Introduction
Acute, severe, exfoliative, and necrotizing diseases of skin and underlying structures may cause significant morbidity and mortality in the afflicted patient. The problems associated with these diseases, such as wound infection, sepsis, inadequate nutrition, and pain, are similar to those seen in patients with major burns. Thus burn centers, with their multidisciplinary teams, have been advocated to provide the treatment and management for this unique, critically ill patient population. This chapter describes the pathophysiologic processes of severe exfoliative skin disorders, their diagnosis, and the specialized treatment offered by burn centers.
Severe exfoliative disorders
This classification of exfoliative diseases of the skin and mucous membranes historically consisted of three specific maladies, distinguished by the amount of skin involvement: erythema multiforme major (EM), Stevens-Johnson syndrome (SJS), and toxic epidermal necrolysis (TEN). For the terms of this chapter, we are maintaining that approach. However, some recent classifications list EM as its own distinct disease entity separate from SJS and TEN and most commonly associated with the herpes simplex. This new designation does not affect the classifications of SJS and TEN: each is still determined by the extent of total body surface area (TBSA) affected by the disease process. SJS is considered to affect less than 10% TBSA, whereas TEN covers more than 30% TSBA, leaving a zone of overlap between 10% and 30% TBSA, which is referred to as SJS/TEN. , The most common characteristics of these disease entities are defined in Table 36.1 . ,
Table 36.1
Characteristics of Erythema Multiforme, Stevens-Johnson Syndrome, and Toxic Epidermal Necrolysis
| Erythema Multiforme | Stevens-Johnson Syndrome | Toxic Epidermal Necrolysis | |
|---|---|---|---|
| Prodrome | Absent | High fever, malaise | High fever, malaise |
|
Acute phase
|
4–8 days | 4–8 days | Sudden onset, 1–2 days |
| Sensation of skin burning or tenderness | Sensation of skin burning or tenderness | ||
| Skin lesions | Symmetric, primarily located on the extremities, some target lesions without blisters | Variable distribution, individual vesicles on an erythematous base <10% TBSA | Diffuse generalized epidermal detachment, absence of target lesions, large confluent plaques >30% TBSA |
| Nikolsky positive | |||
| Nikolsky positive | |||
| Mucosal involvement | Limited to one surface, usually oral | Severe, two or more surfaces involved | Severe, two or more surfaces involved |
| Histopathology | Dermoepidermal separation, mononuclear perivascular cell infiltrate, small areas of epidermal detachment associated with target lesions | Dermoepidermal separation, more intense dermal infiltrate, areas of epidermal detachment | Epidermal necrosis, dermoepidermal separation, minimal dermal inflammatory infiltrate, large areas of epidermal detachment |
| Recovery | 1–4 weeks | 1–6 weeks | 1–6 weeks |
| Mortality | 0% | 0%–38% | 25%–80% |
TBSA, Total body surface area.
Toxic epidermal necrolysis
Epidemiology
TEN represents the severe extreme of the spectrum of necrolytic disorders. A rare disease, the incidence of TEN in this country is estimated at 0.4 to 1.9 cases per million persons per year and that of SJS has been reported to be only slightly higher at 1 to 7 cases per million persons per year. This incidence is similar to 1.89 cases of TEN per million persons per year reported for Europe in 1996, but higher than reported for Asia. , The overall rarity of this disease process has been, and continues to be, a barrier to research. However, over the past several decades, the concentration of physician experience with TEN into a limited set of regional burn centers has facilitated an increasing quantity and quality of active research.
These exfoliative disorders occur in all age groups; however, the incidence is increased in the elderly (fifth and seventh decades of life) and females. , In addition, TEN has been linked to certain infectious disease processes. The annual incidence of TEN in the human immunodeficiency virus (HIV)-infected population is 1000-fold higher than in the general public. Whether this increase is due to their immunocompromised state or to the increased prescription of high-risk drugs, particularly sulfonamides, is debated. , However, cases with no drug history or preceding illness have been reported. An additional infectious disease process associated with SJS/TEN is Mycoplasma pneumonia. Finally, idiopathic cases not related to drugs account for 3% to 4% of TEN. ,
Prognosis, morbidity, mortality
On the surface, these exfoliative disorders may mimic the symptoms of a partial-thickness thermal injury, specifically in relation to the involvement of the skin. However, these diseases also affect all epithelial surfaces, thus increasing the risk and incidence of infections, other complications, and death. Patients suffering from particularly complicated cases of SJS may benefit from the expertise of a burn center, although these patients are generally referred on an as-needed basis. In contrast, those diagnosed with TEN carry a specific set of severe and complicated medical needs that are clearly best addressed in the context of a specialized burn center.
Mortality of TEN ranges from 25% to 80%, with morbidity being reported as high as 65%. However, reports are variable and usually based only on small patient populations. , , Death may occur early in the course of the disease, with sepsis being the most frequent cause. Pseudomonas aeruginosa and Staphylococcus aureus are the predominant organisms involved. Pulmonary embolism and gastrointestinal hemorrhage are other causes of death.
Mortality is increased significantly in those patients at the extremes of age and in relation to the percentage of denuded skin and serum urea nitrogen levels. , , Bastuji-Garin et al. in 2000 created the Score of Toxic Epidermal Necrolysis (SCORTEN), a scoring system to predict mortality in the adult population presenting with TEN. The scoring system uses seven independent risk factors to predict mortality by allotting 1 point for each variable :
-
a.
Age older than 40
-
b.
Heart rate greater than 120 beats per minute
-
c.
Comorbid malignancy
-
d.
Epidermal detachment of greater than 10% of body surface area (BSA) on day 1
-
e.
Blood urea nitrogen greater than 28 mg/dL
-
f.
Glucose greater than 252 mg/dL
-
g.
Bicarbonate less than 20 mEq/L
The scoring system should be performed on day 1 and day 3 postadmission to maximize its predictive value. Mortality from TEN increases from 3.2% for a score of 0 or 1 to 90% for a score greater than 5 ( Table 36.2 ).
Table 36.2
SCORTEN Scores and Mortality
| SCORTEN (Sum of Scores) | Predicted Mortality |
|---|---|
| 0–1 | 3.2% |
| 2 | 12.1% |
| 3 | 35.8% |
| 4 | 58.3% |
| >5 | 90% |
Although originally developed for adults, the scoring system has been validated in the pediatric population, but overall it has been challenged for its lack of incorporating no more than one morbidity (malignancy) in its calculation. , Although other investigators have developed formulas based on logistic regression analysis (i.e., ABCD 10), the SCORTEN system is the most accurate and widely used.
SJS is associated with a mortality rate of 0% to 38%. , EM rarely causes death.
Etiology
Keratinocyte apoptosis and secondary epidermal necrosis represent the pathopneumonic cellular process of TEN. The origins of the cellular process remain an active area of research, with an intricate meshwork of overlapping risk factors and processes starting to emerge as the picture sharpens. What has become clear is that the TEN disease process results from a complicated interaction of multiple processes and risk factors: genetic predisposition, environmental triggers, immunologic reaction, inflammatory mediators, and cellular apoptotic machinery.
Triggers and risk factors
TEN appears to be driven by immunologic reactions to foreign antigens, often referred to as triggers. Medications are by far the most commonly identified trigger, implicated in 77% to 94% cases of TEN. Antimicrobials, anticonvulsants, analgesics, and nonsteroidal antiinflammatory agents of the oxicam type have been implicated. , Naturally, the particular profile of TEN instigators will vary from population to population depending on the epidemiology of medication exposures in any given population.
Attempts to identify drugs suspected of having caused exfoliative necrolysis by skin test and laboratory tests seldom have been successful. Although some assays are trialed in research settings, there are currently no fully vetted, reliable methods available for identifying the inciting trigger in a patient with TEN. Historically, the medication-specific trigger for any given case of TEN was ultimately a matter of speculation. However, Sassolas et al. in 2010 developed an algorithm of drug causality for epidermal necrolysis termed ALDEN. The algorithm assigns a score of 1 to 10 for each drug based on six parameters. The score is then categorized as very probable (>6), probable (4–5), possible (2–3), unlikely (0–1), and very unlikely (<0) ( Table 36.3 ). The results of this algorithm were compared with a case-controlled analysis of the European Study of Severe Cutaneous Adverse Reactions (EuroSCAR) and found to have good accordance. , The use of ALDEN in the clinical setting may greatly improve the ability for clinicians and researchers to link medication-specific triggers and TEN.
Table 36.3
Algorithm of Drug Causality for Epidermal Necrolysis (ALDEN)
| Criterion | Values | Rules to Apply | |
|---|---|---|---|
|
Delay from initial drug component intake to onset of reaction (index day)
|
Suggestive +3 | From 5 to 28 days | –3 to 3 |
| Compatible +2 | From 29 to 56 days | ||
| Likely +1 | From 1 to 4 days | ||
| Unlikely-1 | >56 days | ||
| Excluded −3 | Drug started on or after the index day | ||
|
|||
|
Drug present in the body on index day
|
Define 0 | Drug continued up to index day or stopped at a time point less than five times the elimination half-life before the index day | –3 to 0 |
| Doubtful-1 | Drug stopped at a time point before the index day by more than five times the elimination half-life but liver or kidney function alterations or suspected drug interactions are present | ||
| Excluded-3 | Drug stopped at a time point before the index day by more than five times the elimination half-life , without liver or kidney function alterations or suspected drug interactions | ||
|
Prechallenge/rechallenge
|
Positive specific for disease and drug: 4 | SJS/TEN after use of same drug | –2 to 4 |
| Positive specific for disease and drug: 2 | SJS/TEN after use of similar drug or other reaction with same drug | ||
| Positive unspecific: 1 | Other reaction after use of similar drug | ||
| Not done/unknown: 0 | No known previous exposure to this drug | ||
| Negative-2 | Exposure to this drug without any reaction (before or after reaction) | ||
|
Dechallenge
|
Neutral 0 | Drug stopped (or unknown) | –2 or 0 |
| Negative-2 | Drug continued without harm | ||
|
Type of drug (notoriety)
|
Strongly associated 3 | Drug of the “high-risk” list according to previous case-control studies | –1 to 3 |
| Associated 2 | Drug with definite but lower risk according to previous case-control studies | ||
| Suspected 1 | Several previous reports, ambiguous epidemiology results (drug “under surveillance”) | ||
| Unknown 0 | All other drugs including newly released ones | ||
| Not suspected-1 | No evidence of association from previous epidemiology study with sufficient number of exposed controls | ||
| Intermediate score = total of all previous criteria | –11 to 10 | ||
|
Other cause
|
Possible-1 | Rank all drugs from highest to lowest intermediate score | −1 |
| If at least one has an intermediate score >3, subtract 1 point from the score of each of the other drugs taken by the patient (another cause is more likely) | |||
| Final score | –12 to 10 |
<0, Very unlikely; 0–1, unlikely; 2–3, possible; 4–5, probable; ≥6, very probable.
ATC, Anatomic therapeutic chemical; SJS, Stevens-Johnson syndrome; TEN, toxic epidermal necrolysis.
Although advances have been made in correlating medications as the causative agent of TEN, the role of nonmedication triggers in the etiology of TEN remains murky. Upper respiratory tract infections, pharyngitis, otitis media, or viral illness are frequently reported as preceding or coinciding with the development of TEN in some patients. , Mycoplasma pneumoniae and herpes viruses (cytomegalovirus, Epstein-Barr virus, herpes simplex, and varicella zoster) have been implicated in the cause of EM and SJS, but not TEN. , , Quantifying the association between TEN and antecedent viral syndromes is complicated by the rarity of TEN and the similarities between prodromal symptoms and other more common disorders. This leads to patients presenting with relatively prominent prodromal symptoms who are typically misdiagnosed as having a simple viral syndrome. Because of the delay between early prodromal symptoms and the more specific TEN rash, it is often impossible to determine in retrospect whether the pertinent symptoms were actually prodromal or if the patient had an antecedent viral infection. Furthermore, these prodromal symptoms are often treated with medications before the TEN diagnosis is considered. As such, medications used to treat prodromal symptoms are frequently misinterpreted as TEN triggers.
Genetics
Genetics clearly plays an important role in the pathophysiology of TEN, with multiple alleles identified as potent risk factors. Interestingly, the genetic risk factors identified thus far all appear to be trigger specific. That is, a particular allele may place a person at risk for developing TEN in response to one drug, but not increase that same person’s risk for developing TEN in response to a different medication. The majority of those alleles identified thus far appear to increase risk through two separate mechanisms: drug-antigen metabolism and antigen presentation. As early as 1986, Shear et al. identified a pattern of “slow” sulfonamide metabolism in patients with a history of severe cutaneous sulfonamide reactions. Insights and technologies developed through the maturation of the field have allowed pharmacogeneticists to trace such associations with polymorphisms in genes encoding for components of the cytochrome P450 machinery. Investigators studying TEN patients’ genotypes have assembled a sizable catalog of cytochrome P450C variants that convey an increased risk for developing TEN, with each polymorphism associated with a specific trigger agent. The largest family of genes with a documented association with TEN include polymorphisms at a number of human leukocyte antigen (HLA) loci that have been associated with drug-specific risks for TEN. These polymorphisms presumably alter the morphology of the HLA molecules on antigen-presenting cells, making them more or less inclined to “recognize” a particular antigen. The “antigen” may be the medication molecule, a drug metabolite, a by-product of drug metabolism, or a hapten created by the binding of the drug, metabolite, or by-product to another peptide.
The clinical application of these genetic markers is complicated by the fact that their predictive value varies widely when applied to populations of different ethnic makeups. An example of this strong association between HLA, drug sensitivity, and ethnic background was discovered by Chung et al. They demonstrated a strong association between HLA-B*1502, SJS, and carbamazepine in Han Chinese. This unique relationship was later observed in a Thai population but was absent in the Japanese and European populations. In fact, RegiSCAR, a large European study, suggested that HLA-B*1502 is not a marker for carbamazepine, sulfamethoxazole, lamotrigine, or NSAID oxicam-type–induced SJS or TEN.
Although the HLA-B*1502 and carbamazepine association demonstrated significant ethnic variance, this is not the observation for all HLA-medication interactions. A second strong relationship among HLA, drug sensitivity, and SJS/TEN was observed for allopurinol and HLA-B*5801. Although the strength of the relationship continued to vary between ethnicities, the correlation persisted in Han Chinese, Japanese, Thai, and Europeans, unlike for HLA-B*1502 and carbamazepine.
In summary, for many of these markers, prevalence patterns make the marker too rare to function as a screening tool outside the context of specific ethnicities. Beyond issues of prevalence, some markers are associated with a TEN reaction in one population, but not in another: a phenomenon that likely traces to interactions between the “maker” allele and other genetic variables.
Immunopathology
Multiple lines of evidence point to T cells as critical effectors of the TEN process. T cells are the predominant cell type found in the blister fluid and exudate of patients with acute TEN.
Suppression or cytotoxic T-cell infiltrates are observed in the epidermis in TEN. , The observation of blebbing of the keratinocyte plasma membrane in TEN is considered a reliable morphologic finding of cytotoxic T-lymphocyte cytolysis. Serum and exudate levels of markers of T-cell activation have been shown to correlate with disease activity and resolution.
TEN is perhaps best understood as an immunologically mediated burn. For the most part, TEN resembles a classic type IV (delayed) hypersensitivity disorder. The delay between exposure and reaction, the critical role of T cells, and the accelerated reaction reported in cases of reexposure to an initial trigger all favor this characterization. , Although some have pointed to immunofluorescence microscopy findings of IgM and C3 deposited along the dermoepidermal junction and dermal vessels in cases of postherpetic SJS and EM as evidence of an associated type II hypersensitivity reaction, others attribute this to simple nonspecific exudation. , The exact antigen that activates the T-cell receptor varies depending on the specific trigger agent: the recognized moiety could be a molecule within the medication, a by-product of agent metabolism, or a complex formed between an endogenous peptide and either of the preceding. Keratinocyte apoptosis is central to the pathogenesis of TEN. This event is thought to be mediated by ligand/receptor interaction of the tumor necrosis factor (TNF) superfamily (as TNF-α/TNF receptor or FasL/Fas interaction). , Through a series of experiments, Viard et al. observed, in vitro, that TEN patients expressed lytically active Fas ligand and that the action of this ligand could be blocked by both a monoclonal antibody and human immunoglobins. In SJS, keratinocyte DNA fragmentation has been found in about 90% of cases associated with dermal perforin-positive lymphocytes. ,
Clinical presentation
A prodromal phase of TEN is frequently identifiable in retrospect and usually characterized by some combination of low-grade fever, malaise, cough, conjunctivitis, and dysuria. These symptoms typically precede any cutaneous manifestation by 1 to 21 days but usually last for 2 to 3 days. , This prodrome precedes the development of a frank rash, although patches of tender erythema and inflamed mucosal membranes are sometimes present. Skin involvement usually begins with subtle patches of tender erythema and localized morbilliform eruptions or discrete erythematous or purpuric macules. Later vesicles and large bullae emerge from areas of erythema, either en masse or via coalescence of initial morbilliform eruptions. On light digital pressure, the epidermis desquamates in sheets: Nikolsky’s sign is positive ( Fig. 36.1 ). The TEN rash is extremely painful, even when bullae are still intact. Generally, a lag period of 1 to 3 weeks is observed from initiation of drug until skin eruption, but this may be shorter, particularly in cases of reexposure in a previously sensitized individual. , ,
(A–C) Nikolsky’s sign. Epidermal separation induced by gentle pressure on the skin surface.
Mucosal involvement is extremely common in TEN, with two or more areas typically involved. These mucosal lesions are often most problematic in that they can cause significant immediate and long-term complications and typically persist (symptomatically) longer than cutaneous lesions. , , Site involvement usually follows this order of frequency: oropharynx (93%), ocular (78%), genitalia (63%), and occasionally the anal mucosa.
Mucosal involvement precedes skin lesions by 1 to 3 days in one-third of cases. , As such, any case presenting with skin involvement with no mucosal involvement should raise the suspicion for an alternative diagnosis. However, it should be noted that detection of mucosal involvement often requires a significant index of suspicion: the fulminant skin findings can frequently distract from more subtle mucosal findings, such as enteral mucosal involvement and bronchial involvement, which are often more easily inferred from symptoms rather than direct visualization.
Diagnosis and prognostic evaluation
Histopathology
An early skin biopsy is essential for diagnosis. Skin manifestations vary from patient to patient and with the age of the lesion ( Fig. 36.2 ). Advancing edges of the target lesions show scattered necrotic keratinocytes in the epidermis and only mild dermal inflammation. In older lesions and central zones of target lesions, the dusky appearance corresponds to areas of extensive keratinocyte necrosis, often with the formation of subepidermal bullae and dermoepidermal separation. The surrounding erythematous zone shows papillary dermal edema, vascular dilation with endothelial cell swelling, and perivascular mononuclear cell infiltrate. Extravasated erythrocytes may be seen in the surrounding papillary dermis. The reticular dermis is normal. ,
Toxic epidermal necrolysisis characterized by massive sloughing of the epidermal tissue.
Epidermal and dermoepidermal suppressor or cytotoxic T lymphocytes, in addition to dermal infiltrates of helper T lymphocytes, have been demonstrated. , , Hertl has confirmed that these epidermal cells are cytotoxic T cells. Langerhans cells appear to be reduced in the epidermis, although numerous dermal macrophages are observed. A more intense dermal cell infiltrate is present in SJS, especially in postherpetic cases. Dendritic lymphoid cells are observed, opposed to damaged dermal macrophages and necrotic keratinocytes. Furthermore, at the point where the cytoplasmic processes contact the keratinocyte, the plasma membrane of the keratinocyte is absent. Aberrant expression of HLA-DR on keratinocytes has been observed, a phenomenon that has been present in many other inflammatory skin disorders. ,
Complications
TEN is frequently associated with serious complications. In many cases, the skin reepithelializes from the dermal elements without significant scarring and with long-term effects typically limited to discoloration. Scarring may be more prominent—and accompanied by contractures—if the disease progresses due to secondary infection or peripheral vasoconstriction from shock or vasopressor use. Nail plates are frequently lost, and nail regrowth may be abnormal or absent.
Complications may also affect mucosal membranes throughout the body. One of the most severe long-term complications is ocular sequelae, which occurs in half of the survivors. Pseudomembranous or membranous conjunctivitis resulting from coalesced fibrin and necrotic debris can lead to ocular opacification, secondary infection, and blindness ( Fig. 36.3 ). , Conjunctival scarring may also result in lacrimal duct destruction, leading to reduced tear production and keratoconjunctivitis sicca, a Sjögren-like syndrome. Finally, scar changes can lead to distortion of eyelid anatomy, which can result in ectropion, entropion, trichiasis, and symblepharon. ,
Ocular involvement in toxic epidermal necrolysis is common and can lead to blindness. Early and aggressive ocular care must be initiated to prevent pseudomembranes. ( Arrows demonstrate membranous conjunctivitis.)
Other systems that may be impacted include:
-
■
Oropharyngeal : This is common and often results in pain on chewing, severe dysphagia, and odynophagia ( Fig. 36.4 ). The mucositis is associated with an increase in secretions and sloughing mucosa, which can present an airway concern. Naturally, oropharyngeal involvement can interfere with oral intake, requiring direct enteral access for an alternate route of feeding. Buccal gingiva epithelial fusing can occur, thus demonstrating the importance of good oral hygiene.
Fig. 36.4 Toxic epidermal necrolysis patient demonstrating significant oropharyngeal involvement.
-
■
Respiratory : Respiratory tract involvement occurs and is associated with increased mortality. , These complications include diffuse erythema to extensive confluent tracheal and bronchial erosion covered by fibrinous exudate. Epiglottal swelling necessitating intubation has also been reported. However, bronchopneumonia has been found to be the most frequent complication, occurring in 50% of patients. , ,
-
■
Gastrointestinal : The onset of intestinal symptoms generally occurs concurrently with the cutaneous lesions. Epidermal and epithelial sloughing may extend into the gastrointestinal mucosa and may induce esophagitis with frequent subsequent stricture formation. Gastrointestinal erosions macroscopically resemble ulcerative or pseudomembranous colitis, and massive hemorrhage requiring resection has been reported.
-
■
Urologic : Male urethral involvement is fairly common, with visible involvement at the meatus. Long-term sequelae include urethral stricture and phimosis.
-
■
Gynecologic : Vulvar involvement appears to be quite common in female patients, with reported incidences increasing over the past few decades as increasing awareness has resulted in improved detection and more frequent practice of routine screening exams. Mucosal erosions are clearly quite painful, and involvement of associated glandular structures can result in obstruction and dysfunction. Long-term sequelae can be particularly troublesome. Vaginal wall synechiae and clitoral hood adhesions can result in significant dyspareunia and sexual dysfunction. , Vaginal webbing and synechiae can result in dysfunctional menstruation with resultant infertility. Consultation with a gynecologist is recommended for the majority of these cases.
Systemic and other nonmucocutaneous complications
Although mucocutaneous erosions are the most common features of TEN/SJS, the disease may present with multisystem involvement. Renal manifestations like glomerulonephritis and acute tubular necrosis, as well as hepatitis and hepatocellular necrosis, have been described. , , Hypoalbuminemia, asymptomatic hyperamylasemia, increased erythrocyte sedimentation rate, leukocytosis, thrombocytopenia, and normochromic and normocytic anemia are not uncommon. , Leukopenia is a frequent and poor prognostic sign. , , This is due in part to depletion of the T helper/inducer lymphocyte population (CD4 + ). The white blood cell count generally returns to normal levels after 2 to 5 days. The cause of this immunosuppression is unclear.
Management
As previously stated, TEN is a life-threatening disease and is best managed in a burn intensive care unit where a multidisciplinary approach, including goal-directed fluid resuscitation and nutritional support, is used. , , ,
General management and resuscitation
Drugs suspected of having initiated the disease should be discontinued immediately. Administration of pain medication is of high priority, and antipyretic agents may be required. The use of broad-spectrum antibiotics should be carefully considered: neutropenia is the only complication in which “prophylactic” antibiotics are indicated. Otherwise, systemic antibiotics only should be used for documented infections or suspected sepsis.
Intravenous replacement of fluid losses through the exposed body surface is required. However, because patients do not develop the massive edema and fluid losses evident in burn patients, fluid resuscitation formulas commonly employed in the management of thermal injuries overestimate the actual need. , Lactated Ringer’s solution is given at a rate determined by close monitoring of the patient’s condition, resuscitation indexes, and urine output. Once wound coverage is accomplished, fluid requirements usually decrease.
Central line placement should be avoided if possible to reduce the risk of infection and sepsis. To further minimize this risk, lines should be placed in areas of uninvolved skin. Invasive devices are removed as soon as possible, and oral and nasogastric routes are used at earliest convenience. The environmental temperature should be raised to between 30°C and 32°C to reduce metabolic energy expenditure. Heat shields and infrared lamps are beneficial in patients’ rooms, bathrooms, and operating rooms.
Stress ulceration prophylaxis is advisable.
Immunomodulation therapy
Because the pathophysiology of TEN appears to be initially immunologic, it is logical to consider immunosuppressive therapy as an early treatment modality. The following sections will briefly review the literature with regard to the use of corticosteroids, cyclosporine A, intravenous immunoglobins, and thalidomide.
Corticosteroid therapy.
Corticosteroid treatment of TEN has produced much controversy. In relation to the delayed hypersensitivity reaction or antibody-dependent cytotoxicity theories of pathogenesis, corticosteroids would seem to be an appropriate form of medical therapy. However, the practice of administering continuous high-dose corticosteroid in an attempt to stop the progression of the disease is widely rejected. , , , , , Rational assessment of the benefit of corticosteroids is not possible because of the lack of randomized, controlled, prospective trials. Many authors feel that steroids enhance the risk of sepsis, increase protein catabolism, delay wound healing, cause severe gastrointestinal bleeding, prolong hospitalization, and increase mortality. , , , One study found no decrease in the progression of SJS with steroids, but instead found significant morbidity. In a prospective—although not randomized—study, increased survival (66%) was seen in matched patients who did not receive steroids compared with only 33% survival in those who did receive steroids. Pediatric SJS patients treated with steroids had a longer hospital stay and a complication rate of 74% compared with 28% in those without steroids. Another study demonstrated 80% mortality associated with steroid therapy, which was reduced to 20% when steroids were withheld. In several studies, patients with antecedent glucocorticoid therapy before the onset of TEN showed no significant survival benefit, and corticosteroid use itself has been linked to an increased risk for developing TEN. , , , Advocates of corticosteroid therapy suggest that improved results are possible when steroids are applied in a limited “pulse” dose early in the course to interrupt the active necrolytic process and limit complications. Kardaun et al. studied 12 patients over a 10-year period and suggested that short-term dexamethasone pulse therapy was safe and may contribute to a reduced mortality rate. This was followed by the largest study of this approach, the EuroSCAR, which did identify a trend but not a statistically significant improvement with the early pulse of systemic corticosteroids. Thus corticosteroid therapy remains controversial in this disease because of the absence of strong evidence of efficacy.
Cyclosporine A.
Cyclosporine A is an agent that has the properties of being both a powerful immunosuppressant and an antiapoptotic. The mechanism of action is inhibition of the synthesis of interleukin-2 by selective inhibition of calcineurin, thus arresting the proliferation of T helper cells. In the only case series, Arevalo et al. observed a significantly shorter time to disease arrest (24–36 h) and time to reepithelialization when compared with historical controls. This study was followed by a few small studies suggesting a potential benefit of cyclosporine A. In 2010, a phase II trial by Valleyrie-Allanore et al. found a treatment of 3 mg/kg per day of oral cyclosporine for 10 days followed by a tapering schema over the next month was not clinically significant. However, mortality appeared to be reduced when compared with predictive mortality. Although intriguing, the currently published studies do not have similar methodologies, varying with regard to the dosage administered, route of administration, and duration of therapy. Furthermore, cyclosporine A therapy has been associated with a septicemia rate of 55%. Therefore a well-designed prospective clinical trial is warranted before advocating the use of cyclosporine A in the treatment of TEN.
Intravenous immunoglobulin.
Intravenous immunoglobulin (IVIG) has been suggested as a means of interrupting the autoimmune process fueling TEN. Furthermore, some have proposed that pooled human immunoglobins may contain a Fas blocking antibody, which would directly disrupt the keratinocyte apoptosis trigger. Unfortunately, clinical data have been conflicting, creating difficulty in advocating IVIG treatment for TEN. To date, there have been 12 noncontrolled clinical studies examining the efficacy of IVIG in the treatment of TEN. Interestingly, the data suggest that IVIG dosages of greater than 2 mg/kg may be superior to less than 2 mg/kg. Huang et al. performed a meta-analysis on the efficacy of IVIG therapy in TEN patients. In adults, the high-dose IVIG group had a significantly lower mortality rate when compared with the low-dose IVIG group. However, the multivariate logistic regression model found the dosing of IVIG did not correlate with mortality when controlling for age, total BSA involvement, and delay in treatment. This finding was supported by the largest clinical study to date, EuroSCAR, which failed to demonstrate efficacy of IVIG in the treatment of TEN.
Despite these findings, some continue to advocate for the use of high-dose IVIG (3 mg/kg total dose given over 3–4 days) in the treatment of TEN based on the low complication risk and lack of alternative therapies. As in the case with cyclosporine A, a well-designed controlled multicenter clinical trial is warranted before advocating the use of human immunoglobins routinely in the treatment of TEN.
TNF-α inhibitors, thalidomide.
The primary mechanism in the pathogenesis of TEN is keratinocyte apoptosis. Accordingly, TNF-α has been implicated in the pathogenesis of TEN. Thalidomide, a potent inhibitor of TNF-α, would appear to be a logical therapeutic agent in the treatment of TEN. Unfortunately, Wolkenstein et al. had to prematurely terminate a randomized clinical trial of thalidomide versus placebo in the treatment of TEN because of excess mortality in the treatment group. Ten of 12 patients expired in the thalidomide group compared with 3 of 10 in the control group. The authors theorized that thalidomide may have paradoxically increased the production of TNF in the treatment group, a previously reported phenomenon of thalidomide administration. Therefore thalidomide as a treatment for TEN should not be initiated owing to the detrimental effects, but this does demonstrate the usefulness of randomized, double-blinded, placebo-controlled clinical trials. Despite the failure of thalidomide, investigators are still exploring the use of TNF-α antagonists and inhibitors (infliximab, etanercept, etc.), in the treatment of TEN. , Unfortunately, these new therapies have only been reported in case reports and thus cannot be supported for routine use in this patient population.
Until these treatment modalities have proved their efficacy in controlled trials, the gold standard of treatment for TEN patients consists of a multidisciplinary approach as used in severe burns, focusing on wound care, infection control, and prevention of complications.
Future pharmacological interventions for SJS/TENS.
Unfortunately to date, there have been no double blinded randomized controlled trials evaluating which pharmacological agent or agents are the most effective at reducing either morbidity and/or mortality in this unique patient population.
While the standard of care has centered around prompt termination of the offending agent and aggressive intensive care support, several investigators have continued to explore a more effective treatment regime for the Stevens-Johnson Syndrome/TENs patient. Based on our current understanding of the pathophysiology behind SJS/TENs, most of these studies have investigated the administration of immunosuppressants alone or in combination, such as cyclosporine and etanercept. The concept behind the administration of these agents appears to be supported by both in vitro and in vivo data demonstrating the reduction of key factors (perforins, granzyme B, granulysin) thought to drive keratinocyte apoptosis. , In the study by Wang et al., the investigators enrolled 96 patients in an unblinded randomized control trail comparing etanercept to corticosteroids. The results suggested an improved clinical course with fewer complications for the etanercept treatment group compared to the corticosteroid group. While unblinded, the investigation suggests an effective treatment option with few reported complications for SJS/TENS patients. More recently, investigators continue to report from small studies the beneficial attributes of etanercept to be improved skin re-epithelization, reduced hospital stay, and reduced side effect profiles compared to corticosteroids. ,
Fortunately, the first multicenter double blinded randomized controlled trail has begun enrolling patients to compare two immunosuppressive arms of therapy (etanercept, cyclosporine) to standard supportive care. This well-designed clinical trial will hopefully provide much needed guidance to the best treatment regime for SJS/TENS patients.
Finally, the increasing utilization of proteomics and genomics strategies may lead to even greater advances in the treatment of SJS/TEN. Nordmann et al. recently published in Nature, the utilization of a Janus Kinase inhibitor (JAKi) for the treatment of TEN. The investigators used deep visual proteomics that combine imaging, artificial intelligence-based cell segmentation, laser dissection of individual cells and mass spectrometry-based proteomics to compare self-resolving maculopapular rashes and TEN.(9) They found high JAK-STAT signaling in the skin and immune cells in patients with TEN and the involvement of JAK-STAT signaling in pathogenesis of TEN. While in vivo and animal tests were promising, off label administration of JAKi in seven TEN patients demonstrated positive results and complete resolution of the disease in a patient refractory to corticosteroid therapy. While the results are very exciting and promising, larger clinical studies are necessary to examine the true benefits of this new therapy. Hopefully, these newer agents will allow practitioners to rapidly terminate the pathological process of SJS/TEN and dramatically reduce the morbidity and mortality of this unique disease process.
Surgical approach.
Debridement of necrotic epidermis and coverage of the large wound surface with biologic or synthetic dressings have been advocated by several authors. , , Sloughed epidermis should be removed to reduce bacterial growth and the risk for infection. The exposed and tender dermis should be covered. Debridement is best undertaken under general anesthesia as soon as diagnosis by histology is established. Blood loss associated with debridement is minimal, so overresuscitation must be avoided.
Synthetic dressings, such as Biobrane, Suprathel, and biologic dressings, such as homograft (cadaver allograft) and porcine xenograft skin, greatly reduce the pain, decrease fluid loss, and promote healing. Biobrane and similar products should be used with caution when covering wound areas greater than 40% TBSA secondary to the increasing incidence of local infections. Porcine xenograft adheres well to the skin and is commercially available in large quantities. , Homograft is more likely to become vascularized and therefore reduces the number of graft changes. However this must be weighed against the potentially poor cosmetic results of vascularized homograft ( Fig. 36.5 ). Grafted areas must be immobilized and protected from shear forces. In both adults and children, continuous rotation or air fluidized (Clinitron) beds frequently are used.
Homograft vascularization occurring over a second-degree thermal injury, resulting in a poor cosmetic result.
Topical therapy.
As separation occurs at the dermal-epidermal junction, varying depths of viable dermis remain. If this dermis can be protected from toxic detergents, desiccation, mechanical trauma, and wound infection, then rapid reepithelialization by proliferation of basal keratinocytes from the skin appendages will occur. Bacterial proliferation on the unprotected wound surface with invasive infection leads to full-thickness skin necrosis. Hydrotherapy and topical antimicrobials provide debridement and infection control, which should be initiated early in the course of the disease. Effective topical antimicrobial agents include silver sulfadiazine cream, silver nitrate solution, chlorhexidine gluconate solution, and polymyxin-bacitracin ointment. , , Although silver sulfadiazine is widely used, concerns that its sulfonamide component can exacerbate the disease process remain a theoretic concern even though these concerns have not been confirmed in the literature. Additionally, an inhibitory effect on epithelialization and leukopenia requiring discontinuation has been observed. Alternatively, silver nitrate solution does not contribute to the ongoing drug reaction, and epithelialization is not inhibited. For patients with contaminated wounds due to delayed initiation of treatment, silver nitrate soaks can reduce contamination and prepare the wound for eventual biologic dressing. Silver nitrate solutions are hyponatremic and thus associated with approximately 350 mmol of sodium loss per day/m 2 treated. Serum electrolytes and osmolarity must be carefully monitored.
Chlorhexidine gluconate and polymyxin ointment are effective against gram-negative organisms, including P. aeruginosa , with low incidence of sensitivity. Moreover, chlorhexidine gluconate also shows bactericidal effects against gram-positive organisms.
Oropharyngeal mouth erosion resulting in severe dysphagia can be alleviated by the use of viscous lidocaine or cocaine rinses and thus ease oral administration of nutrients and fluids. Oral debris should be removed and the mouth rinsed or sprayed with antiseptic several times a day. Oral nystatin prevents intestinal overgrowth of Candida and decreases the risk of Candida sepsis.
Pulmonary involvement requires close supervision, with careful toileting including bronchoscopy, incentive spirometry, mobilization, and coughing to prevent infections and complications. If mechanical ventilatory support is necessary, the prevention of bronchopulmonary infection gains even more importance. Daily monitoring by blood assessment, including blood gas analysis, chest x-ray, and bacteriologic culture, are required to initiate timely antibiotic therapy or ventilatory support. Measures to prevent thromboembolism, such as the administration of low-dose or low-molecular-weight heparin, should be instituted on admission.
Ocular involvement should be assessed daily by an ophthalmologist. Conjunctival crusting can be minimized by the application of saline eye drops every hour. Any adhesions should be broken using a blunt instrument and bland eye drops or ointment applied frequently. Documented ocular infections are treated with organism-specific antibiotic therapy. Lacrimal duct obstruction may be detected early by performing Schirmer’s test. There are a wide range of ophthalmic treatment options, a review of which would be beyond the context of this chapter. One reasonable, practical approach is the “Triple-TEN” protocol described by Tomlins et al., which includes (1) subconjunctival steroids to blunt local inflammation, (2) amniotic membrane application, and (3) insertion of a scleral shell spacer to prevent symblepharon formation. Regardless of the specific treatment options taken, involvement of an ophthalmologist is clearly indicated.
Although it is not common in TEN, genitourinary mucosal involvement should be treated acutely with supportive care: pain control, hygiene, and topical treatments for pain relief and lubrication. Urinary catheterization needs to be weighed against the clinical stability and clinical scenario of the patient. Does the need for precise urine output outweigh the risk of increased infections that could occur with the placement of a catheter? Long-term sequelae include urethral stricture and phimosis, which can usually be managed with serial dilation and circumcision, respectively.
Vulvar involvement should also be managed proactively to minimize symptoms and (theoretically) attenuate the risk of long-term sequelae. The use of some topical medication options has been suggested, but none of these is considered the standard of care at this point. Mechanical treatments should be considered to prevent prolonged apposition of opposing inflamed mucosal surface to avoid fusion and synechiae. Vaginal dilators can be used to avoid fusion, although monitoring and regular changing are necessary to avoid infection. Finally, menstrual suppression should be considered to minimize the risk of vaginal adenosis. Depending on the extent and severity of the involvement of the vaginal area, consider a consultation with a gynecologist.
Nutritional support
Enteral nutrition should be initiated immediately once the patient is resuscitated. Because of the frequent presence of oral mucosal ulcerations, patients may be reluctant to take nutrition orally and thus require a nasogastric tube placement. Unlike burned patients who have significantly elevated metabolic rates, these patients appear to have metabolic rates only slightly above basal requirements. Weight stabilization and a positive nitrogen balance have been achieved in adults with 2500 kcal/day. ,
Soft tissue infections and other acute skin disorders
Staphylococcal scalded skin syndrome, necrotizing fasciitis, and purpura fulminans are examples of a group of conditions characterized by extensive soft tissue loss, rapid onset of critical illness, and death. Early, accurate diagnosis is essential to initiate appropriate action, such as extensive surgical excision in the case of necrotizing fasciitis or crepitant soft tissue infections. Burn care centers, with their acute and reconstructive capacities, have much to offer these patients with extensive skin loss.
Staphylococcal scalded skin syndrome
Staphylococcal scalded skin syndrome is the severe condition caused by exfoliative staphylococcal toxins and is characterized by systemic signs and symptoms and generalized involvement of the skin ( Fig. 36.6 ). It is important to make a diagnosis early, particularly to differentiate it from TEN, which has a different management and much greater mortality. Staphylococcal scalded skin syndrome is predominantly a disease of infancy (Ritter disease) and early childhood, with most cases occurring before the age of 5 years. Newborn nurseries are often the sites of outbreaks. Attendant staff may be infected or colonized with S. aureus strains producing epidermolytic toxins, thus emphasizing the importance of standard hygienic measures. Adult staphylococcal scalded skin syndrome is rare and usually associated with compromised renal function. Mortality is generally only 4% but can be much higher in adults (40%) depending on underlying diseases. ,
Staphylococcal scalded skin syndrome is characterized by diffuse, erythematous lesions with bullae formation (see left forearm). Epidermis is shed in sheets with minimal abrasion. The wounds are partial thickness and heal without surgical intervention.
Pathology
Two distinct epidermolytic toxins (ETA and ETB) are responsible for the blistering in staphylococcal scalded skin syndrome. ETA is heat stable, whereas ETB is heat labile and encoded by a bacterial plasmid. Most toxigenic strains of S. aureus are identified as group 2 phage. The exfoliative toxin is metabolized and excreted by the kidneys, leading to a predisposition of patients with renal immaturity (children) or renal compromise. The exfoliative toxins produce blistering by disrupting the epidermal granular cell layers through interdesmosomal splittings but without epidermal necrosis and with very few inflammatory cells. The exact mechanism of action of the toxins has not been determined, although it is felt that the toxins directly affect desmosomes. One might be proteolytic disruption of desmosomes with the toxin or part of its sequence act acting as a serine protease. , ,
Presentation
Onset may be marked by fever, malaise, and irritability. Scarlatiniform erythema is often accentuated in flexural and periorificial areas. The skin is generally tender to touch, and sheets of skin may peel away in response to minor trauma (Nikolsky’s sign). Blisters appear within 24 to 48 hours of rupture, leaving a characteristic moist erythematous epidermal base. Severe mucosal involvement is not a typical feature.
Diagnosis
Diagnosis of staphylococcal scalded skin syndrome can be made rapidly with a skin biopsy. The characteristic intraepidermal level of splitting is seen, with the split occurring at the granular layer level (stratum granulosum) with no epidermal necrosis or inflammatory cells in the corium. Immunofluorescent studies of the skin are negative. A Tzanck preparation from a scraping of the base of a freshly denuded area will reveal the affected cell population (i.e., acanthocytic keratinocytes). Bullae, denuded skin, and blood are usually sterile, however, and staphylococci can usually be cultured from nares, conjunctiva, or pharynx.
Management
With diagnosis, antibiotics should be started, and semisynthetic penicillinase-resistant penicillin analogs are indicated (e.g., methicillin or oxacillin) because the majority of group 2 staphylococci show resistance to penicillin. Administration of steroids to these patients is contraindicated. After screening for colonization, decontamination of colonized areas, especially the nasopharyngeal region in patients and nursing staff, may be advisable to prevent further spread. Fluid resuscitation is usually required at a lesser volume compared with a burn patient with a similarly involved BSA. Fluid substitution should be guided by urine output, hemodynamic parameters, and electrolyte and colloid status.
Until skin barrier function is restored, patients should receive appropriate wound dressings to prevent secondary wound infection. Topical agents are soothing and bacteriostatic. It needs to be pointed out that the wound initially is not colonized or infected, so alternatively, large areas can be more effectively managed with biologic or synthetic dressings. They have the advantage of eliminating the need for frequent dressing changes, which can be particularly traumatic for young children. Mortality usually is low but may occur in very young and adult patients, usually from sepsis or electrolyte imbalance on the basis of underlying disease. Complete wound healing is usually observed within 7 days, and scarring and altered pigmentation are not common.
Necrotizing fasciitis and bacterial myonecrosis
Necrotizing fasciitis is a soft tissue infection characterized by widespread necrosis of fascia and subcutaneous tissue, which may progress to muscle and skin necrosis. Overall mortality may still be as high as 50%. , Most cases of necrotizing fasciitis are due to polymicrobial infection including both anaerobic gram-positive cocci and gram-negative bacilli. Streptococcus, Staphylococcus, Enterococcus, and Bacteroides are commonly found. Infection with many bacterial species may result in bacterial myonecrosis. However, gas gangrene by Clostridia spp. results in severe systemic toxicity and higher mortality than necrotizing fasciitis. A deep contaminated wound frequently precedes the severe soft tissue infection. Streptococcal myositis has a mortality rate of between 80% and 100%. , Risk factors for both necrotizing fasciitis and bacterial myonecrosis have been identified as diabetes mellitus, intravenous drug use, age greater than 50, hypertension, and malnutrition/obesity. The presence of three or more of these risk factors was found to give a predictive mortality rate of 50% ( Fig. 36.7 ).
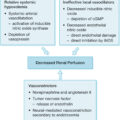
Flowchart of management of exfoliative and necrotizing conditions of the skin. SJS, Stevens-Johnson syndrome; TEN, toxic epidermal necrolysis.
Diagnosis
Early diagnosis is of extreme importance and consequence. Initial presentation is deceptive because the findings may be localized pain and edema without discoloration of the skin. Later, induration and erythema may be evident. Paresthesia of overlying skin and eventual dusky discoloration and local blistering may occur in the later course. Severe toxemia may develop, usually out of proportion to the local signs. Severe systemic alterations are characteristic of myonecrosis. Gas inclusion may be evident in subcutaneous tissues on x-ray. Computed tomography and magnetic resonance imaging may help in the diagnosis and provide information on the nature and extent of the infection. Frozen section biopsies may provide early histologic evidence of infection. Gram stains and microbiologic testing are very important diagnostic tools and guide antibiotic treatment. However, a definite distinction between necrotizing fasciitis, myonecrosis, and other soft tissue infections often can only be established during surgery.
Management
The key to successful management of necrotizing infections is early diagnosis and radical surgical intervention. Surgical exploration involves complete excision of all necrotic tissues. If more than one operation for debridement of infected necrotic tissue is needed, mortality increases from 43% to 71%; this outcome drastically highlights the importance of adequate initial necrosectomy. In patients with many risk factors, early amputation of the extremity, especially in cases of myonecrosis, should be considered. Broad-spectrum antibiotics are started preoperatively, although high-dose penicillin is appropriate for clostridial infections. However, antibiotic treatment is no substitution for surgical intervention. Adequate fluid resuscitation and nutritional support are also required. Wounds are packed open with antiseptic-soaked dressings, which need to be changed frequently. Kaiser and Cerra have reported unsatisfactory results with either early application of porcine xenografts or burn wound topical antimicrobials. Complete control of local and systemic infection is required before wound closure is addressed.
As in burns, secondary infections must be prevented by proper wound management. Biologic or synthetic dressings offer the advantages of decreased pain, decreased fluid loss, and prevention of secondary infection. Frequently large areas of skin and soft tissue loss result from this disease and will eventually require extensive surgery to achieve adequate closure.
Some authors advocate the use of hyperbaric oxygen and claim that it results in decreased mortality and reduced need for debridement; however, most of these reports are case reports or uncontrolled trials, and adequate prospective controlled trials in patients are still lacking. , In animals, hyperbaric oxygen therapy alone did not improve survival or bacterial colonization but did show adjuvant effects to antibiotic treatment. In summary, hyperbaric oxygen therapy, if available, should not delay radical surgical debridement and should be used as an adjunct to radical surgery and antibiotic therapy. ,
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree