Eyelid defects disrupt the complex natural form and function of the eyelids and present a surgical challenge. Detailed knowledge of eyelid anatomy is essential in evaluating a defect and composing a reconstructive plan. Numerous reconstructive techniques have been described, including primary closure, grafting, and a variety of local flaps. This article describes an updated reconstructive ladder for eyelid defects that can be used in various permutations to solve most eyelid defects.
Key points
- •
The primary goals of eyelid reconstruction are restoration of eyelid function, corneal protection, and recreating the natural appearance and symmetry of the eyelids.
- •
The anterior and posterior lamella and the tarsoligamentous sling are considered discrete subunits of the eyelid and their distinction can guide reconstructive options.
- •
Disruptions of the lacrimal system should be repaired to prevent epiphora.
- •
Whenever possible, vertical surgical tension near the lid margin should be converted to horizontal tension in the eyelids to minimize vertical tension, lid retraction, and cicatricial ectropion.
- •
A variety of options exist for eyelid reconstruction and familiarity with many different methods will give the reconstructive surgeon the ability to analyze an eyelid defect and choose an optimal method for repair.
Introduction
The eyelids are an important aesthetic unit of the face. They have multiple functions, most notably serving as the primary protectant of the globe. Surgically restoring the natural form and function of the eye can be complex and challenging. Defects of the upper and lower eyelids frequently result from cancer ablation but also arise from trauma, burns, congenital defects, and autoimmune disease. The eyelids are composite structures with an anterior lamella comprising skin and orbicularis oculi muscle, the middle lamella comprising the orbital septum and lower lid retractors, and a posterior lamella comprising tarsus and conjunctiva. This article discusses the anterior and posterior lamellae as discrete units during repair. Eyelid reconstruction involves replacing one or both lamella, depending on the size and anatomic position of the defect, as well as other structures such as the lacrimal drainage system. Thus, reconstruction can be approached in a variety of ways and familiarity with a diversity of methods will yield the best reconstructive outcome.
Introduction
The eyelids are an important aesthetic unit of the face. They have multiple functions, most notably serving as the primary protectant of the globe. Surgically restoring the natural form and function of the eye can be complex and challenging. Defects of the upper and lower eyelids frequently result from cancer ablation but also arise from trauma, burns, congenital defects, and autoimmune disease. The eyelids are composite structures with an anterior lamella comprising skin and orbicularis oculi muscle, the middle lamella comprising the orbital septum and lower lid retractors, and a posterior lamella comprising tarsus and conjunctiva. This article discusses the anterior and posterior lamellae as discrete units during repair. Eyelid reconstruction involves replacing one or both lamella, depending on the size and anatomic position of the defect, as well as other structures such as the lacrimal drainage system. Thus, reconstruction can be approached in a variety of ways and familiarity with a diversity of methods will yield the best reconstructive outcome.
Content
Physiology of the Eyelid and Lacrimal System
The primary functions of the eyelids include the protection and maintenance of the orbital contents, light regulation, and facial expression. They also serve as an important aesthetic focal point of the face. Intact eyelid closure establishes an air-tear barrier over the cornea. Eyelids rest on the surface of the globe and wick tears across as they glide over the corneal surface. The bulbar conjunctiva on the surface of the globe is continuous with the palpebral conjunctiva lining the inner surface of eyelids by means of a redundant fornix. Conjunctival relationships must be maintained or restored during reconstruction to preserve blink efficiency for corneal wetting and normal tear flow. Corneal drying and irritation leads to exposure keratopathy that, if prolonged, can result in corneal scarring and infection.
The lacrimal system is closely associated with the medial canthus of the eyelid and allows for proper outflow of tears into the nasal passage. Physical disruption of the lacrimal system can cause epiphora, blurred vision, and severe patient annoyance. Lacrimal punctal eversion (aka punctal ectropion) after lower lid reconstruction can also result in improper tear drainage.
Surgical Anatomy of the Eyelids
The eyelids are essentially bilamellar structures comprising the anterior and posterior lamella and supported by the tarsoligamentous sling a branch of the oculomotor nerve
- •
The anterior lamella comprises skin and orbicularis oculi muscle.
- •
The posterior lamella comprises the tarsal plate and conjunctiva.
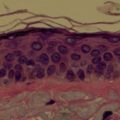
The upper eyelid layers vary depending on their distance from the palpebral fissure or eyelid crease. The eyelid crease is formed by the cutaneous insertion of the aponeurosis of levator palpebrae superioris muscle ( Fig. 1 ):
- •
Below lid crease: epidermis, orbicularis oculi, levator aponeurosis, tarsus, and conjunctiva.
- •
Above lid crease: epidermis, orbicularis oculi, orbital septum (inserts onto the levator aponeurosis before attaching to the tarsal plate), orbital fat, levator aponeurosis, Müller muscle, and conjunctiva.
In the lower eyelid, the capsulopalpebral fascia (aka lower lid retractors) is similar and analogous to the levator aponeurosis of the upper lid. This is a fascial extension of the inferior rectus muscle sheath and causes downward movement of the lower lid via the ophthalmic nerve (cranial nerve 3). Additionally, the inferior tarsal muscle is analogous to Müller’s muscle and causes downward movement of the lid via sympathetic input.
The medial and lateral canthal tendons attach to the tarsal plates and provide anterior-posterior stability to the eyelids as the tarsoligamentous sling. The medial canthus attaches to the anterior and posterior lacrimal crest. The lateral canthus attaches posterior to the lateral orbital rim at Whitnall’s tubercle. The levator aponeurosis and capsulopalpebral fascia attach to the superior and inferior tarsal plates, respectively, and provide vertical stability.
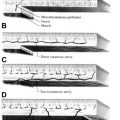
The orbicularis oculi muscle, innervated by the facial nerve, is subdivided into the pretarsal, preseptal, and orbital segments based on its location overlying the tarsus, septum, and orbital rim, respectively. The gray line of the eyelid margin represents the pretarsal orbicularis insertion. The pretarsal and preseptal orbicularis muscles surround the lacrimal system and facilitate the movement of tears from the canaliculi to the tear sac. The lacrimal puncta are located at the medial edge of the upper and lower eyelid. They open into the lacrimal canaliculi, which are encased in orbicularis oculi muscle as discussed previously. Lacrimal canaliculi coalesce into the lacrimal sac, which is located posterior to palpable anterior limb of medial canthal tendon ( Fig. 2 ). The orbicularis oculi muscle inserts on the lateral wall of the lacrimal sac, which aids in dilation of the sac for tear drainage. The lacrimal sac continues into the nasolacrimal duct, which drains into the inferior nasal meatus.
The ophthalmic branch of the internal carotid is the major vascular contribution to the eyelids, supplying the superior and inferior tarsal arcades in the eyelids, as well as the supraorbital and supratrochlear arteries of the superior orbit. The facial and maxillary artery branches of the external carotid systems contribute to the medial and lateral canthus. The upper lid has a marginal lid arterial arcade, located 2 to 3 mm from the eyelid margin, and a peripheral arcade, located at the border of the levator aponeurosis and Müller’s muscle. The lower lid only has a marginal arcade, located 4 mm below the eyelid margin (see Fig. 1 ). Vascular compromise exists if the arterial arcades are disrupted both medially and laterally. The venous supply to the lids is ample and complex. The angular and superficial temporal veins receive the superficial eyelid venous drainage and the muscular tributaries of the ophthalmic vein receive the deep venous drainage.
Reconstructive Principles
A detailed knowledge of the components and anatomy of the eyelid serve as a framework for reconstruction based on the underlying structures involved. Surgical objectives rely on the principles of restoring the basic function and appearance of the eye ( Box 1 ).
- •
Restore a nonkeratinizing mucosal epithelium to the inside of the eyelid to protect and wet the cornea.
- •
Provide a rotationally stable eyelid margin to protect the cornea from skin, hairs, and lashes.
- •
Ensure eyelid apposition to the globe to facilitate formation of corneal tear film.
- •
Use flexible and firm connective tissue frame to provide support and shape for the eyelid.
- •
Restore protractor and levator muscle function to close and open the eyelid.
- •
Achieve symmetry with the contralateral eyelid.
In other areas of facial reconstruction, closure is oriented parallel to relaxed skin tension lines (RSTLs) to minimize the appearance of scars. In the periocular areas, use of RSTLs provides satisfactory outcomes at the glabella, medial canthus, lateral canthus, and eyebrows. However, at the eyelid margin, closure parallel to the RSTLs can create vertical surgical tension and cicatricial ectropion. Thus, wound closure along the eyelid margin should be oriented perpendicular to RSTLs to convert vertical tension to horizontal tension. In certain cases, dermatochalasis (redundant skin) may permit horizontally oriented ellipses in the lid crease.
Partial-thickness eyelid defects can first be subdivided into anterior lamellar or posterior lamellar defects. In isolated anterior lamellar defects, horizontally oriented local flaps are preferred over free skin grafts or secondary healing. Local flaps provide excellent adjacent skin texture and color match and less tissue contraction. The rich vascular supply of the eyelid provides a unique environment for what might otherwise be considered a tenuous flap. One exception to healing via secondary intention exists in small (<1 cm) medial canthal defects centered between the upper and lower eyelids because of the concave nature of this area.
In full-thickness defects, reconstruction should be considered for each lamella separately with an intact blood supply for at least one. Typically, a local flap will be used to reconstruct one lamella and a graft use to reconstruct the other lamella. Full-thickness defects are categorized based on the percentage of lid involvement.
Upper lid reconstruction poses more challenges than lower lid reconstruction because of several factors. The upper lid levator function must be preserved in contrast to reconstructions in the relatively stationary lower lid. Likewise, the narrower lower lid tarsus (4-5 mm) versus the upper lid tarsus (11–12 mm) provides less tarsal tissue for cross-lid transfer. The upper lid is wider and its adjacent forehead and temporal skin are thicker and less mobile than the cheek and zygomatic tissue adjacent to the lower lid. Fortunately, most eyelid cancers, and thus defects, are found on the lower eyelid.
Grafts for Partial-Thickness Reconstruction
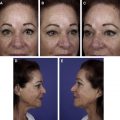
A variety of grafts can be used to reconstruct partial-thickness lid defects. Anterior lamellar defects can be reconstructed with a full-thickness skin graft from an ipsilateral or contralateral blepharoplasty incision to provide the best color and contour match ( Fig. 3 ). Skin grafts are usually reserved for cases not amenable to local flaps because of defect size or patient comorbidities that preclude a complex reconstruction. Skin graft repairs obviate additional incisions or scars near the defect but tend to have a patch appearance with skin texture and color mismatch. The tendency of elderly patients to have thinner skin results in a better color and texture match when compared with similar grafts in younger patients ( Fig. 4 ).

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree