Chapter 14 Breast reshaping after massive weight loss, implant based
• Staging may be appropriate for extremely large or ptotic patients.
• The circumvertical approach is a powerful tool for management of the redundant skin envelope.
• Controlled management of the IMF is key to reducing the number of later revisions.
• Use of an implant can be an excellent adjunct for restoring upper pole fullness.
• Patient education regarding the complex and in some ways potentially imperfect nature of the surgical correction can aid in helping patients understand the potential need for future revisions to obtain the optimal result.
Introduction
Since its development in 1966, bariatric surgery has become an effective modality for sustained weight loss. The growth of bariatric surgery has paralleled the burgeoning obesity epidemic in the United States.1 Roux-en-Y gastric bypass has become the most effective and frequently performed means of sustained surgical weight loss, with mean weight loss at 36 months of 41 kg.2,3 Other surgical procedures include biliopancreatic diversion, adjustable gastric banding, and the creation of a gastric sleeve.4–6 Additionally, some patients are able to achieve weight loss with diet and exercise alone. Regardless of the means of weight loss, massive weight loss (MWL) is defined as weight loss of 45 kg (100 pounds) or more.7
Weight loss causes a multitude of both physiologic and anatomic changes. Severe volume loss results in skin redundancy and sagging, which can lead to issues with hygiene and the potential for infection. Song et al elegantly rated the anatomic changes that occur throughout the integumentary system after MWL.8 Additional consideration must be given to the nutritional status of MWL patients. Appropriate preoperative laboratory testing as well as consultation with a nutritionist may be advisable in these types of patients. The psychiatric changes that accompany MWL, and patient motivation for body contouring must also be considered when dealing with MWL patients.9–13
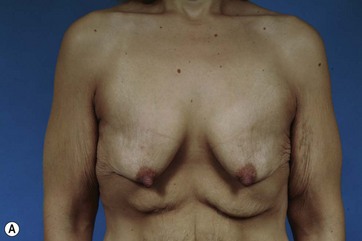
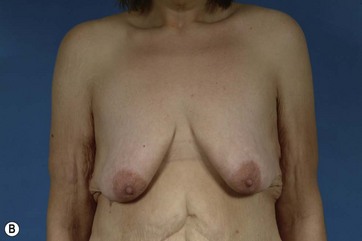
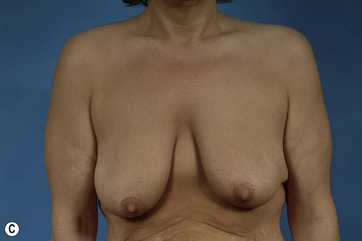
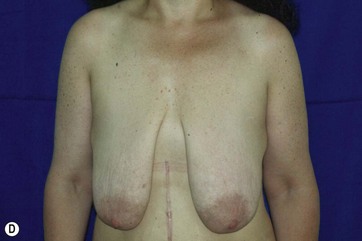
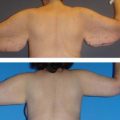
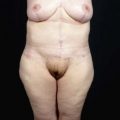
After MWL the breast undergoes a unique set of changes not typically seen in other settings. The breast becomes deflated with a paucity of upper pole tissue. Extreme ptosis of the skin envelope and the nipple can develop, along with inferior malposition of the inframammary fold (IMF). The total amount of volume loss is variable among patients. The nipple areolar complex also often becomes displaced medially. The breast mound itself can be displaced laterally and the chest wall can take on an almost barrel-shaped configuration. Additionally, the skin envelope can become inelastic14–16 (Fig. 14.1A–D). All these anatomic changes serve to make augmentation mastopexy, an already challenging procedure, even more intimidating.
Preoperative Preparation
Proper assessment of the MWL patient begins with ascertaining the method of weight loss. If the patient lost weight through surgical means then determining whether the procedure was restrictive, diversionary or both allows the surgeon to determine what nutritional workup is necessary. Timing of the bariatric procedure and the starting weight at the time of surgery, the amount of weight loss since the procedure, the weight change in the past 3–6 months, and how long the patient has been at the current weight should all be ascertained. Generally, the patient should be at a stable goal weight for 3–6 months or more prior to any plastic surgical procedure. This usually occurs 12–18 months following the weight loss surgery.17
Preoperative assessment of the MWL patient must include a full evaluation of the patient’s nutritional status. This is especially important in patients who have undergone diversionary procedures, and to a lesser extent those undergoing restrictive procedures. MWL patients that were able to lose weight through diet and exercise generally have adequate nutrition and do not need supplementation. Whether or not supplemental Vitamin B12, iron, calcium, and/or multivitamins are being used should be noted, as deficiencies here can lead to altered wound healing. Baseline laboratory values should consist of a complete blood count, electrolytes, prothrombin/partial thromboplastin time, and albumin levels.7 Micronutrients may also need to be assessed in selected cases of possible malnutrition.18–20
Discussion of potential need for revision at the initial consultation helps mitigate some of the later issues that may arise when enhancements of the initial procedure are needed. Meticulous documentation of conversations regarding revisions is also important during the initial visit. Informing patients that scar length is commensurate with the amount of soft tissue resection allows the patient insight into the outcomes of the procedure. Additionally, discussion of recurrent ptosis, or the possibility of breast asymmetry is important in the augmentation mastopexy patient.14 Nipple viability and potential nipple loss must be part included as a potential risk during augmentation mastopexy. Establishing realistic expectations and goals for surgical outcome is an important part of a successful augmentation mastopexy procedure.
Preoperative Planning – Primary Augmentation Mammaplasty
< div class='tao-gold-member'>
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree