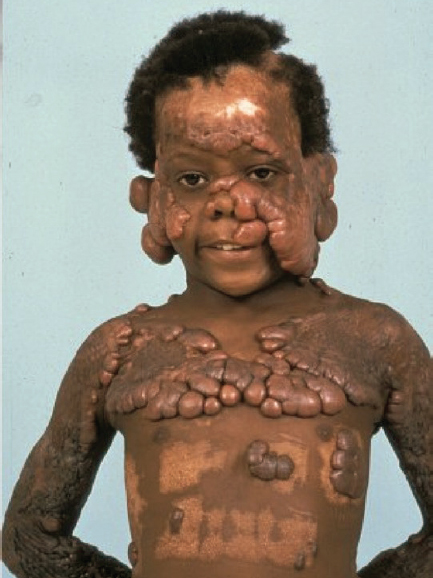
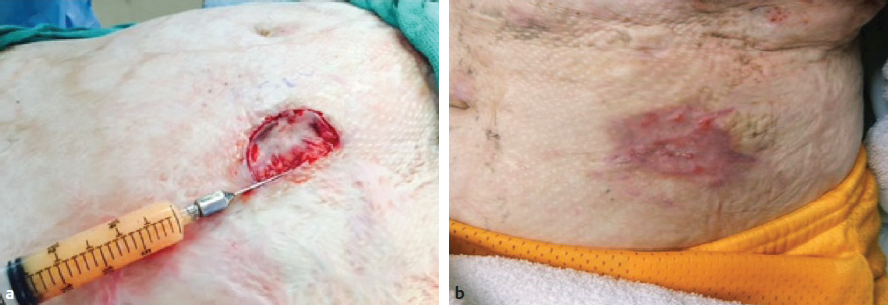
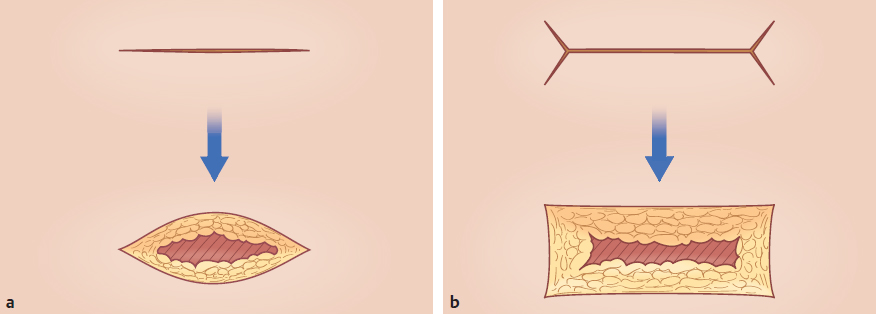
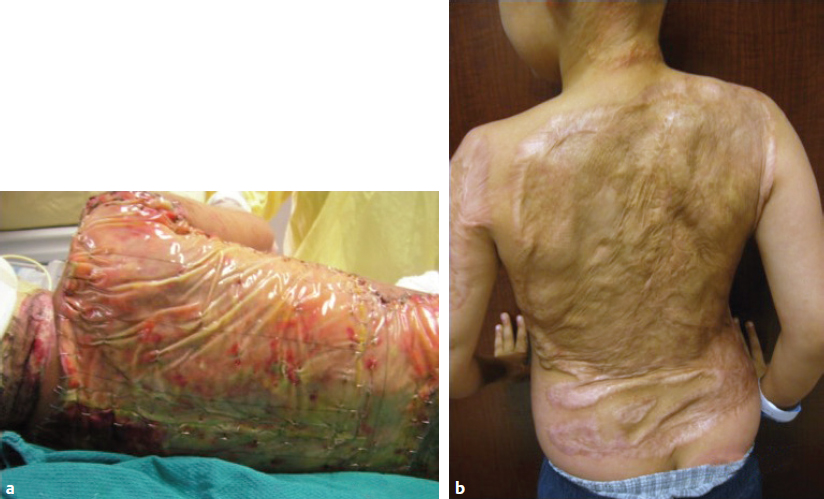
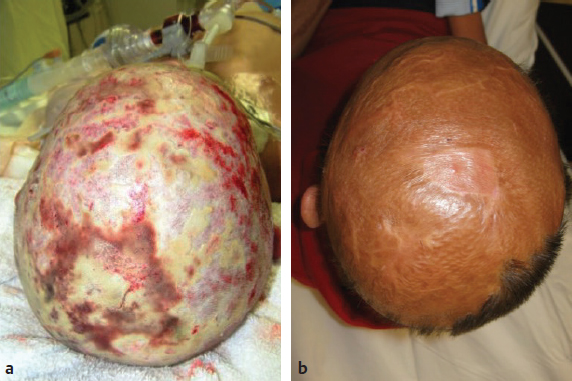
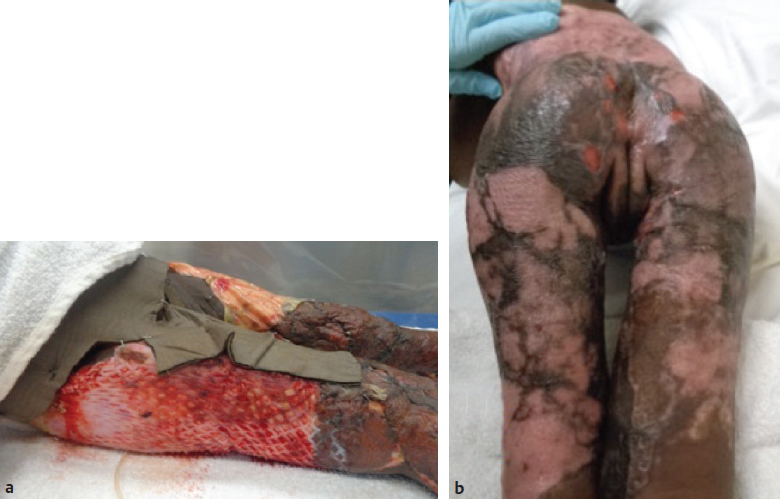
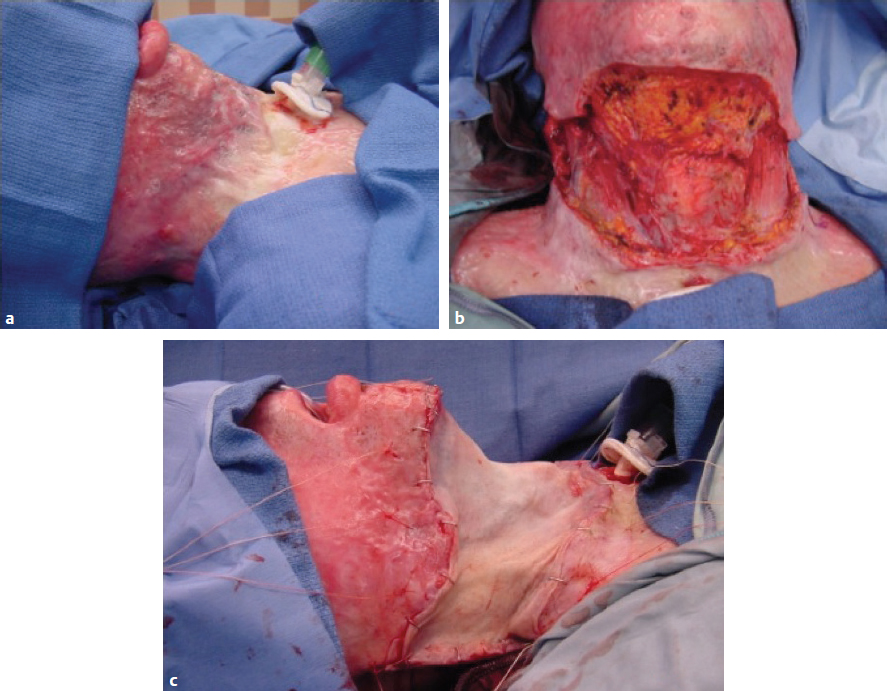
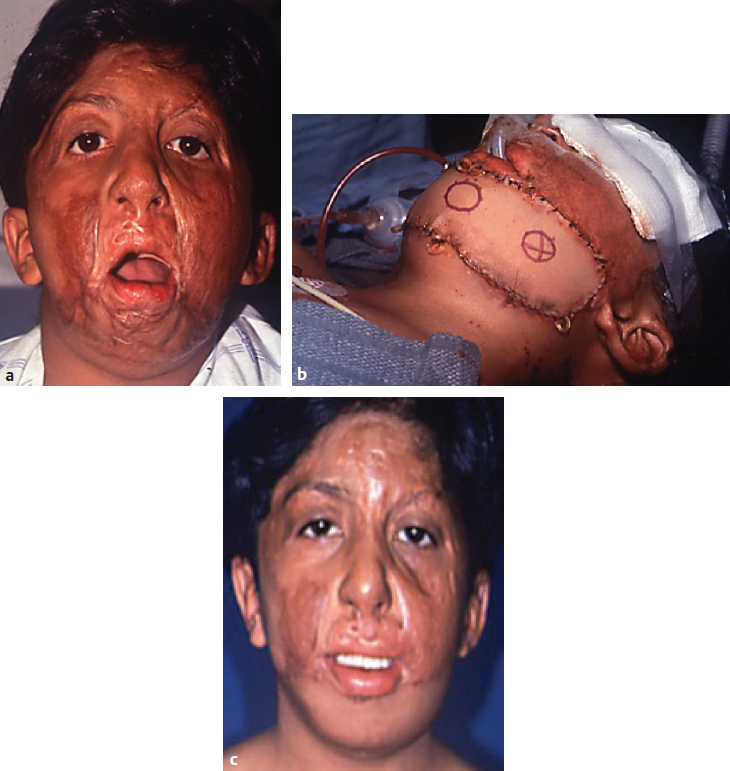
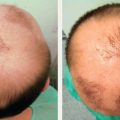
CHAPTER Unfavorable scar maturation is an anticipated and challenging outcome after acute burn management. The goal of acute burn care is to minimize the need for secondary reconstruction. However, secondary burn reconstruction is often necessary to return a patient to a state of optimal function while maximizing the aesthetic appearance. The goal of this chapter is to discuss the most common deformities that result from acute management of burn injury and their treatment (Fig. 70.1). Fig. 70.1 After a scalding injury this 7-year-old had severe keloid formation in areas of split-thickness skin grafts, healed burn, and donor sites. Her brother was also injured in the same bathtub scald and experienced severe keloid formation. Summary Box Common Postburn Deformities • Scar contracture • Hypertrophic and keloid scars • Scar hypopigmentation and hyperpigmentation • Unfavorable scar contour • Scar-associated pruritus and pain • Heterotopic ossification • Alopecia Reconstruction of burn scars should be delayed beyond 12 to 24 months after acute injury unless they interfere with activities of daily living (ADLs). This time will allow for full maturation of the scar tissue and optimization of nonsurgical treatments. Hyperemic, indurated, and immature scars during the inflammatory phase of healing are technically challenging to manipulate because of their immobility and lack of tensile strength. Furthermore, operating on a scar during this immature phase of healing can lead to a heightened and recurrent inflammatory state and overall worsening of the scar. Fig. 70.2 (a) This 14-year-old female pediatric patient had a 40% flame burn 10 years prior that was treated with Integra bilateral dermal regeneration template and a split-thickness skin graft. Fat grafting using the thigh as a donor site was used to improve the pruritic scar, and a split-thickness skin graft was used to reconstruct ulcerations that formed from picking. (b) Follow-up of the healed graft with resolved pruritus. Although it is ideal to allow the scar to mature before reconstruction, there are certain instances in which more prompt intervention is required. This includes deformities resulting in severe functional limitations required for daily living, unstable scars leading to open wounds, exposure of vital structures, and growth and development disturbances. It is imperative to perform a detailed examination and take a complete inventory of the patient’s injuries to prioritize treatment options by first maximizing function and second improving aesthetic outcome. It is also paramount that the patient’s goals for reconstruction align with that of the surgeon and that the patient be committed to the postoperative rehabilitation process to optimize the reconstructive results. Offering a patient an aesthetic reconstruction in conjunction with a needed functional revision may help ameliorate the patient’s postoperative state of stress and help the patient to better cope with issues such as chronic pain. Primary excision, rather than serial excision, and primary closure is the optimal treatment of scar deformities that do not cause great functional impairment. Scar excision and primary closure are reserved for areas of greater skin laxity and tissue excess, and incisions should be placed parallel to relaxed skin tension lines. Scar excision can also be combined with local tissue rearrangement and skin grafting when primary closure is not feasible. Where larger surface areas are planned for resection, staged tissue expansion and scar excision may be the best option. We have used autologous fat injection after scar maturation with great success to decrease the symptoms of pruritus and scar-associated pain (Fig. 70.2). Fat grafting under a mature thermal burn scar has not been associated with any necrosis of the overlying skin in our patients, and pain and pruritus resolved in all treated patients who had a followup visit in the early postoperative period. Laser therapy has been shown to be successful in the reduction of hyperemia and edema and to accelerate the maturation of burn scars, thereby reportedly decreasing pain and the thickness of the scar. A pulsed-dye laser with a wavelength of 595 nm reduces hyperemia and edema of the scar, whereas a fractional CO2 laser with a wavelength of 10,600nm is used to correct the stiffness and texture abnormalities of thicker scars. Laser treatment of scar deformities should be delayed beyond 6 months after injury, and several treatments spaced 4 to 6 weeks apart are necessary.1 Laser therapy is especially useful for small areas of scar and in the management of older scars. Scar contractures are common postburn deformities characterized by a thickened and shortened scar that can involve the skin alone or the underlying muscle and joint space. Contractures can lead to debilitating and permanent deformities that affect the quality of life of a burn patient from both a functional and aesthetic standpoint. During acute burn wound management, the thickness of the skin graft should be tailored to the areas most prone to contracture, such as the hand and antecubital fossa. Judicious use of thicker skin grafts and postoperative splinting will minimize contraction. In addition, grafts can be inset in z-plasty fashion (e.g., web space grafts) to prevent straight-line graft margins that tend to contract with maturation. The first goal of burn contracture reconstruction is to release the contracture. This is performed by several z-plasty variations, or by making a linear incision perpendicular to the contracture band in question at the point of maximal tension. For z-plasty techniques, normal skin becomes interpolated with scarred skin to break up the scar band and facilitate stretch. For incisional releases the entire thickness of the scar is incised and sometimes excised. If the contracture is over a joint surface, stepwise release of the skin followed by the underlying fascia and musculature and finally the joint space may be necessary. The addition of fish tails at the end of the linear incision will change the shape of the resultant defect from an ellipse (Fig. 70.3a) to a rectangle (Fig. 70.3b), increasing the area of release and thereby leaving a larger defect for reconstruction. Multiple incisions along the scar contracture may be necessary depending on the anatomic location of the scar and the amount of release required. The intervening bipedicled flap that results from making adjacent lineal incisions should not be elevated to optimize the blood supply. The ultimate size of the resulting defect is difficult to predict, and this should be taken into consideration during preoperative planning because reconstructive options become limited as the size of the defect increases. Full-thickness grafts or layered grafts of dermal construct with split-thickness skin graft overlay are preferred (see Fig. 70.3). Skin grafting is the most common approach to reconstruction of a contracture release. It has the advantage of providing skin from uninjured areas of the body, rather than compromising fragile tissue immediately adjacent to the burn. The choice between split-thickness and full-thickness skin grafts depends on numerous factors. Full-thickness skin grafts increase the success of contracture release, because they contain more dermis and undergo less secondary contraction compared with split-thickness skin grafts. They are more pliable and durable and may also result in improved appearance by providing better texture and color match to the adjacent tissue. However, full-thickness skin grafts have decreased graft take and survival compared with split-thickness skin grafts and are limited in size by the availability of donor skin. Full-thickness skin grafts are usually reserved for reconstruction of scars of the face and hands and over joint surfaces.2,3 Skin grafts can also be used to reconstruct areas of hypopigmentation, replacing sheet grafts containing melanocytes over areas of hypopigmented scar. Split-thickness skin grafts are generally harvested over a thickness of 0.012 to 0.020 inch. Not only is graft survival increased with the use of thinner split-thickness skin grafts, the donor site can be harvested several times once reepithelialized. This is useful for a larger percentage total body surface area burn, but the quality of subsequent harvests and the intensity of repigmentation will be decreased. First-pass donor site harvest should be saved for aesthetic and cosmetic areas such as the hands and face. In contrast to full-thickness skin grafts, split-thickness skin grafts result in a greater recurrence of contractures requiring reoperation.3 In addition, harvesting a thicker split-thickness graft has the disadvantage of potential hypertrophic scarring of the donor site, which should be discussed in advance with the patient. After skin grafting, a pressure dressing or bolster must be applied to optimize the take of the graft. We prefer a fibrin sealant to adhere the skin graft to the recipient site and use a negative pressure dressing for 5 to 7 days postoperatively when applicable (Video 70.1). Fig. 70.4 (a) Staged closure with Integra dermal regeneration templates of full-thickness flame burns to the back of 4-year-old boy. (b) After 4 years, he has no limitations to growth or flexibility. Dermal regeneration templates such as those made by Integra are versatile tools in the reconstruction of scar contractures. Integra is a bilaminar structure. The first layer is made of cross-linked bovine collagen and chondroitin-6-sulfate, followed by an outer silicone layer. This can be advantageous in contracture reconstruction because it provides immediate coverage of large wounds without contributing to any donor site morbidity (Fig. 70.4). Once the defect is created, the silicone outer layer of Integra is left in place for several weeks to allow for dermal regeneration. This time also allows for regeneration of skin graft donor sites. After removal of the silicone layer, a thin epidermal autograft is secured to the wound. The use of this product promotes rapid dermal regeneration and can provide a cosmetic outcome and scar quality similar to that of a full-thickness skin graft (Fig. 70.5). This has been shown to provide a durable reconstruction with minimal contracture recurrence.4,5 Similar dermal constructs donated from both humans and animals are now available for similar staged reconstructive procedures. These can be especially useful when an unstable scar or a scar release exposes underlying nonvascular structures (Fig. 70.6). The use of staged dermal regeneration templates is also useful in the acute burn setting. Reports of more elastic scars with markedly less pain and pruritus have been reported. In addition, in the case of exposed bone after acute débridement, these staged procedures can preempt the need for a flap reconstruction. For a mature burn scar, these same products can be used to mimic a full-thickness skin graft using commercially available dermal templates and thinner autografts. The resulting suppleness of the scars is especially gratifying, because the donor site morbidity is often less than in the acute phase of grafting (because of the thinness [0.004 to 0.008 inches] of the harvest). Flaps provide specific advantages and options when used in postburn deformity reconstruction, particularly when compared with grafting. Flaps maintain their blood supply, provide more uniformity of matched skin quality, and can replace significant tissue deficits. Using healthy tissue allows the potential for growth and expansion of the healthy flap tissue to counter the opposing tension of the scar, thus reducing the risk of recurrent contracture. Even in locally scarred skin where blood flow to the dermis is affected, local flaps may still be used if healthy, perfused underlying subcutaneous tissue is incorporated. Linear contractures are often addressed by z-plasty. This transposition flap lengthens a scar along the common limb. Derivations using larger angles will afford greater acquisition of length. These local flaps can also be used to reapproximate displaced structures and advance scars to more conspicuous locations. Often we use successive, smaller z-plasties to achieve adequate lengthening of a scar without causing transverse shortening. Variations of the traditional z-plasty can be useful if working in a concave defect (four-flap z-plasty), or lengths of limbs can be adjusted, particularly if some surrounding tissue is mobile but some is involved in dense scar (three-quarter z-plasty). Fig. 70.5 (a) Fourth-degree flame burns of the scalp of the same child as in Fig. 70.4. (b) Result after use of Integra bilayer dermal regeneration templates and repeat split-thickness skin grafts to the central scalp over an exposed outer table of the skull. Fig. 70.6 (a) A 5-year-old girl with full-thickness scald burns to both thighs. Integra dermal regeneration templates were applied to the left thigh, and bovine dermis (PriMatrix [Integra]) was used for the right thigh. (b) Similar healing times and scar characteristics result from both dermal templates after split-thickness skin grafting. V-Y advancement flaps use lateral tissue to lengthen the scar. One must be cautious using these in burn reconstruction, because there can be significant tension once the vertical limb of the Y is closed. Regional flaps have a robust, dependable blood supply that does not abide by the length-to-width ratios dictated for the random flaps previously discussed. Fasciocutaneous or musculocutaneous flaps, depending on the degree of soft tissue bulk required, can be designed around identifiable perforators. Often these perforators lie near the scar contracture and allow for rotation of the soft tissue around this predetermined blood supply. Fig. 70.7 (a) This 10-year-old boy received a fourth-degree contact burn in a rollover lawn mower accident. (b) Early result after a split-thickness skin graft. (c) The second round of tissue expansion. Two expanders were placed each time. (d) Final hairline result, which included a whorl pattern of the hair. Free flaps are likewise designed around predictable vascular anatomy. This allows the burn surgeon to identify well-vascularized healthy tissue and transpose it to large post-burn deformities. Some even combine this technique with pre-expansion, using tissue expanders to provide additional healthy tissue. Tissue expansion has a wealth of applicability in burn reconstruction and is now being used in concert with grafting or flaps. It imparts mechanical stretch on the overlying tissue and, via the delay phenomenon, results in a large and well-vascularized flap for adjacent wound closure. A major drawback to tissue expansion is it re quires a two-stage procedure that can be both painful and socially embarrassing during the expansion process. The expander should be placed such that the expansive forces are parallel to the tensile forces generated. Several weeks must be allowed for incisions to heal before expansion is begun. Complete expansion may take several months to afford adequate amounts of vascularized tissue to be recruited to allow primary wound closure. Without careful preparation and diligent monitoring, complications (reported at nearly 15%) often require aborting the procedure (Fig. 70.7). Burn contractures of the neck are common even with prophylactic extension splinting after acute treatment. These can lead to debilitating functional deformities. At times, these scar contractures need to be addressed during the inflammatory stages of healing for improved airway access and restoration of oral competency for adequate nutritional intake. Furthermore, neck contractures exert an extrinsic force to distort facial features, thus limiting ADLs. Effects can include poor speech, drooling, and poor oral hygiene, and the resulting physical deformity can be psychosocially very stressful for the patient. Neck contracture should be addressed before facial reconstruction, because this tension serves as an extrinsic force, which can severely affect facial scar maturation. Neck contracture reconstruction involves skin grafting and the use of dermal substitutes, local flaps when available, and tissue expansion and distant or free tissue transfer. Fig. 70.8 (a) A 32-year-old man with early neck burn scar contracture after a 60% flame burn. (b) Intraoperative release of the scar with minimal excision and platysma flap release. (c) A thick split-thickness skin graft to the anterior and lateral neck releases. Contractures caused by limited scarring may be released with z-plasties alone. Larger, more diffuse scar contractures, however, once released or excised, result in large defects, making skin grafts a good solution for wound reconstruction when a donor site is available. Split-thickness skin grafts are commonly chosen over full-thickness grafts for reconstruction. When inset as two separate aesthetic subunits, one in the submental plane and one in the vertical plane, the cervicomental angle is restored, resulting in a good range of neck movement and an aesthetically pleasing contour6 (Fig. 70.8). When available, local regional flaps from the neck, shoulder, and chest, such as a deltopectoral flap, may be used for reconstruction with better color and texture match of anterior neck contractures.7 Free flaps have also been used with great success, because they have the advantage of providing pliable tissue from a donor site away from the burn injury with minimal donor site morbidity. This has resulted in good neck mobility and contour without the need for prolonged postoperative splinting and with a low contracture recurrence rate8 (Fig. 70.9). Fig. 70.9 (a) Severe facial scars from a flame burn. (b) Radial forearm free flap reconstruction of the lower face at age 22 years. (c) Early postoperative result. (These images are provided courtesy of Dr. Peter Grossman.) Upper and lower extremities suffer most from contraction deformities after injury, especially the deeper dermal injuries that require grafting. Immediate postoperative splinting regimens in conjunction with scar massage and compression (whether from elastic wraps or custom garments) are essential to minimizing such deformities. Splinting and compression are often continued during the entire maturation phase—even if it takes 2 to 3 years to complete—to minimize subsequent reconstructions (Fig. 70.10). Axillary contracture is common, because it is challenging to maintain an abducted position during the acute phase. Contractures are described as bands that are isolated and anterior or posterior. These are addressed using local flaps followed by rigorous physical therapy. When performing flaps in this region, the surgeon must pay close attention to ensure that skin that bears hair or sweat glands is not transposed to a more conspicuous area. In more significant contractures, release of the underlying pectoralis or latissimus muscle may be necessary. Skin defects are often covered with split-thickness skin grafts, which increases the risk of recurrence of contracture. In addition, limitations on mobilization during revascularization may hinder ultimate range of motion.2,9,10
70
Burns of the Body and Extremities
Avoiding Unfavorable Results and Complications in Burn Management
Patient Selection and Timing of Postburn Scar Reconstruction
General Reconstructive Principles for Management of Postburn Deformities
Scar Excision
Fat Grafting
Laser Therapy
Management of Complications Related to Burns of the Body and Extremities
Management of Burn Scar Contractures
Scar Contracture Release
Skin Grafting
Dermal Regeneration Template
Local, Regional, and Free Flaps
Tissue Expansion
Management of Postburn Deformities of the Head and Neck
Neck
Postburn Deformities of the Upper Extremity
Axilla
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree