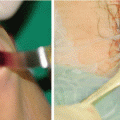
Fig. 22.1
An example of unfavorable results after standard reduction malarplasty using L-shaped osteotomy. This patient with prominent cheekbones and up-slanted eyes underwent reduction malarplasty using standard L-shaped osteotomy. Although malar prominence was effectively reduced from the three-quarter oblique view, she complained that she still had a wide margin below the eyes from the front view. Thus, she wanted to have a further surgery, a lowering lateral canthoplasty, to attain a softer image as a separate procedure
There are two main reasons. One is because much attention on the contouring procedure has focused on the position of the zygomatic body and arch. As a result, periorbital appearance including mongoloid slant of palpebral fissure and the protrusion of the orbital rim as well as cheek soft tissues are often overlooked or ignored. Therefore, remaining up-slanted eyes leaves a wide margin below the eyes and become obvious among their high cheekbones, especially when smiling. Although prominent high cheek bones with the superolateral orientation of the brow and the mongoloid slant of the palpebral fissure are regarded as attractive and youthful by Western standards of beauty, they are not by Asians as it gives a strong and aggressive impression. Thus, recently, to attain a more attractive and smooth midfacial contour, lowering lateral canthoplasty are widely performed with reduction malarplasty as well among Asians.
However, the author believes that there are several advantages of combining the two operations in one sitting. One is the periorbital approach for canthoplasty enables us to reduce the remaining protruding inferolateral orbital rim, which will help refine the contour of the periorbital region including the upper zygomatic body. Another advantage is that reversion of mongoloid slant reduces the wide margin below the eyes and makes their high cheekbones less conspicuous (Fig. 22.2).
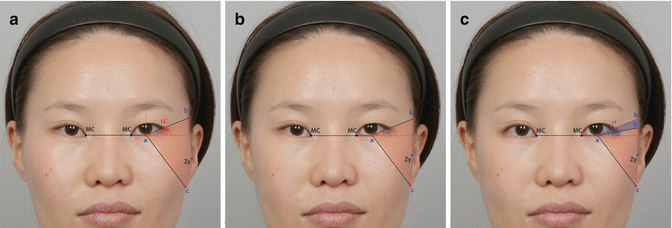

Fig. 22.2
Simulating the lowering lateral canthoplasty after reduction malarplasty. This simulation can demonstrate how vertical lowering and horizontal expanding of the lateral canthus make the high cheek bone less conspicuous by reducing the surface below eyes. 9.2% of malar surface area (a-b′-c) is decreased more than that of reduction malarplasty alone (a-b-c). Through virtual plastic surgery, we can verify the effectiveness of the combination of zyR and LLC. Also it shows the patients the potential changes that might occur
Abundant soft tissue and thick skin frequently causes cheek drooping and exaggeration of the nasolabial fold. Descent of midcheek fat and skin causes jowls to develop [1–3]. Many procedures from the least invasive laser rejuvenation to the most invasive conventional face lift surgery are available to correct soft tissue sagging. However, patients who undergo reduction malarplasty are usually young [4–6]. Thus, we prefer thread lift using elastic thread (Elasticum®, Korpo SRL, Genova, Italy) despite of its limitations.
Patient Consultation and Assessment
Preoperative Evaluation
Patient’s photographic documentation and radiologic examination that includes zygomatic arch view and three-dimensional computed tomographic image are routinely obtained. A comprehensive evaluation of the entire midface including malar prominence, infraorbital rim protrusion, globe-orbital rim relationships, lateral canthal angle, and overlying soft tissues is essential to determine the combination of the procedures needed.
Preoperatively, the patient’s periorbital appearance including lateral canthal slant and inferolateral orbital rim projection is thoroughly examined and discussed in sitting position and in order to determine how much lower the lateral canthus vertically and lengthen the palpebral fissure horizontally. The degree and location of external orbital rim prominence should be evaluated through three-quarter oblique view of the 3D CT to determine how much reduction of the rim by shaving method. Especially, in case of enophthalmic eyes with well-developed orbital rim, it should be reduced more than expected.
The lower lid itself should also be examined for laxity. A preoperative snap-back test and measuring intraoperative lid distraction are useful indicators of lower lid tone. This information can then be used to determine if a canthopexy vs. canthoplasty would be beneficial in restoring lower lid support and preventing postoperative complications related to lid malposition. Similarly, the degree of eye proptosis should also be noted prior to surgery, as this can influence optimal placement of the canthal anchoring suture. In particular, patients with slightly protruding eyes, lateral canthal suture should be placed superiorly to prevent for scleral show.
Patient Selection
Lowering Lateral Canthoplasty (LLC)
The main inclusion criteria were the presence of zygomatic prominence with up-slanted eyes. The exclusion criteria were acute or chronic sinus infection and lack of permeability of the osteomeatal complex. Also, the cases with a small eyeball surrounded by a prominent lateral orbital rim (enophthalmic eyes with well-developed orbital rim) were excluded as the lowering lateral canthopexy (LLC) may be less effective and may keep the lower lid away from the eyeball. In particular, patients with very protruding eyes ought to be excluded for fear of scleral show.
Simultaneous reduction of inferolateral orbital rim may be indicated in selected patients.
Cheek Lifting Procedure
After assessment of the patients’ age, volume of fat and skin elasticity in an upright sitting position, the high-risk groups for skin and soft tissue sagging are selected as follows: (1) age over 40, (2) abundant cheek fat, and (3) thin skin and skin laxity. This is evaluated before the surgery because once the patient lies on a bed, soft tissue distribution is changed. Then, fat removal area, soft tissue sagging area, and lifting design are marked on the patient’s face.
Surgical Technique
Lowering Lateral Canthoplasty Combined with Zygomatic Reduction
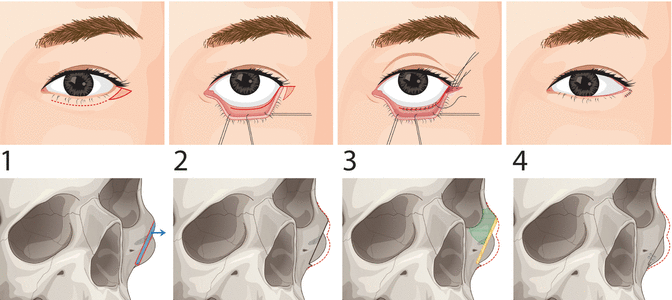
This LLC-Zy contouring procedure involves two, and sometimes three, basic maneuvers, which includes bone sculpturing along with high L-shaped osteotomy, inferolateral orbital rim shaving, if necessary, and, finally, repositioning of lateral canthus (Figs. 22.3 and 22.4). Under general anesthesia, with the patient in neck-extended supine position, the patient’s zygomatic contour was designed. Two possible periorbital approaches are used depending on (1) whether the redundant skin of the lower eyelid needs to be excised or (2) the tendency of entropion. When excision of the lower eyelid skin is required or when ectropion is anticipated after LLC, the subciliary incision is useful. The transconjunctival approach allows for better scar camouflage. A continuous oblique canthotomy incision starting is made from the lateral canthus and extending laterally and inferiorly according to the slope between the lateral part of the upper eyelid and the lateral canthus. The length of the incision is usually 3–4 mm. Then dissection is carried out through preseptal space toward infraorbital rim. It is important to identify the infraorbital nerve and the zygomaticofacial nerve. Of these, the infraorbital nerve should be protected. However, the zygomaticofacial nerve might be sacrificed inevitably to allow the medial oblique osteotomy to be placed close to external orbital rim. When combined with LLC procedures, this high-L osteotomy is a preferred method. The main difference of this technique with conventional L-shaped osteotomy is in the oblique part of the osteotomy line; the oblique line is moved more toward the external orbital rims in comparison with the L-shaped osteotomy, in which medial oblique osteotomy is placed lateral to the zygomaticofacial nerve foramen to avoid the injury. Reduction malarplasty is done in the same way. The lower lid and midface soft tissues are freed by subperiosteal dissection (area of dissection shown in green). It is important to eliminate any possible interference and inspect the transition zones, paying special attention to avoid any periorbital soft tissue injury.