Why Did You Decide to Do These Techniques?
Vulvar and vaginal surgery cause an inevitable scarring process and when major complications occur, an uncontrolled scar process undermines tissue reconstruction. There are inevitable scars and others are true vulvovaginal (VV) complications leading to uncontrolled scars. Here, I explain the differences between these two processes.
Inevitable scar
Vulvar Surgery
The inevitable subdermal and deep scar as a result of incision and sutures may lead to pain caused by nerve inclusion and tissue distortion. Episiotomy incision, Bartolini cyst removal, and partial vulvectomies are good examples. The loss of issue elasticity determines a dramatic anatomical change, transforming the VV dynamic myofascial system into a rigid and static one. For example, vulvoperineoplasty via fascial plication determines reduction of tissue laxity but determines staticity, increase tissue rigidity, and may determine traction on pudendal nerve fibers located posteriorly to transverse muscle.
Vaginal Surgery
The majority of vaginal surgeries require fixation and controlled scar processes.
Sometimes scars may be painful as a result of pudendal nerve fiber inclusion or traction (e.g., vaginal vault fixation on the sacrospinus ligament after vaginal hysterectomy) or to myofascial abnormal tractions.
Slings and transvaginal tape (TVT) meshes determine a rigid system with often uncomfortable/painful sensations as a result of major loss of tissue elasticity.
True vulvovaginal complications leading to uncontrolled scars
Vulvar Surgery
Hematomas, seromas, infections, and the secondary intention healing process lead to uncontrolled scars.
Vaginal Surgery
Rectovaginal fistulas and urethrovaginal fistulas are among the most challenging complications to fix because of anatomy and poor tissue quality surrounding the fistula.
What Is Your Contribution?
My personal experience is as a result of 22 years of cooperation with gynecologists in a public hospital institution, working together on genital malformations, vulvar cancer, VV stenosis, and atrophies.
The of vulvar and vaginal regenerative surgery are to regenerate tissue, to restore trophicity, to enhance tissue elasticity, and to restore muscle continuity and function.
I have always been looking for innovative regenerative and reconstructive solutions that I share with you today. I will go through different surgical complications of cases such as episiotomy complications, vulvar stenosis, TVT mesh erosions, and vaginal vault scarring after vaginal hysterectomy.
Can You Explain to Us the Different Approaches You Offer to Your Patients and the Key Elements for Performing Them?
A regenerative and reconstructive approach to VV scars
The treatment of the VV scar is based on:
- 1.
Tissue regeneration via fat graft (macro-/micro-/nanofat graft according to tissue damage)
- 2.
Soft tissue reconstruction via flaps for major tissue loss
- 3.
Fascial and muscle continuity reconstruction if possible
To achieve best results, the following points are fundamental:
- 1.
Knowledge of anatomy
- 2.
Knowledge of VV function
- 3.
Knowledge of general fat cell regenerative principles and specific knowledge of genital fat graft
- 4.
Knowledge of genital tissue expansion/distraction and pelvic floor rehabilitation
VV scar treatment
- 1.
EPISIOTOMY SCAR
- 2.
VULVAR STENOSIS
- 3.
TVT MESH EROSION/EXTRUSION
- 4.
VAGINAL VAULT SCAR AFTER VAGINAL HYSTERECTOMY
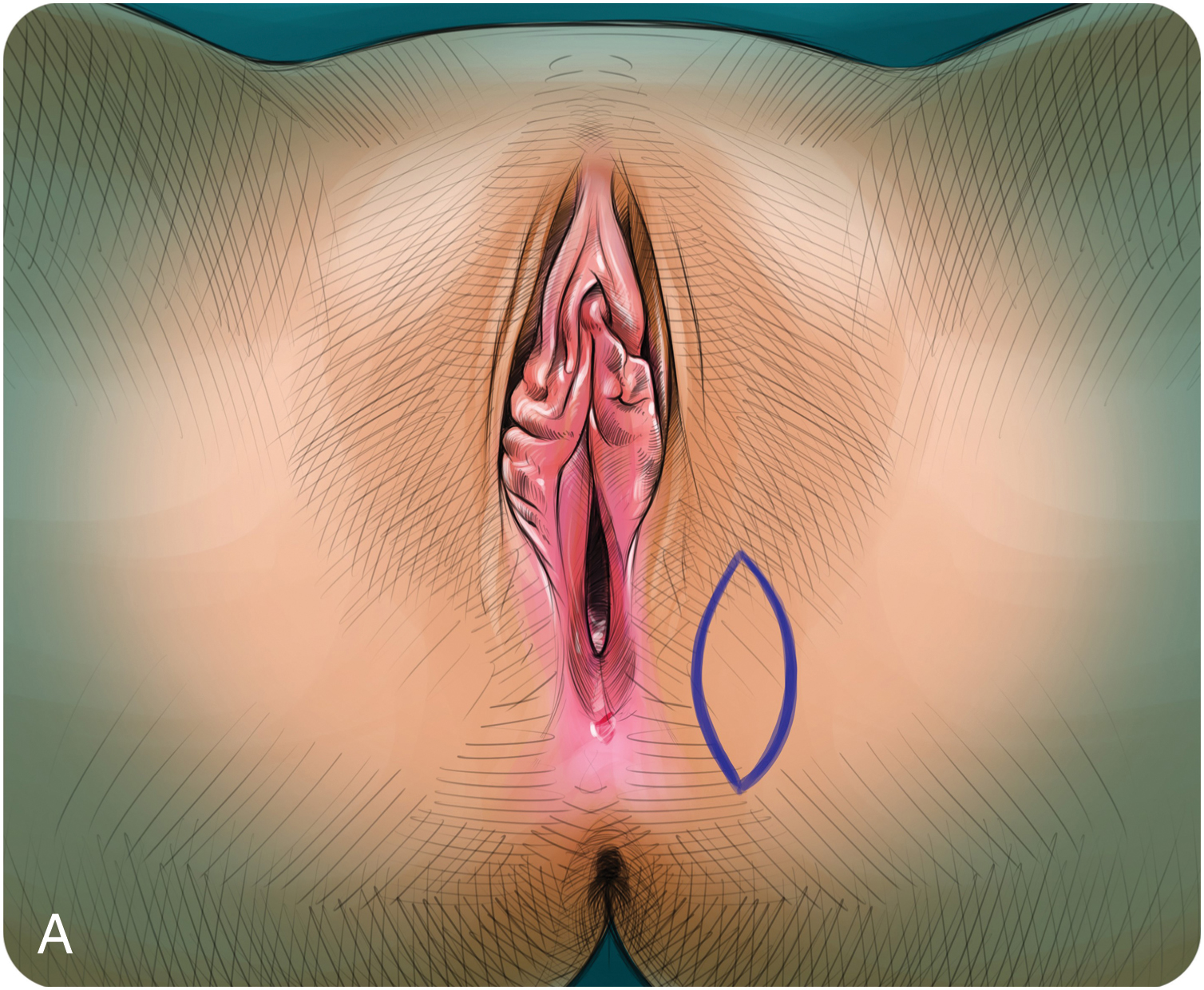
Episiotomy scar treatment
INDICATION: vulvar pain after episiotomy scar nonresponsive to pelvic floor rehabilitation
SURGICAL STRATEGY:
- •
HOSPITALIZATION: day surgery
- •
ANESTHESIA: nerve blocks + local + sedation
- •
ARMAMENTARIUM: microfat graft kit, 18-gauge needle for rigotomies (percutaneous scar release), surgical instruments (if needed)
- •
SURGICAL PLAN:
- a.
no major loss of tissue (<3 cm of tissue loss between ideal medial vulvar wall line and defect)
- •
Microfat graft + rigotomies: Starting from the subdermal area, microfat grafts are placed medially via percutaneous release, reaching most lateral scar tissues. Fat quality: decanted microfat graft (to have fluid graft that can expand tissues) Quantities: 5–15 cc according to tissue damage extension
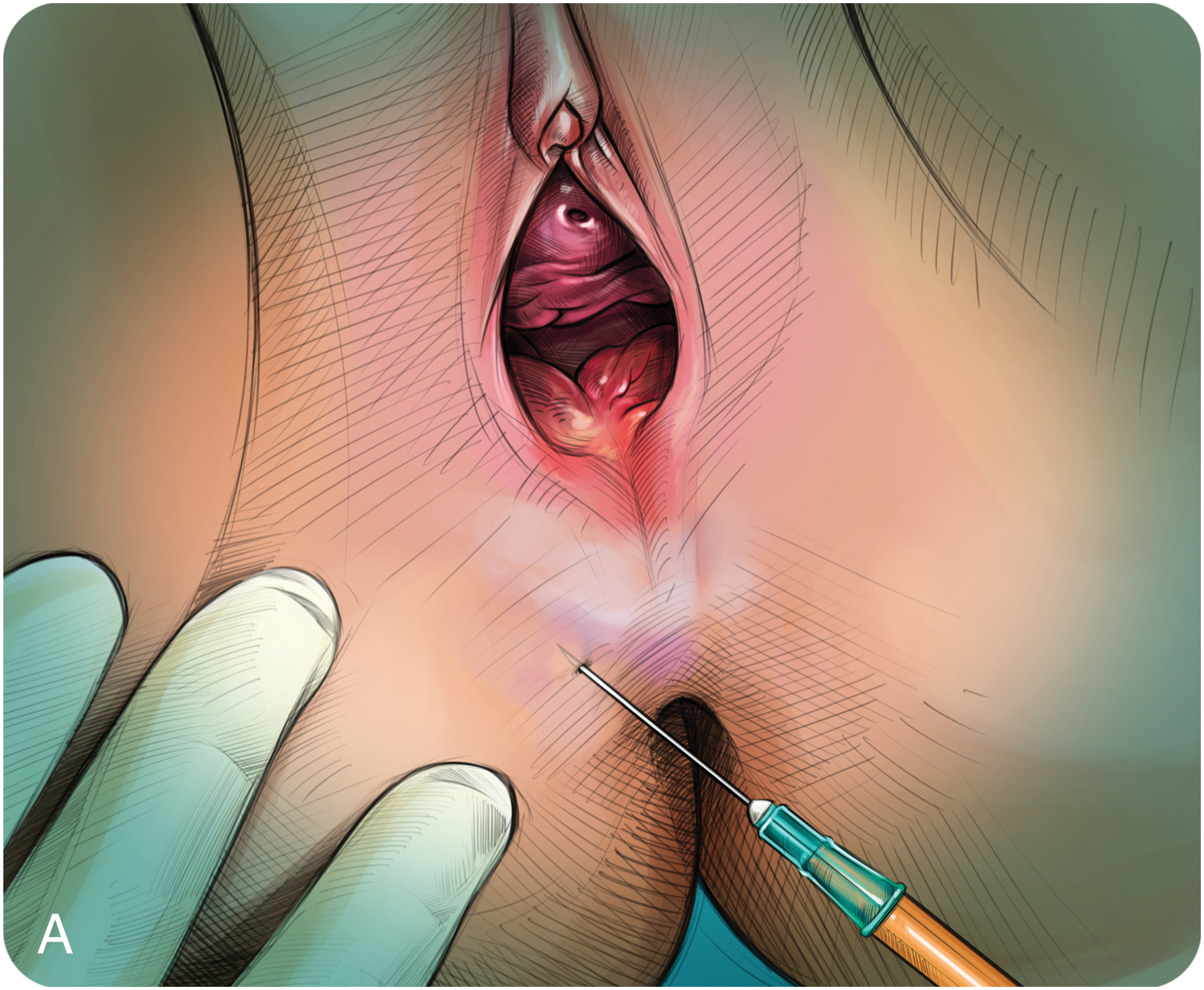
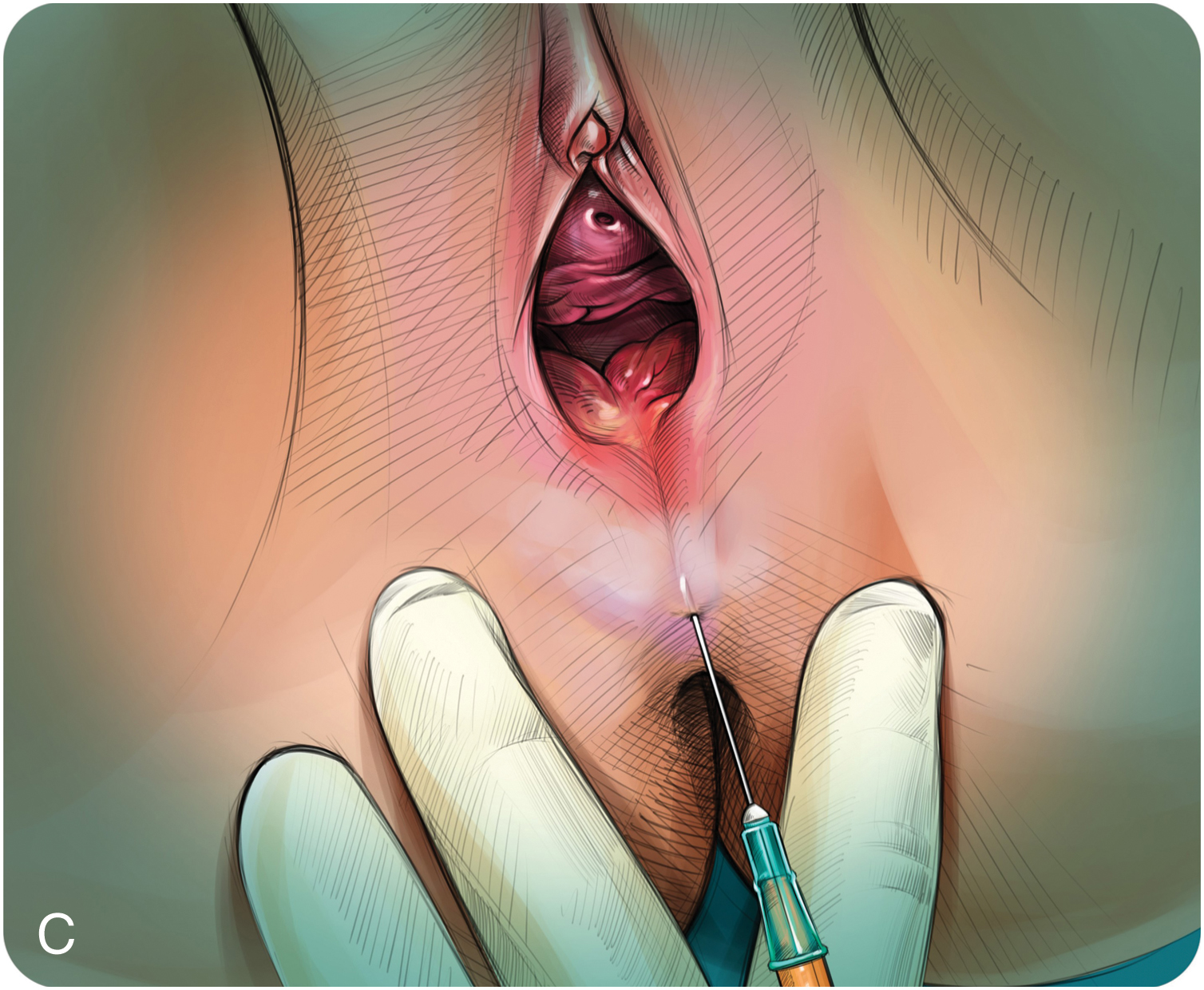
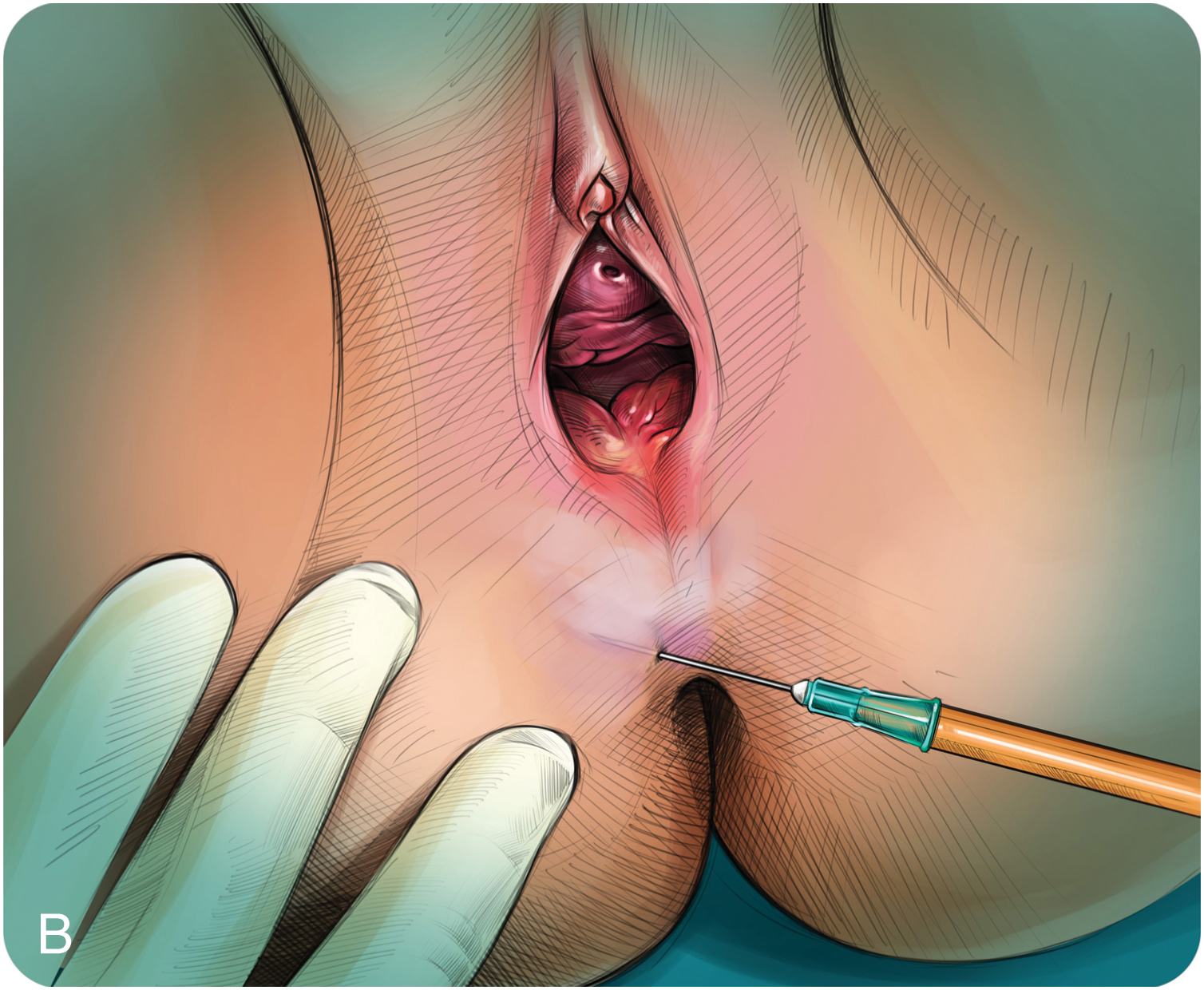
Fig. 4.1
Episiotomy treatment: rigotomies + microfat graft.
(A) Superficial scar release. (B) Deep fat release. (C) Perineal fat release.
- •
- b.
major tissue loss (>3 cm of tissue loss between ideal medial vulvar wall line and defect)
- a.