Introduction
In the 20th century, there were significant improvements in burn care. This resulted in an emphasis on morbidity over mortality. Involvement of the head and neck occurs in approximately 60% of patients who have more than 50% total body surface area (TBSA) burns. The majority of head and neck burns are superficial second-degree burns. It is a natural reaction to flex the neck in many situations, and for that reason the neck is often relatively spared in burn injuries. Because of this and because of the rich blood supply to the skin in the head and neck, most burns can be expected to heal, so the majority are treated conservatively. The general consensus is that if these burns do not heal within 2 weeks—either because of infection or because of the depth of the burn—excision and grafting are required. However, the relative outcomes of conservative versus surgical treatment have been open to conjecture. The skin of the face and neck, with the exception of the scalp and forehead, is very mobile. This area is therefore very susceptible to scarring and contracture. Because of the propensity of these wounds to contract concentrically, scarring of the head and face can cause multiple deformities, ectropion of the eyelids, perioral contraction, destruction of the ears and nose, and of course, contraction of the neck. Reconstruction of these areas is discussed in the previous chapters. However, isolated contraction of the neck can cause significant problems because of the resulting lack of movement. The perioral region is most often affected even though the perioral region may not have been burned, as in the patient in Fig. 61.1 . The mouth opening is not necessarily affected although the neck will exert a considerable restricting force on the lower lip even in the absence of burn injury to the lower lip itself. The big problems with contracture of the oral orifice, whether by intrinsic scar contracture or contracture of adjacent areas such as the neck, are drooling, interference with articulation, chronic dental exposure leading to caries and drying of the enamel, and the obvious cosmetic deformity.
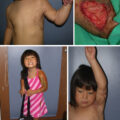
This older adult sustained flame burns to the neck .
(A) Anterior-posterior view. (B) Lateral view. Note the contraction, the cosmetic deformity, and the absence of cervicomental definition.
Reconstruction of the neck
Although the majority of neck burns encountered will heal, the most debilitating sequela to neck burns is contraction. In the neck, this can result not only in restriction of movement but also in significant cosmetic deformity and oral issues as previously outlined. For this reason, it is important to keep the skin well moisturized and, if there is any fear of contraction, to splint the patient. Compression garments, which are used widely in burn care, are problematic in the neck for obvious reasons. However, problems with contraction and restriction of movement often present secondarily because the degree of contraction can increase with time ( Fig. 61.1 A, and B). The choice of reconstruction depends on many factors, including the extent of the burn injury. Burn scars in adjacent areas, such as the chest, can contribute to neck morbidity and increase the amount of contraction that is exerted. This frequently gives rise to an even larger defect when the area to be reconstructed is excised. Any previous attempts at reconstruction and the methods used in those attempts are also important. There are many options for reconstruction: Z-plasties; skin grafting; and tissue expansion or flap reconstruction, either pedicled or free.
Z-plasty
A Z-plasty is considered a local tissue rearrangement, and it has been used since 1837 to break up scar lines. Lindberg noted that the “main effect of local plastic operations is redistribution of local tissues without addition of tissue from distant sources and with minimal excision of normal tissue.” Lindberg further noted that the “goal of plastic surgery is to create a proper contour by making the best distribution of available materials.” In simplistic terms, the Z-plasty lengthens the central limb, and it may be used as a single large procedure or as multiple small “Zs,” either together or separated. Although Gao et al. found that “Z-plasty is not used for burn scar contracture” release, these authors felt it was of great benefit to release scar bands, but not a confluence of bands. When used appropriately, a Z-plasty can accomplish a great deal in neck releases following thermal injuries. The basic principles are simple, but when they are not followed, the scar contracture can actually worsen.
These principles are the following:
-
1.
Place the central limb in the line of the scar band.
-
2.
Adjust the angles of the Z no greater than the pliability of the skin in which the release is performed allows.
-
3.
Place the auxiliary limbs to allow the best blood supply.
-
4.
Place the auxiliary limbs to allow better contour to the reconstructed area when appropriate.
-
5.
Make the flaps thick.
The scar band is best determined by placing the neck on stretch. The bands are usually either centrally or laterally placed, and once the neck is extended, the central limb is marked. Although large Z-plasties may be used, tip necrosis is more common. Limiting the limbs to no more than 3 cm in length decreases the risk of tip necrosis. Theoretically, the greater the angle of the auxiliary limb, the more the central limb is lengthened. Unfortunately, the pliability of surrounding skin and its vascularity dictate how well the flaps rotate and how well they survive. Generally, a 45-degree angle is a safe choice; it lengthens the central limb approximately 50%.
Once the central limb is marked, determine the pliability and vascularity of the surrounding skin by visual inspection and palpation.
After the flap has been designed, lidocaine with epinephrine may be used for the hemostatic effect in conjunction with general anesthesia or as a stand-alone anesthetic agent in small flaps. When injected along the lines of incision and not beneath the flap, epinephrine does not affect flap viability.
Thin flaps have a tendency to have more flap necrosis caused by poor blood supply, and therefore thick flaps should be used. After the injection, a hemostatic wait of 5 to 7 minutes is allowed, and the incision should be carried down to the platysmal or remaining muscle without beveling. The adipose is kept attached to the dermis to assure the best vascularity for the flap. The flaps are then inset with either a single layer of 4-0 or 5-0 nylon or 5-0 Vicryl (Ethicon) or with PDS (Ethicon) deep dermal suture and 5-0 plain gut on the skin. The latter is most often used in my hands because I do not have to remove the skin sutures and because the deep dermal sutures (a maximum of two per side of the limb) provide support without causing unsightly suture marks in the neck. A half-buried corner suture is also used to ensure good approximation of the corners but is not tied too tightly to avoid tip necrosis.
Although the concept of the Z-plasty is quite simple, and the technique follows a geometric process, a simplistic approach to the design and to the technical part of the procedure often produces inferior results. The design includes the determination of the location of the central limb, the location and angles of the lateral limbs, and the ultimate contour once the flaps are rotated. Careful thought should go into the design of the flap, and adherence to the previously discussed technical components provides the best chance for success.
Skin grafting
Skin grafting is the most expedient and common way to cover burn wounds, and it can be very successful in the neck, either as the primary or secondary reconstruction. When using skin grafts, it must be remembered that all skin grafts undergo primary and secondary contracture. Primary contracture is the immediate reduction in the size of skin graft after it has been harvested, a process caused by passive recoil of elastin fibers in the dermis. Full-thickness skin grafts (FTSGs) have a greater amount of dermis, and therefore primary contracture is more significant than in split-thickness skin grafts (STSGs). Secondary contracture is the shrinkage of the skin graft in the wound bed over time, a process caused by myofibroblasts. Secondary contracture is greater for STSGs than FTSGs, because the additional dermis in FTSGs is resistant to the pull of myofibroblasts.
Primary contraction is often addressed by meshing the graft. This not only addresses the issue of primary contraction, but depending on the ratio of meshing, meshing the graft can cover a larger defect with a given area of skin graft. The holes between skin bridges act as drainage holes to prevent fluid, blood, or seroma buildup between the patient’s wound bed and the skin graft, which would cause graft failure. Theoretically therefore meshing improves graft take. However, meshing should generally be avoided in the head and neck because the mesh pattern is always visible and can be unsightly. STSG is also the type of reconstruction that is most likely to lead to recurrence of the contracture, particularly if very thin split-thickness grafts are used. Not only do STSGs undergo secondary contraction, but the wound bed also undergoes contraction. One strategy to mitigate the possibility of contraction is to use a dermal substitute such as Integra (Integra LifeSciences; Princeton, NJ). Integra serves as a scaffold for a neodermis and therefore helps augment the integrity of the skin graft. Integra is placed on the wound after all debridement is complete in much the same way a STSG is applied. Integra’s surface is a silicone sheet that is removed once the underlying material develops a pinkish color indicating revascularization. A STSG is then used to replace the silicone sheet so that when the graft takes, there is a dermal scaffold underneath. Some practitioners have questioned whether Integra may interfere with reinnervation of a skin graft. I have found use of a vacuum-assisted closure ([(VAC) Therapy] 3M; St. Paul, MN) useful as a dressing over Integra and over skin grafts. It obviates the need for strict immobilization, which was necessary in the past to optimize graft take. With the advent of other skin substitutes, including NovoSorb biodegradable temporizing matrix ([BTM] PolyNovo; Victoria, Australia) and a fish-skin product GraftGuide (Kerecis; Isafjordur, Iceland), the reconstructive surgeon has many tools for closure of the mobile neck skin.
Another strategy to minimize wound contraction is to use FTSGs. FTSG’s advantages are two-fold: the graft quality is better, and the risk for secondary contraction is less. The disadvantage is that it is more difficult to achieve revascularization and take of a full-thickness graft than an STSG. A thin STSG heals much more quickly, but the thinner the graft, the greater the likelihood of secondary contraction. Furthermore, the large donor site of the FTSG used has to be closed, possibly by using STSG or by expanding the donor site before full-thickness harvest, so that the ensuing defect can be closed directly. Some advocate that full-thickness grafts offer a better result than either split-thickness grafts or free flaps.
Tissue expansion
A tissue expander can be used in situations where there is adjacent normal unburned skin that can be advanced or rotated to replace the scar that needs to be excised. It can be used to replace a narrow contraction band ( Fig. 61.2 ) or a more diffuse area of contracted scar ( Fig. 61.3 ). The big advantage of tissue expansion is that it introduces unburned adjacent skin into the area to be reconstructed. This, of course, provides excellent texture and color matching, and it leaves minimal donor site morbidity. The expanded skin is particularly well vascularized, akin to the delay phenomenon in a flap, and it tolerates advancement and manipulation very well. Properly planned, tissue expansion can provide an unsurpassed reconstruction. However, tissue expansion should not be used in the acute situation because of the risk for introducing infection into the expander pocket. It is therefore best used in situations where the scar has contracted and is well healed. The recognized complications of tissue expansion apply: extrusion, infection, and inadequate expansion. Expansion in the head and neck has been associated with a relatively high-complication rate. Also, the bigger the expander, the greater the risk for complication. Patients frequently require more than one expander, and appropriate placement of the expander(s) is important to optimize outcome ( Fig. 61.3 ). It is important that the patient understands that this type of reconstruction is tedious, demands meticulous skin care during the expansion phase, and requires regular visits to inject the expander. Also, the patient should be told that the process may need to be repeated to achieve the ultimate result. It therefore requires commitment on the part of the patient, which makes appropriate patient selection imperative.