Histopathologically, there are few clear characteristics associated with the gross clinical pathology, simply because most case studies and series record the status of the patient at the time of presentation [7]. This could occur at any point in the sequence described above so it is not surprising that different reports describe different characteristics for lesions. As a general rule, it can be said that subsequent to biting, there are varying degrees of oedema and spongiosis; mixed inflammatory cell infiltration, comprising varying levels of lymphocytic, eosinophilic and neutrophilic involvement particularly around blood vessels; occasional extravasation of erythrocytes; and some infiltration inflammation of the periadnexa and sweat glands [22–25].
When evaluated immunologically, the lesions exhibit a wide range of presentations, obviously dependent upon what stage of sensitization has been reached. In some cases the vasculitis is characterized by deposition of complex-like masses with immunoglobulin (Ig)M, C1q and C3 in vessel walls [26]. Other presentations include no deposition of globulins, complement or presence of B lymphocytes but numerous CD45RO and CD3 T lymphocytes and macrophages [23]; high levels of IgG, IgG4, IgE [27]; circulating IgG and IgE as well as infiltrating CD4+ lymphocytes [24]. The reason for such confusions appears to be that the case series described contained patients from across the spectrum of sensitivities, including some who were atopic, and the authors did not adequately relate the reaction state to the immunological characteristics but rather inferred that showing a reaction was more or less equivalent across the group examined [7]. Part of this problem is that still many authors refer to insect bite reaction as ‘allergic’ when clearly no true IgE-mediated allergy status exists.
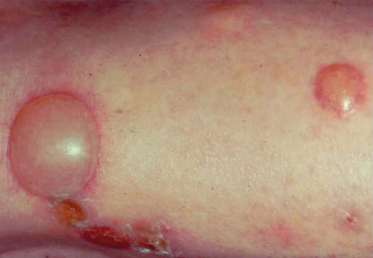
In some cases, anamnestic reactions may not present with the normal responses described above. With passage of time, the level of immunity may regress to an earlier stage if no exposure has occurred for several months or years. Alternatively, the overall presentation may be altered in some cases. For example, this author has observed that children who emigrated from the tropics to temperate countries and had no exposure to mosquitoes for several years but who were later exposed to insects such as Culex quinquefasciatus, the tropical house mosquito that bit them as infants, can suffer extreme bullous reactions, with blisters more like those caused by severe scalding. Bullous reactions of a similar nature were found in one patient who showed IgE antibodies specific to bed bug nitrophorins [28].
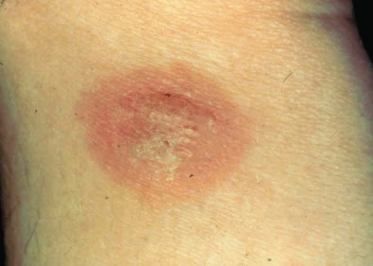
Bites conferred by mites and ticks frequently have a presentation different from those of insects. Some mites, such as the truly parasitic gamasid and cheyletid mites found on birds and rodents, e.g. Dermanyssus, Ornithonyssus and Cheyletiella, feed for a relatively short period and the bite reactions are similar to those of fleas. Others, such as the larval forms of trombiculid ‘harvest mites’ and hard ticks of the family Ixodidae, feed for a prolonged period of several days. The latter feed on blood and engorge only slowly so they require highly effective vasodilators and immunosuppressive salivary components to maintain blood flow to the area during the feeding process. In contrast, the trombiculids feed only on lysed tissue cells and serous exudates drawn through a tube formed by the action of saliva on the tissues. In both cases a lasting scar may form at the biting site (Fig. 71.3), particularly following trombiculid bites, in which case it may be deeply pigmented and last for many months.
Exposure to grain itch mites, Pyemotes spp, may result in spectacular reactions. These mites, which are normally parasites on nuisance insects, often cause extensive bullous reactions that become florid and haemorrhagic. The irritation of the vesicles often results in them being rubbed off and becoming crusted as fluid is expressed. A brownish stain remains that may take several weeks to fade [29].
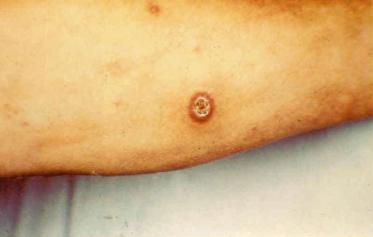
Occasionally, the salivary products of the insect, injected into a bite, may have toxic effects on the victim. Some mosquitoes may induce responses that result in high levels of intense perivascular infiltration, some subcutaneous haemorrhage and fluid accumulation in the tissues so that the area surrounding the bite lesion becomes tense, inflamed, painful and immobile. The associated risk of excoriation, as the person scratches the intensely irritated skin, increases the risk of secondary infection and of development of phlebitis on lower limbs. The bites of some flies, such as the phlebotomine sand flies (Phlebotomus spp) and biting black flies (Simulium spp), are more likely to cause toxic reactions. In the case of the former, a vesicular reaction may develop, with significant localized oedema soon after the first exposures, which then reverts to a crusted lesion that may easily become impetiginized (Fig. 71.4) [30]. Pigmented scars from the response may persist for several weeks or months after exposure. In the case of simuliids, intensely inflamed and swollen limbs, in some cases with erosion of superficial tissues, may develop [31,32] and in severe outbreaks the numbers of patients requiring symptomatic relief may overwhelm local hospitals or surgeries.
The saliva of cat fleas has a toxic effect on some individuals. This author has seen one human case in which the toxic effect of cat flea saliva induced a haemorrhagic reaction that resulted in a bruise-like lesion approximately 25 mm in diameter around each bite. There have also been reports of kittens and calves dying from anaphylaxis after exposure to mass flea bites. Bites from simuliids may induce anaphylactiform reactions. For example, in August 2001, 27 people were hospitalized, many with symptoms of anaphylaxis, after Simulium lineatum and S. variegatum attacked holidaymakers at a water park in the Midlands region of the UK.
Secondary infection following arthropod bites is probably more common than reported. A 5-year retrospective comparison of temperature, the incidence of insect bites referred to general practitioners in the UK and the incidence of impetigo found that peak insect biting occurred soon after temperature peaks and that there was an average 4.6-week lag between reported bites and incidents of impetigo [33]. Where secondary infection occurs, it is not believed to be associated with contamination of the mouthparts of the animal but is more likely the result of contamination of the lesion by bacteria from the skin flora entering either the initial wound or via excoriations resulting from scratching the itchy immune response. Bites by tabanids and simuliids are possibly more likely to result in secondary infection owing to the greater damage to the stratum corneum and other tissues, which may permit invasion of the wound by skin flora or other bacteria coming into contact with the wound prior to healing. Once infected, the bite site may become impetiginized or develop phlebitis, depending upon the depth of penetration and timing of the infection.
Clinical Features.
For most people the presentation of bites is no more than an inconvenience and either it is of little consequence what type of arthropod was involved or else circumstances may make it fairly obvious as to the origin of the bites. In most cases, bites are relatively benign and unlikely to present a continuing problem. In a few circumstances, such as when there is a risk of disease transmission, action of a defined sort is required to avoid biting altogether, such as the use of insect repellents or physical protection in the form of clothing over the skin or using bed nets at night.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree