Chapter 11 Filler Injection of the Nasojugal Groove and Palpebromalar
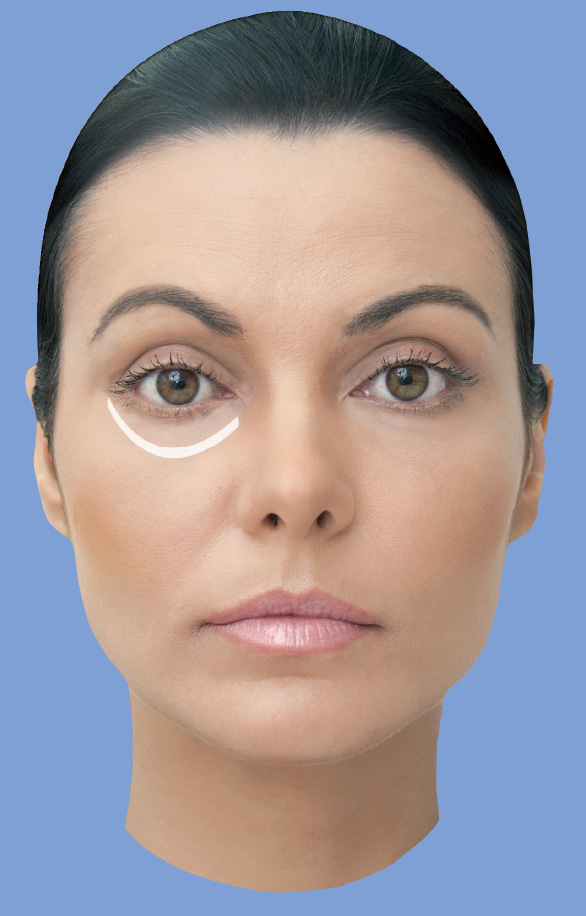
Introduction
The nasojugal groove (NJG) extends inferolaterally from the medial commissure to the midpupillary line. In some patients, the palpebromalar groove (PMG) is visible laterally to this point. Sometimes, the NJG and the PMG merge with age, forming a single continuous groove, which clearly marks the protrusion of orbital fat cranially, and the malar region distally, which is often already atrophied.
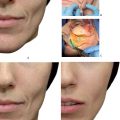
According to Hirmand’s classification, there are three classes of NJG: In class 1, patients have only lost volume in the NJG. In class 2, there is volume loss in the medial and lateral orbital areas, and flattening of the anterior malar region, whereas in class 3, the lateral and medial grooves have been totally depressed, and there is advanced volume loss in the anterior malar and zygomatic regions (Fig. 11.21). 1 ,. 2
These grooves give the face a tired, aged, and/or sad look. This area is considered to be one of the most challenging areas of the face to treat because overcorrection, a very superficial injection, or use of inadequate materials can lead to unacceptable esthetic results.
Anatomy
The orbit is the foundation of the periorbital complex and is formed by seven bones: the zygomatic, frontal, maxillary, ethmoid, sphenoid, lacrimal, and palatine bones. It has a conical structure that holds the eyeball, intraocular muscles, and orbital fat. The principal function of orbital fat is to lubricate and cushion the eyeball and intraocular muscles. Inferior orbital fat is divided into three pads, namely, nasal, central, and lateral, which are contained by the orbital septum that extends from the tarsus to the inferior orbital rim.
The palpebral portion of the orbicularis oculi muscle (OM) covers the orbital septum and inserts distally to the inferior orbital rim. This portion is found below the skin, as often there is no subcutaneous tissue in this region. However, the orbital portion of this muscle originates below the palpebral portion, 0.5 to 1 cm below the inferior orbital rim. The nasolabial and superficial medial cheek fat pads are above the orbital portion; below it, the suborbicularis oculi fat (SOOF) pad, also known as prezygomatic fat, can be seen.
The palpebral and orbital portions are “attached” to the inferior orbital rim medially by the tear trough ligament and laterally by the orbicularis retaining ligament (ORL). 3
The tear trough is an anatomical structure that arises from a separation between the palprebral portion (cranial) and orbital portion (caudal) of the OM at its point of origin in the maxilla. The NJG is the clinical manifestation arising from the sum of the following anatomical elements (Fig. 11.15A andB): 4
Skin and subcutaneous tissue: The palpebral region has extremely thin skin, with very little or no subcutaneous tissue; however, in the malar region, the skin is thicker and there is abundant subcutaneous tissue.
Muscular plane: The distinct separation between the palpebral portion (cranial) and the orbital portion (caudal) of the orbicular muscle at its origin in the maxilla (tear trough) creates a depression at the site of the NJG.
Osseous plane: Constitutional maxillary recession or maxillary bone remodeling during aging (see Chapter 4) makes the palpebral region deeper.
Osteocutaneous ligaments: The tear trough ligament pulls the medial infraorbital skin toward the maxilla. The same effect occurs with the lateral infraorbital skin, which is pulled by the ORL.
Prolapse of infraorbital fat: Aging causes herniation of the infraorbital fat and atrophy of malar fat, which makes the NJG more prominent.
Consequently, it can be concluded that the NJG is the result of “unevenness,” which can be seen medially between the palpebral and nasolabial regions. The PMG in turn lies between the infraorbital fat and the ORL, above the junction between the palpebral portion (cranial) and the orbital portion (caudal) of the OM (Fig. 11.1,11.2,11.5, and11.7–11.13).
Vascularization
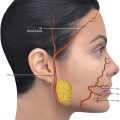
The NJG is supplied by the angular artery and the infraorbital artery, with their respective branches and anastomoses. For example, after crossing the medial canthal tendon superficially, the angular artery anastomoses with the dorsal nasal branch of the ophthalmic artery, which is a branch of the internal carotid artery. In turn, the PMG is supplied by the zygomatico-orbital artery and facial transverse artery, which are branches of the facial artery (Fig. 11.3,11.4, and11.6).
Technique
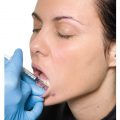
Treating the NJG consists of leveling the junction between the lower eyelid and the nasolabial region. Small amounts (0.1 to 0.5 ml) are used on each side, and the supraperiosteal or intramuscular application planes are used. Very superficial injections should be avoided because of the risk of the Tyndall effect and visible nodules. Nodules, irregularities, and discoloration are easily visible because of the thin skin. As the product is hydrophilic, and because of the water-retaining propensity of this area, 80% of the NJG can be corrected and, if necessary, the remaining 20% can be filled after 2 weeks.
The indication for the procedure is an important factor. It should be performed with caution in patients with moderate to severe palpebral flaccidity and excessive fat protrusion, who usually benefit from surgical treatment. This region should be assessed together with the malar region and, when necessary, this area can be augmented first, and then the NJG. If a cannula used, apply topical anesthetic or subdermal bleb of anesthesia (Fig. 11.22–11.25).
Nasojugal Groove
Technique with submuscular cannula:See Figs. 11.14 and11.16.
Technique with supraperiosteal cannula:See Figs. 11.16 and11.19.
Technique with supraperiosteal needle:See Figs. 11.17–11.19.
Palpebromalar Groove
Small supraperiosteal boluses can be applied with a needle. The skin needs to be stretched beforehand to check for the presence of vessels, then aspiration and slow injection, or retrograde injection with a cannula in the supraperiosteal and/or intramuscular planes, can be performed (Fig. 11.20).
Technique with supraperiosteal cannula:Fig. 11.20.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree