Complications include herpetic whitlows, spread to areas of the face or eye and transfer of infection to other body sites by scratching, including the genital areas.
When lesions are widespread, the clinical diagnosis is not usually in doubt. Differential diagnosis of less severe HSV oral infection and pharyngitis includes aphthous stomatitis, herpangina due to enteroviruses, infectious mononucleosis, streptococcal infection, diphtheria and Stevens–Johnson syndrome.
Recurrent Herpes Gingivostomatitis
Between 20% and 40% of the population, at some stage, will have recurrent orolabial HSV lesions [2,36]. Lesions are usually on the lips rather than intraoral and are colloquially referred to as ‘cold sores’. The site most commonly affected is the mucocutaneous junction of the lips. The lesions of HSV 1 are more frequently recurrent than those of HSV 2 [38]. In comparison with the initial infection, recurrent HSV lesions are usually less severe, more localized and heal more rapidly. A prodrome including irritation, tingling, pain, numbness and a burning sensation occurs at the affected site, usually less than 6 h before a lesion appears. Some 60% of patients will experience a prodrome. Initially erythema is present, followed by papules and then vesicles. The vesicles rupture within 2–3 days, leaving an ulcer that becomes encrusted. Healing is usually complete by 6–10 days. Constitutional symptoms including fever are uncommon but with recurrent HSV lesions, mood changes in children are well documented. Cranial nerve palsies, cluster headaches and psychotic episodes have been associated with HSV recurrences [40,41]. In 80% of cases, a single lesion is present and less than 5% of patients will have two or more lesions.
One-quarter of individuals experiencing recurrences will have two or more episodes per year. Factors that have been implicated in reactivation include ultraviolet light, local trauma, wind, concurrent infections, local dental or surgical procedures, stress and menstruation.
Herpetic Whitlow and Hand Lesions
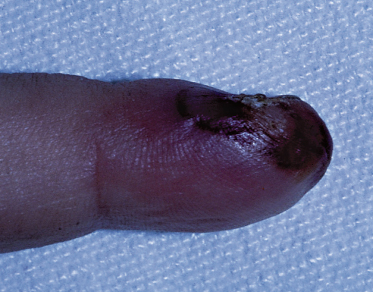
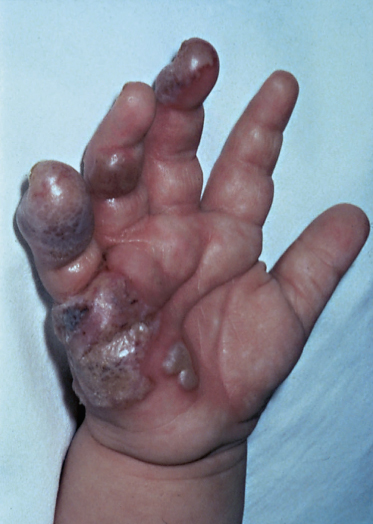
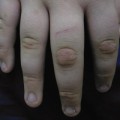
Herpes simplex virus infection of the digits is most commonly described as herpetic whitlow, herpetic paronychia or felon [42–44] (Figs 48.2, 48.3). Lesions may occur anywhere on the hand, and ‘herpes manus’ has been suggested as an appropriate name.
Herpetic whitlows tend to occur in young children with primary HSV gingivostomatitis due to autoinoculation from finger/thumb sucking, and multiple digits may be involved [45,46]. Autoinoculation may occur in older children due to nail biting [47], and in teenage children whitlows may be present in association with primary genital infection [48,49]. HSV infection of the digits less commonly occurs as a result of a contact who has HSV (usually a close adult relative with recurrent HSV labialis), kissing an affected digit [11] or toe [49] or after physical trauma [13]. Most lesions are due to HSV 1.
The finger is the site most commonly affected, accounting for 67% of lesions. HSV infection usually involves the digital pulp space and lateral aspect of the fingers, with the lateral or proximal nailfold being affected only rarely. The thumb, palm and wrist are affected in order of decreasing frequency.
Children with a primary infection from exogenous inoculation have the most severe illness and are often febrile and have constitutional symptoms. Presentation is with sudden onset of pain, redness and swelling around the infected area. The infected site is initially erythematous and swollen followed by vesiculation, development of pustules and rupture of lesions. On heavily keratinized areas such as the palm, vesicles may coalesce and, after pustulation, resolve slowly without breaking [9]. The fluid from lesions is often clear, opalescent or serosanguinous rather than pus. The draining lymph nodes, including the epitrochlear and axillary, are often enlarged and tender. Lymphangitis may be prominent. Spontaneous resolution tends to occur in 18–20 days. Recurrences are usually less severe, occur in approximately 20% of cases and are of shorter duration than the initial infection, lasting 7–10 days. A prodrome of pain, tenderness, pruritus, aching or burning is usually experienced and lasts a variable time interval of a few hours to 3 days. Triggering factors are the same as for recurrent herpes labialis. It is important to distinguish HSV infection from bacterial infection of the hand to avoid unnecessary surgery [10,50].
Complications of HSV infection of the hand are rare but include local hypoaesthesia, secondary ocular involvement and genital disease.
Genital Herpes Simplex Virus Infection (Herpes Genitalis)
Most children with HSV genital infection [2,51–55] are adolescents, after the onset of sexual activity [11]. Most infections are due to HSV 2, although there is an increase in HSV 1 genital disease [53]. Younger children may acquire HSV genital infection due to autoinoculation from herpetic digital disease or gingivostomatitis [54], exogenous inoculation from a carer, usually a parent with recurrent herpetic digital disease [56], close non-sexual physical contact and child sexual abuse [57–59]. In the young child, careful judgement is often needed when considering the route by which herpetic genital disease has been acquired, and the possibility of child sexual abuse must be considered [57,58].
Primary HSV genital infection may be asymptomatic but can be severe if there has been no previous HSV exposure (HSV seronegative). A milder illness tends to occur if antibodies to the heterologous HSV are present. Symptoms tend to be more extensive in females than in males because of a larger area of skin and greater mucous membrane involvement. Multiple anatomical sites (labia majora, labia minora, vagina and cervix) are usually infected. The incubation period is usually 2–7 days. Initially one or more small pruritic erythematous papules appear, which then progress rapidly to vesicles. After 3–5 days, the vesicles develop into painful shallow ulcers that crust. New crops can appear for up to 10 days. Associated symptoms include pain, itching, fever, dysuria, vaginal and/or urethral discharge, malaise, headache, myalgia, paraesthesia, herpetic whitlow, an ulcerative/exudative pharyngitis (10–15% of cases) and, less commonly, self-limited aseptic meningitis. In males, urethritis and dysuria out of proportion to the urethral discharge is suggestive of HSV infection. The illness tends to last 2–3 weeks. Complications include secondary bacterial infection, urinary retention and fibrinous adhesions leading to phimosis in males and labial adhesions in females. When there are ulcerative lesions in adolescents, then syphilis co-exists with HSV in 3–10% of cases and the risk of HIV infection is increased significantly [53]. The ulcers of HSV are often smaller than isolated syphilitic ulcers [53].
Herpes simplex virus 2 genital infections are more frequently recurrent than those due to HSV 1 [37,60]. Recurrences are of shorter duration than the initial genital infection and are less intense and usually without systemic manifestations. Long-term complications of recurrent HSV genital infection include physical discomfort, psychological disturbances [61], transmission of HSV to neonates and an increased risk of human immunodeficiency virus (HIV) infection, probably due to the entrance of HIV into the ulcers [11].
Other Cutaneous Herpes Simplex Virus Infections
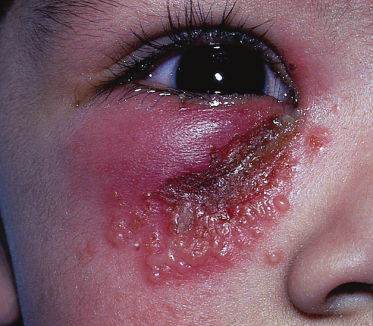
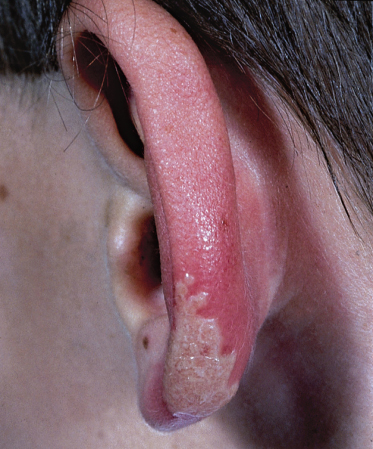
Herpes simplex virus infection may occur at any site on the body, particularly where the skin surface is abraded. Figure 48.4 shows HSV infection beneath the eye and Figure 48.5 shows primary HSV infection of the pinna of an 8-year-old boy. Epidemics may occur in sports involving close physical contact such as rugby players (scrum pox) [62] and wrestlers (herpes gladiatorum) [63]. Young sportspeople often do not report their HSV infection because of an intense desire to compete, and exposed areas of skin of fellow players are susceptible to HSV infection.
Herpes Encephalitis
Herpes simplex virus encephalitis [64–66] tends to present with non-specific symptoms and signs in children. It should be suspected in a febrile child with focal seizures, focal neurological signs and progressive decrease in the level of consciousness. Skin lesions are usually not prominently present. Treatment with aciclovir, especially if started early in the course of the illness, has significantly decreased morbidity and mortality from HSV encephalitis.
Herpes Keratitis
This is rare as a primary HSV infection in children or as an extension of oral lesions [67–70]. It may occur due to inoculation from HSV digital disease. Redness, watering, discharge, itching and eyelid swelling may be present. Less common symptoms include pain, photophobia, lid vesicles, ulcers and blurred vision. Recurrences are not uncommon and iridocyclitis, keratouveitis and corneal scarring may occur.
Disseminated Herpes Simplex Virus Infection
Disseminated HSV infection in otherwise healthy children has been reported but is very uncommon [71]. Predisposing conditions include chronic protein malnutrition, concomitant infection such as measles, pertussis or Haemophilus influenzae [69,71], immunocompromised children, neonates and dermatoses that predispose to cutaneous HSV infection. Predisposing dermatoses include Darier disease [72], ichthyosis vulgaris [73], burns [74–76], congenital ichthyosiform erythroderma [77], incontinentia pigmenti [78] and pemphigus foliaceus [79]. Disseminated infection may involve the liver, lungs, adrenals, pancreas, small or large bowel, kidneys, bone marrow and central nervous system and is usually associated with widespread cutaneous lesions [64,80,81].
Immunocompromised Children
Children with a primary immune deficiency [2,82] mainly affecting cell-mediated immunity are particularly susceptible to HSV infection, unlike those with impaired humoral immunity [9]. Similarly, children with an underlying malignancy on cytotoxic therapy and those with leukaemia or acquired immune deficiency syndrome (AIDS) have an increased susceptibility to HSV. HSV infection is usually due to reactivation of virus. There is a spectrum of disease ranging from lesions that are localized, short-lived and self-limited with normal healing to prolonged destructive lesions occurring with increased frequency. Lesions are usually in sites typically infected by HSV (oral mucous membranes, genital area, cutaneous sites). Less commonly, HSV causing respiratory disease (tracheobronchitis, pneumonia) or oesophagitis, usually due to an extension of oral lesions and HSV colitis, has been reported [83].
Eczema Herpeticum
See Chapter 33.
Neonatal Herpes Simplex Virus Infection
See Chapter 9.
Erythema Multiforme
See Chapter 78.
Treatment of Herpes Simplex Virus Infections
Primary
Mild uncomplicated HSV infections require no treatment.
Supportive Therapy.
Supportive therapy includes effective analgesia, local hygiene and antibiotics for secondary bacterial infection. Oral fluids need to be encouraged when multiple mouth lesions are present. Severe cases of HSV gingivostomatitis should be monitored for dehydration and treated with intravenous fluids if this becomes a problem.
Specific Antiviral Chemotherapy.
Treatment with specific antiviral therapy depends on severity and site of infection [2,37,84–88]. In primary HSV, gingivostomatitis treatment is usually needed only if infection is severe or if the patient presents early in the course of disease. Patients late in acute disease are unlikely to benefit from treatment. Treatment is required in disseminated infection, an immunocompromised child, painful herpetic whitlows and most genital infections. Topical antiviral therapy is used in the treatment of herpetic eye infections.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree