30 Exenteration
Exenteration involves the removal of the soft-tissue contents of the orbit including the eye, extraocular muscles, periorbita, and part or all of the eyelids.
Exenteration is most commonly performed in the treatment of malignant tumors of the eye and ocular adnexa. This includes primary orbital tumors, ocular and eyelid neoplasms with orbital invasion, lacrimal gland malignancies, and tumors extending into the orbit from the adjacent cranial or nasal cavities or from paranasal sinuses. Recent studies suggest that exenteration may offer no benefit over enucleation with local excision in the management of choroidal melanomas with extrascleral extension. In the management of certain neoplasms, such as orbital lymphoma and rhabdomyosarcoma, radiation and chemotherapy have supplanted exenteration as primary therapeutic modalities. In each case, a review of recent treatment advances for the tumor in question is advised. In some cases of orbital metastases or advanced orbital disease, palliative exenteration may be warranted for tumor debulking or pain control. On rare occasions, exenteration may be indicated in the treatment of nonmalignant conditions such as severe trauma, mucormycosis, meningioma, orbital contracture caused by sclerosing pseudotumor, and congenital deformities.
PREOPERATIVE EVALUATION
A definitive pathologic diagnosis based on permanent histologic sections must be established before proceeding with orbital exenteration. Under no circumstances should exenteration be performed based on frozen-section interpretation of a biopsy. Preoperatively, the extent of the lesion should be evaluated by physical examination, computed tomography, magnetic resonance imaging, and ultrasound, as indicated. The surgical procedure may then be modified, depending on the biologic activity, extent, and location of the disease process. For tumors involving the posterior aspect of the orbit, the eyelid skin may be preserved to partially line the exenterated socket. In contrast, partial or complete excision of the eyelids is usually required for lesions arising from the eyelids, conjunctiva, or the anterior segment. If the extent of skin involvement cannot be determined clinically, Mohs microscopically controlled excision may be helpful in clearing the epithelial margins and allowing maximal preservation of the uninvolved eyelid skin. In some cases, bone removal may be required if tumor invasion into the bony orbit has occurred. Malignancies arising from the nose, paranasal sinuses, or cranial cavity often require collaboration with a neurosurgeon or otolaryngologist for optimal management.
Following removal of the orbital soft tissues, the socket may be lined with a split-thickness skin graft, or it may be allowed to granulate by secondary intention. The placement of a skin graft prolongs the surgical procedure slightly and involves a second operative site. However, it shortens the socket healing process and provides a smooth, clean socket surface. Healing by secondary intention will result in a thicker, irregular socket surface that may obscure detection of early tumor recurrence.
Transposition of the temporalis muscle and fascia has been advocated to minimize the depth of the socket postoperatively. The disadvantages of this technique include a cosmetic depression in the temporal area and masking of tumor recurrences by the resultant thick apical lining. However, in some cases of exenteration involving extensive tissue loss or compromised vascularity following radiation therapy, local tissue flaps including the temporalis and median forehead flaps may be used.
PATIENT PREPARATION
The patient must be prepared for the loss of the eye and for the cosmetic deformity that results from orbital exenteration. Hypesthesia of the forehead and cheek owing to removal of branches of the fifth nerve during exenteration should be anticipated. Also, the patient should be aware of the possibility of tumor recurrence or metastatic spread, despite surgical intervention. Discussing the options for cosmetic rehabilitation preoperatively, with the use of photographs to demonstrate the postsurgical appearance with an orbital prosthesis, may be beneficial in gaining acceptance of the planned procedure.
SURGICAL PROCEDURE
Exenteration is performed under general anesthesia.
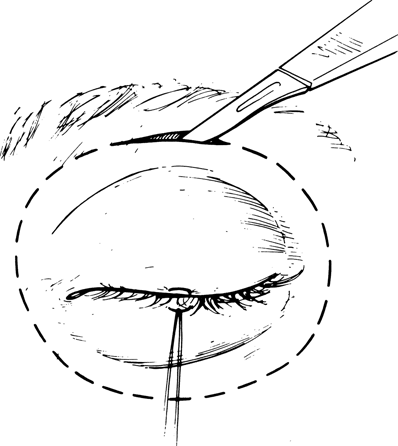
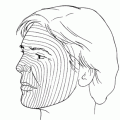
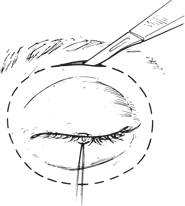
Figure 30-1. The planned incision is marked and the periocular region infiltrated with lidocaine (Xylocaine) with epinephrine for hemostasis. If eyelid skin cannot be preserved, the incision is made directly over the orbital rim. A 4–0 silk traction suture is passed through the upper and lower eyelid margins and tied together.
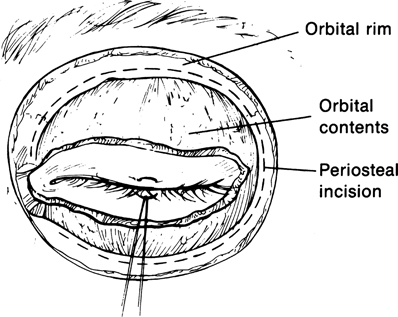
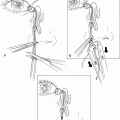
Figure 30-2. The incision is made over the orbital rim and is continued through the underlying orbicularis until the periosteum of the orbital rim is exposed.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree