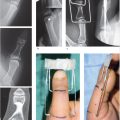
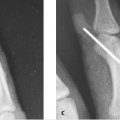
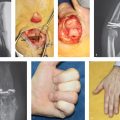
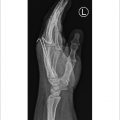
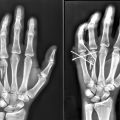
39 Limited-Open Retrograde Intramedullary Headless Screw Fixation of Metacarpal Fractures
Abstract
Most metacarpal fractures can be treated conservatively with immobilization. Surgical intervention includes open reduction and internal fixation (ORIF). There are various indications for ORIF of metacarpal fractures as well as multiple approaches and techniques. Intramedullar fixation with screws has become an increasingly popular method of treatment. This method of fixation may offer clinical advantages over Kirschner wire fixation and other open techniques.
39.1 Description
Fixation countersunk beneath the articular surface is well-accepted for various upper extremity fractures. Multiple fixation techniques for displaced and significantly angulated metacarpal neck and subcapital fractures as well as axially stable shaft fractures have been described, 1 , 2 , 3 , 4 , 5 including percutaneous and limited open antegrade (i.e., bouquet pinning), retrograde (i.e., longitudinal intramedullary fixation), transmetacarpal Kirschner wire constructs, as well as plate fixation. Each technique is associated with its own advantages and disadvantages. There is no consensus on an optimal treatment modality. Selection of technique remains based upon fracture characteristics and surgeon preference. Optimal surgical fixation will limit surgical exposure of the fracture site, allow for early postoperative mobilization to regain full metacarpophalangeal (MCP) joint motion and extensor excursion, expedite return to activities of daily living and work/sport, and minimize the need for removal of hardware.
Limited-open retrograde intramedullary headless screw fixation may offer clinical advantages over Kirschner wire fixation and other open techniques. Retrograde intramedullary fixation using a cannulated headless screw can be achieved using a limited-open, extensor-splitting approach and represents only one additional step beyond longitudinal, intramedullary, retrograde Kirschner wire fixation of these fractures through the metacarpal head articular surface. The headless design allows for fixation buried beneath the articular surface and early postoperative joint range of motion.
39.2 Key Principles
Quantitative three-dimensional computed tomography (3D-CT) data from our group supports the use of an articular starting point for these extra-articular fractures. 6 Direct visualization of the starting point additionally and potentially eliminates multiple attempts at achieving the correct starting point during percutaneous Kirschner wire insertion for retrograde intramedullary fixation. In addition, in 3D models simulating this technique, metacarpal head surface area and subchondral head volume occupied was minimal. Articular surface area violation was least during clinically relevant sagittal plane arc of motion, because the dorsal articular starting point is in line with the medullary canal and avoids engagement of the center of the articular base through a majority of the sagittal plane arc.
In metacarpal neck/subcapital fractures and axially stable shaft fractures that can be close reduced, countersunk, intrame-dullary headless screw fixation achieves relative stability by obtaining isthmal purchase. Reduction and rotational stability are maintained with distal fixation within the subchondral bone and proximal fixation against the endosteal isthmus of the medullary canal of the diaphysis. The buried location of the screw obviates the need for subsequent removal. The rotational stability and lack of requisite hardware removal are improvements over previously described intramedullary nail techniques for metacarpal fractures. In subcapital fractures with limited distal bone stock, this technique avoids low-profile locking plates at the level of the dorsal articular margin which may cause extensor adhesions and extension contractures, necessitating secondary removal of hardware, extensor tenolysis, and extension contracture release. Avery and colleagues found that, when compared to K-wires, headless compression screws for metacarpal neck fractures were biomechanically superior in load to failure, 3-point bending, and axial loading. 7
39.3 Outcomes
As this technique has gained popularity, medium-term clinical, functional, and radiographic outcome data have become available from several centers. In 48 metacarpal fractures treated with this technique by del Piñal et al, 8 the mean total arc of motion was 249 degrees and all patients returned to full work duties or leisure activities. In a retrospective review of 18 metacarpal fractures who underwent intramedullary headless screw (IMHS) fixation, Tobert et al 9 reported excellent functional outcomes in all patients with total active motion in excess of 240 degrees. Similarly, Ruchelsman et al 10 published clinical data on 20 patients with metacarpal neck and shaft fractures treated with IMHS. At 3-month follow-up, all patients had osseous union, full composite flexion, and extension, and no secondary procedures were required. Recently, Ruchelsman et al have presented longer term data in 91 patients treated with this technique. All 91 patients achieved full composite flexion, and all of them also achieved full active MCP extension or hyperextension. Postoperative mean MCP joint flexion-extension arc was 88° degrees. 11 In addition, all 16 elite/professional athletes treated with IMHS fixation for acute displaced metacarpal neck/subcapital and diaphyseal fractures achieved full composite MCP motion and mean return to full play in 5 weeks. 12
A recent multicenter cohort comprising 160 metacarpal neck and shaft fractures treated by three fellowship-trained hand surgeons revealed a low overall complication rate (2.5%). 13 Complications included three refractures due to recurrent blunt trauma (punching mechanism), following complete union and return to full activity, and only one case of early radiographic arthrosis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree