28 Evisceration
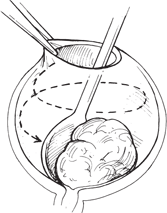
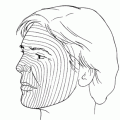
Evisceration is a surgical procedure in which the entire intraocular contents are removed and the scleral shell is left in situ. Evisceration can be performed with or without keratectomy. Since the sclera, Tenon’s capsule, extraocular muscle attachments, and orbital suspensory structures are virtually undisturbed, evisceration is associated with better postoperative cosmesis and motility than with enucleation. There are fewer tendencies for postoperative enophthalmos, superior sulcus deformity, or ptosis. Additionally, evisceration is simpler and quicker to perform than enucleation, which permits performance of this procedure on even the most debilitated patient.
INDICATIONS
The relative indications for enucleation versus evisceration are controversial. Sympathetic ophthalmia, although rare, is the most feared complication associated with this technique. In contrast with enucleation, in which uveal tissue is completely removed, pigmented melanocytes remain within the perineural region and emissary channels of the sclera following evisceration and may potentially incite an inflammatory response in the fellow eye. The benefits of improved cosmesis must be weighed against the risk of sympathetic ophthalmia, and the decision made depending on the particular clinical situation, the philosophy of the surgeon, and the informed preference of the patient.
Evisceration is particularly suited for the treatment of medically uncontrolled endophthalmitis or corneal ulceration in which vision and the structural integrity of the globe cannot be preserved. In this clinical setting, the intraocular abscess is evacuated, with minimal orbital tissue disruption. The intact scleral shell serves as a barrier for the spread of infection into the orbit and the potential subarachnoid space of the optic nerve, thereby minimizing the risk of orbital cellulitis or meningitis. Additionally, excessive bleeding from inflamed orbital tissues is avoided. In the presence of a localized anterior infectious scleritis, evisceration remains an option if adequate sclera will be available following excision of the infected tissues. However, if there is extensive scleritis or an extrascleral abscess has developed, enucleation is necessary for optimal removal and drainage of the infected tissues.
Evisceration is contraindicated for patients in whom an intraocular tumor is suspected or cannot be assured by clinical, computed tomography scan, or ultrasound examinations. This procedure should not be considered if a complete histopathologic examination of the globe is needed. Evisceration should also be avoided if the scleral shell is thinned or inadequate, such as in a posterior staphyloma, posterior segment trauma, or phthisis bulbi. In cases of fungal endophthalmitis, the tendency for early invasion of the scleral wall may also argue for enucleation, rather than evisceration.
SURGICAL PROCEDURE
Evisceration is performed under general or local retrobulbar anesthesia. Retention of the cornea has been advocated to allow for a larger implant and greater volume replacement. However, because of the potential for persistent sensation, thinning, and perforation of the cornea, we prefer the evisceration technique that includes keratectomy.
A speculum is placed between the eyelids. A 360° limbal peritomy is performed. The Tenon’s capsule and conjunctiva are separated from the underlying sclera anterior to the tendinous insertions of the rectus muscles.
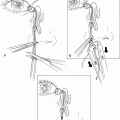
The anterior chamber is entered at the posterior surgical limbus with a size 11 blade. Care is taken to avoid penetrating the iris, lens, or the ciliary body. Cataract scissors are used to perform the keratectomy.
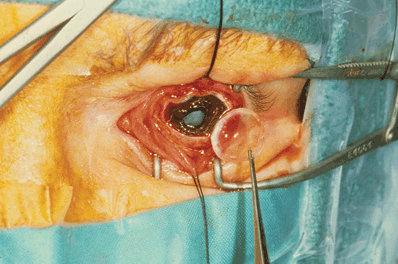
Figure 28-1. Once the corneal button is removed and the anterior chamber exposed, bacterial culture specimen may be collected.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree