastic surrounding response on histology ( Fig. 10.2 ). Simple surgical excision of all forms without a significant margin is usually effective in preventing recurrence.
Trichofolliculoma
Trichofolliculomas arise directly from hair follicle tissue. They are uncommon small solitary nodules found around the face of adults. A central pore may express sebum and/or hair. They are thought to arise from hamartomatous rests of stem cells that show incomplete differentiation towards hair follicles as supported by the prominence of Merkel cells within the follicular epithelium in these lesions. Their central follicle may have secondary or tertiary follicles and hair shafts may be present within the follicle lumen on histology, helping to distinguish them from trichoepitheliomas along with a prominent surrounding stroma. There is a sebaceous variant where the central follicle has well-differentiated sebaceous lobules emptying into it. They are considered benign with only a single case of perineural invasion ever reported.
Tricholemmoma (Trichilemmoma)
Tricholemmoma is an uncommon benign tumor arising from the outer root sheath of hair follicles. It appears as a warty or smooth papule on the face and neck region, and when multiple lesions are present it is diagnostic of Cowden’s syndrome (hamartomatous intestinal polyposis with multiple tricholemmoma lesions). Cowden’s syndrome demonstrates autosomal dominant germline inheritance associated with mutations of the tumor suppressor gene PTEN (phosphatase and tensin homolog) located on chromosome 10q23.3 but other mutations are occasionally found (e.g., BMPR1A ). PTEN is negative in sporadic tricholemmomas, but often positive in Cowden’s syndrome, presumably due to a loss of function mutation. On histology it appears as lobular downward growths of epidermis and is often surrounded by a hyaline band or thickened basement membrane. Clear cells or cells with prominent vacuoles are typically present (glycogen) and the lobules demonstrate peripheral palisading.
Benign Lesions Associated with Sebaceous Glands
Sebaceous Hyperplasia
Sebaceous hyperplasia is a common condition characterized by single or multiple soft small papules on the face, neck, and occasionally chest in middle-aged to elderly individuals. Most common on the forehead, nose, and cheeks, it presents with raised yellowish areas around a central follicular ostium. It can also affect the areola, penis, vulva, and oral mucosa. Rhinophyma is considered by many to be a severe variant of sebaceous hyperplasia, but has closer linkages with acne rosacea. The pathophysiology relates to the effect of androgens on sebaceous glands. Androgens drive sebocyte turnover, and with advancing age androgen levels drop and sebocyte turnover slows down, resulting in over-crowding by primitive sebocytes that do not contain much sebum. As a result, the glands enlarge with a large number of immature cells. There is no malignant transformation potential, but they may be associated with skin cancer in transplant patients. Sebaceous hyperplasia does not normally require any treatment, however patients may present due to esthetic concerns or because the lesions may be confused with BCC. Treatment options are manifold, including cryotherapy, photodynamic therapy, chemical peels, laser therapy (CO 2 or pulsed-dye), shave excision or formal excision, but all of these are associated with varying degrees of scarring and/or pigmentation changes. Oral retinoids (e.g., isotretinoin) have been used with some success, but sebaceous hyperplasia can recur upon cessation of therapy therefore they are indicated only for severe disfiguring sebaceous hyperplasia.
Benign Sebaceous Adenoma
A benign neoplasm with a well-differentiated sebaceous pattern that presents as a slowly enlarging smooth, sometimes yellow papule with a central depression on the face and scalp. It can readily mimic BCC and is distinguishable from sebaceous hyperplasia histologically by a higher turnover of sebocytes, good differentiation of these cells, and because it is often mixed with other pilosebaceous components (e.g., hair). Benign sebaceous adenoma is the benign end of the spectrum of neoplasms involving sebaceous differentiation. Sebaceous neoplasms as a whole can show variable degrees of differentiation (from well to poorly differentiated) and a mixture of differentiation patterns based on the close proximity of the sebaceous gland with the pilosebaceous unit (hair, sebaceous, and apocrine sweat glands). Lesions can either be solitary or multiple, and when multiple may be associated with systemic conditions (e.g., Muir-Torre syndrome – internal malignancy with multiple sebaceous adenomas or sebaceous neoplasms).
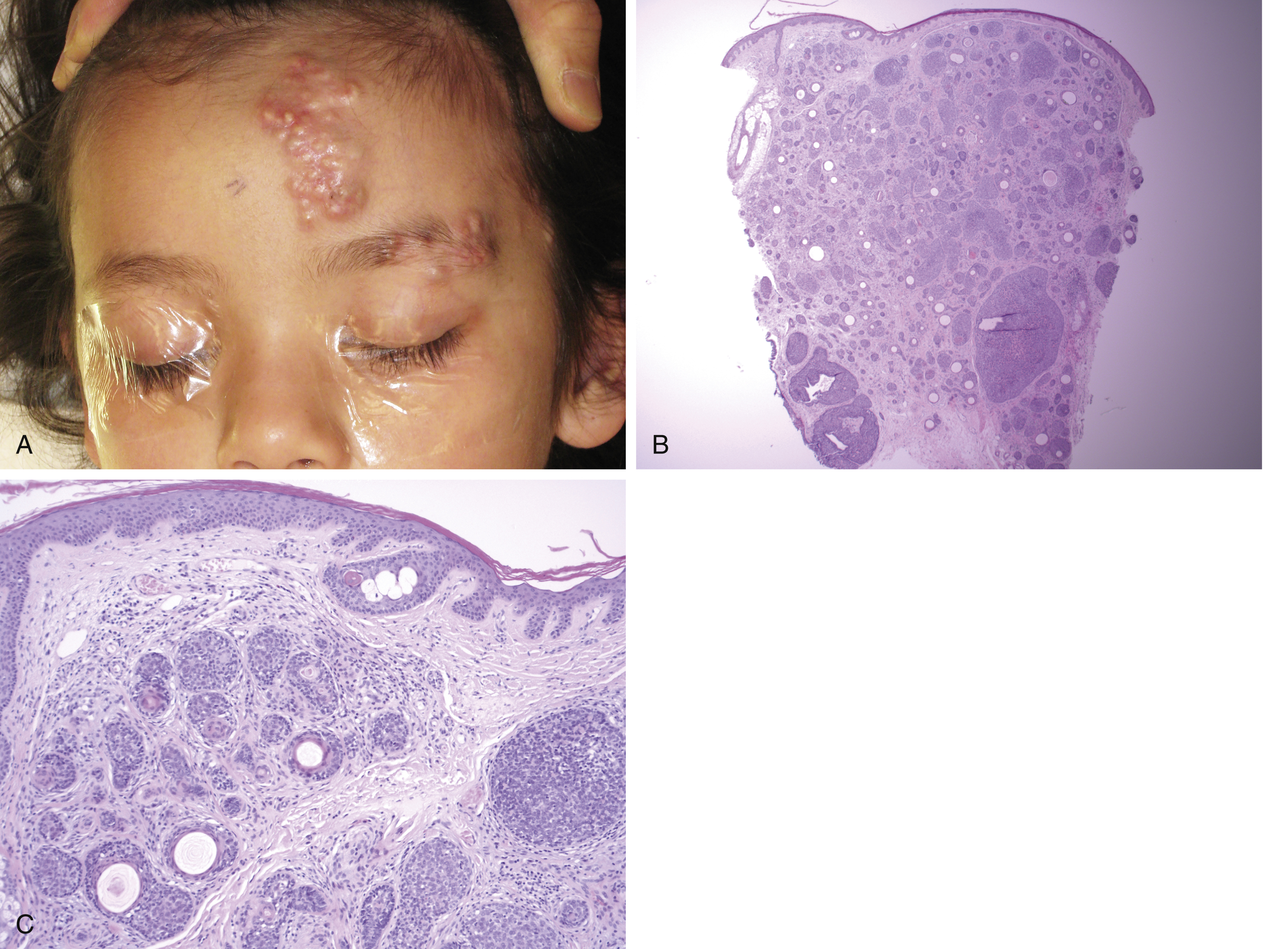
Nevus Sebaceous of Jadassohn
A well-circumscribed benign congenital hamartomatous lesion presenting as a yellow to light brown velvety or papular plaque on the scalp and face of children or young adults. It was first described by Josef Jadassohn, a dermatologist, in 1895. Some lesions have a PTCH gene mutation, but most are considered to have a mosaic genetic abnormality. In addition to esthetic considerations, nevus sebaceous is important because it carries a risk of transformation to other tumors (approximately 24%) and can be associated with neurological phenomena as part of sebaceous nevus syndrome. Lesions may be present at birth, but typically get larger before or around puberty and malignant transformation typically does not occur in patients 10 years or younger. For these reasons, excision is considered optimal just prior to puberty ( Fig. 10.3 ). Nevus sebaceous is relatively unique among the epidermal nevi because it often contains all skin components including epidermis, sebaceous, and apocrine glands, connective tissue and primitive hair follicles. Therefore, it is sometimes called an organoid nevus and can transform into numerous tumors both non-malignant (e.g., syringocystadenoma papilliferum, trichoblastoma or tricholemmoma) or malignant (8%–30% lifetime risk, BCC or other malignant tumors). Recent studies suggest that benign transformation is slightly more common than malignant transformation but the rates of these changes vary across studies. If a focal area of change develops within a sebaceous nevus, this should be biopsied to exclude malignant transformation and patients and their family should be advised to monitor the lesions for such changes. Rarely, patients with very large lesions can experience neurological disorders such as epilepsy. When these neurological disorders are more marked, including a combination of seizures, developmental delay, cranial nerve palsies, and/or hemiparesis and structural abnormalities of the brain, the constellation is referred to as nevus sebaceous syndrome. Nevus sebaceous is well circumscribed and therefore amenable to excision with a minimal margin and most practitioners would advise removal by teenage years or early adult life.
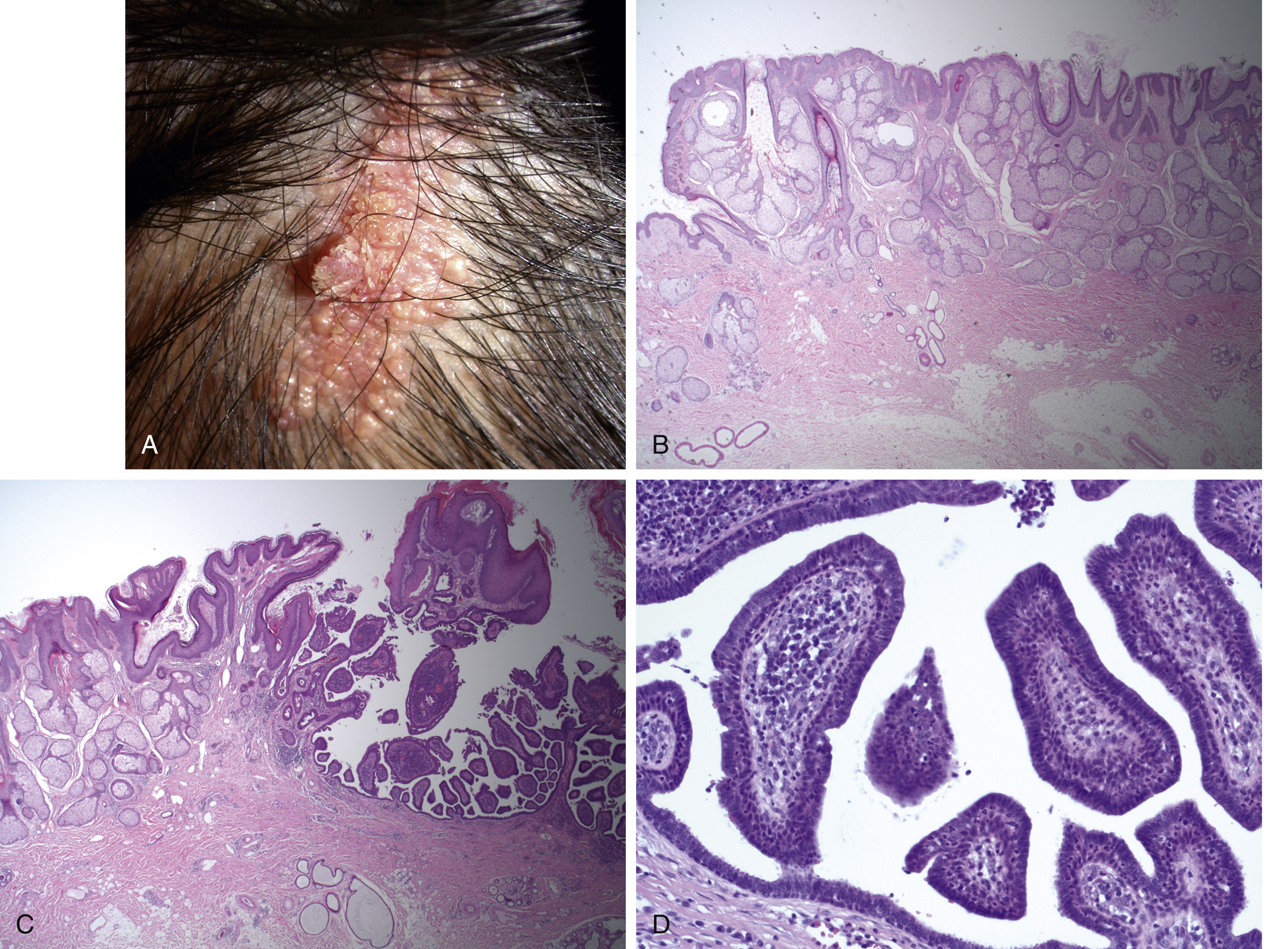
Benign Lesions Associated with Apocrine Glands
Hidradenoma Papilliferum
A benign cutaneous tumor derived from apocrine tissue that most commonly presents in the vulval region of middle-aged women, but can appear at extravulval sites in both sexes. Lesions appear as round, domed nodules that may ulcerate. On histology, they are identical to intraductal papillomas of the breast and therefore are considered to be ectopic breast tissue. They have a complex papillary structure showing an inner layer of PAS-positive columnar/cuboidal epithelium, a basal layer of myoepithelial cells that are S-100-positive, and a fine fibrovascular stroma.
Poroma
Benign adnexal neoplasms of epithelial cells that display ductal (usually distal) differentiation. While often described as “eccrine poromas,” the majority are thought to be apocrine in origin. They present as solitary (<2 cm) skin-colored papules or nodules that may be mistaken for other lesions or develop within nevus sebaceous. They are typically asymptomatic, but can cause pain on ulceration or on the sole of the foot. Simple surgical excision is the treatment of choice because it is usually curative and provides suitable specimens for histopathology.
Benign Lesions Associated with Sweat Ducts
Syringoma
A benign adnexal tumor that typically presents as single or multiple small (<3 mm) skin or yellow colored dermal papules usually around the eyelids, penis or vulva. They affect 1% or less of the adult population and are usually the result of benign growth of eccrine sweat gland elements or eccrine differentiation of pluripotent stem cells. Four variants have been recognized : (1) localized; (2) Down syndrome-associated; (3) generalized/multiple (including eruptive syringomas); and (4) familial variant.
On histology, they are a superficial dermal lesion characterized by abundant small ducts with a double-cuboidal epithelial lining and a sclerotic surrounding stroma. A PAS-positive secretion is present within the ductal lumen and the classic comma-shaped appearance of ducts on this lesion represent ducts that have elongated tails of epithelial cells upon sectioning. There are multiple management options from simple excision through electrocautery, cryotherapy, laser therapy, topical agents, topical or systemic retinoids. Simple excision with minimal margin achieves a definitive histopathology diagnosis (to exclude BCC) and can produce minimal scarring. Scar burden increases with the number of lesions present and therefore there is no perfect treatment for large numbers of lesions.
Cylindroma
Benign adnexal tumors (apocrine or mixed) that present as single or multiple lesions in the head and neck. When single, they are typically sporadic, occurring from middle age onwards as slow-growing, rubbery nodules that may reach up to 5–6 cm in size. Mutations in the CYLD gene (16a12-q13) are the principal cause of multiple cylindromas and may indicate familial inheritance (Brooke–Spiegler syndrome, an autosomal dominant syndrome with variable penetrance). Cylindromas may have a similar origin to related tumors such as spiradenomas and trichoepitheliomas because mixed lesions have been reported. Definitive diagnosis is by biopsy. Histology demonstrates a dermal tumor with islands of basophilic cells demonstrating peripheral palisading, surrounding larger, more pale central cells. Lamina densa-like material (predominantly collagen IV) surrounds the islands and the nests to separate them from the dermal matrix and these often give the lesions a jigsaw-like pattern of polygonal or oval nest shapes. Spiradenomas are related lesions, but are distinct from cylindromas because they have lymphoid invasion. Management is typically through surgical excision, which is curative following complete excision.
Spiradenoma
These benign, solitary tumors that are thought to be of apocrine origin present on the upper, anterior half of the body as pink, red, purple or blue nodules up to 1 cm in diameter. They typically occur in 15–35-year-olds, although infantile cases (with superficial dermal nodules) have been reported. They can be episodically painful, and while most are sporadic, they can be associated with Brooke–Spiegler syndrome (with trichoepitheliomas, cylindromas, spiradenomas, and mixed lesions). Mutations in the CYLD gene on chromosome 9 have been associated with their development, but spiradenomas also have increased expression of p53 . Multiple, giant, linear, and grouped forms have all been described. Malignant transformation can occur, particularly in long-standing lesions. Surgical excision is usually curative, but when multiple, radiotherapy and hyperthermic limb perfusion chemotherapy have been used successfully to avoid widespread excision.
Benign Dermal Tumors
Dermatofibroma
Dermatofibroma (or superficial benign fibrous histiocytoma) is a common cutaneous nodule of the limbs that is typically asymptomatic, but has been reported to be the most common atypical lesion causing pain. Their etiology remains unknown, but it may be trauma. Their prominent mast cells may release TGF-beta and other fibrinogenic factors to promote the fibrotic reaction seen histologically. Syndecan 1 and fibroblast growth factor receptor 2(FGFR-2) have also been implicated in their formation. , Gene fusions have also been implicated in the formation of dermatofibroma, particularly the ALK gene (a receptor tyrosine kinase that has also been found in some malignancies such as anaplastic large cell lymphoma, neuroblastoma and non-small cell lung cancer. Lesions are usually solitary, but may be multiple. When numerous lesions are present (≥15) they may be associated with a systemic conditions, including immune suppression (e.g., HIV), autoimmune conditions (SLE, dermatomyositis, Graves disease, Hashimoto’s thyroiditis, myasthenia gravis), malignancies (leukemia, myelodysplastic syndrome, cutaneous T-cell lymphoma, multiple myeloma), atopic dermatitis or Down syndrome. Dermatofibromas can be PET-avid and may have a similar appearance to many other tumors. Dermoscopy can be useful to display an overlying peripheral pigment network with a central white area. Ultrasound may show a solid hypoechoic nodule. A biopsy is warranted if there is any diagnostic uncertainty. Surgical removal is indicated if lesions are symptomatic, esthetically unacceptable or when diagnostic uncertainty remains. Excision of the tumor with minimal overlying skin is usually effective in preventing recurrence, but aggressive subtypes (aneurysmal, atypical, cellular, deep/subcutaneous) have a local recurrence rate of up to 20%. Rare cases of metastasis have been described with these variants.
Unusual Malignancies of Skin
The malignant tumors described in this section are uncommon at best and hence there is a paucity of high-level evidence to guide treatment. Accurate histopathology evaluation is vital and given the complexity and the rarity of these tumors, referral for expert review may be considered. MMS has been reported for many of these tumors, particularly in sites where obtaining a wide margin may be problematic. In general, lesions successfully treated by MMS tend to be smaller and although results appear to be as good as standard wide surgical excision, the number of cases and/or length of follow-up are limited in most reported series. In cases where the completeness of excision is uncertain, DRAPE (delayed reconstruction after pathology evaluation) should be considered.
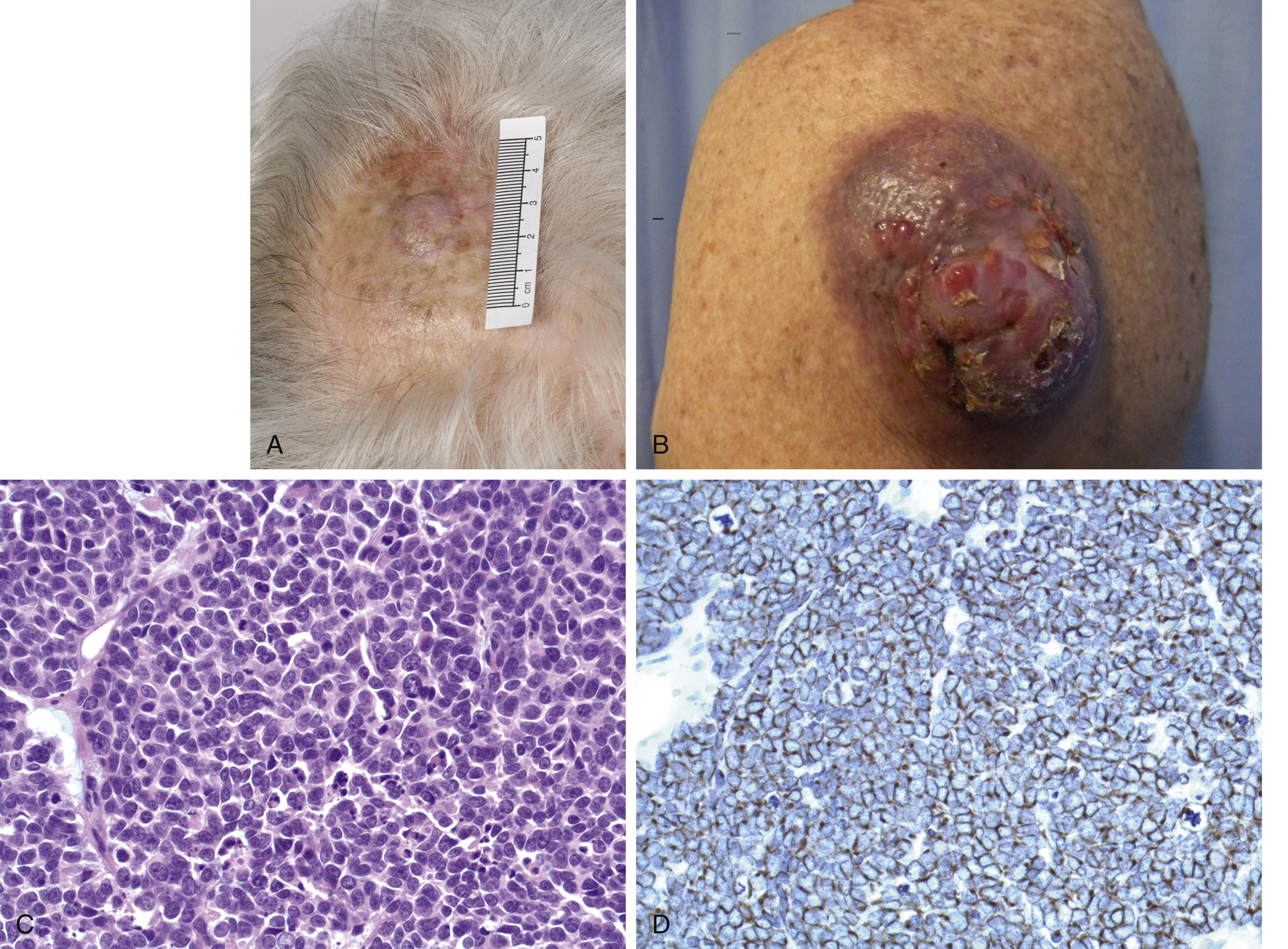
Merkel Cell Carcinoma
Merkel cell carcinoma (MCC) is an uncommon aggressive cutaneous malignancy that is increasing in frequency. The cell of origin is unknown but is unlikely to be the Merkel cell, a mechanoreceptor found in skin. The mnemonic AEIOU has been proposed to summarize the most common clinical characteristics (asymptomatic, expanding rapidly, immune suppression, older than 50 years and UV-exposed site on fair skin). Correspondingly, the lesion affects the sun-exposed areas of elderly males, is related to chronic UV exposure and immunosuppressed patients are over-represented ( Fig. 10.4 ). Over 80% of cases are associated with Merkel cell polyomavirus (MCV or MCPyV), a double-stranded DNA virus that is classified as a class 2A (probably carcinogenic) human oncovirus by the International Agency for Research on Cancer. MCV is almost ubiquitous in the community after infection early in life. In some populations, it may be in as many as 97% of all MCCs. It inserts itself into the recipient cell genome without causing cancer and without the ability to replicate, therefore patients are not infectious with MCV when they develop MCC. The inserted viral genome requires a subsequent mutation to form a spliced variant capable for forming multiple different proteins (including large and small T antigens). These oncoproteins target tumor suppressor genes such as the retinoblastoma protein and thereby promote carcinogenesis. In studies from North America and Europe the incidence of Merkel cell polyoma virus-associated tumors is considerably higher than seen in Australia, where UV exposure may be more important.