Introduction
Since its development in the 1990s, negative pressure wound therapy (NPWT) has had many names: subatmospheric pressure (SAP), vacuum-assisted closure (VAC), topical negative pressure (TNP), and microdeformational wound therapy (MDWT). These arose out of a combination of the rapid adoption and dissemination of the technology and the multiple investigations into its mechanism of action and indications. Its original investigational application was to wounds of varying chronicities and etiologies, but NPWT was immediately identified as being an excellent choice in the treatment of burns. , This chapter will describe the science and utility of NPWT in all phases of burn reconstruction.
Mechanism of action
Despite this therapy evolving and the implementation of much research, the exact mechanism of action resulting from SAP still needs to be fully determined, although many accepted theories have emerged.
NPWT is considered for use as an adjunctive therapy, usually after traditional moist-dressing products have failed or for more extensive wounds. Some indications for NPWT are the treatment of trauma, infection, congenital deformities, tumors, burns, and grafts. The ability of this therapy to increase blood flow to the treatment area, promote granulation tissue formation, and remove bacteria and fluid from the wound makes it an obvious choice when handling complicated wounds related to these indications.
The true mechanism of action continues to evolve for this therapy. Still, more recently, it has been widely accepted that outcomes for acute and chronic wounds are improved through the therapy’s various components, including the wound-foam interface, creating a semiocclusive microenvironment, and the mechanical forces incorporated into NPWT. Several sources have focused on the mechanical forces of NPWT as a more logical explanation for the mechanism of action for this therapy. , ,
The initial motivation for NPWT was to control wound fluid more easily. A sponge of an open-cell, polyurethane ether foam matrix was applied to the wound bed and covered with a semipermeable drape making a closed system. The drape was perforated over the sponge, and a noncompressible tubing was attached to a vacuum device with an attached canister. The technique did manage wound fluid well, but after its application in animal models, the impact on granulation tissue formation and wound healing could not simply be explained by exudate management alone. , The choice of sponge with 400- to 600-μm pore sizes proved to be serendipitous as the interface between the wound and sponge would play a significant role in the mechanism of action of NPWT. ,
NPWT exerts both biophysical and biochemical changes on the wound bed. At the initial decompression of the sponge, there is an immediate macrodeformational change dependent on the wound’s compliance that assists in gross wound contraction. Microdeformational changes happen simultaneously, leading to 5% to 20% tissue strain transmitted through the extracellular matrix to individual cells.
Microdeformation results in stretching the tissues upward into the pores of the wound filler material. This microdeformation is evident by histology. Furthermore, foam and gauze can cause microdeformation of the wound bed, suggesting that this effect is a fundamental mode of action of NPWT.
The combination of macro- and microdeformational forces leads to a cascade of mechanotransduction pathways that alter gene expression and modulate inflammation. , , , , , Whereas NPWT alters expression of inflammatory cytokines and growth factors, the exudative fluid removal action of the vacuum device enhances wound healing by removing toxins, bacteria, and proteases associated with chronic wounds. , The sponge and drape retain moisture ideal for wound healing and provide a thermally insulted environment with osmotic stability. Other mechanical forces exerted by NPWT include shear and hydrostatic pressure from the extracellular fluid.
Macrodeformation refers to the wound shrinkage caused by the collapse of the pores and centripetal forces exerted onto the wound surface by the foam. How large or deformed the wound is will impact the extent of contraction. Other factors that may influence macrodeformation are the type of tissue treated, the suction level, and the foam’s volume.
The following fundamental requirements will allow a full mode of action:
-
1.
A target level of pressure is delivered.
-
2.
A pressure gradient is created.
-
3.
A sealed wound environment is maintained.
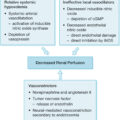
Blood flow to the wound is also affected through NPWT by both immediate and late mechanisms. The immediate effect is secondary to changes in wound edema and pressure. Removal of extracellular fluid improves tissue perfusion by decreasing interstitial fluid pressure and edema. Pressure exerted on the wound from the sponge is thought to limit the fluid shift induced by denatured collagen during the acute burn. The pressure from the sponge induces increased capillary blood flow as registered with laser Doppler. , , NPWT induces angiogenesis by modulating cytokines and growth factors and modulates the ultrastructures of wound bed capillaries and endotheliocytes. , It is this increase in blood flow combined with the control of edema that is thought to limit or prevent burn wound progression. Table 45.1 summarizes the mechanisms of action of NPWT.
Table 45.1
Mechanisms of Action of Negative Pressure Wound Therapy
|
Applications in unexcised burns
Superficial and partial-thickness burns
Because of its demonstrated ability to increase blood flow and reduce tissue edema, NPWT has been used extensively in the treatment of burn wounds. Superficial burns heal well without advanced wound care measures, so the use of NPWT on superficial burns has never been published. ,
Superficial partial-thickness and deep partial-thickness burns can be less predictable with the threat of burn wound progression. Kamolz et al. and Schrank et al. performed similar studies on patients with bilateral hand burns. Using the patients as their own controls, NPWT was applied to the more severely burned hand, and indocyanine green angiography was performed to assess perfusion. When NPWT was applied within 6 hours of the initial injury, the investigators noticed increased flow to the hand under the NPWT dressing and a notable reduction of edema. These and other studies concluded that the increase in perfusion and decreased edema would be protective against burn wound progression. Unfortunately, no randomized controlled studies have been published to demonstrate this effect. , , , ,
Full-thickness burns
Despite the tissue injury in full-thickness burns being irreversible, NPWT can still provide utility to the treatment team. Insensible losses are difficult for teams to measure directly and may complicate resuscitation efforts. NPWT is well designed to manage not only these insensible losses but also simultaneous wound exudate. The “total body wrap concept” can be implemented as a tool to collect wound exudate on large total body surface area (TBSA) wounds. Even fewer NPWT devices can be used to achieve the same benefits by using longer, strategically placed strips of foam. The NPWT canister simplifies estimation and can direct fluid replacement. , ,
NPWT removes fluid so effectively that dressing changes can be performed less frequently, which decreases patient pain and reduces the burden on nursing staff. , , This feature is useful when the patient is not ready for excision or is too unstable for excision or frequent dressing changes. NPWT can also be combined with additional dressings to retain the advantages of both dressings. , , Excision is almost always necessary in large TBSA burns, and NPWT is a useful dressing with many advantages that can be used to bridge a patient to excision.
Applications in excised burns
Directly to wound bed
After burn wound excision, applying any combination of human skin allograft, xenograft, dermal regeneration template (DRT), or autograft is typical. Occasionally, conventional dressings or NPWT can be applied to excised burn wounds instead. NPWT assists in the formation of granulation tissue and improves the wound bed for eventual grafting. When performed in a staged fashion, there is evidence of the decreased need to regraft wound beds prepared with NPWT. ,
To prepare the wound bed, the NPWT settings can be adjusted to meet the specific needs of the patient. The practitioner may select the pressure setting from −50 mm Hg to −150 mm Hg as well as the therapy type: continuous, intermittent, and instillation. Typically, the pressure setting of −125 mm Hg is selected but can reduce to −75 or −50 mm Hg if the higher pressure differential causes pain or impedes participation in physical therapy. , Both continuous and intermittent therapies were originally tested on burns showing improved granulation in the intermittent mode. Later studies confirmed this result, possibly explained by a combination of mechanotransduction from shear, stress, and increased blood flow from the intermittent relief of pressure from the wound bed. , , Compared with continuous mode, intermittent mode is associated with increased patient discomfort from frequent changes in dressing pressure. The instillation mode is a special type of intermittent suction with a variable dwell time of selected liquid medication. Installation mode for burns is most suited for cleaning contaminated wounds without the need for frequent dressing changes. , The continuous mode is best suited for its role as a bolster, which will be reviewed in the following sections.
Application with split-thickness skin graft
Bolsters and splints have been used to secure and improve the incorporation of split-thickness skin grafts. NPWT can be used as a bolster with additional advantages that improve engraftment. There are two distinct mechanisms that improve skin graft take. When NPWT is applied to a wound bed, there is a blood flow increase and the release of angiogenic cytokines. These characteristics improve the health of the wound bed to facilitate granulation and also improve the wound bed to enhance skin graft take. The next mechanism does not depend on the effect NPWT has on the wound bed but rather on the effect the device has on the contact between the skin graft and the wound bed. Because the sponge can be tailored to fit almost any wound, NPWT can be fashioned into an extremely effective bolster. Instead of the traditional tie-over bolsters and meticulous suture techniques required for conventional skin graft recipient site dressings, NPWT simplifies and improves the technique by allowing omnipresent atmospheric pressure to produce uniform pressure over the sponge collapsing at SAP. The sponge is able to contour the skin graft to the usual hills and valleys of a wound without the need for quilting sutures or fibrin glues. Fig. 45.1 demonstrates the contouring ability of NPWT.
Above: Negative pressure wound therapy (NPWT) dressing applied to skin graft before initiating suction. Below: NPWT dressing with suction activated with improved contouring of the skin graft to the wound bed.
Skin graft take rates, when combined with NPWT, are reliable and high compared with conventional dressings. Petkar et al. showed a series of burn reconstructions patients with a skin graft take rate of 96.7% with NPWT compared with 87.5% with conventional dressing. The NPWT group also demonstrated reduced duration of graft dressings compared with the control group. A systematic review and metaanalysis of 10 randomized controlled trials demonstrated improved graft take, reduction in days from grafting to discharge, and lower relative risk of reoperation when using NPWT combined with split-thickness skin grafting.
In addition to excellent graft take, NPWT allows for excellent splinting, as well as early mobilization of patients compared with conventional dressings. , In children who cannot cooperate with postoperative instructions, NPWT can provide a more tolerable alternative to splinting and also give clinicians and parents an alarm if the dressing starts to fail in the form of a leak alarm. The adherence of the dressing to the skin and hair prevents many curious children from exploring the dressing or inadvertently removing it.
Until a method to grow sheets of architectural dermis and epidermis is developed, the process of harvesting split-thickness skin grafting will necessarily create a patient donor site. The ideal split-thickness skin graft donor site dressing would be able to handle significant drainage, reduce pain, and promote epithelialization. NPWT is well suited to manage drainage and has been used to treat donor and recipient sites simultaneously. The donor sites were noted to have double the drainage of the recipient sites, and this volume was used to inform maintenance IV fluid replacement. Donor sites reepithelialized in an average of 11.25 days. There are reports of NPWT improving reepithelialization rates for donor sites, but there is not enough high-quality literature to support NPWT over other widely used donor site dressings.
Application of npwt with dermal regeneration templates
DRTs have applications throughout reconstructive surgery and have specific uses in burn reconstruction in particular. , , Whereas conventional excision and grafting require a well-vascularized wound bed, DRTs are initially not viable and do not have the metabolic demands of autografts. DRTs can be applied over complex wound beds, including tendon, ligament, and bone, to incorporate over time. NPWT has been employed to assist in the vascularization of DRTs and has become routine in the reconstructive surgeon’s practice.
The earliest research on the combination of NPWT with DRTs showed improved adherence of the graft at 3 to 5 days. NPWT was also shown to decrease the time to engraftment and readiness for skin grafting from the usual 2 to 4 weeks down to just 1 week. Others have pushed the envelope further by performing single-stage reconstructions with a DRT and skin graft in combination with NPWT. Enhanced engraftment of the DRT was shown to reduce time to healing from 8.9 to 5.8 days in conventional dressings compared with the NPWT dressing.
Whereas some argue that incorporation times are not significantly affected by NPWT, , others agree that other variables such as percentage of graft take, pain, scar elasticity, color match, treatment time, and number of dressing changes are all improved by combination with NPWT. Bloemen et al. performed a prospective, multicenter, randomized controlled trial comparing the use of skin grafts, DRTs, and NPWT in burned patients. Patients were randomized into one of four groups: skin graft (STSG) alone; STSG/NPWT; DRT/STSG; and DRT/STSG/NPWT. They found the best scar elasticity ratio and color match in the DRT/STSG/NPWT group and improved pain scores in DRT/STSG compared with STSG groups. The authors concluded that improved scar elasticity makes DRT/STSG/NPWT useful for reconstruction at critical joints such as the hands, elbows, and knees.
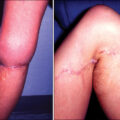
The application of DRTs with NPWT can be performed on an outpatient basis. After excision of the burn or the burn scar, the resultant defect can be cleaned and the DRT applied. Securing the DRT can be performed with suture or with skin glue. The NPWT dressing can be directly applied to templates with a silicone bilayer or with a nonadherent barrier dressing on templates without a silicone layer. Because NPWT reduces the needs for frequent changes, the device can be left in place for 3 to 10 days and engraftment can be checked in the outpatient setting. Fig. 45.2 demonstrates NPWT portability and effective outpatient management of a pediatric patient.
Above left: Preoperative picture of young female with left axillary burn scar contracture. Above right: Intraoperative picture of dermal regeneration template placed to wound after contracture release. Below left: Postoperative picture demonstrating portability of negative pressure wound therapy at outpatient follow-up. Below right: Final postoperative picture demonstrating normal range of motion after contracture release.
Special cases
Electrical injury
Electrical injuries represent a unique and challenging area of burn care. An electrical injury can be initially deceptive, with the full extent of the injury evolving over multiple days and requiring many debridements. Injury is often deep, and critical structures are often injured or exposed in the wound requiring careful consideration for reconstruction. Because NPWT has been shown to improve the development of granulation tissue, limit burn wound progression, and decrease painful dressing changes, its use in electrical injury is fitting. Series of high-tension electrical injuries managed with NPWT are uncommon, but the few that do exist show promising results. NPWT has been used in 60% TBSA, fourth-degree electrical injuries with successful salvage, although it took the authors 6 weeks to achieve sufficient granulation tissue for grafting. A small case series out of Colombia showed off the versatility of NPWT using a combination of continuous suction and instillation to prepare the excised wound bed for eventual skin grafting and used NPWT again as the bolster for the skin graft. Eyvaz et al. demonstrates a relatively large series of 39 patients with complicated electrical injuries with bone or tendon exposure, lack of wound progression, or failed skin grafting. After 3 to 4 dressing changes with NPWT, they were able to reconstruct these wounds with a 90.7% success rate. Although the data set is small, NPWT reveals itself to be an excellent choice in the management of electrical injuries.
Infection
Burn wound sepsis is a major source of mortality in the burn unit. Patients may arrive with environmental pathogens and because of the pathophysiology of the burned body, patients are more likely to contract nosocomial infections as well. Classically, NPWT is contraindicated in highly contaminated wounds, over untreated osteomyelitis, underlying malignancy, and in the presence of necrotic tissue. Decreased frequency of dressing changes and occlusion of the wound theoretically increased the risk of wound deterioration or spread of infection. Clinicians have challenged this paradigm, which has led to widespread usage and the invention of the silver-based sponge.
In an open fracture goat model, wet-to-dry dressings were compared with NPWT. By the sixth day of testing, the levels of Pseudomonas aeruginosa were reduced by NPWT but not the levels of Staphylococcus aureus. In a follow-up study, the authors employed silver dressings alone compared with standard NPWT and to silver dressings combined with NPWT on the same goat model. The authors found reduced bacterial loads of P. aeruginosa and S. aureus with the silver dressings with and without NPWT. The effect was greatest on S. aureus, leading the researchers to conclude that the silver/NPWT combination was more effective in gram-positive organisms. Contrary to this finding, Van Hecke et al. compared black, silver, and white foams in an ex vivo equine model and found that P. aeruginosa was inhibited by the white foam more than the silver foam. To determine whether antibiotic pharmacokinetics were affected by NPWT, drug levels found in wound exudates were compared with plasma steady-state concentrations. When comparing cefazolin, ciprofloxacin, piperacillin-tazobactam, and vancomycin, these authors found that cefazolin only achieved a subtherapeutic 51% wound-to-plasma ratio, whereas the others tested achieved a therapeutic 80% ratio. Differences in antibiotic distribution and the conflicting results on the influence of the type of sponge used complicate the relationship between NPWT and infection.
The question of the relevance of bacteria on the foam itself was asked by Anagnostakos and Mosser. They retrospectively evaluated 101 dressing foams from 64 patients to determine the correlation of wound cultures and bacterial isolates from black or white foams. Although only 39% of the foams yielded bacterial isolates, there was no definitive correlation between the species isolated on the foam and that isolated from the wound. Sometimes, bacteria grew uniquely on the sponge but not in the wound tissue. In a different study, black and white foams from chronic wounds were sonicated to determine relative amounts of colony-forming units. In this experiment, white foam had higher bacterial counts compared with black foam. The authors also found that higher levels of negative pressure were associated with fewer colony-forming units.
Specific to burns, a porcine model compared bacterial loads among four common burn dressings: normal saline, silver sulfadiazine, continuous NPWT, and intermittent NPWT. After 14 and 21 days, no differences were found among the groups. A systematic review of the effect of NPWT on the bacterial load and type of bacteria also could not make definitive conclusions for infected or noninfected wounds, but they did find low-level evidence that NPWT did not change the bacterial load. Overall, NPWT does not affect wounds in the setting of infection negatively, and clinicians may tailor their choice of antibiotics and foam to the specific needs of each patient.
Pediatric burns
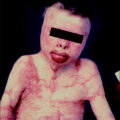
The pediatric burn population faces unique physiologic and developmental challenges. Physiologically, children have higher surface area to body ratios making the risk of dehydration and heat loss greater when burned. Pediatric skin is thinner and more fragile than adult skin and puts children at greater risk for deeper burns and an increased risk of sepsis. Regarding development, children are more active and less cooperative. Children are less able to comply with restrictions requiring self-monitoring and often need bulky, immobilizing dressings or casts to facilitate healing. At the same time, it is developmentally appropriate for children to be mobile and not delay specific motor milestones with such immobilization.
NPWT is well suited to the pediatric population allowing the clinician to secure DRTs and eventually split-thickness skin grafts with a high take rate and few dressing changes. NPWT replaces the bulky splints and casts previously employed and additionally acts as an alarm for disruption of the dressing. In the acute setting, NPWT can provide valuable information regarding fluid losses, manage edema, improve microcirculation, and decrease the pain and anxiety of dressing changes. Decreased bulk and portability of the device can facilitate early mobilization, decreased hospital stay by up to 22%, and decreased costs 89% of the time. , , , ,
Complications
Because of the macrodeformational changes and microdeformational changes of the foam, the most common complaint of NPWT is pain, particularly with intermittent suction. , Pain can somewhat be mitigated by decreasing the absolute amount of negative pressure. The most serious complication of NPWT is bleeding. For this reason, the manufacturer recommends NPWT not be used in situations of arterial erosion, exposed vessels, and necrotic tissue. Furthermore, the device’s canister can only hold up to 500 mL; in the event that there is a significant bleed, the device cannot exsanguinate the patient. This lends credence to the warnings made of attaching the dressings to wall suction where such volume limitations are removed. In addition, wall suction does not maintain consistent pressure over a long period of time, resulting in variable outcomes and increased pain.
Rare complications of NPWT include infection, stomal dehiscence, necrotizing fasciitis, and tissue adherence. As granulation is stimulated in the wound bed, whatever contact layer exists between the suction and the bed can be susceptible to adherence. When NPWT is placed over a split-thickness skin graft that has been meshed, the granulation tissue can overgrow the interstices and completely envelop the skin graft, leading the clinician to inadvertently believe there has been graft loss. Discontinuing NPWT and treatment with topical steroids leads to the recession of the hypertrophic granulation tissue and the healing of the wound from the autograft.
If the contact layer is foam, granulation tissue can grow into the pores and lead to foam retention in the wound during dressing changes. Retained pieces of foam can be found in up to 10% of wounds treated with NPWT. This foam is not radiopaque, so diagnosis can be challenging. Black foam has a higher chance of retention compared with white foam because of the difference in pore size and stimulation of granulation tissue. Enterococcus faecalis, Staphylococcus epidermidis, Enterobacteriaceae, S. aureus, and Escherichia coli are the most frequently isolated organisms on retained foam. Retained foam has an intense inflammatory reaction with pseudoepitheliomatous changes. The inflammatory changes and persistent infection limit healing and should be on the differential for stalled wounds being treated with NPWT. Strategies to mitigate retention are to perform frequent dressing changes at least every 24 to 120 hours and to write the date of the last and next dressing change with a permanent marker on the drape.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree