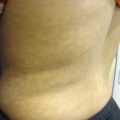
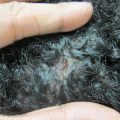
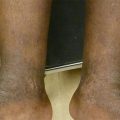
Figure 5.1
Dissecting cellulitis. Scattered erythematous papules and pustules are noted on the vertex with alopecia and tufted hairs
Clinical Differential Diagnosis
The patient’s presentation is most consistent with dissecting cellulitis of the scalp (DCS). Other conditions to be considered in the differential diagnosis included acne keloidalis nuchae, tinea capitis or kerion, folliculitis decalvans, and cutis verticis gyrata. Unlike DCS, acne keloidalis does not present with sinus tracts, suppurative nodules, or cicatricial alopecia. A KOH preparation or positive fungal culture can help differentiate DCS from tinea capitis. Folliculitis decalvans can present with cicatricial alopecia like DCS, but does not present with sinus tracts or nodules. It is sometimes categorized as a more superficial variant of DCS. Cutis verticis gyrata is usually asymptomatic and does not present with sinus tracts or suppurative nodules (Madu and Kundu 2014; Ross et al. 2005).
Histopathology
A biopsy was not performed in this case because the history and physical exam were felt to be sufficient for diagnosis. When biopsy of DCS is performed, histopathology reveals distention of the follicular infundibulum with perifollicular, mixed neutrophilic and lymphoplasmacytic inflammation. The inflammatory process involves the lower dermis and subcutaneous junction. Scarring and fibrosis can be seen in chronic lesions (Sperling 2001).
Diagnosis
Dissecting cellulitis of the scalp (DCS)
Case Treatment
The nature of the diagnosis of DCS was reviewed with the patient. Treatment options including oral antibiotics, oral or intralesional corticosteroids, oral isotretinoin, laser treatments, and tumor necrosis factor alpha (TNF-α) inhibitors were discussed. After a discussion of the risks and benefits of each treatment, the patient elected to start oral isotretinoin given the extensive presentation of his disease and the desire to reduce the development of further scarring alopecia. The patient was started on 1 mg/kg/day of oral isotretinoin until clinical remission of the disease was achieved 3 months later, followed by a maintenance dose of 0.75 mg/kg/day for 4 months afterwards. His cumulative dose was 180 mg/kg. Upon completion of the treatment, the patient had satisfactory partial hair regrowth in areas of previous hair loss and did not have recurrence of the disease at 1-year follow-up.
Discussion
Dissecting cellulitis of the scalp is a chronic inflammatory condition of the follicles of the scalp characterized by fluctuant nodules, cysts, draining sinus tracts, and secondary scarring alopecia (Madu and Kundu 2014). At least 80 % of all cases of dissecting cellulitis of the scalp occur in black men between the ages of 18–40. It has been less frequently reported in white males (10 % of cases), in women, and in children (Ross et al. 2005).
DCS follows a chronic and relapsing course (Ross et al. 2005). It initially presents as a follicular pustule (folliculitis) at the scalp vertex or occiput, which then transforms into a painful nodule. Multiple similar and contiguous papules and nodules occur shortly thereafter, giving the scalp a cerebriform appearance. During periods of waning, hypertrophic or atrophic scarring of the scalp remains and a pattern of cerebriform folds and furrows mimicking cutis verticus gyrata may occur (Coley and Alexis 2009). The condition does not usually involve the entire scalp. Purulent or keratinaceous discharge may be expressed from the lesions spontaneously or with applied pressure. Due to the interconnecting sinus tracts, pressure applied on one nodule/abscess can lead to expression of purulent material from an interconnected nodule. An unpleasant odor can be associated with the disease due to the presence of secondary infection. Early disease can present with a nonscarring alopecia. Long-standing disease can lead to cicatricial alopecia. The inflammatory nature of the disease can lead to the development of post-inflammatory hyperpigmentation.
The precise mechanism for the development of DCS is unknown but is thought to involve follicular occlusion. Keratin debris can occlude the pilosebaceous unit leading to follicular expansion, subsequent inflammation, and dilation (Madu and Kundu 2014). Secondary bacterial infection of the follicle with either Staphylococcus aureus, Pseudomonas aeruginosa, or anaerobic bacteria leads to a folliculitis or perifolliculitis (Coley and Alexis 2009). When these inflamed follicles rupture they release keratin and bacteria, which precipitates a localized neutrophilic and granulomatous response leading to abscess formation. Abscesses can then expand and coalesce to form interconnecting abscesses and sinus tracts (Coley and Alexis 2009). The presence of hair follicles is necessary for the disease process; when follicles are eliminated, such as by laser hair removal or scalpectomy, the disease improves (Coley and Alexis 2009).
On trichoscopy of DCS, early findings can mimic non-scarring alopecia with empty follicular openings, yellow dots, and black dots. With progression of disease, dermoscopy reveals yellow structureless areas and dystrophic hair shafts with overlying yellow dots that have a “three-dimensional” structure. Dermoscopy of long-standing disease will reflect scar formation and reveal confluent, ivory-white areas lacking follicular openings (Mubki et al. 2014).
Biopsy may or may not be necessary to make a diagnosis of DCS, depending on the extent of the disease and the phase of disease that the patient presents in. Before undertaking biopsy, the physician should consider the risk of hypertrophic scarring and keloid formation, which occur at higher rates in patients with ethnic skin (Robles and Berg 2007). Cosmesis should be considered when choosing a biopsy site on the scalp. Intralesional corticosteroid injection can be considered to minimize the risk of keloid formation in patients with a known keloid diathesis.
DCS is associated with hidradenitis suppurativa and acne conglobata, collectively referred to as the follicular occlusion triad or, when seen in conjunction with pilonidal cysts, a tetrad. All of these disorders share pathogenesis related to follicular occlusion, secondary infection, and deep inflammation (Ross et al. 2005). Hidradenitis suppurativa is the development of deep-seated painful nodules, abscesses, draining sinuses, and scarring in intertriginous areas. Acne conglobata is a nodulocystic form of acne vulgaris that presents with comedones, papules, pustules, nodules, abscesses, and draining sinus tracts on the face, chest, back, and buttocks. Pilonidal cysts present as painful cyst near the intergluteal cleft that can lead to the development of an abscess or draining sinus tracts.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree