57 Total Wrist Arthrodesis
Abstract
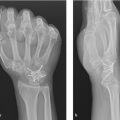
Total wrist arthrodesis is the gold standard treatment for the end-stage arthritic wrist. The procedure involves the fusion of radiocarpal, intracarpal, and sometimes the carpometacarpal joints. High rates of union (98%), satisfaction (96%), grip strength, and physical function underscore the value of the procedure. Total wrist arthrodesis is classically indicated in the higher demand patient with posttraumatic arthritis to include scapholunate advanced collapse and scaphoid nonunion advanced collapse. The procedure is also indicated for inflammatory arthropathy, salvage cases, segmental bone loss, and cerebral palsy. Fusion is most often commonly achieved with an anatomic spanning dorsal plate. The most common complication is tendon irritation. Despite this, the total wrist fusion provides a stable and functional wrist in the setting of advanced arthritis.
57.1 Description
Total wrist arthrodesis offers stability and pain relief, most commonly in the setting of a posttraumatic arthritis.
57.2 Key Principles
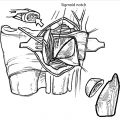
Total wrist arthrodesis involves the preparation and fusion of radiocarpal, intracarpal, and sometimes the carpometacarpal joints. Most surgeons prefer plate fixation but intramedullary devices are another option.
57.3 Expectations
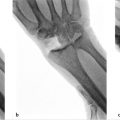
Following total wrist arthrodesis using a compression plate in the setting of posttraumatic arthritis, 98% will go on to union at an average of 10 weeks. Postoperatively, the vast majority are satisfied (91%), would undergo the procedure again (96%), and would have the procedure sooner (91%). 1 Grip strength is 77 to 83% of the contralateral hand. 2 However, most patients will have some degree of pain and experience some limitations with work. 3 These points are critical in preoperative counseling.
57.4 Indications
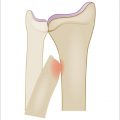
Posttraumatic arthritis of midcarpal and/or radiocarpal joints to include degenerative carpal collapse, following a scaphoid fracture non-union, scapholunate dissociation, or Kienbock disease.
Inflammatory arthropathy of the wrist with instability to include rheumatoid arthritis.
Segmental bone loss from trauma, infection, or malignancy.
Salvage following failed total wrist fusion, limited intracarpal fusion, proximal row carpectomy, distal radius fixation, or total wrist arthroplasty.
Paralytic disorders such as cerebral palsy.
57.5 Contraindications
Cases in which wrist motion is required, either for high-demand activity or to augment digital motion. Some authors would consider a bilateral wrist arthrodesis a relative contraindication.
Active infection.
57.6 Special Considerations
Carpal tunnel syndrome may be concurrently present preoperatively; however, the examination may be veiled by trauma or the pain of an arthritic wrist. In addition, carpal tunnel syndrome may be present in up to 10% of patients following total wrist fusion. 1 Symptoms could be made worse following total wrist fusion secondary to postoperative edema. A complete preoperative physical examination should include testing for carpal tunnel syndrome and, if necessary, a carpal tunnel release should be completed intraoperatively.
Postoperative ulnocarpal abutment should be considered, particularly in the setting of inflammatory arthritis or preoperative ulnar positive wrists. Resecting the distal ulna in patients with rheumatoid arthritis should be preoperative considerations.
57.7 Special Instructions, Positioning, and Anesthesia
The patient is placed supine with the arm extended on a hand table.
In addition to general anesthesia, 20 ml of 0.5% marcaine without epinephrine is used at the onset of the case. Regional anesthesia is always an option, but it is often difficult to obtain adequate intraoperative pain relief.
A posterior interosseous neurectomy may provide a small degree of postoperative pain relief.
57.8 Tips, Pearls, and Lessons Learned
A step cut in the extensor retinaculum may facilitate closure at the conclusion of the case.
Although rarely necessary, the triquetrum may be excised to reduce the likelihood of ulnar impaction and can be subsequently used as bone graft.
Reconstruction plates are not advised because these do not provide adequate stiffness.
First removing the scaphoid, lunate, and triquetrum (PRC) before fusion has a few advantages 4 :
The removed bones are a source of bone graft for the fusion mass.
There is a theoretically decreased risk of nonunion by decreasing the number of moving articular fragments which need to fuse.
There is a theoretically decreased risk of ulnar carpal abutment.
This is a technically simple procedure and is particularly indicated after a previous PRC or spastic pathology.
After a previous PRC, autologous bone grafting is recommended.
Decortication of the radiocarpal and intercarpal joints.
Proximal tibia bone graft is recommended if autogenous bone graft is required.
Some authors prefer not to remove the proximal carpal row in a younger patient to avoid the theoretical shortening of the wrist with a “PRC” wrist fusion. In this situation, bone graft is suggested but not essential.
Additional pearls:
Apply the plate distally over the third metacarpal with fixation of the capitate.
Use the short bend, precontoured wrist fusion plates.
Create a small trough in the distal radius to accommodate the plate. Ensure the plate is centered over the distal radius to properly align the wrist.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree