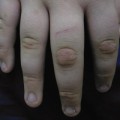
Fig. 39.2 In this adolescent, pompholyx is in a late phase in which small crusts are intermingled with scales but always in a typical bilateral distribution.
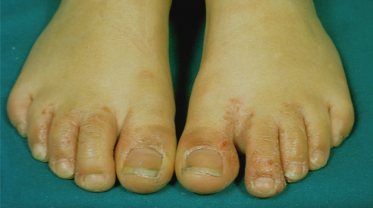
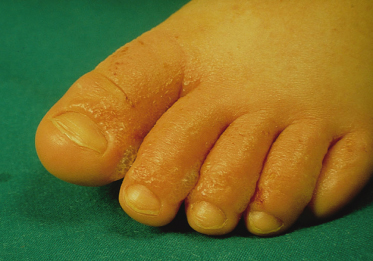
Fig. 39.3 Discrete vesicles are present on the plantar surface of this infant who is affected by atopic dermatitis.
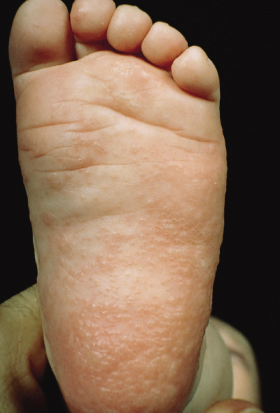
Fig. 39.4 A closer view of the lesions illustrated in Fig. 39.1 reveals that the vesicles have become confluent and have formed multiloculated bullae.
Even in the absence of treatment, the course of the disease can vary greatly from case to case; one common occurrence is a series of attacks that last for a few days to a few weeks and subside spontaneously in 2–3 weeks with desquamation. Exacerbations are the rule, but it is difficult to predict both the number and the severity of the attacks. When superinfection of primary blisters occurs, pustular lesions may develop. Erosions and ulcerations may also complicate the clinical appearance. Extensive vesiculation may cause disability by compromising the function of hands (and feet) and therefore disturbing school activities. Secondary lymphoedema [33] can occur but constitutional symptoms, such as fever, are exceptional. In some of those patients, lymphoscintigraphy revealed a failure of small lymphatics of the hand to absorb and drain lymph to regional nodes [34].
Differential Diagnosis.
Infantile acropustulosis characteristically affects darker-skinned infants in the first months of life [35,36], an age at which pompholyx is exceptional, and the lesions are easily seen as pustular rather than vesicular. Histopathologically, eosinophils and neutrophils predominate. ‘Hand, foot and mouth disease’ should be easily differentiated from pompholyx by the presence of lesions on the oral mucosa. In hand, foot and mouth disease, vesicles are oval, correspond with the hand-lines, show a typical lilac border and do not tend to merge but remain individually distinct [37]. Palmoplantar psoriasis starts with pustules rather than vesicles and the subjective sensation is burning rather than itching [38].
Dermatitis herpetiformis, besides the other symptoms associated with gluten sensitivity, can involve the palmar and plantar surfaces, but the flexor surfaces of the fingers rather than their sides are affected and the blisters are often haemorrhagic [39]. Blistering distal dactylitis is a rare streptococcal disease of children [40] which, unlike pompholyx, is rarely pruritic and, rather than being present on the sides of fingers, is found typically at their tips. Localized bullous pemphigoid, another rare disease, shows blisters, and not vesicles, which are often haemorrhagic [41].
Recurrent palmoplantar hidradenitis [42] is an entity that has in common with pompholyx only the topography; the lesions are completely different as they are tender and inflamed papules and nodules. Papular–purpuric ‘gloves and socks’ syndrome, previously described in adults as a characteristic exanthem affecting the distal part of the extremities, has also been observed in children [43]; the lesions are erythematous, involving the dorsa of the hands and feet, which rapidly become purpuric.
Treatment.
Treatment of pompholyx should be based around avoiding the offending cause. However, this is difficult, especially in children, in whom the possibility of pompholyx from nickel allergy or superficial mycosis is low. Causal treatment of the pompholyx related to metal allergy includes avoidance of any contact with nickel-containing metals, a low-nickel/chromium/cobalt diet (in both the child and the mother in cases of breastfed infants) [16,17] and, in cases of clearly defined nickel allergy, the administration of chelating agents, such as diethyldithiocarbamate and tetraethylthiuram disulphide [44] and disodium cromoglycate [45] have occasionally been helpful. Causal treatment of pompholyx related to superficial mycosis involves the eradication of the fungus and local hygiene.
Treatment of pompholyx associated with atopy, the most common form in children, involves symptomatic treatment, including topical corticosteroids of medium or high potency [46], zinc oxide ointments and oral antihistamines. Topical steroids are used widely for management of the condition, but their efficacy is limited by low percutaneous absorption of drugs in palmar–plantar areas unless super-potent molecules are used. Zinc oxide or water pastes can be used in the acute phase for their mild anti-inflammatory and protective properties. Oral antihistamines appear, in most cases, only moderately effective. A short course of oral steroids is rarely indicated but it may be justified in severe cases. In adult patients, the following treatments have also been used: intradermal botulinum toxin [47], topical calcineurin inhibitors: tacrolimus [48] and pimecrolimus [49], radiation therapy [50], azathioprine [51], methotrexate [52], mycophenolate mofetil [53], UVA1 irradiation, topical or bath PUVA [54] and tap water iontophoresis with pulsed direct current [55].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree