Viral Infections
Herpes Simplex.
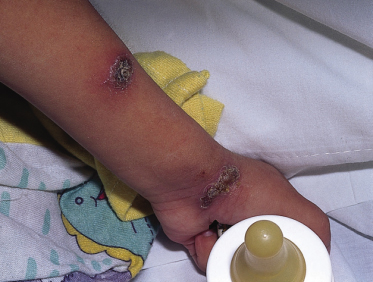
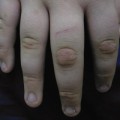
Mucocutaneous infection with herpes simplex is sometimes a severe problem in the child with AIDS [43]. Chronic or recurrent herpetic gingivostomatitis is characterized by painful vesicles and superficial ulcerations on the lips, tongue, buccal mucosa and palate. Without proper treatment, these lesions may progress to large, black eschars. Not infrequently, children with oral herpes simplex develop infection of the fingers, and chronic herpetic ulcers at other locations have also been observed.
Varicella Zoster Virus Infection.
The course of varicella zoster virus infection in children with AIDS is variable [44,45]. For many children with HIV infection, varicella is a benign and uncomplicated infection. However, some of these patients go on to have recurrent episodes of varicella, which may or may not be more severe than the original episode.
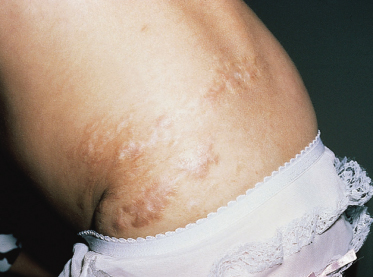
Children with HIV infection have a higher incidence of herpes zoster than do healthy individuals of the same age. Herpes zoster in the child with HIV infection tends to be more severe and painful than in the healthy child; the incidence of permanent scarring (Fig. 52.2) and of recurrence seems to be higher.
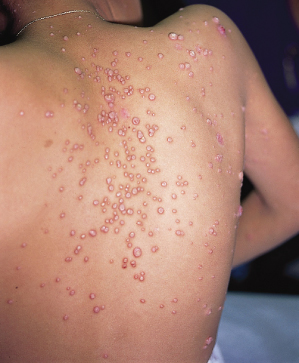
Some HIV-infected children who develop varicella go on to have chronic and persistent infection with varicella zoster virus. The skin lesions in these patients are characteristically hyperkeratotic nodules and plaques (Fig. 52.3), which may be widespread [46,47]. Children with this form of chronic infection may develop pneumonia or central nervous system infection due to varicella zoster virus.
Measles.
In children with HIV infection, measles is often complicated by pneumonia, and the disease can be life-threatening [48]. In most cases, the exanthem is typical (see Chapter 49), although patients with atypical eruptions or without skin disease have been reported. In cases in which the rash is atypical or the patients do not develop antibodies, examination of the skin biopsy can be helpful in confirming the diagnosis [49].
Cytomegalovirus.
A case of napkin dermatitis (nappy rash) from infection with CMV has been reported [50]. The patient, a 6-month-old infant with AIDS, developed an erythematous eruption in the perineum, with crusting, erosions and bullae. Conspicuous viral inclusions were noted on the skin biopsy and CMV was cultured from the skin.
Oral Hairy Leucoplakia.
Oral hairy leucoplakia is induced by the presence of Epstein–Barr virus infection within the oral mucosal epithelium. This disorder is characterized by the appearance of corrugated white plaques, which are usually located on the sides of the tongue. Although oral hairy leucoplakia appears to be relatively unusual in paediatric AIDS, occurrence in children has been reported [51].
Molluscum Contagiosum.
Widespread lesions of molluscum contagiosum are frequently associated with HIV infection (Fig. 52.4). In some children with AIDS, giant and confluent lesions have been reported [30,52].
Human Papillomavirus (HPV).
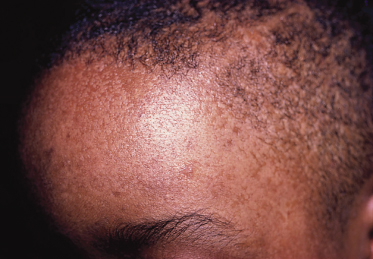
Children with immune suppression secondary to HIV infection may develop widespread common warts. A patient with widespread flat warts due to HPV5 has been reported (Fig. 52.5) [53]. In this case, the appearance of the lesions resembled the phenotype of epidermodysplasia verruciformis. Children with HIV infection may also develop genital or perianal condyloma acuminata [54,55]. In some cases, these lesions are extremely large and difficult to treat.
Gianotti–Crosti Syndrome.
The occurrence of Gianotti–Crosti syndrome in children with HIV infection has been reported [56]. These cases may have been triggered by CMV, hepatitis C virus or by HIV itself.
Infestations
In children with AIDS, scabies usually presents with nodules and crusted papules. However, some patients develop a generalized papulosquamous eruption, with diffuse areas of crusting and scale [57]. Patients with crusted scabies (sometimes termed ‘Norwegian scabies’) are infested with numerous mites, and are highly contagious to family members and health personnel [58].
Demodex infestation has been noted to occur in patients with HIV infection. A facial papular follicular eruption due to Demodex infestation was observed in such a child [59]. Histological examination revealed the presence of tuberculoid granulomas.
Parasitic Infection.
Acanthamoeba infection of the skin may rarely occur in patients with HIV infection [60]. The lesions are pustules, subcutaneous and deep dermal nodules, and ulcers, most often on the extremities and face [61].
Inflammatory Disorders
The incidence of atopic dermatitis may be higher among children with HIV infection. The onset or worsening of this disorder was observed among haemophiliacs after seroconversion [62,63]. The onset or worsening of atopic dermatitis in children with HIV infection may be due to an increased atopic diathesis or to xerosis, bacterial or viral superantigens, or epidermal barrier disruption [64].
Seborrhoeic dermatitis also appears to be somewhat more severe in children with HIV infection. The presentation of this disorder varies markedly with the age of the patient. Among infants, diffuse scaling of the scalp (‘cradle cap’) may progress to widespread involvement of the intertriginal folds and napkin area. Older children develop erythema and scaling of the scalp, nasolabial folds and postauricular skin.
Psoriasis may develop and turn into a severe form during the course of HIV infection [65]. This may occasionally occur in children and adolescents.
Children with HIV infection are at significant risk for drug eruptions, especially due to trimethoprim–sulphamethoxazole. In a single study, 16% of 50 children with AIDS developed a cutaneous eruption from this medication [66]. Lesions may be macular and papular, or morbilliform. Although most HIV-related drug eruptions resolve rapidly after discontinuing the causative medication, severe Stevens–Johnson syndrome and toxic epidermal necrolysis have been observed [67,68].
Hypersensitivity reactions to antiretroviral agents may also result in skin changes. The two most notable reactions are those to nevirapine and abacavir. These reactions are critical to recognize because either can be fatal; stopping the offending agent can be life-saving. Skin reactions to nevirapine, a non-nucleoside reverse transcriptase inhibitor, were recognized during the initial treatment trials of this agent. This drug primarily produces two types of reactions. The first type occurs commonly (32% in one study) and includes moderate-to-severe diffuse maculopapular lesions or dry desquamation generally occurring within the first 2 weeks of starting the medication. The frequency and severity of these lesions can be decreased by increasing the medication dose slowly; hence the 2-week lead-in period where nevirapine is administered once per day instead of twice [69]. If this rash is mild and there are no manifestations suggesting Stevens–Johnson syndrome, then treatment can continue and the rash will generally resolve. The second and more serious reaction that occurs with nevirapine is a typical Stevens–Johnson reaction which does require immediate treatment discontinuation [70]. Drug rash with eosinophilia and systemic symptoms (DRESS syndrome) can also occur as a side-effect of nevirapine in children [71]. Similar rashes can occur with other drugs in this class, including efavirenz; however, skin reactions to these other agents occur less frequently than with nevirapine.
Abacavir produces a significant hypersensitivity reaction in about 5% of recipients, usually beginning within 6 weeks of starting the medication. The reaction is strongly correlated with the presence of the HLA-B57 antigen [72]. This reaction includes fever in 80% and rash in 70% [73]. Multiple organ systems are often involved. The eruption is papular and diffuse, but may include macules. It is only occasionally itchy, and is often mild; sometimes the rash is not noticed by the patient [74]. If abacavir hypersensitivity is suspected, the medication must be stopped immediately and never restarted. Patients with suspected abacavir hypersensitivity should never be rechallenged as the reactions with repeat exposure are rapid, severe and often fatal.
Other reported adverse cutaneous effects of highly active antiretroviral therapy (HAART) in children include xanthomas and hyperlipidaemia [75] and lipodystrophy syndrome [76]. Lipodystrophy syndrome is characterized by fat redistribution, with peripheral fat wasting and abdominal adiposity.
Chronic leucocytoclastic vasculitis has been observed in a number of children with HIV infection. In one child, chronic palpable purpura of the lower extremities was the sole manifestation of HIV infection [77].
Pyoderma gangrenosum has been reported in two children with AIDS [78]. In one patient, this skin disease responded to treatment with dapsone. Pityriasis rubra pilaris (PRP) has been reported in both children and adults with HIV infection. In these patients, PRP appears to have a poor response to treatment; nodulocystic and lichen spinulosus lesions may occur [79,80]. Ashy dermatosis (erythema dyschromicum perstans) has also been observed in children with HIV infection [81].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree