Acne Scars
8.4.i
Atrophic Acne Scars
Atrophic Acne Scars
Karina C. Furlan
Brian W. Petersen
Murad Alam
BACKGROUND
Acne is an exceedingly common condition, with the vast majority adolescents impacted to some degree at some point in their lives.1 Although the time of onset is typically in the teen years, coincident with puberty, patients may have acne for the first time later in adulthood, with this particularly notable in women.2,3 Inflammatory lesions of acne can be painful. Moreover, the psychosocial impact of acne on individual patients can be immense, with the associated perceived disfigurement of active acne resulting in self-consciousness and depression in adolescents and the associated scarring further exacerbating these effects. Atrophic scars, the most common type of acne scars,4,5 can have a profound impact on self-image, lead to self-imposed social isolation, and otherwise impair the process of normal socialization during late childhood and early adulthood. Affected patients are literally “scarred for life.”
PRESENTATION
Patients may present as early as adolescence or in adulthood with a complaint of scars associated with a history of acne. Scars may present with various lesion morphologies, and the distribution is usually on the face but may involve the torso or extremities.
DIAGNOSIS
Clinical Diagnosis
Scarring emerges as a sequela of healing as lesions of active acne involute. There is individual variation, as acne
can heal with little scarring in some and in others scarring is more extensive. Acne scars can be atrophic, meaning there is a site-specific decrease in collagen and other cellular structures, or they can be hypertrophic, with an excess deposition of collagen. More than three-quarters of acne scars are of the atrophic type. Indeed, it is estimated that there are three times as many atrophic acne scars as all keloids and hypertrophic scars from all causes combined.6
can heal with little scarring in some and in others scarring is more extensive. Acne scars can be atrophic, meaning there is a site-specific decrease in collagen and other cellular structures, or they can be hypertrophic, with an excess deposition of collagen. More than three-quarters of acne scars are of the atrophic type. Indeed, it is estimated that there are three times as many atrophic acne scars as all keloids and hypertrophic scars from all causes combined.6
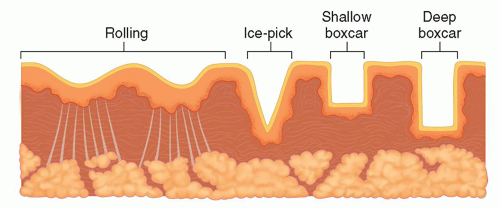
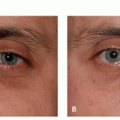
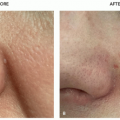
The nosology of atrophic acne scars has been much studied. A variety of classification systems have been developed to sort scars based on morphology and also to assess the overall extent of atrophic acne scarring in a particular patient. Some of the more complex methods are too laborious for routine clinical assessment and likely better suited for research. The scheme popularized in clinical practice differentiates atrophic acne scars into 3 primary categories: (1) ice pick, (2) rolling, and (3) boxcar scars (Figure 8.4.i.1; see also the section “Subtypes”). Based on one estimate, the relative proportion in the population is 60% to 70% ice pick, 20% to 30% boxcar, and 15% to 25% rolling scars.7
Most patients will have a mix of scar types.4,7 Anatomic areas at greatest risk for atrophic scars include those with densely spaced sebaceous glands. In addition to the face, the back and chest are often affected. Prompt treatment of active acne can prevent or reduce the extent to which inflammatory lesions culminate in scars.8
Histopathology
On histology, atrophic acne scars are notable for thin and long fibroblasts with a low cytoplasm to nuclear ratio and a paucity of organelles. Elastic fibers are remarkable for their sporadic deposition in the elastic microfilaments of the dermis centered on a morphologically normal hair follicle.9,10
Subtypes
Ice Pick Scars
These are minute at the skin surface (ie, 2 mm or less), penetrating, and often quite deep, up to several millimeters. Such scars tend to be funnel shaped, wider at the aperture than at the base.6
Rolling Scars
The skin associated with such scars is gently undulating, like hills and valleys, without sharp edges as with ice pick or boxcar scars. It is postulated that fibrous tethers in the deeper dermis are responsible for pulling down and securing the “valleys” in rolling scars. Rolling scars are generally broad, from several millimeters to over a centimeter wide.6
Boxcar Scars
These round, ellipsoid, or rectangular scars have vertical walls that descend to a flat floor. They are named after the rectangular containers on a train that carry cargo rather than people. In contradistinction to ice pick scars, these are often relatively wide at the skin surface and the aperture and the base are the same size. Boxcar scars can be subcategorized as shallow or deep.6
Differential Diagnosis
Pox scars
Traumatic scars
Elastolysis
PATHOGENESIS
The pathogenesis of acne is multifactorial, and important contributors are elevated sebum levels, anomalies in the composition of sebum, heightened androgenic hormonal influences, follicular colonization by Propionibacterium acnes, and impaired follicular differentiation resulting in hyperkeratinization.11 The induction of 5-lipoxygenase and cyclooxygenase-2 in sebaceous glands causes production of proinflammatory lipids.12,13 Keratinocytes and sebocytes are stimulated to become more active by the presence of P acnes.14 Monocytes and macrophages in the pilosebaceous units cause the production and release
of various cytokines and chemokines, including interleukin (IL)-8 and IL-12.15
of various cytokines and chemokines, including interleukin (IL)-8 and IL-12.15
There is a 3-stage process by which an acne lesion results in a scar. Specifically, inflammation is followed by granulation tissue formation and matrix remodeling. In inflammation, an initial vasoconstrictive stimulus is followed by vasodilatation, which manifests as erythema. This erythema, in turn, can result in the erythema and hyperpigmentation routinely seen after resolution of active acne.16 Based on the assessment of histological specimens, Holland et al. determined that the inflammatory process at the sebaceous glands was stronger and slower in patients with acne who tended to develop scars, as compared with those whose acne resolved without scarring. The presumptive conclusion was that early treatment and hence abbreviation of the inflammatory phase in acne may reduce the risk of scarring.17 The formation of granulation tissue, which includes new capillaries as well as new collagen deposition by fibroblasts, is initiated several days after the inflammatory reaction associated with an acne lesion. The early preponderance of type III collagen changes in the mature scar to approximately 80% type I collagen.18 Thereafter, the activity of fibroblasts and keratinocytes activate enzymes that modify the extracellular matrix metalloproteinases (MMPs) and result in tissue remodeling.19 The specific type of MMP activity determines whether atrophic or hypertrophic scars are formed. Lesser activity results in diminished collagen formation and an atrophic scar, and an excessively intense response gives rise to an exophytic growth of fibrotic tissue, or a hypertrophic scar.20
TREATMENT
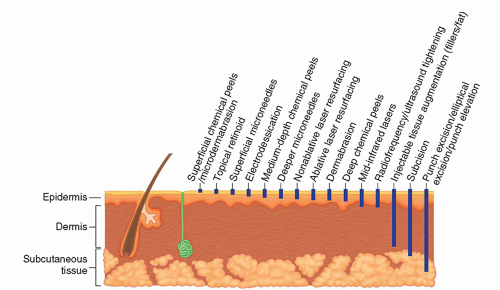
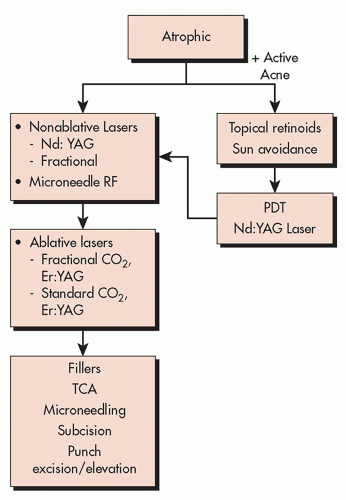
The management of acne scarring can be medical, cosmetic, or surgical. Surgical or procedural management may include excision or incision, minimally invasive tissue augmentation or reduction, and resurfacing by various modalities, including laser and energy devices, chemical peels, and mechanical dermabrasion.21 Individual patients have different types of scars, usually an assortment of types and sizes, with additional variation in terms of anatomic location. The particular mix of scars and their particular features directs selection of appropriate therapies6,22 (Figure 8.4.i.2, Algorithm 8.4.i.1).
Medical
Cosmetic
Procedural management of atrophic acne scars includes resurfacing modalities in addition to those based on laser and other sophisticated energy modalities. These include electrodessication, chemical peels, microdermabrasion, dermabrasion, and cold microneedling.21
Electrodessication
Chemical Peels
Superficial. Superficial chemical peels, such as light glycolic and salicylic acid peels applied at home, can mitigate active acne and may temporarily improve the appearance of atrophic scars by buffing and smoothening the stratum corneum. There are anecdotal reports and popular belief that a variety of other substances may improve atrophic acne scars through topical use, but there is sparse to absent high-quality evidence in support. Superficial peels appear to transiently improve the appearance of atrophic scars by smoothening the stratum corneum, but these very modest results recede within a few weeks.
Medium and Deep. Chemical peels include superficial peels that rarely injure full-thickness epidermis, as well as medium and deep chemical peels that provide dermal injuries of various depths. Common peeling agents include alpha hydroxyacids, beta hydroxyacids, Jessner solution, resorcinol, and dilute (<10%) trichloroacetic acid (TCA). Medium-depth chemical peels are typically more concentrated TCA (25%-35% is common), possible with concomitant application of Jessner solution. Deep chemical peels include phenol or croton oil, and the Baker-Gordon variant is often performed. Medium-depth peels can reduce some ice pick or shallow boxcar scars, but the degree of effectiveness is generally less than that of nonablative or ablative laser resurfacing (discussed
later).27,28 Deep chemical peels are highly effective at treating atrophic scars but are also risky, associated with hypopigmentation and depigmentation, as well as scar creation. As a consequence, deep peeling is frequently used only to treat specific, localized scars. The so-called CROSS (chemical reconstruction of skin scars) technique pioneered by Lee et al entails delivery of very concentrated (up to 100%) TCA to individual ice pick or boxcar scars.29 A tiny droplet is delivered from a hypodermic needle or a sharpened wooden stick to the base of the scar until a slight frost is elicited. This dissolves the epidermis, and over the ensuing weeks, allows the dermis to granulate and raise up as reepithelialization occurs. After a series of up to 6 treatments, the depressed scar may be filled in and flush to the surrounding normal skin.
later).27,28 Deep chemical peels are highly effective at treating atrophic scars but are also risky, associated with hypopigmentation and depigmentation, as well as scar creation. As a consequence, deep peeling is frequently used only to treat specific, localized scars. The so-called CROSS (chemical reconstruction of skin scars) technique pioneered by Lee et al entails delivery of very concentrated (up to 100%) TCA to individual ice pick or boxcar scars.29 A tiny droplet is delivered from a hypodermic needle or a sharpened wooden stick to the base of the scar until a slight frost is elicited. This dissolves the epidermis, and over the ensuing weeks, allows the dermis to granulate and raise up as reepithelialization occurs. After a series of up to 6 treatments, the depressed scar may be filled in and flush to the surrounding normal skin.
Microdermabrasion
Microdermabrasion, a technique comparable in effectiveness to superficial peels, uses exfoliating crystals, often blown onto and vacuumed off the skin surface, to abrade the stratum corneum. After several treatment sessions, mild transitory improvement in acne scars is possible. At high power, or when using very abrasive crystals, such as aluminum oxide or diamond-tipped abrasive devices, deeper injury in the dermis may be achieved, with consequent pinpoint bleeding. Still, despite patient enthusiasm for this treatment, objective, persistent improvement in treated acne scars is minimal at best.30
Dermabrasion
Dermabrasion, confounded by many patients and some physicians with microdermabrasion, is a more aggressive procedure that removes full-thickness epidermis and partial-thickness dermis with abrasive devices,
such as a diamond fraise, a wire brush, or sandpaper. Dermabrasion, in the right hands, is more effective for the treatment of atrophic acne scars than medium-depth chemical peels, and possibly even than some nonablative and ablative lasers procedures. Dermabrasion is highly operator dependent, and this has resulted in less widespread adoption of this technique. As with deep chemical peels, aggressive dermabrasion procedures can risk injury that destroys follicular structures and induces scarring.
such as a diamond fraise, a wire brush, or sandpaper. Dermabrasion, in the right hands, is more effective for the treatment of atrophic acne scars than medium-depth chemical peels, and possibly even than some nonablative and ablative lasers procedures. Dermabrasion is highly operator dependent, and this has resulted in less widespread adoption of this technique. As with deep chemical peels, aggressive dermabrasion procedures can risk injury that destroys follicular structures and induces scarring.
Microneedling
Microneedles are fine metal or plastic needles, provided either singly or mounted in an array on a surface that can be used to perforate the skin. They are available in various lengths, and the associated skin penetration depths range from the superficial epidermis to full-thickness dermis. Microchannels created in the skin by microneedles are a macroscopic, less dense analog of the microthermal zones induced by fractional lasers. Also, unlike fractional lasers, microneedles are not associated with thermal injury, which can improve their safety profile in darker-skinned patients at risk for hyperpigmentation, but limit the degree of treatment-associated tissue contraction. Microneedling has been used in combination with topical serums, including platelet rich plasma, to accelerate scar remodeling, but this combination treatment is of uncertain benefit. Use of nonsterile, nonbiocompatible serums with microneedling is inadvisable because of the risk of infection, granuloma, or immunogenicity.31
Laser Resurfacing
When resurfacing of all or part of the face or other body area is performed to reduce atrophic acne scarring, the most commonly used devices are lasers and other high-energy devices. Resurfacing with laser and energy therapy can be further subclassified into treatment with ablative devices and treatment with nonablative devices. Moreover, ablative and nonablative treatments can be delivered to cover the full skin surface or a fractional part thereof. So-called fractional devices treat, in a gridline pattern, minute skin zones while sparing the area between these, thereby allowing for less downtime and more rapid healing. Fractional treatments may also consequently be less effective than full coverage or require repeated treatment iterations to attain comparable results.
Ablative Resurfacing Devices. Ablative devices vaporize the skin, typically removing all of the epidermis and partial-thickness dermis. The traditional workhorses in this category are the carbon dioxide (CO2) and the erbium yttrium-aluminum-garnet (Er:YAG) lasers. Carbon dioxide lasers tend to induce relatively more thermal injury and char than erbium lasers and also more thermal contraction of scars and are relatively contraindicated in patients with darker skin types, who may have hyperpigmentation after treatment.
Fractional Ablative Resurfacing. Fractional ablative devices are associated with shorter healing times than full-field devices, and less risk of inducing scar or hyperpigmentation or hypopigmentation, but more treatments may need to be performed for equivalent effect. Ablative resurfacing, whether full field or fractional, is useful for the treatment of ice pick and boxcar scars, and the thermal contraction induced by carbon dioxide lasers may even help attenuate some rolling scars. If other, more invasive treatments for atrophic acne scars are required, including excisional and incisional procedures, these are typically performed before ablative laser resurfacing. Neocollagenesis and remodeling of the dermis after ablative resurfacing can hide marks, scars, and depressions created by previous acne reduction procedures. Ablative resurfacing does result in prolonged erythema and edema, and a variable degree of crust and erosion, with downtime of approximately 2 weeks after full-field and 1 week after fractional treatment. Ablative treatments are often chosen over nonablative treatments when the degree of atrophic acne scarring is severe. Great care should be taken when considering fractional or full-field ablative treatments for acne scars off the face, such as the chest, neck, and back, as the risks of treatment may outweigh the potential benefits.32
Nonablative Resurfacing. Although traditional conventional wisdom was that full-field carbon dioxide laser was by far the best way to treat atrophic acne scars, expert opinion has evolved to support the use of other treatment approaches as well. Nonablative resurfacing, in which the epidermis and dermis are damaged but not vaporized, can also be helpful in stimulating collagen remodeling and improving depressed scars. Like ablative resurfacing, nonablative treatments can be full field or fractional.
Fractional Nonablative Resurfacing. Repeated fractional nonablative treatments at low density (small proportion of skin treated) and high energy (each treated zone affected to higher depth) have been found to be highly effective for the treatment of atrophic acne scars.
For patients with mild or moderate atrophic acne scars, particularly ice pick and boxcar scars, a series of 5-6 such treatments may provide dramatic improvement, comparable with that of several fractional carbon dioxide laser treatments. Although relatively more nonablative fractional treatments are typically required, downtime is seldom more than a weekend, and the intensity of downtime is less acute, with an attendant decreased risk of pigmentary abnormality or treatment-induced scarring. Patients with Fitzpatrick skin types IV to V can be safely treated with appropriate settings. Common devices in this category include the fractional 1550-nm erbium laser.33,34
For patients with mild or moderate atrophic acne scars, particularly ice pick and boxcar scars, a series of 5-6 such treatments may provide dramatic improvement, comparable with that of several fractional carbon dioxide laser treatments. Although relatively more nonablative fractional treatments are typically required, downtime is seldom more than a weekend, and the intensity of downtime is less acute, with an attendant decreased risk of pigmentary abnormality or treatment-induced scarring. Patients with Fitzpatrick skin types IV to V can be safely treated with appropriate settings. Common devices in this category include the fractional 1550-nm erbium laser.33,34
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree