References
1 Ferahbas A, Utas S, Akcakus M et al. Prevalence of cutaneous findings in hospitalized neonates: a prospective observational study. Pediatr Dermatol 2009;26:139–42.
2 Hoeger PH, Enzmann CC. Skin physiology of the neonates and young infant: a prospective study of functional skin parameters during early infancy. Pediatr Dermatol 2002;19:256–62.
Harlequin Colour Change
Definition.
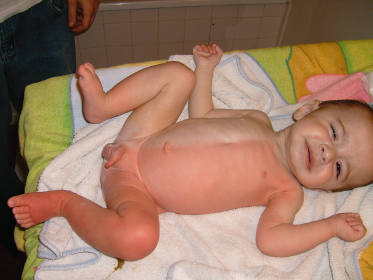
Harlequin colour change (HCC) is defined as transient erythema involving one-half of the infant’s body with simultaneous blanching of the other side and a sharp demarcation on the midline. In some cases, HCC may be associated with tonic attacks and bradycardia, triggered by various factors, including defecation, rectal pain, perineal stimulation or emotion. Such a phenomenon has been referred to as paroxysmal extreme pain disorder (PEPD) [1].
History.
Harlequin colour change was first described by Neligan and Strang [2], who described infants admitted to the nursery of the Princess Mary Hospital in Newcastle upon Tyne, UK, over a 1-year period. They observed that 22 of 250 infants had at least one attack of this condition, with a peak frequency on day 3. Owing to its transient nature, this condition is rarely observed, photographed or studied, and there is probably some confusion between complete HCC and localized transient flushing in neonates.
Aetiology.
Since original reports concerned mostly premature/low-weight babies or infants with intracranial injury, it was long thought that the abnormality in the central nervous control of the vascular tone was located at the hypothalamic level. Indeed, most affected infants are in good general health with no other signs of dysregulation of vital functions. For those infants, the pathophysiology remains unknown.
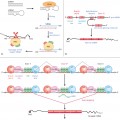
In the subgroup of infants with HCC and non-epileptic tonic seizures triggered by abnormal painful stimulations (PEPD), it has been shown that the disorder is produced by mutations in the SCN9A gene, which encodes the Na 1.7 sodium channel that is preferentially expressed within nociceptive dorsal root ganglion neurones and sympathic ganglion neurones [3].
Clinical Features
Flushing and Isolated HCC
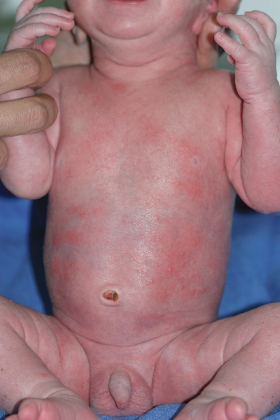
Premature infants are more commonly affected than full-term infants. Harlequin colour change usually occurs on the third or fourth day of life, though it has been noted up until the 21st day of life. The midline demarcation of the erythema and the transitory colour changes (30 s to 20 min) are diagnostic (Fig. 6.2). The face and genitalia are usually spared. The tongue and lips are unaffected. Accentuation occurs following gravitational changes. Turning the infant on the other side may induce blanching of the red side and reddening of the pale side [4].
Paroxysmal Extreme Pain Disorder (PEPD)
Typical flares are precipitated by perineal pain or stimulation, such as insertion of a thermometer into the anus, and consist of stiffening in flexion position, turning pale, and screaming inconsolably, followed by hemicorporeal flushing. After the attack, infants may experience intense sweating, and neurological examination is normal between attacks [3].
Prognosis.
This condition is generally believed to be completely benign. Changes in skin colour should subside after the third week in common HCC, and during the first years in PEPD.
Differential Diagnosis and Treatment.
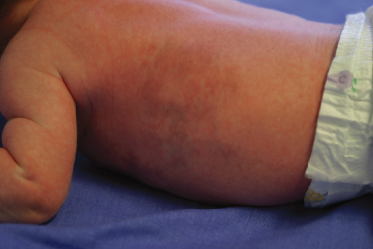
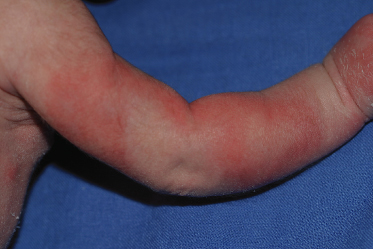
When the transient nature of these changes is not perceived, a large capillary malformation or cutis marmorata telangiectatica congenita (Fig. 6.3) may be suspected. Cyanosis in the newborn is usually not found in a harlequin pattern. Transient dermatographism presenting within the first hours after birth is characterized by urticarial papules and plaques with no midline demarcation (Fig. 6.4) [5].
No treatment is required in isolated flushing or HCC. In PEPD, carbamazepine therapy may be effective to reduce the frequency of the flares.
References
1 Fertleman CR, Ferrie CD, Aicardi J et al. Paroxysmal extreme pain disorder (previously familial rectal pain syndrome). Neurology 2007;69:586–95.
2 Neligan GA, Strang LB. A ‘Harlequin’ colour change in the newborn. Lancet 1952;ii:1005–7.
3 Choi JS, Boralevi F, Brissaud O et al. Paroxysmal extreme pain disorder: a molecular lesion of peripheral neurons. Nat Rev Neurol 2010 Nov 16. [Epub ahead of print].
4 Selimoglu MA, Dilmen U, Karakelleoglu C et al. Harlequin color change. Arch Pediatr Adolesc Med 1995;149:1171–2.
5 La Shell MS, Tankersley MS. Transient dermatographism presenting within the first 18 hours after birth in an otherwise healthy newborn. Pediatr Dermatol 2008;25:130–1.
Transient Localized Hyperpigmentation
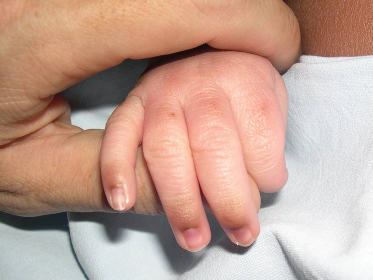
The maturation of the pigmentary system is not completed at birth and some areas may appear markedly hyperpigmented. The genital area, and particularly the scrotum in male infants, and the dorsal surfaces of the distal phalanges of both hands (Fig. 6.5) and feet are the most frequently involved [1,2]. Less frequently, other body areas may be involved, including nipple and areola, helix, umbilicus, and sometimes large skin folds. It is usually a prominent feature of dark-skinned newborns, but it has also been observed in fair-skinned newborns [3].
Perineal or periungual hyperpigmentation is considered as a physiological melanic pigmentation mainly observed during the first year of life and declining around the age of 2 years.
References
1 Taieb A, Boralevi F. Hypermelanoses of the newborn and of the infant. Dermatol Clin 2007;25:327–36.
2 Crespel E, Plantin P, Schoenlaub P et al. Hyperpigmentation of the distal phalanx in healthy Caucasian neonates. Eur J Dermatol 2001;11:120–1.
3 Iorizzo M, Oranje AP, Tosti A. Periungual hyperpigmentation in newborn. Pediatr Dermatol 2008;25:25–7.
Sterile Transient Neonatal Papulopustular Eruptions
Pustular and vesiculopapular lesions represent frequent features that can be observed in newborns, in both transient benign disorders and potential severe diseases, i.e. infections, inflammatory disorders or genodermatoses (Box 6.2). Erythema toxicum neonatorum (ETN) and transient pustular melanosis (TPM) are probably closely related adaptive processes in the newborn. Their description has been separated for the sake of clarity.
Box 6.2 Differential diagnosis for sterile pustular neonatal eruptions (transient pustular melanosis , erythema toxicum neonatorum)
Infections
- Bacterial pustules: bullous impetigo, systemic sepsis (listerosis)
- Congenital cutaneous candidiasis
- Herpes, varicella, cytomegalovirus infection
Non-Infectious Disorders
- Incontinentia pigmenti
- Eosinophilic pustulosis (eosinophilic pustular folliculitis) of the scalp
- Infantile acropustulosis
- Omenn type of severe combined immunodeficiency
- Buckley–Job hyperimmunoglobulin syndrome
- Self-healing histiocytosis
Erythema Toxicum Neonatorum (ETN)
Definition.
Erythema toxicum neonatorum (synonyms: erythema neonatorum allergicum, toxic erythema, urticaria neonatorum, erythema neonatorum) is the most common transient rash in healthy term neonates, affecting 43% of the newborns in a large recent study [1]. It is characterized by small erythematous macules with or without a central papule or pustule (Fig. 6.6) that contains mostly eosinophils. Generally, ETN arises between the first and fourth days of life and lasts 2 or 3 days [2].
History.
The first mention of ETN is attributed to Metlinger, a doctor in Augsburg, Bavaria, who claimed that ETN was a cleaning process from ‘bad blood’ transmitted by the mother. That hypothesis was based on a widespread popular belief, and its treatise ‘Ein Regimen der jungen Kinder’ was published in 1472 [3]. However, there was no good clinical description of the rash until Steiner’s account of the rash, which he named ‘erythema papulatum of the newborn’ [4]. Later, in 1912, Leiner suggested the term ‘erythema toxicum neonatorum’, including toxicum because he postulated that systemic absorption of enterotoxins accounted for the rash [5]. Mayerhofer and Lypolt-Krajnovic found blood eosinophilia as well as eosinophils in pustules, and proposed an allergic cause [6]. Several studies performed in the 1950s aimed to elucidate the pathogenesis of this disorder, with special consideration of the role of eosinophils in neonatal skin and the possible role of allergy [7–10]. In the 1990s, the graft-versus-host (GVH) theory was proposed by Basukas et al. [11], and more recently, Marchini et al. suggested that ETN may be considered as an innate immune response to commensal microbes penetrated into the newborn skin [12].
Aetiology.
The cause of ETN is not yet established, and the different hypotheses found in the historical literature review from the 18th century to the present, remain hypotheses. In 1752, Smellie stated that some features of ETN – ’the red gum’ – are a common process linked to a too long exposure with the meconium [13]. According to Leiner [5], many newborn infants with the condition have dyspeptic disorders; thus, he proposed the term erythema ‘toxicum’ because he postulated that systemic absorption of enterotoxins accounted for the rash. Eosinophilia in skin biopsies and blood is the major finding in support of the allergic theory put forward by Mayerhofer and Lypolt-Krajnovic [6]. However, attempts to identify allergenic agents transmitted transplacentally or in milk or vaginal secretions have not been fruitful, and a history of atopy or allergic diseases in the parents of affected infants has been found to be no more frequent in ETN-affected babies than in control infants [14]. However, administration of an antihistamine, Pyribenzamine, to a series of 75 babies with ETN was found to reduce by half the duration of the rash [7], and several paediatricians have noted that simply stroking the skin of a newborn baby may induce erythema followed by eruption of ETN-like papules. It has been speculated that this is a reaction to mechanical stimulation or simple pressure and thus ETN has been considered to be a transient adjustment of the skin of the newborn to mechanical/thermal stimuli. This condition might be accentuated by removal of the vernix caseosa, which is believed to confer protection against irritants [14].
The specificity of the eosinophilic infiltrate in newborn tissues is an important underlying issue. This phenomenon was investigated 40 years ago by the method of sterile abrasion, a predecessor of the suction blister technique, which is used to obtain a qualitative assessment of the cells that participate in cutaneous inflammation [15]. Application of this technique showed that an inflammatory eosinophilia averaging 19% of the exudate cells is seen in infants at 2–21 days of age, 2 h after the initiation of inflammation. By contrast, infants less than 24 h old, older children and adults exhibit an initial neutrophilic response [15]. This finding may help to explain the differences noted between ETN and TPM.
Carr et al. have clearly shown that the incidence of ETN increases with maturity, as determined by birthweight, gestational age or breast hypertrophy grade in the mother [10]. This suggests that maturity influences the inflammatory response of the skin and may lead to the development of ETN. Several distinct molecules may attract eosinophils to the dermis. These include histamine, lipo-oxygenase products (leukotriene B4), eosinophil chemotactic factor (ECF) and ECF-A produced by mast cells, interleukin 5, and complement factors C5, C5a and C567. None of these molecules has been formally studied in ETN.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree