Key points
• Chin augmentation can often result in asymmetry, an irregular transition between the implant and the underlying bone, excessive width, or unaesthetic disproportion.
• Optimization of results requires careful preoperative analysis, refinements in surgical technique, and appropriate implant design.
• With 3D CT imaging and/or models, bone irregularities, deficiencies, asymmetries, any prior implant, and the soft tissue envelope can be visualized.
• Many patients benefit from defatting the submental area. Precise defatting improves neck contour and improves mandibular border definition.
• We prefer a two-piece implant because segmentation facilitates placement of the relatively long and stiff, porous implant.
• Screw fixation ensures implant position and obliterates any gaps between the implant and the underlying skeleton that would result in unintended increases in implant projection.
• Chin and mandible augmentation can inadvertently lead to masculinization of a female.
• Chin implants can create vertical lengthening up to 2mm, additional lengthening may look contrived and a lengthening genioplasty is preferred.
• Implants that augment only the chin point produce an abrupt, protruding chin rather than a jaw–chin continuum resulting in an unnatural chin contour.
Introduction
Chin augmentation is the most frequently performed facial implant surgery. Although considered a simple procedure by many, chin augmentation can often result in asymmetry, an irregular transition between the implant and the underlying bone, excessive width, or unaesthetic disproportion. Any of these complications can negatively impact the skeletal structures of the lower facial third and the overlying soft tissue.
Mandible augmentation can benefit three groups of patients: those with normal, deficient, or surgically altered anatomy. Implants can be placed on the mandibular body, angle, or ramus giving the surgeon the ability to change the shape of the mandible or alter the vertical and horizontal dimensions.
Optimization of results requires careful preoperative analysis, refinements in surgical technique, and appropriate implant design.
Patient evaluation
History
It is most important to elucidate and understand the patient’s desires and goals. Occlusal status, history of orthodontics, orthognathic surgery, or prior chin augmentation should be documented. If a previous chin implant has been placed, it is important to know the material of the implant. It is also important to inquire if the patient snores or has a suspected sleep disorder.
Differential diagnosis
The patient who presents for a chin implant frequently exhibits retrognathia, a risk factor for obstructive sleep apnea. If a sleep disorder is suspected, a full evaluation should be undertaken. If the study reveals obstructive sleep apnea, the patient should be counseled on the use of continued positive airway pressure (CPAP) versus orthognathic surgery. The presence of sleep apnea does not preclude the placement of a chin implant if the use of CPAP will effectively manage the airway obstruction, but it is imperative that alternative treatment approaches, such as CPAP and orthognathic surgery, be discussed with the patient.
Physical examination
Physical examination should include analysis of the skeleton and its soft tissue envelope and how the lower one third of the face relates to the upper two thirds of the face.
Sagittal projection
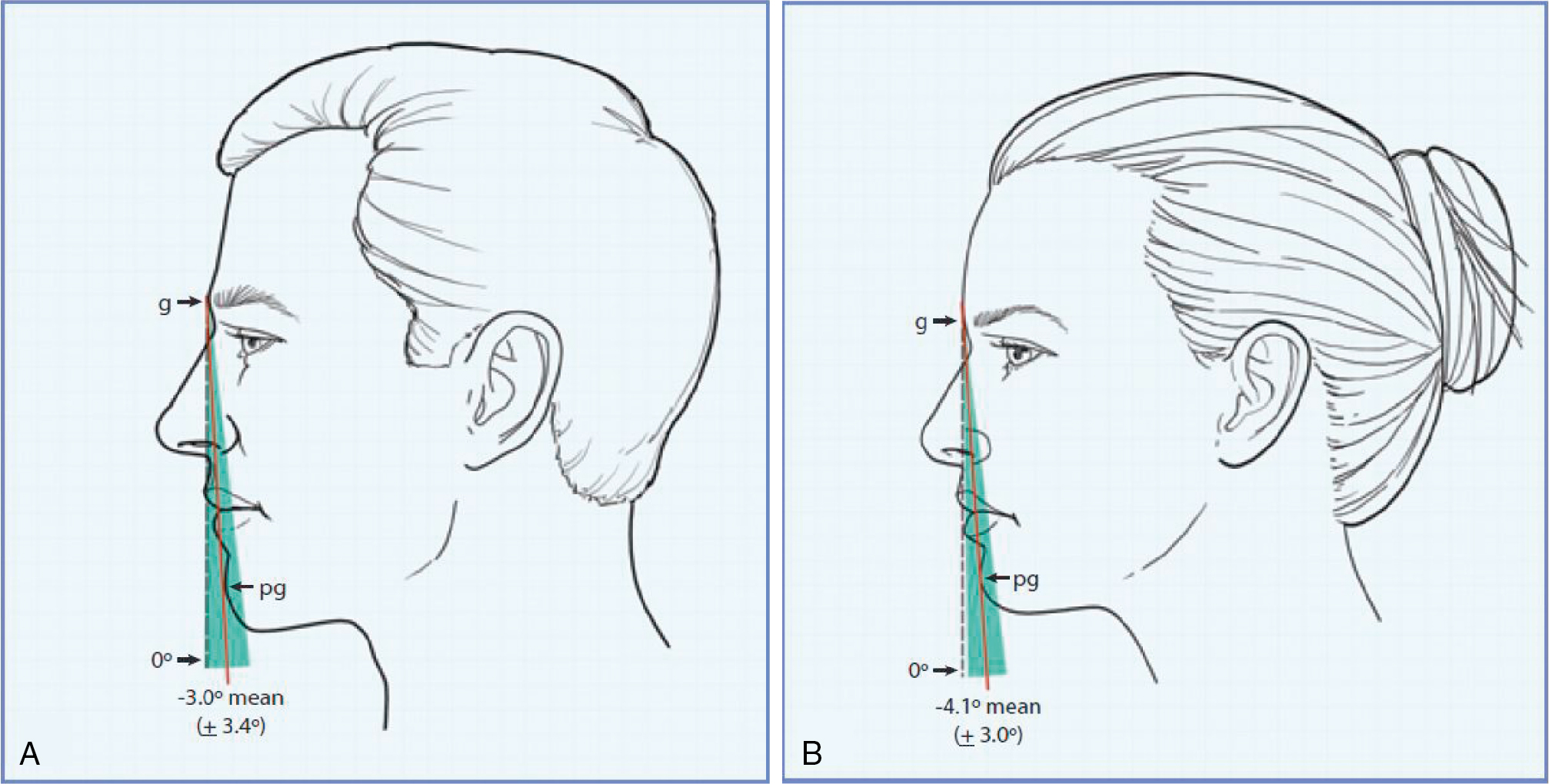
The mean inclination of the facial profile as defined by a line from the glabella to the pogonion was −3 ± 3.4 degrees in men and −4.1 ± 3.0 degrees in women ( Fig. 26.1 ). This demonstrates that the “normative” position of the female chin is, not surprisingly, less than that of the male chin, but that augmenting the chin too aggressively can lead to defeminization in a female.
The ideal relationship between the chin and the lips should be considered when evaluating a patient for a chin implant. The lower lip should lie slightly posterior to the upper lip and the chin slightly posterior to the lower lip.
The labiomental angle must also be considered when placing a chin implant. In general, the inclination is more acute in men (113 degrees ± 21 degrees) than it is in women (121 ± 14 degrees). With placement of an implant, this can result in a more acute angle and deepening of the labiomental sulcus. Because this can be dysaesthetic, this potential change should be discussed with patients preoperatively.
Vertical projection
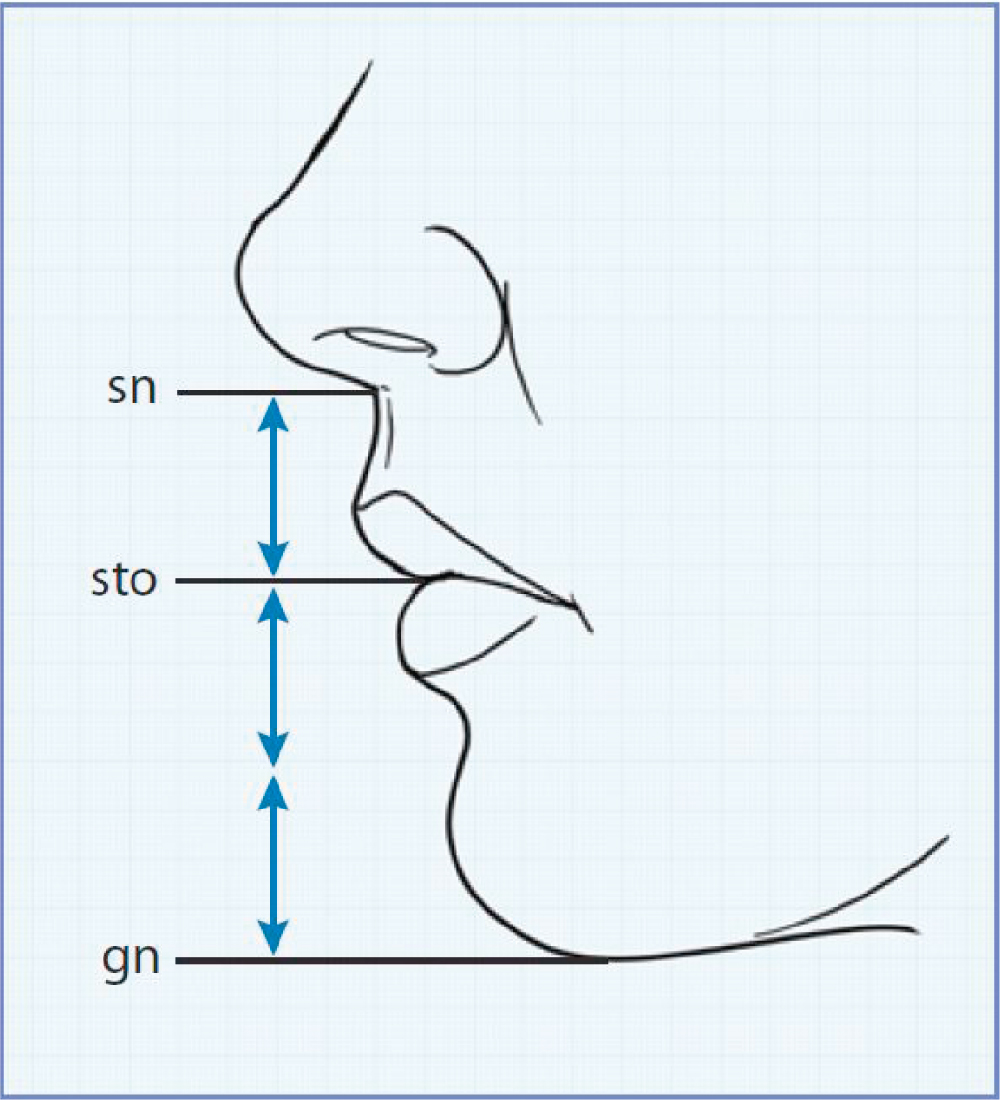
On average, the subnasion (sn) to the stomion (sto) is one third of the distance from the sn to the gnathion (gn) ( Fig. 26.2 ). The height of the mandible should account for two thirds of the lower face height (sn–gn). Increases in vertical height require computer-aided design/computer-aided manufacturing (CAD/CAM) implants or horizontal osteotomy.
Horizontal projection (chin width)
The width of the chin should be proportional to the vertical height and the patient’s upper face. To prevent a step-off between the implant and the mandible, an extended chin implant can be used. However, one must take care to narrow the implant, especially in women, so as to not masculinize the lower face.
Imaging
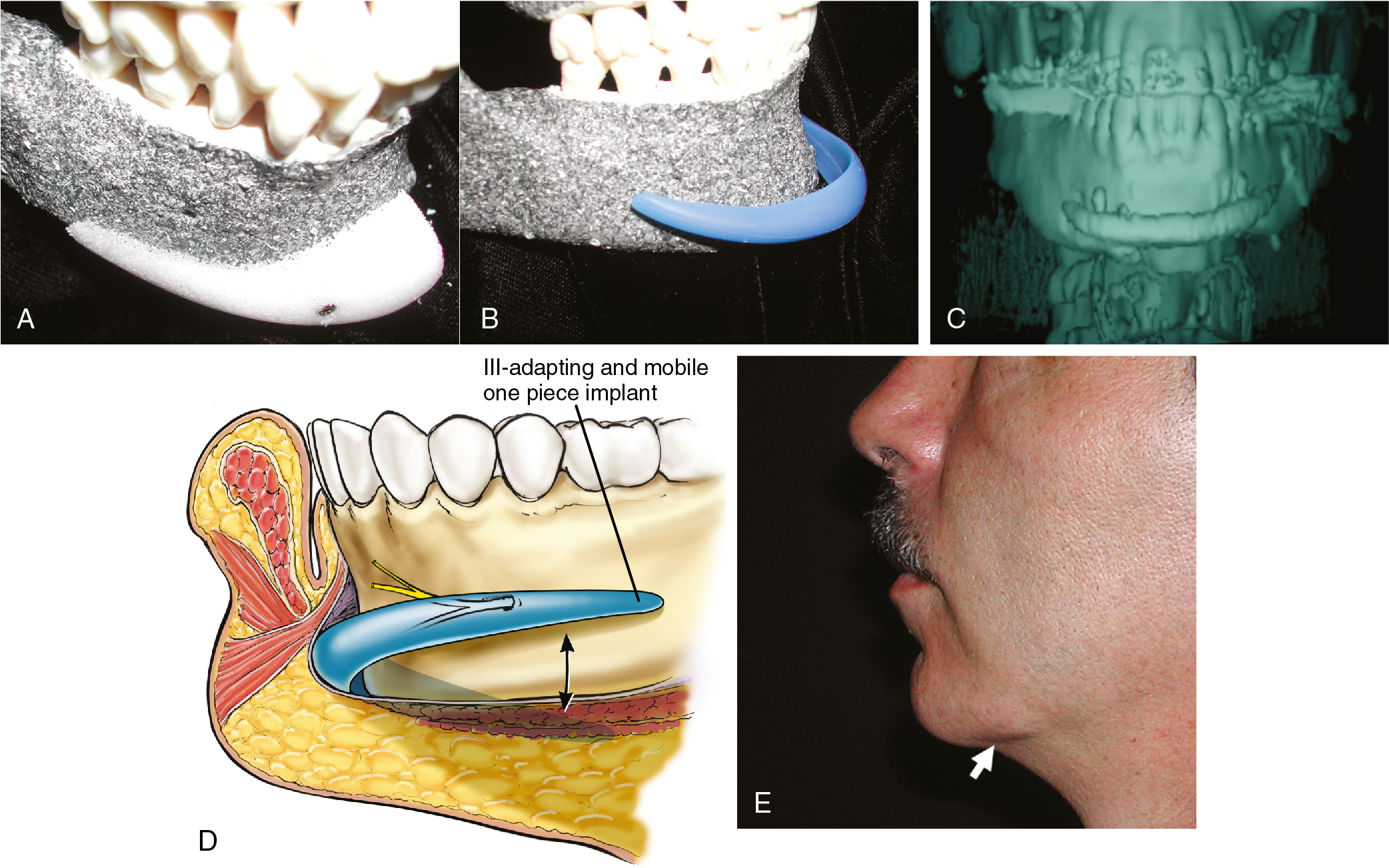
Most facial implant surgery is done without radiographic evaluation. Posteroanterior (PA) and lateral cephalograms can be helpful in understanding the underlying bone structure and how the dimensions of the implant might be altered to best suit the patient. The authors believe that three-dimensional computed tomography (3D CT) is invaluable. With 3D CT, bone irregularities, deficiencies, asymmetries, any prior implant, and the soft tissue envelope can be visualized. Because noncustom implants are based on normative anatomic data, it may be useful to print a 3D model from the CT data if there is any uncertainty regarding abnormal mandibular anatomy and implant fit. Patients who benefit from this are those who have undergone previous surgery on the mandible or chin and now seek further augmentation with implants. Recent advances in 3D printing have allowed the surgeon to obtain 3D printed models at a reasonable cost.
Indications/contraindications
Patients who have realistic expectations of what alloplastic augmentation of the chin and jaw may achieve are good surgical candidates. In mandibular deficiency, when occlusion cannot be normalized through orthodontics alone, patients should be informed of the advantages of orthognathic surgery; however, if these patients decline and still desire augmentation of the chin, an implant can be placed. A patient whose sleep apnea cannot be successfully managed with CPAP is also a candidate for orthognathic surgery rather than a chin implant.
Preoperative planning
Chin augmentation
Effective preoperative planning requires understanding of the patient’s desires, recognition of the impact of previous facial surgery or orthodontic treatment on the patient’s appearance, and careful facial examination. When chin augmentation is considered an adjunct to rhinoplasty or neck rejuvenation, the preoperative analysis should be as rigorous as it is when chin deficiency alone is the presenting complaint.
Normative data are helpful in analyzing the chin in the sagittal, vertical, and horizontal projections. These dimensions and the potential changes with chin augmentation should be considered in the context of lip projection and deepening of the labiomental angle.
Mandible augmentation
Patients who desire mandible augmentation perceive a wider and more sculpted lower face as desirable. In these patients, usually males, implants can be designed to augment the ramus and posterior body of the mandible, thus increasing the bigonial distance. Patients who desire more angularity and definition can have implants designed to augment the anterior mandible back to the ramus.
Another subset of patients that can benefit from mandibular augmentation often has skeletal deficiencies resulting in a class II relation. In patients who have mandibular deficiencies and have already had orthodontic therapy to normalize the occlusion, alloplastic augmentation can offer an effect similar to that by sagittal osteotomy while avoiding further dental manipulation. ,
The last subset of patients includes those who have already had their class II malocclusion corrected with sagittal split osteotomy and advancement of the distal segment. This ultimately results in a contour irregularity at the site of the body osteotomy, which is always palpable and often visible and disfiguring to some individuals. In these patients, mandibular implants can be designed to improve the jaw line contour. ,
Implant selection
The most frequently used materials for facial implants are silicone and porous polyethylene. The goal of surgery is to create chin and mandibular contours in line with the aesthetic goals of the patient. Both have advantages and disadvantages related to their surface characteristics. Porous polyethylene implants can be carved easily and can be fixed with screws. The porosity allows some soft tissue ingrowth making capsule formation less problematic. Tissue ingrowth makes the implants more difficult to remove. The smooth surface of silicone allows easier placement and removal. The smooth surface also makes capsule formation more vigorous.
Primary operative approach
After a 3D analysis of the patient, a mutual decision is made on whether to place chin, mandible, or both types of implants to achieve the patient’s desired goals.
The preoperative physical examination should aid the surgeon in determining the dimensions of implant that will successfully meet the patient’s expectations.
Alternative approaches
Osseous genioplasty
Osseous genioplasty is an alternative technique for enhancing chin projection. Because it mobilizes the chin, it allows for a 3D change in position.
Dermal fillers
Fillers may be useful to add 1 to 3 mm of chin projection, but beyond 3 mm, they may produce a ptotic mobile chin pad anterior to the mentalis muscle. The chin is a bony structure with a uniform amount of soft tissue draping the bone, and when an excessive degree of filler is injected in an attempt to create chin projection, the aesthetic result may be compromised.
Autologous fat grafting
Similar to dermal fillers, fat may create an unnatural appearance when used to replace insufficient skeletal projection. Additionally, fat grafting may be less forgiving in the chin compared with dermal fillers and result in visible contour irregularities.
Optimizing outcomes
Photographic imaging
Taking photographs of the patient in standard AP, lateral, three quarter profile, worm’s eye, and bird’s eye views and reviewing them with the patient is key during the consultation. Often, patients are unaware of their lateral profiles, and reviewing photographs with them can be instrumental during the discussion of the patients’ goals. It can also be helpful to have patients bring in photographs of chins and jawlines that they find ideal. 3D imaging is also invaluable in showing the patient what the likely effects of various types of implant placement would be. As surgeons gain experience in placing implants and assessing the outcomes, they will become more adept at accurately morphing the patient’s expected outcome.
Predicting the soft tissue response to skeletal augmentation
The soft tissue response to alloplastic augmentation of the chin is slightly less than 1:1. One would anticipate variations in the soft tissue response because of the variability in the thickness of the chin soft tissue envelope. The thicker the overlying soft tissue envelope, the less is its surface response to the underlying skeletal augmentation. The thickness in the soft tissue envelope overlying the chin varies within the individual, varies between individuals for any given area, and is usually thicker in males than in females.
Submental lipectomy
Many patients benefit from defatting the submental area. Precise defatting improves neck contour and improves mandibular border definition. Our preference is to use the submental incision to create a full-thickness skin and subcutaneous flap by dissecting directly on the platysma. The fat is trimmed from the full-thickness flap with scissors. The wound is closed in layers and a mildly compressive dressing applied.
Defatting could also be done with liposuction. We prefer excision under direct observation because it avoids irregularities and possible overresection, which, in our experience, is more possible with liposuction.
Unless the patient is obese, fat is rarely removed from beneath the platysma or strap muscles. Over resecting fat can create a submental depression that will be disfiguring.
Realistic expectations
During the consultation, the role of each patient’s individual and unique bone structure and soft tissue envelope that will affect the ultimate outcome should be discussed. It is important to explain that the goal will be to bring the patient toward the direction of his or her ideal aesthetic goal but cannot replicate the look in the photos brought by the patient, even with custom-designed implants.
Chin implant selection
We prefer a two-piece implant because segmentation facilitates placement of the relatively long and stiff, porous implant. The two-piece design also provides flexibility in positioning the lateral extensions of the implants, ensuring that it mimics the inclination of the patient’s mandibular body ( Fig. 26.3 A).
A one-piece implant, particularly one with lateral extensions, is unlikely to have the arc, projection, and inclination appropriate for every mandible ( Fig. 26.3 B). A two-piece design allows for adaptation of each of these parameters for a given mandible. When placed through the submental approach, the two-piece implant limits asymmetry in the horizontal plane. With one-piece implants, asymmetry in horizontal positioning increases as one proceeds laterally. It is not uncommon to find one end of an extended silicone implant impinging on the mental nerve, while the other end extends beyond the edge of the mandibular border ( Fig. 26.3 C).