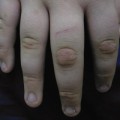
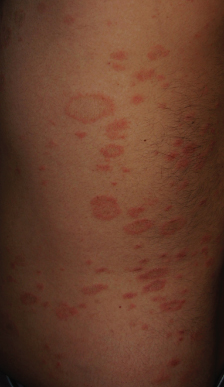
In children with typical pityriasis rosea, only the trunk and proximal aspects of the four extremities are involved. This distribution pattern is traditionally termed T-shirt-and-shorts or bathing suit pattern [64]. Palms and soles are typically spared in children. The orientation of lesions is typically along lines of skin cleavages (Fig. 84.2) [65].
Fig. 84.2 Truncal lesions of PR in an adolescent boy showing scaly round and oval plaques on trunk.
Reproduced from Expert Rev Dermatology 2010;5(3):325–333 with kind permission of Expert Reviews Ltd.
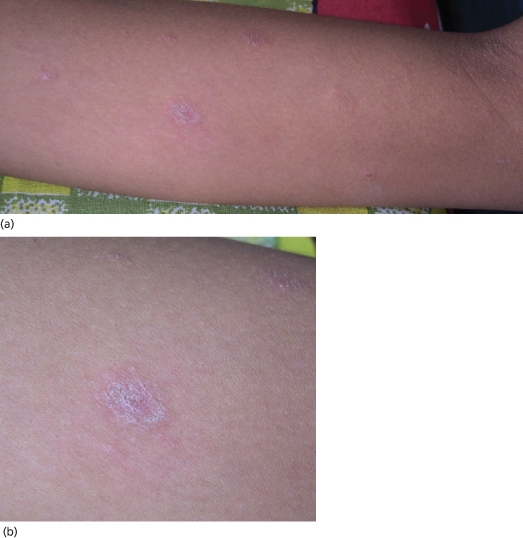
Most children do not experience intense pruritus (Fig. 84.3) [62]. The impact of the rash on the quality of life of children with pityriasis rosea is significantly less than for children with atopic dermatitis [62]. Complications are rare for children and adolescents. When complications do occur, they are more likely to be related to the drug treatments rather than the disease [18]. Most children have no relapse in their lifetime.
Fig. 84.3 (a) Typical lesions of PR on the left forearm of a young girl. (b) She had a herald plaque as the initial lesion on the left arm.
Atypical Presentations.
Atypical features include atypical rash morphology (vesicular, purpuric, haemorrhagic and urticarial), atypical rash size (pityriasis rosea gigantea for exceptionally large lesions, papular pityriasis rosea for exceptionally small lesions), atypical rash distribution (distal aspects of extremities), atypical number of lesions, atypical site of lesions (oral cavity) and atypical severity of symptoms. Atypical rashes are fairly common for adults [66] but are uncommon for children [63]. Papular pityriasis rosea is the most common atypical feature for children.
Differential Diagnosis.
Typical pityriasis rosea in children should be diagnosable clinically. Common differential diagnoses for children and adolescents include guttate psoriasis, lichen planus, nummular dermatitis, parapsoriasis, pityriasis versicolor, tinea corporis, viral rashes and drug eruptions [17]. Uncommon differential diagnoses are secondary syphilis for adolescents, and the early stage of erythema multiforme, guttate hypomelanosis and pityriasis lichenoides [67].
Papular pityriasis rosea in children has to be differentiated from viral rashes including roseola infantum and rubella. Vesicular pityriasis rosea is uncommon in children. Differential diagnoses of this variant include pompholyx, bullous erythema multiforme, chickenpox, dermatitis herpetiformis, linear immunoglobulin A disease and pemphigus vulgaris.
Treatment.
Pityriasis rosea in children and adolescents is a self-limiting disease. Unlike their adult counterparts, this eruption usually has little to no impact on the quality of life of children [62]. The aim of treatment is thus mainly to relieve pruritus, not to modify the course of the disease.
For children with little or no pruritus and a limited number of lesions, no treatment is generally required. For those with moderate pruritus, topical calamine lotion and/or topical emollients might be considered. For children with severe pruritus affecting their quality of life, oral sedating antihistamines might be given as a single nocturnal dose. Topical corticosteroids of mild to moderate potency might be considered to be applied for short durations for children with particularly severe pruritus.
A pseudo-randomized trial (alternate allocation of subjects) reported the efficacy of oral erythromycin in children and adults with pityriasis rosea [68]. However, further studies on children found no significant efficacy for erythromycin [69] and azithromycin [70]. There are also studies and case reports on the efficacy of antiviral agents [71,72], systemic corticosteroids [73] and ultraviolet radiation [74,75]. A Cochrane systematic review found that oral erythromycin might be effective for adult patients, but further clinical studies are necessary before erythromycin or other macrolides can be formally recommended for adult patients [76]. At the present stage of knowledge, for children with pityriasis rosea, these treatment modalities cannot be routinely recommended.
References
1 Feinstein A, Kahana M. Pityriasis rosea of Gibert. J Am Acad Dermatol 1987;16:1260.
2 Percival GH. Pityriasis rosea. Br J Dermatol 1932;44:241–53.
3 Klauder JV. Pityriasis rosea with particular reference to its unusual manifestations. JAMA 1924;82:178–83.
4 Sarkany I, Hare PJ. Pityriasis rotunda (pityriasis circinata). Br J Dermatol 1964;76:223–7.
5 Weiss L. Pityriasis rosea – an erythematous eruption of internal origin. JAMA 1903;41:20–8.
6 De Souza Sittart JA, Tayah M, Soares Z. Incidence pityriasis rosea of Gibert in the Dermatology Service of the Hospital do Servidor Publico in the state of Sao Paulo. Med Cutan Ibero Lat Am 1984;12:336–8.
7 Olumide Y. Pityriasis rosea in Lagos. Int J Dermatol 1987;26:234–6.
8 Vollum DI. Pityriasis rosea in the African. Trans St Johns Hosp Dermatol Soc 1973;59:269–71.
9 Jacyk WK. Pityriasis rosea in Nigerians. Int J Dermatol 1980;19:397–9.
10 Ahmed MA. Pityriasis rosea in the Sudan. Int J Dermatol 1986;25:184–5.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree