31 Distal Phalanx Fractures: Percutaneous Pinning and Open Reduction Internal Fixation
Abstract
The majority of distal phalangeal fractures can be successfully treated nonoperatively. However, there are several fracture subtypes that warrant surgical intervention. Surgical stabilization of mallet fractures, Seymour fractures, and open fractures may aid in early rehabilitation and prevent long-term sequelae. In the following text we will review operative indications and various techniques to confer skeletal stability to fractures of the distal phalanges.
31.1 Description
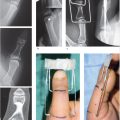
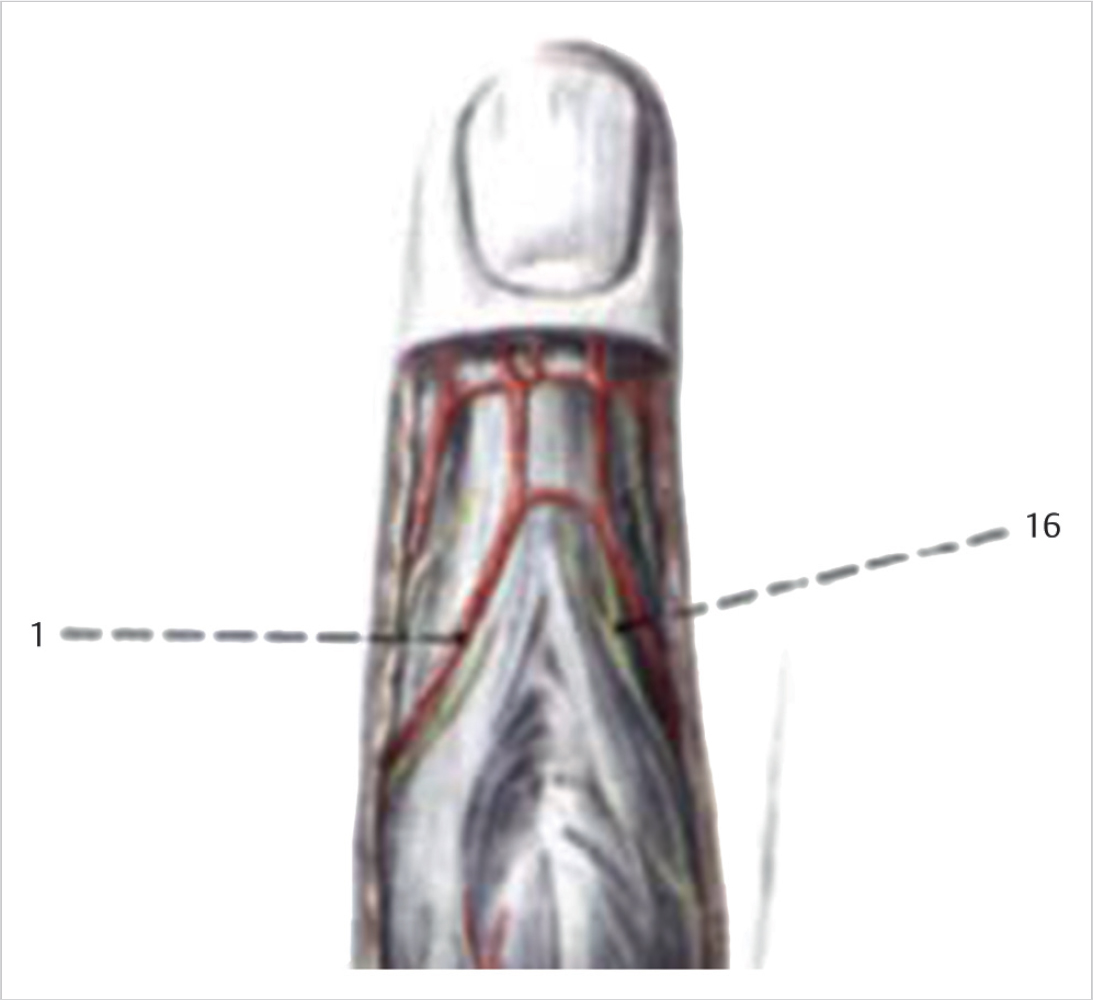
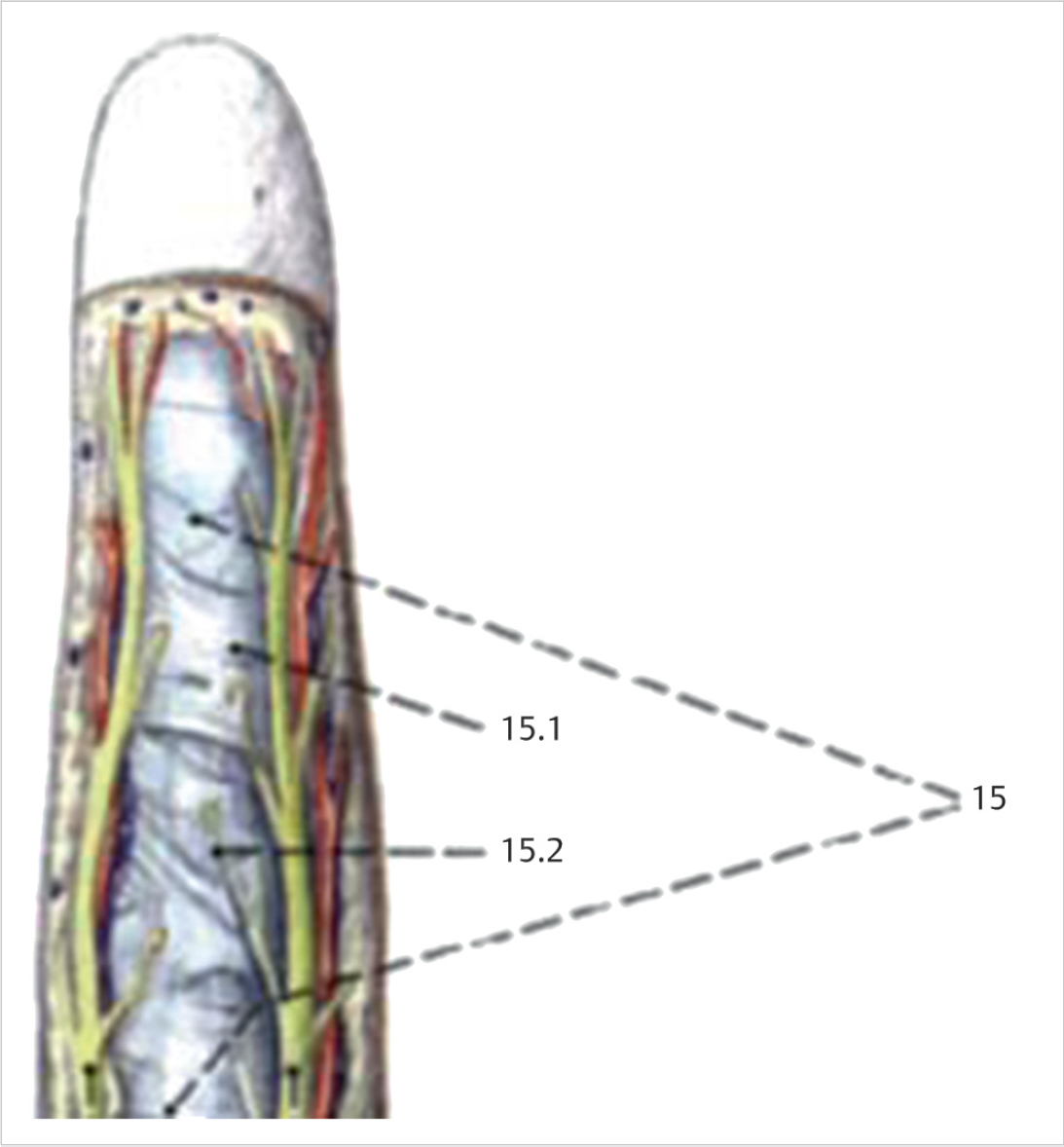
To employ the appropriate treatment of fractures of the distal phalanx one must be familiar with its unique and complex anatomy. The digital arteries and nerves trifurcate distal to the distal interphalangeal joint (DIP) joint and converge centrally. The extensor tendon complex inserts dorsally proximal to the physis/epiphyseal scar (► Fig. 31.1). The flexor digitorum profundus (FDP) inserts volarly over a broad area in the metaphysis (► Fig. 31.2). The fibrous septae that comprise the volar pulp stabilize the distal phalanx volarly. Dorsally the nail plate confers significant stability to the distal phalanx.
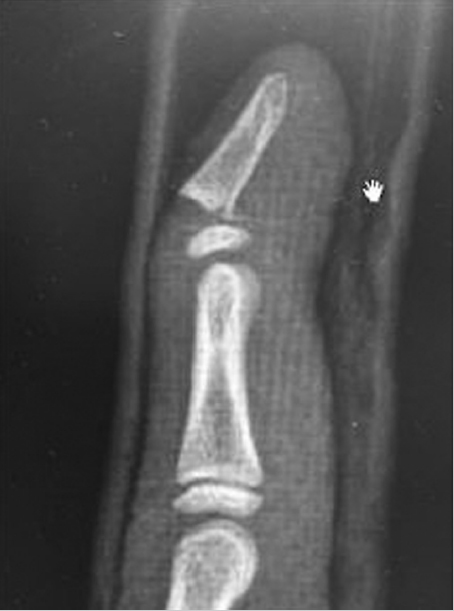
Various fracture patterns are observed in the distal phalanx. Tuft and shaft fractures are often due to a high energy or crushing mechanism. Fractures of the articular base are usually due to an axial load with a torsional component. Two additional fracture patterns bare special mention: mallet fractures and Seymour fractures. Extensor tendon avulsion fractures (mallet fracture) are due to a hyperflexion or resisted extension moment. The dorsal corner of the base of the distal phalanx fractures is often retracted proximally with the extensor tendon complex. Seymour fractures occur in skeletally immature patients due to a hyperflexion moment on the distal phalanx. This results in failure of distal phalangeal physis. These are often confused with a mallet fracture. In these fractures the germinal matrix can become incarcerated in the physis causing growth disturbance and infection that may result in osteomyelitis.
31.2 Key Principles
Most distal phalangeal fractures are inherently stable due to the support conferred by the fibrous septae and nail plate. Surgical fixation is reserved for specific indications (discussed below). Often fractures are due to a crush-type mechanism resulting in significant comminution and involvement of the tuft. In this setting, evaluation for associated nailbed injuries should be performed to prevent infection and/or chronic deformity. If possible, restriction of proximal interphalangeal joint (PIP) joint range of motion (ROM) following either operative or nonoperative treatment should be avoided.
31.3 Expectations
The majority of patients with simple transverse fractures will recover well with no sequelae. Patients who experience crushing injuries, especially those associated with soft tissue injury such as nailbed lacerations will often demonstrate hypersensitivity about the fingertip for many months. In addition, these patients have a high incidence of nail deformities. Mallet fractures usually do well regardless of the quality of the joint reduction. It is not uncommon to observe a persistent extensor lag of 10° to 20°. This does not typically impact function. Seymour fractures are prone to growth arrest with resultant cosmetic deformity but minimal functional deficits.
31.4 Operative Indications
31.4.1 Seymour Fractures 1
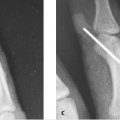
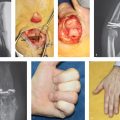
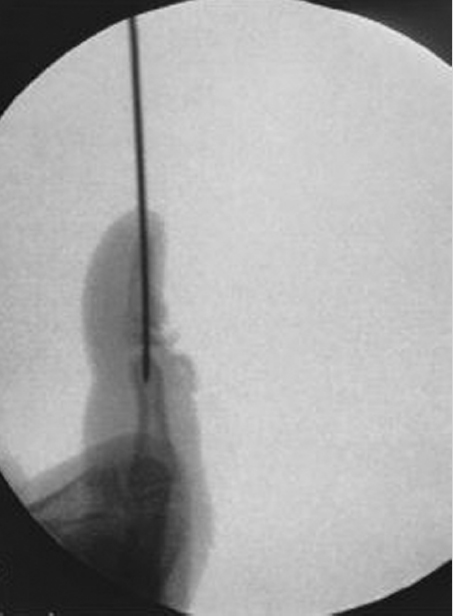
Surgical intervention is reserved for open injuries with associated nailfold/skin lacerations. If the fracture is open and/or the nail plate has been dislodged from the eponchial fold, surgical irrigation and debridement as well as fracture reduction is warranted. Any interposed germinal matrix has to be excised from the physis to limit the degree of nail deformity and minimize the likelihood of bone growth disturbance. The necessity of skeletal fixation is dependent upon the stability of the fracture following reduction but it is not mandatory (► Fig. 31.3 and ► Fig. 31.4).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree