34 Fixation of Uni and Bicondylar Phalangeal Fractures
Abstract
Phalangeal condyle fractures represent a complex spectrum of injury ranging from nondisplaced to inherently unstable fracture patterns. The challenge for the clinician is to decide which fractures require fixation and what fixation technique to use. An overview of surgical indications, techniques, and challenges is provided.
34.1 Description
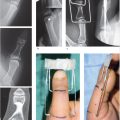
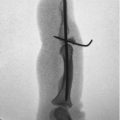
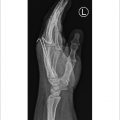
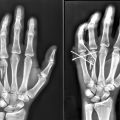
Condyle fractures are intra-articular fractures involving the distal aspect of the proximal and middle phalanx. The majority of condyle fractures tend to be inherently unstable, even if nondisplaced initially. 1 Management of these injuries must account for the unique architecture of this joint, as it is not a simple hinge. The condyles of the proximal and middle phalanx have smaller radii of curvature compared with the concave base of the middle phalanx, providing motion with 4 degrees of freedom. 2 3 The structure of this joint provides mobility, stability, and circulation of synovial fluid. These relationships are lost with intra-articular and comminuted fractures, which must be repaired or reconstructed to restore normal function.
34.2 Key Principles
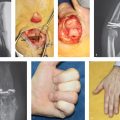
Evaluation must take into account (1) angulation or malrotation at the fracture site; (2) fracture pattern to judge stability; (3) and status of the surrounding soft tissues. Operative management is focused on restoring articular congruity and fracture stability. The priorities in postoperative management for isolated condyle fractures are early range-of-motion and edema management, given the propensity for PIP joint stiffness.
34.3 Expectations
Outcomes are patient-specific because of the multiple factors that influence recovery of motion. Diligent and aggressive rehabilitation is often required to maximize results; therefore, patient compliance with therapy is essential. An average result would typically be an arc of motion from 10° of extension to 80 to 90° of flexion. Among unicondylar fractures, volar shear fractures tend to have the greatest limitations in total active motion (57°) at an average 3-year follow-up. 4 Postreduction limitations in motion are more often related to soft tissue contracture than fracture alignment.
34.4 Indications
Unstable/Displaced intra-articular unicondylar fractures
Bicondylar fractures
Malunion
Traumatic loss of condyle—osteochondral graft
34.5 Contraindications
Nondisplaced unicondylar fractures in children (relative contraindication: thicker periosteum may be intact and confer stability) 5
Unrealistic expectations
Inability to engage hand therapy
Low functional demands
Concomitant severe injuries
34.6 Special Considerations
Small unicondylar fragments take their sole blood supply from the retained collateral ligament attachment. This attachment must not be stripped during exposure of the fracture to avoid osteonecrosis of the fracture fragment.
No intra-articular displacement should be tolerated as this will likely lead to angulation of the digit. 5
If managed nonoperatively, nondisplaced oblique fractures should be followed closely with weekly X-rays for a minimum of 3 weeks.
34.7 Special Instructions, Positioning, and Anesthesia
Can be performed under general anesthesia, regional block, or a digital block
Supine with hand outstretched on a hand table
A tourniquet can be applied to the upper arm or digit
Mini C-arm fluoroscopy available for intraoperative use
Kirschner (K) wires (0.028-0.045 inch)
Modular handset (1.0, 1.3-mm screws and 0.7- to 2-mm drill), depth gauge, screw driver
If osteotomies are planned: Small osteotome, sagittal saw (0.4- to 1-cm blades)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree