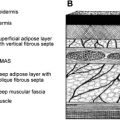
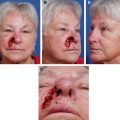
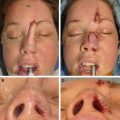
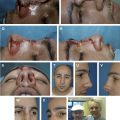
The bilobed flap is a local transposition flap useful for the repair of nasal defects commonly seen after Mohs surgery. The bilobed flap has benefits over other nasal transposition or advancement flaps because it distributes wound closure tension over a larger surface area through the use of 2 lobes. This property is especially helpful for defects of the caudal portion of the nose, where the skin is less elastic. This article discusses the bilobed flap for nasal reconstruction along with the appropriate selection, design, and placement of the flap and the potential complications.
Bilobed flaps are local flaps useful for the reconstruction of nasal defects. These flaps are especially useful for defects of the caudal portion of the nose. Defects in this region pose a reconstructive challenge because the skin is thick, sebaceous, and lacks elasticity. Significant advancement, rotation, or transposition in this area can result in distortion of the nasal tip.
The bilobed flap is a double transposition flap whose basic principle relies on transposing mobile skin from the cephalic portion of the nose in order to close defects of the thicker immobile skin of the caudal portion of the nose. This double transposition flap distributes tension over an area greater than a single transposition, allowing for successful closure of defects in the inelastic skin of the nose.
The bilobed flap for nasal reconstruction was first described by the Dutch surgeon Esser in the early twentieth century. He described a total transposition arc of greater than 180°. The large degree of rotation created large lobes that required the flap to extend into the glabella, resulting in significant standing cutaneous deformities. Later in the twentieth century, McGregor and Soutar discussed the use of the bilobed flap with smaller pivotal arcs, which resulted in smaller standing cutaneous deformities and decreased pincushioning. Zitelli’s modification of the bilobed flap emphasized a total pivotal arc no greater than 90° to 110°, with an approximately 45° pivotal arc between each lobe. His results demonstrated the practical utility of this flap in nasal reconstruction.
Flap selection
Bilobed flaps are ideal for defects of the central or lateral nasal tip that range up to 1.5 cm in size. These flaps are best suited in the distal third of the nose, where most other skin flaps would cause significant distortion of the nasal tip. Defects that extend onto the nasal ala are generally not favorable for this type of repair because of a high likelihood for alar retraction. The defect should be at least 0.5 cm away from the nostril-free margin in order to reduce the risk of notching.
Bilobed flaps may also be used to repair more cephalically positioned nasal defects; however, size limitations exist as the donor site of the second lobe moves cephalad. In these cases, the second lobe donor site would be located at the medial canthus or glabella and donor site closure may lead to distortion of these structures, compromising the overall aesthetic and functional reconstructive outcomes. In these locations, alternative flap selection may lead to a more desirable outcome.
Bilobed flaps are especially advantageous for defects whose depth extends into and past the level of the subcutaneous fat, which is the main benefit of the bilobed flap over skin grafts when considering reconstruction of the nasal tip. Skin grafts placed over deeper defects often results in visible depressions over the nose and a less-than desirable aesthetic result. The depth of the nasal defect often dictates the use of a bilobed flap over a skin graft in this area.
Flap design
Bilobed flaps are classified as random flaps whose blood supply originates at the base of the flap. The flap is most commonly based laterally, on the nasal sidewall, where there is a robust arterial supply to the nose. However, medially based flaps can also be placed successfully, if necessary, with little risk of flap necrosis. The high vascularity of this region makes the blood supply to the bilobed flap robust and provides for a high success rate of flap viability.
The design of the bilobed flap is based on a geometrically configured pattern that spans a 90° pivotal arc. The first step in the proper design of this flap is to mark the 2 arcsthat will define the boundaries of the flap and its proper angulations. In order to do so, the radius and diameter of the nasal defect are measured with calipers. A pivot point is selected 1 radius from the free edge of the defect and is placed in the region from where the standing cutaneous cone has to be removed. This pivot point is most commonly placed within the alar groove. A marking pen is used to mark the pivot point over which the arcs are based.
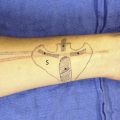
A suture is then passed full thickness through the nose at the pivot point, and a knot is placed within the suture itself to anchor it into position at the nasal vestibule ( Fig. 1 A). Next, the suture is marked at the center of the defect with a hemostat. The hemostat is then pivoted cephalad in a 120° rotation, using a marking pen at the level of the hemostat to draw the first arc (see Fig. 1 B). The second arc is then configured by repositioning the hemostat at the center of the defect’s distal edge (see Fig. 1 C) and marking out the resultant arc using a similar 120° rotation (see Fig. 1 D). Alternatively, a standard geometry compass can be used to perform these markings.
Once the 2 arcs are properly drawn, the 2 lobes of the flap are configured. The thick skin of the nasal tip has minimal elasticity and does not allow for significant advancement without distortion. Unlike bilobed flaps in the rest of the face and body, the first lobe of a nasal bilobed flap should have the same diameter as the defect itself (see Fig. 1 E). The first side of the first lobe is drawn as a perpendicular line between the 2 arcs, 45° away from the defect. The second side of the first lobe is then drawn parallel to this line, 1 diameter away from the first side. The first side of the second lobe is then marked, 45° away from the adjacent lobe. A line marking this side of the second lobe is then drawn. The second lobe is then marked out to be similar or slightly smaller then the nasal defect (see Fig. 1 F), which will depend on the elasticity of the skin in this region and can be judged by pinching the skin of the lateral nasal wall. Once again, the final side of the second lobe is marked, extending the planned incision past the arcs in order to allow for the excision of an additional triangle of skin for adequate donor site closure (see Fig. 1 G).
When designing a bilobed flap, the standing cutaneous cone excision, at the base of the defect, is taken into consideration and preferably placed within the alar crease. The apex of the cone is positioned at the pivot point that was previously marked. However, one should not be too conservative as to the amount of skin to remove because small dog-ears in this area do not settle out well. A disadvantage of the bilobed flap is the amount of incision necessary, which cannot be placed within the relaxed skin tension lines. Despite this, incisions of the nose heal well when meticulously closed in layers.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree